You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Understanding the central role vertical dimension of occlusion (VDO) plays in oral health, including comfort, function, and esthetics, is a necessity when replacing or restoring the dentition. But what is vertical dimension? It is generally defined as the infero-superior position of the mandible to the maxilla when the teeth are in maximum contact. Maximum tooth contact (and the resulting relationship of the mandible to the maxilla) is not 1-dimensional, however. It is the 3-dimensional (3D) spatial positioning of the mandible-to-maxilla infero-superiorly, medio-laterally, and antero-posteriorly in response to muscle and tooth interaction (Figure 1).
Understanding this 3D relationship requires an intimate knowledge of the structures that make up the craniofacial complex1 and how the complex works. In the anterior, the complex encompasses the lower third of the face and the muscles of the head and neck, including the hyoid and sternocleido-mastoid muscles, to the C5 vertebral region in the posterior. As with all other complexes, the craniofacial complex describes a functioning, multipart system whose borders are connected to, interact with, and influence the functions of the body’s other complexes.
Evolution of the Craniofacial Complex
The craniofacial complex developed from saclike early animals floating in primitive seas, whose inner surface of organized cells absorbed nutrients and released waste.2-4 Folding of these sacs into tubelike organisms brought the development of specific openings for food entrance and waste elimination.5,6 The food-entering end was the beginning of the primitive craniofacial complex.
Over eons, specialized tissues arose to enhance food gathering, digestion, and elimination.7 Smell, taste, and vision formed, at least in part as attributes to provide better discrimination for food detection.8-11 Jaws, muscles, and teeth likely arose separately from the confluence of evolving ectodermal and mesodermal germ cells.12-14 They joined to form one of the first weapon systems for grasping and tearing flesh. Then, these newly associated muscles pushed the acquired food into the gullet.15 The slow process of genetic adaptation enhanced efficiency of various segments of the craniofacial complex, thereby influencing the creation or modification of other parts.
As early primates evolved to standing and walking man, neck muscles altered in size, shape, and position to help balance and swivel the head on the spinal column for better vision.16 Hominids’ teeth morphed to help digest a complex diet of meat, grain, and fruit.17,18 Speech followed, allowing more sophisticated interaction for the easier and faster location and collection of food.19-21 Tongue and teeth, the ancient organs for the manipulation of food, became integral for clearer communication and social cooperation.
Functional Components of the Craniofacial Complex: The Musculature
The craniofacial musculature of humans keeps the head balanced on the spinal column.22-24 It is the anterior and posterior muscles of the neck that primarily keeps the head from flopping side-to-side, forward, or backward. These muscles also have an intimate relationship to the muscles of mastication.25-27 If the masticatory muscles are not working harmoniously, the muscles of the neck may be affected.28
This working relationship is homeostatic; that is, these related muscle groups must maintain their internal equilibrium by adjusting their physiologic processes to work together harmoniously in a 3D environment.29-32 Poor adaptation of one muscle group may lead to the dysfunction of the other muscle group. Loss of function can lead to hypotrophy and excessive function can lead to hypertrophy.33
The stability of the muscles of mastication is maintained by the dentition.34 When the dentition is damaged or lost, and the adaptive capacity of the craniofacial musculature cannot accommodate to that loss, the complex, interdependent masticatory and neck muscles are affected. The resulting head drop reduces pharyngeal space and decreases breathing efficiency.35 Such muscular incoordination can lead to trouble breathing and tempero-mandibular dysfunction.36-39
Functional Components of the Craniofacial Complex: The Dentition
Eating
The continuing primary function of the craniofacial complex is eating. Incisors are designed to tear and molars are designed to crush to prepare foods for digestion.40 The number and amount of teeth and their contacts is central to optimal function.41-44 It comes as no surprise that the location of the greatest chewing force is in the center of the posterior biting surface, the first molars.45 In addition to eating, talking, smiling, and the way we look (to ourselves and others) are also vitally important functions, namely for social communication and cooperation.46,47
Speaking
Teeth, or their replacements, are important in producing the complex sounds that make up speech. Speech is clearer when they are appropriately placed.48 Vowels are shaped when the tongue’s borders are supported by the palatal surfaces of the maxillary posterior teeth. For many consonant sounds, the tip of the tongue is braced on the rugae or lingual surfaces of the lower anterior teeth. The fricative [f] and [v] sounds are expressed as air is forced between the incisal edges of the upper anterior teeth and the lower lip. Sibilants, the hissing [s], [sh], and the buzz of [z] are produced when air is compressed between the palatal-incisal edges of the upper front teeth, and the facial-incisal edges of the lower front teeth. Clear, distinct pronunciation is a hallmark of an intact dentition. Mushy speech is frequently a byproduct of lost teeth.49
Appearance
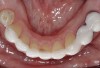
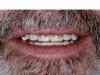
The lower third of the face is essentially described by the craniofacial complex.50,51 Facial attractiveness is strongly linked to the height of the lower third of the face,52 and damage from diseases of the jaws and teeth can be devastating. When all of the teeth are lost, the lower third of the face is decreased in height, the lips fall inward and appear thinner, and the cheeks seem hollowed out. Severe wear or damage of the teeth, especially with posterior tooth loss and the drifting of the posterior dentition, can make the lower third of the face appear “scrunched up.” The effects of lost teeth also include discomfort and pain to the mucosal tissue of the residual ridge, limited food choices, nutritional insufficiency, and muscle pain in the head and neck. 37,39,53,54 In the past, tooth loss was accepted as an unfortunate part of aging, but such loss is less tolerated today.18 Increasing height by making new dentures with proper tooth positioning and vertical dimension, or with a full-mouth rehabilitation of some kind, remarkably enhances facial attractiveness (Figure 2 and Figure 3).55 Missing, malpositioned, and dingy teeth are no longer acceptable. Poor accommodation to missing teeth, both physically and psychologically, can result in a significant decrease in a patient’s quality of life.56,57 To function comfortably today, well-positioned, well-shaped, and appropriately shaded teeth or their replacements are a social necessity.58
Muscle/Dentition Interaction
A healthy dentition is also the foundation for healthy muscle function of the craniofacial complex. Teeth and the muscles of the head and neck develop and adapt together from birth. Teeth provide the normal “door stop” for contraction of the muscles of mastication. Limits on the contraction of most other muscles are a result of muscle bulk or ligamental restrictions. If all of the teeth are lost, the muscles of mastication may overclose the jaw.59 Overclosure results in head droop, downcast eyes, and a decrease in pharyngeal space.60,61
To see better and breathe easier, the posterior muscles of the neck contract to pull the head up. Hypertonicity of the posterior muscles of the neck and stretching of the anterior neck muscles are the result. Such overcompensated contraction and stretching may lead to muscle tenderness and fatigue. With the dentition as the natural limit of contraction, the masticatory muscles help maintain normal balancing tonicity of the muscles of the neck to keep the head balanced properly on the spine. Indeed, research on posture,62,63 gait,64,65 and even acuity of sight66 has been related to a proper dental occlusion.
The inclined planes of the teeth along with the ligaments of the temperomandibular joint keep the joints in homeostatic positions in the glenoid fossae.67 Damage to individual or multiple teeth from disease, tooth restoration, orthodontic treatment, or wear, as well as the loss of individual or multiple teeth unilaterally or bilaterally, can mean a potential change in the muscular “stop” on one or both sides.68 With such loss, the medial and lateral pterygoids, masseter, and temporalis muscles may become hypertonic or hypotonic and relocate condyles laterally or up and back, invading the retro-discal or latero-discal space.69,70 If teeth are lost, tilted, or more worn on one side, the change in tooth contact changes the unilateral vertical dimension on that side. Change in tonicity of the muscles that have no teeth to limit contraction can lead to their fatigue, spasm, and soreness.70,71
In animal studies, muscle damage can be temporary or even permanent depending on the amount of time from tooth structure loss.72,73 Muscle “imbalances” from complete or partial tooth loss, or possible disc space inflammation from tooth loss, have been implicated in the etiology of tempero-mandibular disorders.74 A healthy dentition maintains all of the 3D vectors of vertical dimension: the antero-posterior, medio-lateral, and infero-superior 3D positions75,76 needed for muscular balance.
