You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Dental caries or tooth decay is the most common chronic infectious-disease affecting children today.1-3 Tooth decay occurring in children aged six and younger is known as Early Childhood Caries (ECC)1 and is considered one of the most significant public health problems throughout the world, in both developed and developing countries.1-3 In the United States (U.S.), among children aged 2 to 5 years, 75% of the cases of ECC have been identified in 8% of the population,4 indicating that dental caries is more common in lower socioeconomic households and racial ethnicities.5 Dental caries is a preventable disease, yet despite all efforts, little improvement has been made in preventing ECC in the U.S.1
A systematic review of the literature by Castilho et al. identified that parents' previous caries experience, including the transmission of cariogenic bacteria, along with parents' oral self-care, and sugar intake, could increase the risk of caries development in their children. Children's oral health was linked with their parents' knowledge, attitude, socioeconomic status, level of education and maternal age.6 Furthermore, parental attitudes and beliefs were shown to be changed through increased oral health knowledge.7 Parental support during the implementation process of behavior changes has been linked to increased success in the adoption of positive oral health behaviors.6,7
Dentistry has focused on individual health promotion primarily using health education, rather than incorporating behavioral and population approaches.8 Early Childhood Caries has proven to be resistant to oral health promotion on the individual level.9 Challenges to the problem are further precipitated by the difficulty in accessing young children. During the first two years of life, children average 10 or more visits to a primary health care provider and may not ever visit a dentist or oral health care provider.10 Developing an oral health promotion program to reach parents and caregivers prior to their child's first dental visit has the potential to be an effective intervention tool.
Behavior strategies have been identified as necessary elements to ensure implementation and adherence of any health promotion intervention tool.9 The Theory of Planned Behavior (TPB) has been identified as a predictor of intent to engage in positive oral health behaviors.11 The constructs of the TPB are: behavioral norms (attitudes), normative beliefs (subjective norms); and control beliefs (perceived behavioral control).12
Dumitrescu and colleagues designed a cross-sectional study to evaluate five social cognitive theories including the TPB to explain current oral health behaviors and predict individuals' intentions to engage in positive oral health behaviors. Results of the study indicated that TPB and the Health Action Process Approach (HAPA) were the best predictors of intention to engage in oral health behaviors. Research findings of Dumitrescu et al. indicate that oral health education should focus on perceived behavioral control by improving knowledge and attitudes and removing barriers to daily oral health care through addressing performance difficulty, confidence, perceived control, and locus of control.11
Smartphone applications (apps) have the capacity to provide computer-tailored, population based interventions throughout the day and night, as 90% of mobile phone users in the U.S. are reported to be in possession of their phone at all times.13 Health promotion strategies have been proven to be successful when behavior change strategies have been incorporated into modern technology, including the Internet,14 mobile phone text messaging,15,16 and more recently smartphone apps.13,17-21 In addition, apps incorporating behavior change strategies are typically associated with increased effectiveness of the intervention.21
Smartphones, mobile phones with the capacity of a hand-held computer, are widely used across all socioeconomic groups, making them an excellent resource for health promotion messaging.18,22 An estimated 85% of adults aged 18-29 in the U.S. possess a smartphone and ownership has not been shown to be influenced by socioeconomic status (SES).23 However, lower SES users have been shown to spend more money downloading apps and are more likely to use their smartphone as their only source of Internet access than higher SES users.24 This user profile provides an opportunity to deliver remotely administered oral health promotion and the ability to access lower socioeconomic populations. Development of a smartphone oral health app requires a review of current literature to determine the theoretical basis for the prototype and testing for acceptability within the target audience.25 The purpose of this study was to develop and test a prototype of a smartphone app (ToothSense) as an oral health promotion tool for the prevention of ECC targeting parents and caregivers of children six years and younger. The study assessed the app's usability, quality, performance, likelihood to recommend, and users' perceptions of TPB intervention strategies.
