You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
The American Cancer Society estimates that in 2014 there were over 1.5 million new cases of cancer in the United States alone. Many cancer patients are unaware that cancer treatment can affect the oral tissues, and that visiting their dentist should be an integral step in the treatment of the disease. Oral complications can affect patients undergoing treatment for cancer. The dental team must be able to treat, educate, and support these patients. Open communication must exist between the patient, the dental team, and the radiation and/or oncology team. This course will provide the dental team members with information about potential oral complications and how these potentially serious problems can be prevented or managed. The dental team's role in patient management can extend benefits beyond the oral cavity.
Oral complications from radiation to the head and neck or chemotherapy for any malignancy can seriously compromise health and quality of life, as well as affect the ability to complete planned cancer treatment. Moreover, pre-existing or untreated oral disease can complicate cancer treatment. The complications can be so debilitating that patients may only tolerate lower and less effective doses of therapy, may postpone scheduled treatments, or may have to discontinue treatment entirely. Mucositis is the number one reason for the interruption of chemotherapy and head and neck radiation protocols. Oral complications also can lead to potentially life-threatening systemic infections. In 54 percent of cancer patient deaths from infection, the causative organism is from the oral cavity. Medically necessary oral care prior to, during, and after cancer treatment can prevent or reduce the incidence and severity of oral complications, enhancing both patient survival and quality of life.
Oral Complications Related to Cancer Treatment
Oral complications of cancer treatment arise in various forms and degrees of severity, depending on the individual and the cancer treatment. Chemotherapy often impairs the function of bone marrow, suppressing the formation of white blood cells, red blood cells, and platelets (myelosuppression). Some cancer treatments are described as stomatotoxic because they have damaging effects on the oral tissues. The chart below outlines the oral complications common to both chemotherapy and radiation therapy. Charts summarizing complications specific to each type of treatment follow. It is important to consider the possibility of these complications when evaluating a cancer patient (Table 1 through Table 3).
Patients at Risk for Oral Complications
Oral complications occur in almost all patients receiving radiation for head and neck malignancies, in more than 75 percent of bone marrow transplant recipients, and in nearly 40 percent of patients receiving chemotherapy. Risk for oral complications can be classified as low or high.
Lower risk: Patients receiving mild or nonmyelosuppressive chemotherapy
Higher risk: Patients receiving stomatotoxic chemotherapy resulting in prolonged myelosuppression; patients undergoing head and neck radiation for oral, pharyngeal, and laryngeal cancer; and patients undergoing bone marrow transplantation
Some complications occur only during treatment; others, such as xerostomia, may persist for years afterward. Unfortunately, many cancer patients do not receive oral care until serious complications develop.
Oral Care Prior to Cancer Treatment
A thorough oral evaluation by a knowledgeable dental professional at least two weeks before cancer treatment begins is important to the success of the regimen. Pretreatment oral care achieves the following:
• Reduces risk and severity of oral complications
• Allows for prompt identification and treatment of existing infections or other problems
• Improves likelihood that the patient will tolerate the optimal schedule and doses of cancer treatment
• Prevents, eliminates, or reduces oral pain
• Minimizes oral infections that could lead to potentially fatal systemic infections
• Prevents or minimizes complications that compromise nutrition
• Prevents or reduces later incidence of bone necrosis
• Preserves or improves oral health
• Provides an opportunity for patient education about oral hygiene during cancer therapy
• Contributes to quality of life
With a pretreatment oral evaluation, the dental team can identify and treat problems such as infection, fractured teeth or restorations, or periodontal disease that could contribute to oral complications when cancer therapy begins. The evaluation also establishes baseline data for comparing the patient's status in subsequent examinations.
Prior to the exam, obtain the patient's cancer diagnosis, treatment plan, medical history, and dental history. In patients with hematologic cancers (such as leukemia), consult the oncologist before conducting any oral procedures; do not conduct procedures in patients who are immunosuppressed or have thrombocytopenia (low platelet count). Open communication with the patient's oncologist is essential to ensure that each provider has the information necessary to deliver the best possible care.
Pretreatment Evaluation
For the majority of cancer patients, time is a major concern in receiving this evaluation. As such, the dental team should see the patient within 24 hours of referral from the oncologist. Most oncologists assert that a delay in treatment is the main reason they do not refer their patients for a pretreatment dental evaluation.