Tooth Contacts in Maximum Intercuspal Position and Lateral Excursions
The craniofacial complex musculature is robust,39,77 and like most other body complex components, can withstand minor, and sometimes major, insults before actual dysfunction occurs. Maintaining a healthy dentition is the best way to maintain healthy muscle homeostasis and thus maintain the three vectors of vertical dimension. The prevention of caries and periodontal disease to keep the dentition intact is the first priority for the healthy relationship of the mandible to the maxilla.
Static Occlusal Contact
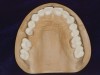
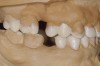
Loss of tooth contact or near contact78,79 on one quadrant of the mouth has the potential for dysfunction and perhaps even lasting damage to the musculature, not just on the noncontact side, but on both sides.80 Tooth contact during maximal force chewing is the same as in static maximum force intercuspal contact,81 indicating the role stable functional tooth contacts play in optimal muscle function. However, not all of the teeth have contact in maximum intercuspation.82,83 Moreover, most of the contacts that do occur are in the molar region, and, not surprisingly, the greatest forces of contact are also found posteriorly (Figure 4).84 It can be inferred that one of the functions of the posterior teeth is to hold the infero-superior component of vertical dimension, and in some cases (ie, group function), the medio-lateral vector as well.
Lateral Excursive Contacts
Medio-lateral contact is often referred to as lateral excursive guidance. There is no preferred lateral excursive occlusal scheme, although there seems to be a tendency toward canine guidance in young adults.85-87 Canine guidance, group function, and even bilateral occlusal contact (bilateral balance) are seen in healthy dentitions in which there are no signs or symptoms of temporomandibular disorders.88
Restoring the medio-lateral vector of the maxilla-mandible relationship depends on whether or not the existing relationship is problematic. In general, if there are no pathologies diagnosed, then no change in the lateral excursive contact relationships should be considered.89
Protrusive Guidance
Protrusive guidance—the lower incisors sliding against the upper incisors forward to the incisal edges from maximum intercuspation—is not actually a functioning movement of the mandible. The incisors are configured to begin the process of eating by coming together for grasping, shearing, and tearing food90,91 before the molars and premolars smash and mix the pieces with saliva for easier swallowing.
The incisors meet in incision and frequently during chewing movements107; however, the “idea” of protrusive guidance is a very useful articulator convenience. It provides for the creation of a functioning occlusion by developing those lateral and protrusive guidances in which there is minimal chance of interference during function between the posterior teeth and the anterior teeth. Articulator movement does not perfectly mimic intraoral function, but careful use of this instrument can reduce the chances of inappropriate contacts during chewing.92,93
It should be noted that in restoration of the anterior teeth, an attempt should be made to ensure even contact of restored incisal edges over more than one tooth. Such sharing of contact force spreads the forces over a greater surface area and reduces the stresses on the restorative materials during that first incisional contact.
Bilateral Simultaneous Contact
Aside from the importance laid on the development of tooth guidance during function, the most important single criterion for a healthy dentition is bilateral simultaneous contact. The second is even, gliding movements of the teeth when functioning in lateral contact.94-96
Restoring Contacts with Minimal Tooth Damage
Maximum intercuspal position is the jaw relationship with which to develop occlusal contacts on single-tooth restorations. Thus, when tooth damage or loss occurs, it is sensible that the restoration of missing parts of the teeth should provide similar, if not exact, occlusal stops.83,97,98
Infero-Superior Vector of Vertical Dimension
Single Intracoronal Restorations
The traditionally taught idea that every restored tooth must have an occlusal contact—even if no contact existed previously—is not always valid. Replacing an occlusal contact that actually did exist should always be attempted, especially if that contact is the only contact, is one of two to three contacts, or is a molar contact in a quadrant. Restoring a contact with an amalgam or composite restoration can be done with careful evaluation of both the pre- and post-insertion occlusion.
Many approaches have been used to identify tooth contacts and, unfortunately, none are totally satisfactory.99 The use of thin articulating paper to first identify the preoperative contact and then the postoperative contact, though seemingly time consuming, is most appropriate and reasonably successful.100 The “cut them low and let them grow” idea is not appropriate.101
Contacts for Single-Tooth Full- or Partial-Coverage Restorations
It is more difficult to determine where and how many contacts should be made for full-coverage restorations. Often the tooth or teeth are damaged to the point that it would be impossible to know the contacts. However, wear facets on opposing teeth can provide an indication of the contacts in maximum intercuspal position and/or lateral excursions.
Well-written directions for the dental laboratory can be helpful in achieving the goal of maintaining the existing contacts by prescribing a crown whose contours match the opposing wear facets in some contact positions, whether in maximum intercuspal position or lateral contact. In fact, digital applications in dentistry are becoming more sophisticated in constructing crowns to do just that. The manufacture of computer-aided designed/computer-aided manufactured crowns can produce good results for occlusion in maximum intercuspal position and lateral excursive contacts as well as for providing good esthetics.102
Occlusal adjustment is often necessary for computer-produced or traditionally fabricated crowns.103,104 Adjustments can be accomplished with any number of techniques and materials, depending on the preference of the practitioner, including wax, digital sensor, inked paper, or plastic film.105 The objective is the same: to determine the contacts that will create as closely as possible those occlusal interactions that maintain the 3-dimensionality of VDO.106,107 Because the predominance of posterior contacts is on the first molars, followed by the second molars and the second premolars, it is generally appropriate to restore contacts on these teeth unless they had none previously.
Complete Prosthodontic Reconstruction
Recreating an entire occlusion from severely damaged or worn dentition is one of the great challenges in dentistry. The ultimate challenge is when all of the teeth are lost and complete dentures or implant-retained prostheses must be made.108 The functional criteria to achieve the quality-of-life objectives for either tooth-retained fixed prosthodontics, implant-retained prosthodontics, or removable prosthodontics are similar: create acceptable appearance; ensure satisfactory speech, comfortable incision, and chewing; and provide stable occlusal contacts to which the muscles of the craniofacial complex can adapt.
This can be achieved by finding the most reliable and stable jaw relationships from which to create the occlusion, determining acceptable esthetics, and developing an appropriate 3D VDO. VDO can be developed by establishing stable, bilaterally simultaneous intercuspal static contacts in maximum intercuspal position to ensure muscle homeostasis for the 3D relationship between the maxilla and mandible and by determining lateral stability of functional incisional and chewing contacts that will provide for acceptable muscle adaptation.