Methods
This study was granted exempt status from the Institutional Review Board of MCPHS (Massachusetts College of Pharmacy and Health Sciences) University. The app prototype development and resting process used both quantitative and qualitative measures in two phases of the study: app prototype design and development based on the Theory of Planned Behavior (TPB) followed by beta testing of the app prototype.
Design and Development
An interdisciplinary team including a dental hygienist (primary researcher), graphic motion designer, and two app software developers collaborated to develop and beta test an oral health promotion prototype app, titled ToothSense. To ensure the development process was replicable and systematic, the Behavioral Intervention Technology (BIT) model was used. The BIT model was designed to process the delivery of BITs from a clinical to a technological framework,26 and has been used previously to document app development.27 The BIT model describes the clinical aims, intervention strategies, and their incorporation into the features of the app.27 Furthermore, the BIT model accounts for the how, what, why and when questions of document design features in technological intervention strategies.26
Intervention Aims and Strategies
The overall clinical aim was to increase positive oral health behaviors in children 6 years and younger by influencing their parents and/or caregivers to adopt positive oral health behaviors. Usage aims were designed to encourage daily interaction/use of the application.
Doshi's Intervention Strategies (DIS) by Behavior Change Model or Theory provides intervention strategies including knowledge, general information, perceived benefits/barriers/risks, self-efficacy/talk and perceived social norms accounting for all the constructs of behavior modification theories.28 The app prototype features included goal setting, motivation, monitoring, and feedback to account for DIS. Education increased knowledge and the user's understanding of the overall goal and steps to reach that goal.26 Motivation included strategies to increase the likelihood users would engage in certain desirable behaviors and be useful in addressing self-efficacy. Goal setting involved future planning that included activity scheduling, while monitoring involves recording past or current states.26 Both goal setting and monitoring accounted for the self-efficacy strategy. Feedback provided information on current or past oral health behaviors and was used to address self-efficacy and perceived social norms.
Goal Setting
The app prototype features for goal setting were found in the settings screen. Users were prompted to set toothbrushing reminders for morning and evening which resulted in push notification sent to the iOS device. A push notification is the delivery of information from a software application to a computing device without the request of the user.29 The push notification read, "Time to brush!" and was sent to the user twice a day at the designated times. Additionally, push notifications helped to meet the initial usage aims.
Monitoring and Feedback
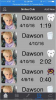
The app prototype accounted for monitoring and feedback in the following features: Sugar Bug Status, Brush Along, Smiles Club, and Mouth Journal. To monitor the strategies, reports were compiled through data collection and displayed to the user within the app. The data was displayed in two locations: Smiles Club and Mouth Journal. Smiles Club displayed a picture, age, brushing experience information (time and date), and badges that corresponded to the time and affirmation of flossing. (Figure 1) Brushing experiences (time) were automatically recorded when users brushed to a video found on the Brush Along screen (Figure 2). Users were then able to "share" that experience with the Smiles Club by selecting "Share." Smiles Club information was displayed only to friends of the users; all information remained private unless the user accepted a friend request. Mouth Journal was a linear graph displaying a week of individual brushing experiences and the average time. Logs entries allowed the user to manually enter a brushing experience. The log option was located on the "Smiles Club" screen and allowed users to enter the length of brushing and time of day if the user chose not to use the "Brush Along" feature.
Interactive Elements
Interactive features incorporated into the prototype app included information delivery, notifications, logs, peer support, reviews, and visualization. All oral health information (OHI) was obtained from the American Dental Association (ADA) website.30 Educational texts were used to deliver OHI for toddler oral health care, nutritional advice, importance of dental visits, infant oral health care, importance of family/parental involvement in maintaining habits, and social rewards and consequences of oral health. Two oral health videos were available for viewing and provided the following OHI messages: importance of primary teeth, and OHI for children two years and older. A link for texts and videos was accessible on an "Oral Health Information" page located on the home screen, the first screen to appear when application is active. Two icons appeared on this screen titled "Tooth Sense" and "Sugar Bug Status." (Figure 3). All educational and media texts could be accessed on a separate screen linked through the Tooth Sense icon.