The pretreatment evaluation includes a thorough examination of hard and soft tissues, as well as appropriate radiographs to detect possible sources of infection and pathology. Also take the following steps before cancer treatment begins:
• Identify and treat existing infections, problem teeth, and tissue injury or trauma
• Stabilize or eliminate potential sites of infection
• In adults, extract nonrestorable teeth that may pose a future problem to prevent later extraction-induced osteoradionecrosis
• Conduct a prosthodontic evaluation if indicated
• Perform oral surgery at least 2 weeks prior to the initiation of radiation therapy; For patients who will be receiving radiation treatment, this is potentially the only time to consider surgical procedures; For patients receiving chemotherapy, oral surgery should be performed 7 to 10 days before the patient becomes myelosuppressed
• In children, extract loose primary teeth and teeth that are expected to exfoliate during treatment
• Remove orthodontic bands and brackets if highly stomatotoxic chemotherapy is planned or if the appliances will be in the radiation field
• Prescribe an individualized oral hygiene regimen to minimize oral complications
• Patients undergoing head and neck radiation therapy should be instructed on the use of supplemental fluoride
Physician Consultations
Before beginning treatment, be sure to discuss the case with the patient's oncologists.
Questions for the Patient's Radiation Oncologist
• What parts of the mandible/maxilla and salivary glands are in the direct path of radiation?
• What is the total radiation dose received and possible impact to those bodily areas?
• Has the vascularity of the jaw bone been previously compromised by surgery?
• How quickly does the patient need to start radiation treatment?
• Will chemotherapy also be performed during the course of the radiation treatment?
Questions for the Patient's Medical Oncologist
• What is the patient's complete blood count, including absolute neutrophil and platelet counts?
• If an invasive dental procedure needs to be done, are clotting factors adequate?
• Does the patient have a central venous catheter?
• What is the scheduled sequence of treatments so that safe dental treatment can be planned?
Preparing the Cancer Patient for Dental Treatment
Divide dental treatment into immediate and long-term needs. Always include the patient's care giver when providing instructions on home care and recall visits.
When seeing cancer patients, try to remain positive. You can be assured that they are having a worse day than you. Remember that these patients are likely to be overwhelmed and frightened. They feel their life is out of their control. Explain to the patient that oral complications are very common and that the dental team will help them control the oral side effects of the cancer treatments. Keeping the oral cavity as healthy as possible will help alleviate pain and enhance the ability to eat.
Patient Education
Patient education is an integral part of the pretreatment evaluation. The dental team must impress on the patient the need for optimal oral hygiene during treatment, including proper care of the mouth and teeth, adequate nutrition, and the need to avoid tobacco and alcohol. To ensure that the patient fully understands what is required, provide detailed instructions on specific oral care practices, such as how and when to brush and floss, how to check for signs of complications, and other instructions appropriate for the individual. Patients should understand that good oral care minimizes oral complications and contributes to the success of cancer treatment and to their future dental health.
Recommended advice to patients:
• Gently brush teeth, gums, and tongue with an extra-soft toothbrush after every meal and before bed; If brushing hurts, soften the bristles in warm water
• Floss teeth gently every day; If gums are sore or bleeding, avoid those areas but keep flossing other teeth
• Use fluoridated toothpaste
• Follow instructions for using fluoride gel
• Don't use mouthwash that contains alcohol
• Rinse the mouth with a baking soda and salt solution, followed by a plain water rinse (Use 1/4 teaspoon of baking soda and 1/8 teaspoon of salt in 1 cup of warm water) This can be done several times a day
• To help treat mucositis, some oncologists are recommending that their patients "swish and swallow" pure honey three times a day; It is important to note that oral hygiene is extremely important as honey contains sugars that can lead to a greater risk of tooth decay
• To prevent and treat trismus (jaw stiffness), exercise the jaw muscles 3 times a day by opening and closing the mouth as far as possible (without causing pain) 20 times
• Avoid candy, gum, and soda unless they are sugar-free
• Avoid using toothpicks, tobacco products, and alcohol
• For dry mouth, sip water often, suck ice chips, and use liquids to soften or thin foods; Chew sugarless gum or suck on sugar-free candy to help stimulate saliva flow, and use a saliva substitute recommended by the dentist; Avoid lemon glycerin swabs
• Choose soft, easy-to-chew foods; Protect your mouth from spicy, sour, or crunchy foods; Take small bites of food and sip liquids while eating
• Choose lukewarm foods and drinks instead of hot or icy-cold
• To avoid enamel etching after vomiting, rinse the mouth with 1/4 teaspoon of baking soda dissolved in 1 cup of water
• Keep dentures clean by soaking in antimicrobial solutions and clean water daily
• Remove prostheses if any irritation or soreness occurs
• Request medicine from the dentist to help numb mouth pain; A rinse known as "Philadelphia Mouthwash" or "Magic Mouthwash" can be used as a topical anesthetic rinse to reduce pain; The mouth rinse is often comprised of diphenhydramine, lidocaine, Maalox®, and water; The rinse can be used every four hours to help ease oral pain
• Take a moment each day to check how your mouth looks and feels; Call your oncology and/ or radiology team if you notice any new mouth problems, if an old problem gets worse, or if you notice any changes you are not sure about including any soreness, swelling, bleeding, or a sticky white film in your mouth
Supplemental Fluoride
Rinses containing fluoride are not adequate to prevent tooth demineralization associated with radiation treatment. Instead, fluoride gel, delivered via custom gel-applicator trays, is recommended. Several days before radiation therapy begins, patients should start a daily 5-minute application of 1.1% neutral-pH sodium fluoride gel or 0.4% stannous fluoride (unflavored) gel. Patients with porcelain crowns should use a neutral-pH fluoride as other types of fluorides may damage porcelain dental work. Be sure that the trays cover all tooth structure without irritating the gingival or mucosal tissues. Patients with radiation-induced salivary gland dysfunction must continue lifelong daily fluoride applications.