Centric Relation: A Starting Point for Full-Mouth Reconstruction
The majority of dentists have been taught to reconstruct the dentition beginning in centric relation. The debate over centric relation position (also referred to as reference position or retruded contact position) continues,109,110 but the literature presently seems to regard this guided position as the most practical and reliable to obtain and record and as the preferred starting point from which to develop a reconstructed dentition. The reliability of recording this guided position is likely muscle dependent, however.111
Mandibular Functional Position
Studies on normal dentition indicate that its function does not coincide with centric relation.69 The reason for this is unknown, but function seems to occur between centric relation and 1.0 mm to 1.5 mm anterior and/or lateral to the centric relation contact.112 If the condyles do translate slightly down and forward during function, the mandible will rotate forward and upward, producing fewer tooth contacts in the molar region and more contacts on the premolar and anterior teeth (Figure 5). The presence of solid, stable contacts and near contacts on the posterior teeth, especially the molars, is associated with the most efficient chewing and comfort.113,114 Creating a centric relation reconstruction on the articulator with precise (or holding) contacts on both the anterior and the posterior teeth can “lock in” the occlusion in a posterior position. The anterior contacts may then serve to force the jaw back, thus functioning in a space that is not optimal and uncomfortable.115
The resiliency of many individual’s muscles and joints might ultimately adapt to nonoptimal static contact or near contact in the posterior dentition if the wear of materials and/or movement and the wear of teeth ultimately provide for more and stable occlusal posterior contacts. However, it is better to provide those stable contacts initially in the final reconstruction. Care in assessing posterior occlusal contacts on the restorations must be made both in the laboratory phase as well as at insertion of the prosthesis. Evaluating static contacts intraorally using the approaches with which the practitioner is most comfortable (eg, computer sensor, wax, inked articulating paper, or films) is very important before final cementation or insertion of the reconstruction.116,117
Establishing sound posterior contacts or near contacts in the posterior occlusion as well as minimal contacts in the anterior occlusion are important final adjustments to produce a successful outcome. Unfortunately, there is no good information on the long-term reliability of recreating occlusions using any of the currently available techniques and instrumentation. For orthodontically or prosthetically reconstructed dentitions developed in centric relation, the discussion continues about when, if, and for how long function in centric position may occur. Long-term follow-up studies in orthodontics and prosthodontics are needed to help forward an evidence-based discussion.118
Diagnosis and Treatment Planning
Information on past and present medical and dental status is necessary before beginning a treatment plan. Treatment type and length of treatment all depend on a thorough patient assessment. Special attention to existing occlusal-related problems or damage is especially important in creating an adaptable 3D VDO for appearance, comfort, and function.
Intraoral and Extraoral Examination
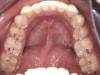
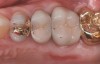
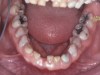
Loss of vertical dimension can be assessed through patient examination intraorally, extraorally, and functionally. Missing teeth and/or teeth worn from clenching or bruxing are the most common intraoral signs of a decreased VDO. Congenitally missing teeth can result in loss of vertical dimension with possible implications of compromised comfort, speech, and chewing (Figure 6 through Figure 8).
Pursing of the lips to make the fricative [f] and [v] or sibilant [s] or [z] sounds is another indication of loss of VDO. Tooth wear, old or poorly constructed dentures, full-mouth rehabilitations, or orthodontics that did not properly develop 3D VDO can result in both function and appearance problems.119
Radiographic Information for VDO
Pre-existing records are valuable in assessing current VDO if changes in vertical dimension are contemplated.120 Conventional periapical and panographic X-rays assess most damage to the dentition and the supporting structures in the jaws. Cephalometric information helps determine vertical dimension and is a well-established technique.121 This information alone cannot provide tooth position for any individual’s functional characteristics, however, particularly in terms of appearance or speech. For such information, testing of these specifics is necessary.122
Morphologic Information for VDO: Mounted Study Casts
Mounted study casts are needed as the first step in providing current evidence of the state of the dentition and will provide a platform from which to develop the basis for the reconstruction.123
When many or most teeth are present, regardless of damage, they provide invaluable information on existing tooth position and contacts, tissue contours, and esthetic concerns. If all or most of the teeth are lost, mounted study casts provide greater visualization of the damage to the remaining teeth or contours and the amount of residual tissues. They are also needed to create diagnostic wax-ups and set-ups of denture teeth to begin testing the esthetics and speech functionality of an appropriate 3D VDO.
Facebow and Centric Relation
Study casts should be mounted in centric relation with a facebow. A facebow transfer shows antero-posterior and medio-lateral occlusal plane inclinations and a reasonably accurate relationship of the maxillary arch to the rotational axis of the condyles (Figure 9 and Figure 10).124,125 Thus the arc of closure of the mandible in centric relation on the articulator is close to that of the mouth. During articulator closure or movement, existing tooth contacts on inclined planes can be observed. Based on such information, decisions can be made regarding how initial tooth contact will be used in the reconstruction.
Because the posterior bar of many articulators is parallel to the “floor,” it is a convenient reference to set the lower anterior teeth so that the incisal edges will close perpendicular to the line of the bar. Closure perpendicular to the lower and upper incisal edges produces efficient incisional/shearing contact (Figure 11 and Figure 12).
Centric relation is perhaps best found after deprogramming the jaw’s muscles with either an anterior deprograming method such as a Lucia jig or, if long-term deprogramming is desired, with a mouth guard.126 All specific techniques for recording centric relation have advocates, but no one technique fits all circumstances.127 Whichever technique is comfortable and provides the reliability that the practitioner desires is the best choice.128,129
Determining the 3D VDO
For decades, there has been concern about increasing a patient’s existing VDO, even if that vertical dimension has become decreased because of trauma, severe tooth wear, or complete or partial edentulousness. Yet, there is no doubt that increasing a patient’s current vertical dimension will do no harm and will likely have great benefit to the patient’s oral health–related quality of life.22,130-132
Cephalometry
Cephalometric analysis has long been used in orthodontics to provide a statistically oriented approach to determining vertical dimension.133 Much data have been developed for both children and adults, and long-term excellent results for establishing the length of the lower facial are well established. This approach has been used in prosthodontic research and now more frequently in prosthodontic treatments.122,134
Sounds of Speech in Determining VDO
There is a functional VDO for speech that is created when teeth, lips, palate, and the tongue interact to form sounds. The position of the teeth in relation to supporting the upper and lower lips and the positions of the posterior and anterior teeth in relation to the tongue, palate, and each other are important in the production of the consonants and vowel sounds we all make during speech.49
Speech generally begins when the mandible is at rest with the muscles of the jaw in a state of relaxation with the lips touching. This relaxed muscular state, the vertical dimension of rest, creates a space between the upper and lower teeth called the freeway space or closest speaking space, which is generally between 2 mm and 4 mm in the vertical plane. This is also approximately the distance between the teeth when the sibilant sounds are made. There is no preferred method of determining closest speaking space,135,136 but the development of certain functional sounds is useful for determining what is appropriate for each patient.
The [m] sound is often the first sound used in determining vertical dimension of rest/freeway space. The [m] sound creates a relaxed muscular space in which speech can begin without interference of the dentition. It is made with the muscles relaxed and lips touching. The [m] sound is then voiced, usually by pronouncing the name “Emma,” words such as “mother” or “most,” or by making a humming sound. When the lips are parted after the [m] sound is made, there should be approximately 2 mm to 4 mm of space between the upper and lower teeth.
The plosive [b] and [p] sounds are made with the lips closed but are made most clearly when supported by the upper and lower anterior teeth. Without the teeth supporting the lips, the plosives sound “flabby,” as the lips cannot make an initial tight seal.
An appropriate position of the upper anterior teeth to the lower lip is needed to make the fricative [f] and [v] sounds. These are made when the upper anterior teeth touch the wet/dry border of the lower lip.137 Clear sibilant [s] and [z] sounds are made when the lower and upper incisal edges almost touch, allowing on a clear hissing sound to be produced.138 Posterior teeth should have sufficient freeway space between them when the sibilants are made. Dentures made with too great an increase in infero-superior vertical dimension will touch or “click” together when speaking words that contain sibilants.
Most consonant sounds are made when the tip of the tongue interacts with the palatal surfaces of the upper anterior teeth and rugae, and/or with the lingual inclines of the lower anterior teeth. The rolling [r] develops with the tongue again braced on the maxillary posterior teeth and junction of the hard and soft palate and the sounded “rrrr” is made with the center of the tongue open. The hard [k] and [q] and softer [ch] are made with the tongue braced on the palatal surfaces of the maxillary posteriors and posterior hard palate, and then the center of the tongue quickly released with a click and rush of air from the pharynx. All clear vowel sounds occur when the lateral border of the tongue is braced on the palatal surfaces of the maxillary posterior teeth.139
Appearance
A way of developing infero-superior vertical dimension clinically is to evaluate the “golden proportion”—the proportion of the lower third of the face to the upper two thirds of the face and facial width proportions.140 One approach to estimate this is cephalometrics.141,142 Another is to measure certain facial dimensions.