Workflow
The app prototype primarily used a user-defined workflow to administer its interventions. In addition, the prototype directed users to a specific workflow based upon their pre-determined oral health status in the Sugar Bug Status feature. Users were also able to specify the frequency of the push notification intervention in the Settings menu.
Application Prototype Testing
In addition to design features, user satisfaction also plays a vital role in the overall success of health promotion. Satisfactory usability of a website or app is based on compliance with five interface design heuristics known as Jakob Nielsen's (JN) general principles for interaction design, in which users value an app that is efficient, intuitive, and allows for easy input of information.31
Upon completion of initial prototype development, the testing phase was conducted through a user testing service (UserTesting; Mountain View, CA), specializing in consumer feedback on quality and performance of mobile apps.32 Participants were recruited by the user testing service to serve as beta testers. Inclusion criteria were: owner/user of an iOS operating system smartphone (iPhone; Apple Inc., Cupertino, CA); parent or primary caregiver of one or more children age six years or younger; and U.S. resident. Dental professionals were excluded from participating. The study required the beta testers have a personal smartphone capable of downloading the app prototype. Eight beta tests were deemed sufficient for evaluating the app prototype for usability and perception of the TPB intervention strategies. Determination of the number of beta tests was based on research findings demonstrating that usability testing with a minimum of 5 market testers will identify 85% of all usability problems.32,33
Beta testers were asked to complete a series of tasks to ensure all features of the app were utilized. Tasks were created based upon the app features and from suggestions provided by the user testing web site.32 Most tasks were accompanied by a prompt to encourage feedback on the testers experience with the application features. A camera was placed on the shoulder of each beta tester while they conducted the tasks to record the video and audio and they were encouraged to think aloud and talk through their actions and feelings. This method reduced the need to rely on self-reported measures, which can be biased.33
Upon completion of the tasks, the testers were asked to complete a survey consisting of usability statements based upon JN's five principles for interaction design,31 and the presence of the TPB intervention strategies based on DIS.34 Responses were recorded using a 5-point Likert-item (1=strongly disagree, 2=disagree, 3=neither agree or disagree, 4=agree, 5=strongly agree) and were tallied to obtain a mean score for each question on usability and perceptions of TPB. Mean scores of 4 and above indicated agreement with the statement, features and positive perception of interventions. Mean scores of 3 to 4 indicated some user indifference with the statement, app features, and perceptions of intervention strategies. Mean scores lower than 3 indicate disagreement with the statement, significant usability issues, and negative perceptions of the intervention strategy. A final question asked testers to rate the likelihood to recommend the app prototype (0=Not at all likely, 10=Very likely) using a Net Promoter Score calculated by the user testing service and compared to all sites tested by the service. A Net Promoter is a commonly used customer loyalty metric derived from survey responses to the question: "How likely are you to recommend this website/app to a friend or colleague?"32 Beta testers rating an app as a 9 or 10 are considered "promoters", a rating of 7 or 8 "passives", and rate 0 to 6 "detractors."32 The percentages of detractors are subtracted from the percentages of promoters to give a Net Promoter Score.32
Data from the audio and video recordings was analyzed to better understand the beta testers interactions and perceptions of the app. A template approach using codes was applied to organize the data.35 Preliminary codes were developed based on the audio and video recordings and the theoretical framework of TPB.35 Key points made by the participants were transcribed after listening and watching beta testers responses to prompts and complete tasks.34 Analysis of texts were guided by the preliminary codes.35 Similarities and differences of data emerged, and themes were identified, further clustered and defined.35
Results
Eight beta testers, 6 females and 2 males, ranging in age from 22 to 36 years, participated in the study. The average age of the participant was 27.5 years. One tester had an annual income level below 40K while the remaining seven had income levels between 40K and 100K. The average amount of time the beta testers used the prototype app was 00:15:12.
Prototype Application Usability
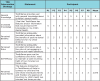
All beta testers agreed the app met three of the five usability statements (Table I). The most common usability concern was regarding the interface design of the OHI and Sugar Bug Status screens, commonly described by the testers as crowded and difficult to read. Testers requested brighter colors and a simpler layout to improve the readability and decrease the number of icons. Several beta testers were unable to use all of the features and requested instructions and/or clarification. It should be noted however that the users rarely read the pop-up instructions incorporated into the app when using a feature for the first time.