Instructions for patients using supplemental fluoride:
1. Place a thin ribbon of fluoride gel in each tray
2. Place the trays on teeth and leave in place for 5 minutes; If the gel oozes out of the tray, too much is being used
3. After 5 minutes, remove the trays and spit out excess gel; Do not rinse
4. Rinse the applicator trays with water
5. Avoid eating or drinking for 30 minutes
Oral Care During Cancer Treatment
Careful monitoring of oral health is especially important during cancer therapy to prevent, detect, and treat complications as soon as possible. When treatment is necessary, consult the oncologist prior to any dental procedure, including prophylaxis.
Oral Health Monitoring
• Examine the soft tissues for mucositis (Figure 1), inflammation, or infection and check for plaque and dental caries
• Review with patients the steps to keeping the mouth moist and clean
• Provide recommendations for treating xerostomia and other complications
• Take precautions to protect against trauma
• Provide analgesics as appropriate for oral pain
Other Factors to Remember
In treating cancer-therapy patients, the following precautions also should be considered.
Schedule dental work carefully. If oral surgery is required, make sure to coordinate with the oncology team to perform treatment while allowing 7 to 10 days of healing before the patient becomes myelosuppressed. Elective oral surgery should not be performed in patients during radiation treatment.
Establish hematologic status. If the patient is receiving chemotherapy, the oncology team will conduct blood work 24 hours before dental treatment to determine whether the patient's platelet count, clotting factors, and absolute neutrophil count (ANC) are sufficient to allow oral treatment. Treatment must be postponed if the platelet count is less than 75,000/mm3, if abnormal clotting factors are present, or if the neutrophil count is less than 1,000/mm3.
Consider oral causes of fever. Fever of unknown origin may be related to an oral infection. It must be remembered that oral signs of infection or other complications may be altered by immunosuppression-related to chemotherapy.
Consider prophylactic antibiotic treatment. If the patient has a central venous catheter, consult the oncologist about implementing the American Heart Association endocarditis prophylactic antibiotic regimen before any dental treatment.
Oral Care Following Cancer Treatment
Chemotherapy
Once all complications of chemotherapy have resolved, patients may be able to resume their normal dental care schedule. If immune function continues to be compromised, the patient's hematologic status must be determined before initiating any dental treatment or surgery. This is particularly important to remember for patients undergoing a bone marrow transplant. The patient's oncologist will have the latest blood work results. The ANC number and platelet count will determine whether treatment should be attempted.
Radiation Therapy
Once the patient has completed head and neck radiation therapy and acute oral complications have abated, evaluate the patient regularly (every 4 to 8 weeks, for example) for the first 6 months. Thereafter, determine a recare schedule based on the needs of the individual. Keep in mind that oral complications can continue or emerge long after radiation therapy has ended. Patients receiving radiation therapy need to know about its risks:
Long-term risks from radiation therapy
• High-dose radiation treatment carries a life-long risk of osteoradionecrosis (ORN)
• Because of the risk of ORN, patients should avoid invasive surgical procedures, including extractions, that involve irradiated bone; If an invasive procedure is required, use of antibiotics and hyperbaric oxygen therapy prior to and following surgery should be considered
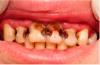
• Radiation to the head and neck may permanently reduce the quantity and quality of normal saliva; Lifelong daily fluoride application, proper nutrition, and good oral hygiene are especially important for patients with salivary gland dysfunction in order to decrease radiation caries (Figure 2)
• Dentures may need to be reconstructed if treatment has altered oral tissues; Some people can never wear dentures again because of friable (fragile, easily crushed) tissues and xerostomia
Special Considerations
Bone Marrow/Stem Cell Transplant Patients
Careful attention to oral care in the immediate and long-term post-transplant period is important to these transplant patients' overall health.