The measurement between the outer canthus of the eye and the external auditory meatus is one measurement needed, and the measurement between the pupils143 or between one pupil and the internal canthus of the other eye is another. Another approach long used with good success to evaluate vertical dimension is taking the measurement between two dots, one on the chin and the other on the nose when the patient’s jaws are at rest and the lips barely touching but teeth not touching, and then subtracting 2 mm to 3 mm (Figure 13). Speech function and facial proportions provide good starting points for determining the infero-superior vector of vertical dimension.144
Measurements are often used as a initial starting point for vertical dimension and are checked against speech and/or cephalometrics to develop a more thorough approach for establishing a functional and esthetic VDO for the individual patient. Variation in vertical dimension occurs between individuals as well as among races. For this reason, it is appropriate to evaluate cephalometric studies for differences within and between racial groups, especially for races that differ from European norms.
The positions of all teeth are extremely important for socially acceptable appearance and clear creation of the sounds of speech.145 Getting it right will take a little bit of work in positioning the teeth to satisfactorily create esthetic and functional tooth and tissue relationships.
Diagnostic Wax-Ups and Set-Ups
One of the most valuable ways to assess vertical dimension is to use wax-ups to create mock overlays to test clear speech for an appropriate vertical dimension (Figure 14 and Figure 15). When anterior diagnostic acrylic or composite overlays (or “mock veneers”) are used to test fricatives, clear [f] and [v] sounds are made when the incisal edges of the maxillary teeth touch just inside the wet/dry border of the lower lip. Clear sibilant [s] and [z] sounds occur when the lower and upper incisal edges almost touch, allowing a clear hissing sound to be made. Improved esthetics is also dramatic. Once these sounds are clear, the closest speaking space can be created with diagnostic wax-ups in the posterior space (Figure 16 through Figure 19). The final result will depend on successful development of 3D VDO comparing a number of methodologies.
When most or the entirety of the dentition is missing, denture tooth set-ups most frequently develop the esthetics and tooth position best suited for the individual patient. When a fixed implant-retained prosthesis is planned146 instead of a conventional removable prosthesis set-up with a flange to support the lips and cheeks, however, there will be no flange for soft tissue support or for deflecting food into the buccal sulcus. This problem provides an opportunity as well as a challenge. The challenge is producing size, shape, shade, and tooth position that are acceptable without a flange. The opportunity is to clearly communicate with the patient the limitations to esthetics, speech, and comfort that inevitably occur when all teeth are lost.147
The decided-upon wax-up/set-up also becomes a blueprint for the reconstruction. Implant placement is optimized when a surgical template is made from the set-up. A provisional prosthesis can also be fabricated from this diagnostic set-up, as the vertical dimension has been tested with the diagnostic set-up for speech and the esthetics of lip support (Figure 20 and Figure 21). When implant placement is closely related to the planned prosthodontic design, it is much easier to achieve realistic patient outcomes.
Informed Consent
It is extremely important to obtain informed consent for all treatments, but particularly for those in which a considerable investment in time, emotion, and money are involved. Unfortunately, it is nearly impossible to recreate even with the best prosthodontic procedures what once “grew there,” and the amount of damage from trauma or disease largely determines the level of esthetics, comfort, and function obtainable.148 Informed consent is a patient’s right, and whatever treatments are realistic should be placed in writing. Facing considerable time and expense for treatment, patients often stop listening when, or if, anxiety becomes the prominent emotion. A written informed consent provides information for study after verbal communication. A detailed discussion of logistics can occur at another appointment, making treatment easier for the patient and the doctor. Trust is established during such communication and, if subsequent problems occur or the final result is not what was expected, fear and anger are mitigated. Disappointments in treatment are generally accepted well if there is discussion of realistic results.149
Prosthodontic Techniques
Intermaxillary Relationships
As previously described, a centric relation record using any technique comfortable to the dentist is most likely to ensure simultaneous contact of both the unreconstructed and reconstructed sides.127,150 If the replacement teeth come together harmoniously, most treatment goals for occlusion are pretty much accomplished.
Provisionalization
Testing patient adaptation with a provisional prosthesis provides information on tooth position for the final prosthesis151 and, most importantly, vertical dimension.152 If a substantial increase in vertical dimension is made, up to 3 months using the provisional prosthesis for assessing and making needed modifications on the provisional would be appropriate.153 Testing esthetics, eating, speaking, and comfort vis-à-vis the tongue, lip, and cheek can be accomplished before the final prosthesis is completed.154 The diagnostic set-up/wax-up can be used as a template for the provisional.155 If temporization is decided upon, a laboratory-processed provisional may be relined on temporary or final abutments.
If the provisional restoration meets all or most of the occlusal functional parameters, an impression and photographs of these provisional restorations should be made, and the casts, preferably mounted in centric relation and with a facebow, are sent along with the mounted final casts so the laboratory technician has a pattern for developing the plane of occlusion, esthetic placement of the anterior teeth, and centric and lateral contacts of the final restoration.156 The photographs assist the lab in determining the overall shape and shade coordination needed for the patient.
Insertion of the Prosthesis
Three key indicators should be evaluated at prosthetic insertion: occlusal contacts, esthetics, and comfort. Even with meticulous records, it will be necessary for occlusal adjustment at the insertion of the prosthesis.157 As long as occlusal contacts are solid, bilateral, and simultaneous with a generally even distribution on each side, it is best to avoid the temptation to adjust the occlusion to “completion” at this time.
The most important measure of the restoration’s functionality is chewing, and the factor most associated with efficient and comfortable chewing is contact on the posterior teeth, especially the first molars.158-160 Thus, ensuring sound contacts on the molars is one of the more important adjustments that must be made before insertion of the final restoration. A lack of or minimal contacts on the anterior teeth provide for some slight anterior rotation of the mandible if function anterior to centric relation occurs.
Adjusting the palatal surfaces of the incisors to achieve comfortable incision should also be accomplished at this time. Muscle adaptation to the newly restored bilateral 3D VDO may require some time, especially with a new material such as metal or porcelain that will have different perception characteristics from acrylic provisional restorations.161 Adjusting the contacts 1 to 4 weeks after they appear stable is advised.162 Certainly if the patient feels discomfort, minor adjustments are necessary at any time.
Implant-Supported Reconstruction
Dental implant retention for complete maxillary and mandibular reconstructions has been a great help for patients who have suffered with complete dentures. When the reconstruction is partly or completely implant retained, the phenomenon of osseoperception163 helps redevelop adequate muscular function.164 Patients can identify stress applied to dental implants similarly to the forces applied to the natural dentition.165 The mechanism is not perfectly understood, but evidence strongly suggests it is the central nervous system that recognizes stresses in the jaws as similar to the proprioceptive impulses from the teeth. This may be the central nervous system processing jaw stress information and relating that information to the habituated patterns of muscular function.
Indeed, muscle function may not be totally dependent on proprioception from the periodontal ligament.166 The relative success of complete dentures is an example.167 However, control of jaw function seems to be similar with the natural dentition or with prosthetic reconstructions on dental implants.
It is most often necessary to make a new set of complete dentures to test the 3D VDO and the parameters of appearance, comfort, and function that result form complete maxillary and mandibular implant reconstructions. Speech is usually not adapted immediately. Within a few days or weeks, however, the majority of patients have adapted to their prostheses. This denture prosthesis (or prostheses) can also be used to create provisional prostheses on the uncovered implants for further evaluation of the above parameters. This is especially needed when immediately loaded implants are planned.168,169
The restoration of acceptable or better esthetics and function with an implant-retained prosthesis will always help the patient better accept the needed after-restoration adjustments.
Conclusion
Loss or damage to teeth decreases a patient’s ability to function socially or biologically. To some, a tooth lost is just part of living; to others, it is an amputation and a very difficult adjustment to make. Sympathetic, yet very realistic, appraisal and communication of the treatment and possible outcomes for both the short- and long-term outcomes of any restoration is strongly advised. Even with today’s prosthodontic and implant reconstruction techniques, it is still impossible to bring back the entire functionality, esthetics, and comfort that have been lost. However, knowledge about the craniofacial complex and how damage to its function can be appropriately treated can dramatically increase the oral health related quality of life of patients.