Prototype Application and the Theory of Planned Behavior
Beta testers agreed the TPB strategies were met in the app (Table II). All users felt strongly the app provided oral health knowledge and features/information that addressed the risks and benefits of engaging in or not engaging in oral health behaviors. Most testers agreed the app would increase their oral health knowledge and felt the app gave them the confidence and skills needed to maintain positive tooth-brushing habits for their children. When asked about the ability of the application to provide features that would connect their children with other children who engage in positive oral health behaviors, only two users strongly agreed, while the remaining users were neutral or disagreed.
Intention to Recommend
Beta testers were asked to rate the likelihood to recommend the app prototype (0=Not at all likely, 10=Very likely) and a positive Net Promoter Score of 20 was calculated by the user testing site and compared to all sites tested.32 Three beta testers were "promoters", 3 "passives", and 2 "detractors". The prototype received positive reviews in terms of concept, information provided, and likelihood to recommend the app, indicating the potential for an oral health promotion app.
Qualitative Analysis of Audio and Video Recordings
Qualitative analysis of the audio and video recordings regarding the usability of the app prototype indicated that while most of the testers found the app to be helpful especially with regards to the timer and alarm function, some felt the features to be too advanced for their child's age. Testers had negative comments in regards to the interface design particularly regarding the color, images and the location and size of the icons on the screen. Navigation through the Smiles Club and Mouth Journal presented difficulties for some testers and others indicated the need for more guidance in the app for error recovery and task completion. Terminology was another theme in the qualitative analysis with some testers having concerns over the use of "sugar bugs" to describe bacteria or not understanding the meanings of some of the buttons on the app. Testers responded positively to the oral health information available on the app prototype indicating that this was new information that helped them understand the risks related to not caring for their child's teeth. The themes of interface design, navigation, feedback, terminology, information, health promotion and selected comments are shown in Table III.
Discussion
The development and testing of embedding the TPB in a prototype contributes to the understanding of how to provide parental support during the implementation of oral health promotion to increase the adoption of positive oral health behaviors.6,7 The beta testers feedback was positive with respect to accounting for the TPB as well as for recommending the app. The prototype serves as a model to address parental involvement in the prevention of ECC. The positive Net Promotor Score (likelihood to recommend) indicates the potential for a cascade effect in which users would recommend or discuss their experience with the app prototype and resulting in encouraging others to utilize the app. This research study provides a model for a potential app design thus it was important to address the prototype usability issues early in the development process with the goal of increasing user satisfaction and promotion of positive health behaviors.
Although dental apps for children are available from a variety of sources, there are no indications that the apps were developed in a research setting with a behavior modification theory, or specifically directed towards parents and caregivers. The ToothSense app prototype differs from other app products as it was developed to provide an intervention founded in a behavior modification theory for parents and caregivers of children, rather than as a child's game.
There are several limitations to consider with this study. Limited financial resources influenced the development of the prototype and may have contributed to some of the usability issues. While this was a limitation it was beneficial to test a prototype early in the development stages to identify usability issues prior to release and ensure positive user interaction and ratings in the market place. Another limitation of this study was the short amount of time the beta testers used the prototype with an average time of 00:15:12. The iOS operating system may also have been a limitation in this study. Expanding to the Android platform would broaden the base of potential users.
Conclusion
Using a mobile platform for oral health promotion provides the opportunity to engage parents, enable communication, and potentially help overcome oral health challenges for the management of oral diseases such as ECC. Beta testing results from this study provided health promotion project design information for the prevention of ECC using the TPB and highlighted the importance of health promotion smartphone app usability. Future research should include modifications to the app based on the prototype test results, pilot testing among parents and caregivers of children 6 years and younger and expansion of the mobile platforms.