Bone marrow/stem cell transplantation causes pronounced immunosuppression, greatly increasing a patient's risk of mucositis, ulceration, hemorrhage, infection (commonly herpes simplex and Candida albicans), and xerostomia. Although the complications begin to resolve when hematologic status improves, immunosuppression may last up to a year after the transplant, along with the risk of infectious complications. Also, the oral cavity and salivary glands are commonly involved with graft-versus-host disease in allograft recipients. This can result in mucosal inflammation, mucositis, and/or xerostomia, so continued monitoring is necessary. Consult the oncologist prior to any dental procedure. Elective oral procedures should be delayed for one year.
Before the Bone Marrow Transplant
• Conduct a pretreatment oral health examination
• Consult with the oncologist about scheduling dental treatment
• Schedule oral surgery at least 7 to 10 days before expected date of myelosuppression (absolute neutrophil count [ANC] of less than 1,000/mm3 and/or platelet count of less than 75,000/mm3)
• Prevent tooth demineralization and radiation caries by instructing patient to use an in-home fluoride gel
• Instruct the patient on the proper oral hygiene regimen
After the Bone Marrow Transplant
• Watch for infections on the tongue and oral mucosa
• Monitor the patient's oral health for plaque control, tooth demineralization, dental caries, and infection
• Consult with the patient's oncologist prior to any dental procedure, including prophylaxis
• Delay elective procedures for one year
• Follow the patient for long-term oral complications
• Check the patient carefully for subsequent malignancies in the oral cavity and perioral region
Pediatric Cancer Patients
Children receiving chemotherapy and/or radiation therapy are at risk for the same oral complications as adults. Chemotherapy and radiation therapy may cause other side effects, depending on the child's age. Problems with teeth are the most common. Permanent teeth may be slow to erupt and may look different from normal teeth. Their teeth may fall out. A dentist should closely monitor children who have received radiation to craniofacial and dental structures, checking for abnormal growth and development. Prior to treatment, loose primary teeth and teeth that are expected to exfoliate during treatment should be extracted. The removal of orthodontic bands and brackets should be performed as such treatment should be delayed until cancer treatments are completed.
Summary
One in every two males and one in every three females will develop cancer in their lifetimes. Of those receiving chemotherapy, 40 to 50 percent will develop treatment-related oral side effects. Three of four people receiving bone marrow transplants will experience oral side effects. The oral health team plays an important role in the cancer patient's overall treatment plan. It is imperative that the oral health care team convey to the patient the importance of oral care prior to, during, and following cancer treatment (Table 4 and Table 5). The prevention and management of oral complications can greatly enhance a patient's chance for survival and quality of life during and after treatment. The patient is a key player in maintaining oral health during cancer treatment, but communication between all members of the cancer care team is essential in preventing and controlling painful complications from cancer treatment.
Glossary
absolute neutrophils- real number of white blood cells (WBC's) that are neutrophils (commonly called the ANC, or absolute neutrophil count)
allograft- transfer of tissue between two genetically dissimilar individuals
ANC- calculation involving the multiplication of WBC's, neutrophil segments, and band percentages; counts from 1,500 to 8,000 are considered normal
Central venous catheter- also known as a central line; surgically placed in the chest or peripherally into the upper arm to receive high doses of chemotherapy medications
dysphagia- difficulty in swallowing
functional disabilities- impaired ability to eat, speak, and swallow because of mucositis, xerostomia, trismus, or infection
Graft-versus-host- condition that results when cells from a transplant attack the cells or tissues of the recipient
hyperbaric oxygen therapy- administration of oxygen at greater than normal atmospheric pressure
immunosuppression- an abnormal condition of the immune system characterized by inhibited ability to defend against foreign substances in the body
myelosuppression- inhibition of blood cell and platelet production within the bone marrow
mucositis/stomatitis- inflammation and ulceration of the mucous membranes, which can increase the risk for pain, oral and systemic infection, and nutritional compromise
neurotoxicity- persistent, deep aching and burning pain that mimics a toothache but for which no dental or mucosal source can be found
neutrophil- type of white blood cell that helps to kill and digest microorganisms