To this end, it is crucial to have a thorough understanding the role vertical dimension plays in treatment this complex. There is no completely accurate or foolproof method of determining vertical dimension.170 Clinical judgment based on comparing and even melding different techniques is a reasonable approach. Input from the patient is crucial. If the patient is comfortable with the planned vertical dimension during speech and chewing with wax set-ups or provisional restorations, then it is likely the most appropriate one. If the patient is not comfortable, then careful thought and planning must be given to providing the 3D VDO the patient will tolerate.
Creating a 3D VDO using approaches that reflect the functionality of esthetics, the functions of speech and eating, and which positively interacts with other of the body’s complexes, will provide restorations that maintain or enhance patients’ long- and short-term quality of life.
References
1. Chapter 2: The Craniofacial Complex. National Institute of Dental and Craniofacial Research website. www.nidcr.nih.gov/DataStatistics/SurgeonGeneral/sgr/chap2.htm. Accessed May 25, 2011.
2. Morris VB. Origins of radial symmetry identified in an echinoderm during adult development and the inferred axes of ancestral bilateral symmetry. Proc Biol Sci. 2007;274(1617):1511-1516.
3. Morris VB. Early development of coelomic structures in an echinoderm larva and a similarity with coelomic structures in a chordate embryo [published online ahead of print Sept 22 2012]. Dev Genes Evol. 2012;222(6):313-323.
4. Maxmen, A. Evolution: a can of worms. Nature. 2011;470(7333):161-162.
5. Potts WT. The physiological function of the coelom in starfish larvae and its evolutionary implications. Physiol Biochem Zool. 2003;76(6):771-775.
6. Morris SC, Caron JB. Pikaia gracilens Walcott, a stem-group chordate from the Middle Cambrian of British Columbia. Biol Rev Camb Philos Soc. 2012;87(2):480-512.
7. Gillis JA, Fritzenwanker JH, Lowe CJ. A stem-deuterostome origin of the vertebrate pharyngeal transcriptional network [published online ahead of print Jun 15 2011]. Proc Biol Sci. 2012;279(1727):237-246.
8. Jacobs LF. From chemotaxis to the cognitive map: the function of olfaction [published online ahead of print Jun 20 2012]. Proc Natl Acad Sci U S A. 2012;109(suppl 1):S10693-S10700.
9. Barreiro-Iglesias A, Anadón R, Rodicio MC. The gustatory system of lampreys. Brain Behav Evol. 2010;75(4):241-250.
10. Hering L, Henze MJ, Kohler M, et al. Opsins in onychophora (velvet worms) suggest a single origin and subsequent diversification of visual pigments in arthropods. Mol Biol Evol. 2012;29(11):3451-3458.
11. Cronin TW, Porter ML, Bok MJ, et al. The molecular genetics and evolution of colour and polarization vision in stomatopod crustaceans. Ophthalmic Physiol Opt. 2010;30(5):460-469.
12. Graham A. Deconstructing the pharyngeal metamere. J Exp Zool B Mol Dev Evol. 2008;310(4):336-344.
13. Heude E, Bouhali K, Kurihara Y, et al. Jaw muscularization requires Dlx expression by cranial neural crest cells [published online ahead of print Jun 7 2010]. Proc Natl Acad Sci U S A. 2010;107(25):11441-11446.
14. Fraser GJ, Hulsey CD, Bloomquist RF, et al. An ancient gene network is co-opted for teeth on old and new jaws. PLoS Biol. 2009;7(2):e31.
15. Anderson PS. Using linkage models to explore skull kinematic diversity and functional convergence in arthrodire placoderms. J Morphol. 2010;271(8):990-1005.
16. Crawford JD, Ceylan MZ, Klier EM, Guitton D. Three-dimensional eye-head coordination during gaze saccades in the primate. J Neurophysiol. 1999;81(4):1760-1782.
17. Ungar PS, Sponheimer M. The diets of early hominins. Science. 2011;334(6053):190-193.
18. Gibbons A. Evolutionary biology. An evolutionary theory of dentistry. Science. 2012;336(6084):973-975.
19. Lameira AR, Hardus ME, Wich SA. Orangutan instrumental gesture-calls: reconciling acoustic and gestural speech evolution models. Evol Biol. 2012;39(3):415-418.
20. Sterelny K. Language, gesture, skill: the co-evolutionary foundations of language. Philos Trans R Soc Lond B Biol Sci. 2012;367(1599):2141-2151.
21. Aboitiz F, García R. Merging of phonological and gestural circuits in early language evolution. Rev Neurosci. 2009;20(1):71-84.
22. al-Abbasi H, Mehta NR, Forgione AG, Clark RE. The effect of vertical dimension and mandibular position on isometric strength of the cervical flexors. Cranio. 1999;17(2):85-92.
23. Wakano S, Takeda T, Nakajima K, et al. Effect of experimental horizontal mandibular deviation on dynamic balance. J Prosthodont Res. 2011;55(4):228-233.
24. Koolstra JH, van Eijden TM. Functional significance of the coupling between head and jaw movements. J Biomech. 2004;37(9):1387-1392.
25. Zafar H. Integrated jaw and neck function in man. Studies of mandibular and head-neck movements during jaw opening-closing tasks. Swed Dent J Suppl. 2000;(143):1-41.
26. Kondo E, Aoba TJ. Case report of malocclusion with abnormal head posture and TMJ symptoms. Am J Orthod Dentofacial Orthop. 1999;116(5):481-493.
27. Kondo E. Features and treatment of skeletal class III malocclusion with severe lateral mandibular shift and asymmetric vertical dimension. World J Orthod. 2004;5(1):9-24.
28. Gillies GT, Christy DW, Stenger JM, Broaddus WC. Equilibrium and non-equilibrium dynamics of the cranio-mandibular complex and cervical spine. J Med Eng Technol. 2003;27(1):32-40.
29. Van Eijden TM, Korfage JA, Brugman P. Architecture of the human jaw-closing and jaw-opening muscles. Anat Rec. 1997;248(3):464-474.
30. Murray GM, Peck CC. Orofacial pain and jaw muscle activity: a new model. J Orofac Pain. 2007;21(4):263-278.
31. Rues S, Lenz J, Türp JC, et al. Muscle and joint forces under variable equilibrium states of the mandible. Clin Oral Investig. 2011;15(5):737-747.
32. Hattori Y, Satoh C, Seki S, et al. Occlusal and TMJ loads in subjects with experimentally shortened dental arches. J Dent Res. 2003;82(7):532-536.
33. Fitts RH, Riley DR, Widrick JJ. Functional and structural adaptations of skeletal muscle to microgravity. J Exp Biol. 2001;204(pt 18):3201-3208.
34. Narita N, Kamiya K, Yamamura K, et al. Chewing-related prefrontal cortex activation while wearing partial denture prosthesis: pilot study. J Prosthodont Res. 2009;53(3):126-135.
35. Bucca C, Cicolin A, Brussino L, et al. Tooth loss and obstructive sleep apnoea. Respir Res. 2006 Jan 17;7:8.
36. Dulci? N, Panduri? J, Kraljevi? S, et al. Incidence of temperomandibular disorders at tooth loss in the supporting zones. Coll Antropol. 2003;27(suppl 2):S61-S67.
37. Casanova-Rosado JF, Medina-Solís CE, Vallejos-Sánchez AA, et al. Prevalence and associated factors for temporomandibular disorders in a group of Mexican adolescents and youth adults. Clin Oral Investig. 2006;10(1):42-49.
38. Schmitter M, Balke Z, Hassel A, et al. The prevalence of myofascial pain and its association with occlusal factors in a threshold country non-patient population [published online ahead of print Apr 5 2007]. Clin Oral Investig. 2007;11(3):277-281.
39. Wang MQ, Xue F, He JJ, et al. Missing posterior teeth and risk of temporomandibular disorders. J Dent Res. 2009;88(10):942-945.