About the Authors
Sara L. Nolen, RDH, MS is a graduate of the Master of Science in Dental Hygiene Program; Lori J. Giblin-Scanlon, RDH, MS is an associate professor and associate dean for clinical programs; Linda D. Boyd, RDH, RD, EdD is a professor and dean; all at the Forsyth School of Dental Hygiene, MCPHS University, Boston, MA. Lori Rainchuso, RDH, DHSc is an associate professor, Doctor of Health Sciences Program at MCPHS University, Boston, MA.
Corresponding author: Lori Giblin, RDH, MS; lori.giblin1@mcphs.edu
References
1. Colak H, Dülgergil CT, Dalli M, et al. Early childhood caries update: A review of causes, diagnoses, and treatments. J Nat Sci Biol Med. 2013 Jan-Jun; 4(1):29-38.
2. Dye BA, Tan S, Smith V, et al. Trends in oral health status: United States, 1988-1994 and 1999-2004. Vital Health Stat 11. 2007 Apr; (248):1-92.
3. Tinanoff N, Reisine S. Update on early childhood caries since the Surgeon General's Report. Acad Pediatr. 2009 Nov-Dec; 9(6):396-403.
4. Macek MD, Heller KE, Selwitz RH, et al. Is 75 percent of dental caries really found in 25 percent of the population? J Public Health Dent. 2004 Winter; 64(1):20-5.
5. Dye BA, Thornton-Evans G, Li X, Iafolla TJ. Dental caries and sealant prevalence in children and adolescents in the United States, 2011-2012. NCHS Data Brief. 2015 Mar; (191):1-8.
6. Castilho AR, Mialhe FL, Barbosa TeS, et al. Influence of family environment on children's oral health: a systematic review. J Pediatr (Rio J). 2013 Feb; 89(2):116-23.
7. Adair PM, Pine CM, Burnside G, et al. Familial and cultural perceptions and beliefs of oral hygiene and dietary practices among ethnically and socio-economically diverse groups. Community Dent Health. 2004; 21(1 Suppl):102-11.
8. Bracksley-O'Grady SA, Dickson-Swift VA, Anderson KS, et al. Health promotion training in dental and oral health degrees: a scoping review. J Dent Educ. 2015 May; 79(5):584-91.
9. Albino J, Tiwari T. Preventing Childhood Caries: A Review of Recent Behavioral Research. J Dent Res. 2016 Jan; 95(1):35-42.
10. Douglass JM, Clark MB. Integrating oral health into overall health care to prevent early childhood caries: need, evidence, and solutions. Pediatr Dent. 2015 Aug; 37(3):266-74.
11. Dumitrescu AL, Dogaru BC, Duta C, et al. Testing five social-cognitive models to explain predictors of personal oral health behaviours and intention to improve them. Oral Health Prev Dent. 2014;12(4):345-55.
12. Ajzen I. Behavioral Interventions Based on the Theory of Planned Behavior [Internet]. University of Massachusetts, Amherst; 2006 [cited November 2015]. Available from: http://people. umass.edu/aizen/pdf/tpb.intervention.pdf.
13. Glynn LG, Hayes PS, Casey M, et al. Effectiveness of a smartphone application to promote physical activity in primary care: the SMART MOVE randomised controlled trial. Br J Gen Pract. 2014 Jul; 64(624):e384-91.
14. Webb TL, Joseph J, Yardley L, et al. Using the internet to promote health behavior change: a systematic review and meta-analysis of the impact of theoretical basis, use of behavior change techniques, and mode of delivery on efficacy. J Med Internet Res. 2010 Feb; 12(1):e4.
15. Krishna S, Boren SA, Balas EA. Healthcare via cell phones: a systematic review. Telemed J E Health. 2009 Apr; 15(3):231-40.
16. Hashemian TS, Kritz-Silverstein D, Baker R. Text2Floss: the feasibility and acceptability of a text messaging intervention to improve oral health behavior and knowledge. J Public Health Dent. 2015 Winter; 75(1):34-41.
17. Abroms LC, Lee Westmaas J, Bontemps-Jones J, et al. A content analysis of popular smartphone apps for smoking cessation. Am J Prev Med. 2013 Dec; 45(6):732-6.