neutropenia- severely decreased number of neutrophils making a person vulnerable to infection
osteoradionecrosis- blood vessel compromise and necrosis (tissue death) of bone exposed to high-dose radiation therapy, resulting in decreased ability to heal if traumatized and dramatically increased susceptibility to infection
platelets- cells, also known as thrombocytes, made in the bone marrow that aid in clotting
radiation caries- lifelong risk of rampant dental decay that may begin within 3 months of completing the radiation treatment
rampant dental decay and demineralization- rapid decay or erosion of the tooth's surface as a result of changes in both the quality and quantity of saliva following cancer treatment
stomatotoxic- causing damaging effects on oral tissues
thrombocytopenia- condition in which the blood has a lower than normal level of platelets; predisposing the patient to bleeding problems
trismus/tissue fibrosis- loss of elasticity of masticatory muscles that restricts normal ability to open the mouth
xerostomia/salivary gland dysfunction- dryness of the mouth because of thickened, reduced, or absent salivary flow, which increases the risk for infection and compromises speaking, chewing, and swallowing; persistent dry mouth also increases the risk for dental caries
Additional Information
The information in this course is from the awareness campaign titled "Oral Health, Cancer Care, and You: Fitting the Pieces Together," which is sponsored by the National Institute of Dental and Craniofacial Research (NIDCR) through its National Oral Health Information Clearinghouse (NOHIC). The campaign also is being conducted in partnership with the National Cancer Institute, the National Institute of Nursing Research, the Centers for Disease Control and Prevention, and the Friends of the NIDCR. Additional information and FREE patient education materials can be ordered from:
National Institute of Dental and Craniofacial Research
National Oral Health Information Clearinghouse
1 NOHIC Way
Bethesda, MD 20892-3500
1-866-232-4528
www.nidcr.nih.gov
References
American Cancer Society (2014) Cancer facts and figures 2014. Retrieved June 2, 2014, from http://www.cancer.org/research/cancerfactsstatistics/cancerfacts-figures2014/index
Calderbank DMD, S. (2005, July 14). Oral complications of cancer therapy: Treatment, diagnosis, prevention. Conference of the American Dental Assistants Association. Lecture conducted by ADAA, Washington D.C.
Motallebnajad, DDS, M., Akram, MD, S., Moghadamnia, PhD, A., Moulana, MSc, Z., Omidi, DDS, S. (2008) The effect of topical application of pure honey on radiation-induced mucositis: A randomized clinical trial. The Journal of Contemporary Dental Practice, 9 (3), 1-9.
National Institute of Dental and Craniofacial Research. (2009, September 1). Oral health, cancer care, and you. Retrieved from www.nidcr.nih.gov
Swartzentruber, L., & Bablenis Haveles, Bs Pharmacy, PharmD, (2013, December) Oral health care during chemotherapy. Dental Economics, 75-80.
Additional Readings
The National Institute of Dental and Craniofacial Research has many resources concerning this topic. Their website has a section devoted to Cancer Treatment and Oral Health. They cover the following topics:
For health professionals
- Dental Provider's Oncology Pocket Guide
- Oncology Pocket Guide to Oral Health
- Oral Complications of Cancer Treatment: What the Dental Team Can Do
For patients
- Chemotherapy and Your Mouth.
- Head and Neck Radiation Treatment and Your Mouth
- Three Good Reasons to See a Dentist BEFORE Cancer Treatment
All of this information and more can be found at: http://www.nidcr.nih.gov/OralHealth/Topics/CancerTreatment/
Acton Ph.D., Q.(2013) Xerostomia: New insights for the healthcare professional. Scholarly Editions.
Deboni, A., Giordani, A., Lopes, N., Dias, R., Segreto, R., Jensen, S., et al. (2012) Long term oral effects in patients treated with radiochemotherapy for head and neck cancer. Supportive Care in Cancer, 20, 2903-2911.
Gilliam, K. Oral health maintenance in head and neck cancer patients. RDH April (2014), 63-76.
Haas Ph.D., M.L., McBride R.N., D.L. (2011). Managing the oral effects of cancer treatment: Diagnosis to survivorship. Pittsburgh: Oncology Nursing Society.
Meurman, J., & Gronroos, L. (2010) Oral and dental healthcare of oral cancer patients: Hyposalivation, caries and infections. Oral Oncology, 46, 464-467.
Xerostomia: Helping patients with dry mouth. (2014, January 1). Retrieved June 10, 2014, from http://www.oralcancerfoundation.org/complications/xerostomia.php
About the Authors
Members of the 2001-2002 ADAA Council on Education originally developed this course. All members of the Council on Education are ADAA Active or Life Members with an interest in dental assisting education. Each one volunteers their time to the lifelong learning of dental assistants.
The 2005-2006 ADAA Council on Education updated this course.
The 2010-2011 ADAA Council on Education updated this course.
The 2013-2014 ADAA Council on Education updated this course.