40. Tumrasvin W, Fueki K, Ohyama T. Factors associated with masticatory performance in unilateral distal extension removable partial denture patients. J Prosthodont. 2006;15(1):25-31.
41. Osterberg T, Mellström D, Sundh V. Dental health and functional ageing. A study of 70-year-old people. Community Dent Oral Epidemiol. 1990;18(6):313-318.
42. Tatematsu M, Mori T, Kawaguchi T, et al. Masticatory performance in 80-year-old individuals. Gerodontology. 2004;21(2):112-119.
43. Gotfredsen K, Walls AW. What dentition assures oral function? Clin Oral Implants Res. 2007;18(suppl 3):S34-S45.
44. Nakatsuka Y, Yamashita S, Nimura H, et al. Location of main occluding areas and masticatory ability in patients with reduced occlusal support. Aust Dent J. 2010;55(1):45-50.
45. Ikebe K, Matsuda K, Murai S, et al. Validation of the Eichner index in relation to occlusal force and masticatory performance. Int J Prosthodont. 2010;23(6):521-524.
46. Freeberg TM, Dunbar RI, Ord TJ. Social complexity as a proximate and ultimate factor in communicative complexity. Philos Trans R Soc Lond B Biol Sci. 2012;367(1597):1785-1801.
47. Saintrain MV, de Souza EH. Impact of tooth loss on the quality of life. Gerodontology. 2012;29(2):e632-e636.
48. Rodrigues LC, Pegoraro LF, Brasolotto AG, et al. Speech in different oral prosthetic rehabilitation modalities for elderly individuals. Pro Fono. 2010;22(2):151-157.
49. Rosenberg D, Kaplan S, Senie R, Badner V. Relationships among dental functional status, clinical dental measures, and generic health measures. J Dent Educ. 988;52(11):653-657.
50. Ricketts RM. The biologic significance of the divine proportion and Fibonacci series. Am J Orthod. 1982;81(5):351-370.
51. Ferring V, Pancherz H. Divine proportions in the growing face. Am J Orthod Dentofacial Orthop. 2008;134(4):472-479.
52. Knight H, Keith O. Ranking facial attractiveness. Eur J Orthod. 2005;27(4):340-348.
53. Mohindra NK, Bulman JS. The effect of increasing vertical dimension of occlusion on facial aesthetics. Br Dent J. 2002;192(3):164-168.
54. Fueki K, Igarashi Y, Maeda Y, et al. Factors related to prosthetic restoration in patients with shortened dental arches: a multicentre study. J Oral Rehabil. 011;38(7):525-532.
55. Yamashita S, Sakai S, Hatch JP, et al. Relationship between oral function and occlusal support in denture wearers. J Oral Rehabil. 2000;27(10):881-886.
56. Knipfer C, Bocklet T, Noeth E, et al. Speech intelligibility enhancement through maxillary dental rehabilitation with telescopic prostheses and complete dentures: a prospective study using automatic, computer-based speech analysis. Int J Prosthodont. 2012;25(1):24-32.
57. Niesten D, van Mourik K, van der Sanden W. The impact of having natural teeth on the QoL of frail dentulous older people. A qualitative study. BMC Public Health. 2012;12(1):839.
58. Henson ST, Lindauer SJ, Gardner WG, et al. Influence of dental esthetics on social perceptions of adolescents judged by peers. Am J Orthod Dentofacial Orthop. 2011;140(3):389-395.
59. Kovats JJ. Overclosure of the jaws: a clinical syndrome. J Prosthet Dent. 1967;18(4):311-315.
60. Wang MQ, He JJ, Wang K, Svensson P. Influence of changing occlusal support on jaw-closing muscle electromyographic activity in healthy men and women. Acta Odontol Scand. 2009;67(3):187-192.
61. Baba K, Yugami K, Akishige S, Ai M. Immediate effect of occlusal contact pattern in lateral jaw position on the EMG activity in jaw-elevator muscles in humans. Int J Prosthodont. 2000;13(6):500-505.
62. Milani RS, De Perière DD, Lapeyre L, Pourreyron L. Relationship between dental occlusion and posture. Cranio. 2000;18(2):127-134.
63. Sakaguchi K, Mehta NR, Abdallah EF, et al. Examination of the relationship between mandibular position and body posture. Cranio. 2007;25(4):237-249.
64. Watanabe I. Influence of wearing complete dentures on body balance in edentulous elderly. Kokubyo Gakkai Zasshi. 1999;66(1):8-14.
65. Fujimoto M, Hayakawa L, Hirano S, Watanabe I. Changes in gait stability induced by alteration of mandibular position. J Med Dent Sci. 2001;48(4):131-136.
66. Gangloff P, Louis JP, Perrin PP. Dental occlusion modifies gaze and posture stabilization in human subjects. Neurosci Lett. 2000;293(3):203-206.
67. Koolstra JH, van Eijden TM. Three-dimensional dynamical capabilities of the human masticatory muscles. J Biomech. 1999;32(2):145-152.
68. Yoshino G, Higashi K, Nakamura T. Changes in head position due to occlusal supporting zone loss during clenching. Cranio. 2003;21(2):89-98.
69. Cordray FE. Three-dimensional analysis of models articulated in the seated condylar position from a deprogrammed asymptomatic population: a prospective study. Part 1. Am J Orthod Dentofacial Orthop. 2006;129(5):619-630.
70. Grünheid T, Langenbach GE, Korfage JA, et al. The adaptive response of jaw muscles to varying functional demands. Eur J Orthod. 2009;31(6):596-612.
71. Dahlström L. Conservative treatment of mandibular dysfunction. Clinical, experimental and electromyographic studies of biofeedback and occlusal appliances. Swed Dent J Suppl. 1984;24:1-45.
72. Bani D, Bani T, Bergamini M. Morphologic and biochemical changes of the masseter muscles induced by occlusal wear: studies in a rat model. J Dent Res. 1999;78(11):1735-1744.
73. Sumioka T. Systemic effects of the peripheral disturbance of the trigeminal system: Influences of the occlusal destruction in dogs. J Kyoto Pref Univ Med. 1989;98(10):1077-1085.
74. Slavicek R. The Masticatory Organ: Functions and Dysfunctions. Klosterneuburg, Austria: GAMMA Medizinisch-wissenschaftliche Fortbildung-AG; 2002.
75. Wang M, Mehta N. A possible biomechanical role of occlusal cusp-fossa contact relationships. J Oral Rehabil.
76. Korioth TW, Hannam AG. Effect of bilateral asymmetric tooth clenching on load distribution at the mandibular condyles. J Prosthet Dent.1990;64(1):62-73.
77. Hannam AG, McMillan AS. Internal organization in the human jaw muscles. Crit Rev Oral Biol Med. 1994;5(1):55-89.
78. Takai A, Nakano M, Bando E, Hewlett ER. Influence of occlusal force and mandibular position on tooth contacts in lateral excursive movements. J Prosthet Dent. 995;73(1):44-48.
79. Berry DC, Singh BP. Daily variations in occlusal contacts. J Prosthet Dent. 1983;50(3):386-391.
80. Watamoto T, Egusa H, Mizumori T, et al. Restoration of occlusal and proximal contacts by a single molar crown improves the smoothness of the masticatory movement. J Dent. 2008;36(12):984-992.
81. Iwase Y, Saitoh I, Okamoto A, et al . Do occlusal contact areas of maximum closing position during gum chewing and intercuspal position coincide? Arch Oral Biol. 2011;56(12):1616-1623.
82. Riise C, Ericsson SG. A clinical study of the distribution of occlusal tooth contacts in the intercuspal position at light and hard pressure. J Oral Rehabil. 1983;10(6):473-480.
83. Donegan SJ, Knap FJ. A study of anterior guidance. J Prosthodont. 1995;4(4):226-232.
84. Filtchev AD, Kalachev YS. Phenomenon of domination of the strongest contacts in centric occlusion . Quintessence Int. 2008;39(3):e99-e106.