18. Casey M, Hayes PS, Glynn F, et al. Patients' experiences of using a smartphone application to increase physical activity: the SMART MOVE qualitative study in primary care. Br J Gen Pract. 2014 Aug; 64(625):e500-08.
19. Carter MC, Burley VJ, Nykjaer C, et al. Adherence to a smartphone application for weight loss compared to website and paper diary: pilot randomized controlled trial. J Med Internet Res. 2013 Apr; 15(4):e32.
20. Hebden L, Cook A, Van Der Ploeg HP, et al. Development of smartphone applications for nutrition and physical activity behavior change. JMIR Res Protoc. 2012 Aug; 1(2):e9.
21. Direito A, Dale LP, Shields E, et al. Do physical activity and dietary smartphone applications incorporate evidence-based behaviour change techniques? BMC Public Health. 2014 Jun; 14:646.
22. Fogg BJ. Mobile Persuasion: 20 perspectives on the future of behavior change. 1st Ed. Stanford: Stanford Captology Media; 2007; p 5-11.
23. Smith, A. The smartphone difference [Internet]. Wasahington, DC: Pew Research Center; 2015 Apr [cited 2018 Feb 27]. Available from http://www.pewinternet.org/2015/04/01/us-smartphone-use-in-2015/.
24. Ahmad R, Tossell C, Shepard C, et al. Exploring iPhone usage: the influence of socioeconomic differences on smartphone adoption, usage and usability, Proceedings of the 14th international conference on Human-computer interaction with mobile devices and services, Sept 21-24, 2012, San Francisco, California.
25. Kirwan M, Duncan MJ, Vandelanotte C, et al. Design, development, and formative evaluation of a smartphone application for recording and monitoring physical activity levels: the 10,000 Steps "iStepLog". Health Educ Behav. 2013 Sept; 40(2):140-51.
26. Mohr DC, Schueller SM, Montague E, et al. The behavioral intervention technology model: an integrated conceptual and technological framework for eHealth and mHealth interventions. J Med Internet Res. 2014 Jun;16(6):e146.
27. Anderson J, Wallace L. Applying the Behavioural Intervention Technologies model to the develop- ment of a smartphone application (app) supportinig young peoples' adherence to anaphylaxis action plan. BMJ Innoventions. 2015; 1:67-73.
28. Doshi A, Patrick K, Sallis JF, et al. Evaluation of physical activity web sites for use of behavior change theories. Ann Behav Med. 2003 Spring; 25(2):105-11.
29. Tech Target: search mobile computing [Internet]. Massachusetts: Techtarget; c2003-2018. Definition push notification; no date [cited August 2016]: [about 3 screens] Available from http://searchmobilecomputing.techtarget.com/definition/push-notification.
30. American Dental Association [Internet]. Chicago; American Dental Association; c2018 Mouth healthy: babies and kids [cited 2015 Nov 1]; [about 2 screens]. Available from http://www. mouthhealthy.org/en/babies-and-kids.
31. Mendiola MF, Kalnicki M, Lindenauer S. Valuable features in mobile health apps for patients and consumers: content analysis of apps and user ratings. JMIR Mhealth Uhealth. 2015 May; 3(2):e40.
32. UserTesting [Internet]. California: User Testing: c2018. UserTesting platform; 2016 May [cited July 12, 2017]: [about 6 screens] Available from https://www.usertesting.com/platform.
33. Nielsen J. How many test users in a usability study [Internet]. Nielsen Norman Group; 2012 Jun 4 [cited 2016 Feb 10]; [about 2 screens]. Available from https://www.nngroup.com/articles/how-many-test-users/.
34. Doshi A, Patrick K, Sallis JF, et al. Evaluation of physical activity web sites for use of behavior change theories. Annals of Behavioral Medicine. 2003 Spring; 25(2):105-11.
35. Fereday J, Muir-Cochrane E. Demonstrating rigor using thematic analysis: a hybrid approach of inductive and deductive coding and theme development. Int J Qual Methods. 2006 Mar;5(1):1-10.