85. Agrawal KR, Lucas PW. The mechanics of the first bite. Proc Biol Sci. 2003;270(1521):1277-1282.
86. Al-Nimri KS, Bataineh AB, Abo-Farha S. Functional occlusal patterns and their relationship to static occlusion. Angle Orthod. 2010;80(1):65-71.
87. Ingervall B, Hähner R, Kessi S. Pattern of tooth contacts in eccentric mandibular positions in young adults. J Prosthet Dent. 1991;66(2):169-176.
88. Ogawa T, Ogimoto T, Koyano K. Pattern of occlusal contacts in lateral positions: canine protection and group function validity in classifying guidance patterns. J Prosthet Dent. 1998;80(1):67-74.
89. Valenzuela S, Portus C, Miralles R, et al. Bilateral supra- and infrahyoid EMG activity during eccentric jaw clenching and tooth grinding tasks in subjects with canine guidance or group function. Cranio. 2012;30(3):209-217.
90. Wang Q, Wright BW, Smith A, et al. Mechanical impact of incisor loading on the primate midfacial skeleton and its relevance to human evolution . Anat Rec. 2010;293(4):607-617.
91. Paphangkorakit J, Osborn JW. Proclination of lower incisors: a design to maximize food penetration and minimize torque. J OralRehabil.2008;35(11):870-874.
92. Al-Hiyasat AS, Abu-Alhaija ES. The relationship between static and dynamic occlusion in 14-17-year-old school children. J Oral Rehabil. 2004;31(7):628-633.
93. Caro AJ, Peraire M, Martinez-Gomis J, e al. Reproducibility of lateral excursive tooth contact in a semi-adjustable articulator depending on the type of lateral guidance. J Oral Rehabil. 2005;32(3):174-179.
94. Beyron H. Occlusion: point of significance in planning restorative procedures. J Prosthet Dent. 1973;30(4 pt 2):641-652.
95. Atashrazm P, Dashti MH. The prevalence of occlusal disharmony and its associated causes in complete dentures. J Contemp Dent Pract. 2009;10(5):e041-e048.
96. Mahony D. Refining occlusion with muscle balance to enhance long-term orthodontic stability. Gen Dent. 2005;53(2):111-115.
97. Utz KH, Müller F, Lückerath W, et al. The lateral leeway in the habitual intercuspation: experimental studies and literature review. J Oral Rehabil. 2007;34(6):406-413.
98. Ferrario VF, Serrao G, Dellavia C, et al. Relationship between the number of occlusal contacts and masticatory muscle activity in healthy young adults. Cranio. 2002;20(2):91-98.
99. Forrester SE, Presswood RG, Toy AC, Pain MT. Occlusal measurement method can affect SEMG activity during occlusion. J Oral Rehabil. 2011;38(9):655-660.
100. Saad MN, Weiner G, Ehrenberg D, Weiner S. Effects of load and indicator type upon occlusal contact markings. J Biomed Mater Res B Appl Biomater. 2008;85(1):18-22.
101. Parkinson CE, Buschang PH, Behrents RG, et al. A new method of evaluating posterior occlusion and its relation to posttreatment occlusal changes. Am J Orthod Dentofacial Orthop. 2001;120(5):503-512.
102. Fasbinder DJ, Poticny DJ. Accuracy of occlusal contacts for crowns with chairside CAD/CAM techniques. Int J Comput Dent. 2010;13(4):303-316.
103. Reich S, Trentzsch L, Gozdowski S, Krey KF. In vitro analysis of laboratory-processed and CAD/CAM-generated occlusal onlay surfaces. Int J Prosthodont. 2009;22(6):620-622.
104. Reich S, Brungsberg B, Teschner H, Frankenberger R. The occlusal precision of laboratory versus CAD/CAM processed all-ceramic crowns. Am J Dent. 2010;23(1):53-56.
105. Sara.oğlu A, Ozpinar B. In vivo and in vitro evaluation of occlusal indicator sensitivity. J Prosthet Dent.
2002;88(5):522-526.
106. Millstein P, Maya A. An evaluation of occlusal contact marking indicators. A descriptive quantitative
method. J Am Dent Assoc. 2001;132(9):1280-1286.
107. Soboļeva U, Lauriņa L, Slaidiņa A. The masticatory system-an overview. Stomatologija.
2005;7(3):77-80.
108. Johansson A, Johansson AK, Omar R, Carlsson GE. Rehabilitation of the worn dentition. J Oral
Rehabil. 2008;35(7):548-566.
109. Woda A, Pionchon P, Palla S. Regulation of mandibular postures: mechanisms and clinical implications.
Crit Rev Oral Biol Med. 2001;12(2):166-178.
110. Dawson PE. New definition for relating occlusion to varying conditions of the temporomandibular joint.
J Prosthet Dent. 1995;74(6):619-627.
111. Hamata MM, Zuim PR, Garcia AR. Comparative evaluation of the efficacy of occlusal splints fabricated
in centric relation or maximum intercuspation in temporomandibular disorders patients. J Appl Oral
Sci. 2009;17(1):32-38.
112. Foglio-Bonda PL, Migliaretti G, Cavallo F, et al. Incisor and mandibular movement during retrusion
[published online ahead of print Feb 28 2006]. Arch Oral Biol. 2006;51(7):581-586.
113. Hatch JP, Shinkai RS, Sakai S, et al. Determinants of masticatory performance in dentate adults. Arch Oral Biol. 2001;46(7):641-648.
114. Lepley CR, Throckmorton GS, Ceen RF, Buschang PH. Relative contributions of occlusion, maximum bite force, and chewing cycle kinematics to masticatory performance. Am J Orthod Dentofacial Orthop. 2011;139(5):606-613.
115. Glickman I, Haddad AW, Martignoni M, et al. Telemetric comparison of centric relation and centric occlusion reconstructions. J Prosthet Dent. 1974;31(5):527-536.
116. Tripodakis AP, Smulow JB, Mehta NR, Clark RE. Clinical study of location and reproducibility of three mandibular positions in relation to body posture and muscle function. J Prosthet Dent. 1995;73(2):190-198.
117. Zonnenberg AJ, Mulder J. Variability of centric relation position in TMD patients. Eur J Prosthodont Restor Dent. 2006;14(1):32-37.
118. Taylor TD, Wiens J, Carr A.Evidence-based considerations for removable prosthodontic and dental implant occlusion: a literature review. J Prosthet Dent. 2005;94(6):555-560.
119. Niemann W. Lost vertical dimension/hypoxia. A case report and commentary. Funct Orthod. 2005;22(2):14-19.
120. Bissasu M. Pre-extraction records for complete denture fabrication: a literature review. J Prosthet Dent. 2004;91(1):55-58.
121. Strajnić L, Stanisić-Sinobad D, Marković D, Stojanović L. Cephalometric indicators of the vertical dimension of occlusion. Coll Antropol. 2008;32(2):535-541.
122. Orthlieb JD, Laurent M,Laplanche O. Cephalometric estimation of vertical dimension of occlusion. J Oral Rehabil. 2000;27(9):802-807.
123. Rivera-Morales WC, Mohl ND. Restoration of the vertical dimension of occlusion in the severely worn dentition. Dent Clin North Am. 1992;36(3):651-664.
124. Ferrario VF, Sforza C, Serrao G, Schmitz JH. Three-dimensional assessment of the reliability of a postural face-bow transfer. J Prosthet Dent. 2002;87(2):210-215.
125. Paul SJ. Smile analysis and face-bow transfer: enhancing aesthetic restorative treatment. Pract Proced Aesthet Dent. 2001;13(3):217-222.
126. Karl PJ, Foley TF. The use of a deprogramming appliance to obtain centric relation records. Angle Orthod. 1999;69(2):117-124.
127. Eriksson A, Ockert-Eriksson G, Lockowandt P, et al. Clinical factors and clinical variation influencing the reproducibility of interocclusal recording methods. Br Dent J. 2002;192(7):395-400.
128. Squier RS. Jaw relation records for fixed prosthodontics. Dent Clin North Am. 2004;48(2):vii, 471-486.
129. Murray MC, Smith PW,Watts DC, Wilson NF. Occlusal registration: science or art? Int Dent J. 1999;49(1):41-46.
130. Chakfa AM, Mehta NR,Forgione AG, et al. The effect of stepwise increases in vertical dimension of occlusion on isometric strength of cervical flexors and deltoid muscles in nonsymptomatic females. Cranio. 2002;20(4):264-273.
131.Ormianer Z, Palty A. Altered vertical dimension of occlusion: a comparative retrospective pilot study of tooth- and implant-supported restorations. Int J Oral Maxillofac Implants. 2009;24(3):497-501.
132. Abduo J. Safety of increasing vertical dimension of occlusion: a systematic review. Quintessence Int. 2012;43(5):369-380.
133. Amoric M. The golden number: applications to cranio-facial evaluation. Funct Orthod. 1995;12(1):18-21, 24-25.
134. Sofou AM, Diakoyianni-Mordohai I, Emmanouel I, et al. Using cephalometry to evaluate maxillomandibular relationships in complete denture construction. Int J Prosthodont. 1993;6(6):540-545.
135. Meier B, Luck O, Harzer W.Interocclusal clearance during speech and in mandibular rest position. A comparison between different measuring methods. J Orofac Orthop. 2003;64(2):121-134.
136. Burnett CA.Clinical rest and closest speech positions in the determination of occlusal vertical dimension. J Oral Rehabil. 2000;27(8):714-719.
137. McCord JF, Firestone HJ, Grant AA. Phonetic determinants of tooth placement in complete dentures. Quintessence Int. 1994;25(5):341-345.
138. Runte C, Lawerino M,Dirksen D, et al.The influence of maxillary central incisor position in complete dentures on /s/ sound production. J Prosthet Dent. 2001;85(5):485-495.
139. Sharry JJ. Complete Denture Prosthodontics. 3rd ed. New York: McGraw Hill; 1974:130-149.
140. Mack MR. Vertical dimension: a dynamic concept based on facial form and oropharyngeal function. J Prosthet Dent. 1991;66(4):478-485.
141. Tavano KT, Seraidarian PI, de Oliveira DD, Jansen WC. Determination of vertical dimension of occlusion in dentate patients by cephalometric analysis-pilot study. Gerodontology. 2012;29(2):e297-e305.
142. Kharbanda OP, Sidhu SS,Sundrum KR. Vertical proportions of face: a cephalometric study. Int J Orthod. 1991;29(3-4):6-8.
143. Mommaerts MY, Moerenhout BA. Reliability of clinical measurements used in the determination of facial indices. J Craniomaxillofac Surg. 2008;36(5):279-284.
144. Singh JR, Banerjee S.Normal values for interpupillary, inner canthal and outer canthal distances in an Indian population. Hum Hered. 1983;33(5):326-328.
145. Gerritsen AE, Allen PF, Witter DJ, et al. Tooth loss and oral health-related quality of life: a systematic review and meta-analysis. Health Qual Life Outcomes. 2010;8:126.
146. Bidra AS. Three-dimensional esthetic analysis in treatment planning for implant-supported fixed prosthesis in the edentulous maxilla: review of the esthetics literature. J Esthet Restor Dent. 2011;23(4):219-236.
147. Lundqvist S. Speech and other oral functions. Clinical and experimental studies with special reference to maxillary rehabilitation on osseointegrated implants. Swed Dent J Suppl. 1993;91:1-39.
148. Bosse LP, Taylor TD. Problems associated with implant rehabilitation of the edentulous maxilla. Dent Clin North Am. 1998;42(1):117-127.
149. Sadowsky SJ. The implant-supported prosthesis for the edentulous arch: design considerations. J Prosthet Dent. 1997;78(1):28-33.
150. Freilich MA, Altieri JV, Wahle JJ.Principles for selecting interocclusal records for articulation of dentate and partially dentate casts. J Prosthet Dent. 1992;68(2):361-367.
151. Fondriest JF. Using provisional restorations to improve results in complex aesthetic restorative cases. Pract Proced Aesthet Dent. 2006;18(4):217-223.
152. Moslehifard E, Nikzad S, Geraminpanah F, Mahboub F. Full-mouth rehabilitation of a patient with severely worn dentition and uneven occlusal plane: a clinical report. J Prosthodont. 2012;21(1):56-64.
153. Nanda A, Jain V,Srivastava A. An electromyographic study to assess the minimal time duration for using the splint to raise the vertical dimension in patients with generalized attrition of teeth. Indian J Dent Res. 2011;22(2):303-308.
154. Parker HM. Psychological implications of provisional prostheses. Dent Clin North Am. 1989;33(3):343-353.
155. Romeo G, Bresciano M. Diagnostic and technical approach to esthetic rehabilitations. J Esthet Restor Dent. 2003;15(4):204-216.
156. Nemcovsky CE. Transferring the occlusal and esthetic anatomy of the provisional to the final restoration in full-arch oral rehabilitations. Compend Contin Educ Dent. 1996;17(1):72-74.
157. Utz KH, Müller F, Lückerath W, et al. Accuracy of check-bite registration and centric condylar position. J Oral Rehabil. 2002;29(5):458-466.
158. Ikebe K, Matsuda K, Morii K, et al. Association of masticatory performance with age, posterior occlusal contacts, occlusal force, and salivary flow in older adults. Int J Prosthodont. 2006;19(5):475-481.
159. Klineberg I, Kingston D, Murray G.The bases for using a particular occlusal design in tooth and implant-borne reconstructions and complete dentures. Clin Oral Implants Res. 2007;18(suppl 3):S151-S167.
160. Lujan-Climent M, Martinez-Gomis J, Palau S, et al. Influence of static and dynamic occlusal characteristics and muscle force on masticatory performance in dentate adults. Eur J Oral Sci. 2008;116(3):229-236.
161. Lundqvist S, Haraldson T. Oral function in patients wearing fixed prosthesis on osseointegrated implants in the maxilla: 3-year follow-up study. Scand J Dent Res. 1992;100(5):279-283.
162. Kiliaridis S, Tzakis MG, Carlsson GE. Short-term and long-term effects of chewing training on occlusal perception of thickness. Scand J Dent Res. 1990;98(2):159-166.
163. Klineberg I, Murray G. Osseoperception: sensory function and proprioception. Adv Dent Res. 1999;13:120-129.
164. Williams E, Rydevik B, Johns R, BrånemarkP-I, eds. Osseoperception and Musculo-Skeletal Function.Göteborg, Sweden: The Institute for Applied Biotechnology. 1999.
165. Mattes S, Ulrich R, MühlbradtL. Detection times of natural teeth and endosseous implants revealed by the method of reaction time. Int J Oral Maxillofac Implants. 1997;12(3):399-402.
166. Willis RD, DiCosimo CJ. The absence of proprioceptive nerve endings in the human periodontal ligament: the role of periodontal mechanoreceptors in the reflex control of mastication. Oral Surg Oral Med Oral Pathol. 1979;48(2):108-115.
167. Mericske-Stern R, Hofmann J, Wedig A, Geering AH. In vivo measurements of maximal occlusal force and minimal pressure threshold on overdentures supported by implants or natural roots: a comparative study, Part 1. Int J Oral Maxillofac Implants. 1993;8(6):641-649.
168. Leung T, Lai VF. Control of jaw closing forces: a comparison between natural tooth and osseointegrated implant. Eur J Prosthodont Restor Dent. 2000;8(3):113-116.
169. Mericske-Stern R, Assal P, Mericske E,Bürgin W. Occlusal force and oral tactile sensibility measured in partially edentulous patients with ITI implants. Int J Oral Maxillofac Implants. 1995;10(3):345-353.
170. Fayz F, Eslami A.Determination of occlusal vertical dimension: a literature review. J Prosthet Dent.1988;59(3):321-323.