You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
In American culture, judgments and opinions are often made based solely on appearance. Often, peoples’ physical appearance fuels their confidence level. Research has shown that people who are considered attractive receive preferential treatment and are judged more positively.1 An important element to one’s appearance is an attractive smile, which brings balance and proportion to the face, while a perfect white shade of teeth helps a person look their best. In our beauty- and media-driven society, white teeth are highly important.
Historically, tooth whitening is the most commonly used modality in cosmetic dentistry. Yet, eight out of 10 people are unhappy with the appearance of their yellowing teeth,2 and only 25% of the population has tried a professional whitening product.3 Of those consumers who have used an over-the-counter (OTC) whitening product, 65% would not recommend it, and only two out of 10 consumers have gone to the dentist for whitening.3 There is a huge disconnect between the actual usage of tooth whitening and the needs and wants of the consumer.
Dental patients may not pursue whitening options because they are concerned about cost and/or potential discomfort and lack understanding of the options available to them. The busy pace in many dental offices may not be conducive to careful discussions with patients, in terms they understand, about their desires for an attractive smile or the options the practice can offer them to achieve that smile. Clinicians can motivate and engage their patients to help them attain the tooth color they desire and can introduce those aforementioned 65% of patients who are dissatisfied with OTC bleaching treatments to an in-office procedure or take-home custom trays, which is an enormous untapped revenue source.
Questions and Answers
Five basic questions can be addressed to help clinicians create value and attain consensus with patients.
Question 1: What Whitening Options Are Available?
There are many ways to achieve natural-looking white teeth. The use of OTC products is simple, and they are available in a variety of strips, pens, and brushes. However, as noted above, the majority of patients are dissatisfied with the results.3
A second option is for the dentist to fabricate custom trays in the office and dispense whitening gel (eg, KöR Whitening, www.korwhitening.com; Opalescence® PF, Ultradent Products, Inc, www.ultradent.com; Philips Zoom DayWhite, Philips, www.usa.philips.com). The patient applies the gel in the custom trays at home. The success of this technique, however, depends almost solely on patient compliance, which is often inconsistent. Patients may subsequently be dissatisfied because they failed to achieve their desired tooth shade. Their frustration can be compounded by the astounding results they see in television and magazine advertisements, and disappointment sets in when their results fall short of these expectations. Unfortunately for the clinician, the lack of success was not due to any fault of his or her own, but to the patient failing to wear the trays enough.
A third option, however—in-office power bleaching—is a quick, safe, and predictable way to determine whether a simple solution to an esthetic problem can be accomplished. The dentist or the team professionally applies the product in the office. Concentrations of up to 40% hydrogen peroxide (HP) have been used with a barrier to protect the soft tissues of the face and gingiva. Twenty-five percent HP has been proven to be a highly effective concentration,4 and adding a light source accelerates the process.
Question 2: How Does the Whitening Process Work?
Teeth bleach as a result of the diffusion of HP into the tooth structure. The diffusion increases with greater concentrations of HP, increased time of exposure to the bleach, and application of heat, light, or laser. HP is fast-acting, breaking down into water and oxygen radicals in seconds.5 It permeates the enamel and dentin, and its maximum whitening strength is at 30 minutes, with the reaction time being completed within 90 minutes. Carbamide peroxide (CP) breaks down into HP and urea. Ten percent CP produces 3.6% HP. This reaction is complete within 4 to 6 hours, reaching its maximum whitening strength at 2 hours. CP is used in nighttime products because of the longer exposure time available during sleep. There is less salivary flow and, therefore, less dilution, and, thus, faster results. Nighttime whitening is contraindicated with patients with a history of nocturnal bruxism[REF needed for this last sentence].
The higher the concentration of the HP, the faster the whitening, but there is also a higher risk of sensitivity. Highly sensitive patients should start with a low HP or CP concentration and wear the trays for a shorter period of time. Whitening yellow teeth has a more dramatic and predictable result than treating gray teeth. Also, monochromatic, even-toned teeth have a more predictable bleaching outcome than striated, tetracycline-stained, or white-spotted teeth.
Question 3: Why Is a Light Needed?
The use of an in-office light increases the efficiency and speed of the whitening process. Take-home whitening can provide excellent results when patient compliance is exceptional; however, compliance is often lacking. The use of the in-office light provides a bleaching outcome similar to 14 days of continuous home-tray use.6,7 This “jump start” can improve patient compliance in the months to come, and the rapid change in the patient’s smile can provide immediate satisfaction. Both types of systems can whiten between six and nine shades on the shade guide, but the light-activated systems can provide an additional one to two shade guide improvements over non-light-activated systems.6,7
The best results are obtained with 25% HP, as this concentration has the optimal absorption kinetics. The Philips Zoom WhiteSpeed lamp produces very little heat due to its narrow light spectrum. Tooth stain (often caused by double carbon bonds imbedded in the organic portion of the tooth) is more effectively broken down by HP with the light-emitting diode (LED) blue light. The blue light from the lamp is also absorbed by the yellow stains in the dentin.8
Question 4: Will Whitening Harm Teeth, Either Now or Later?
Patients may experience a temporary increase in tooth sensitivity during or after the whitening process. The sensitivity can range from a mild reaction to cold temperatures to a shooting pain that occurs immediately during the procedure and may last up to several hours after treatment. Any history of temperature sensitivity should be noted, and those patients should be prescribed a pre-bleaching regimen for 2 weeks. This regimen requires the use of a desensitizing toothpaste that is sodium lauryl sulfate–free (eg, Sensodyne ProNamel® 5000, GlaxoSmithKline, www.pronamel.us; ClinPro™ 5000, 3M ESPE, solutions.3m.com). If the reported sensitivity was severe, desensitizing gels (eg, Relief® ACP Zoom, Philips; UltraEZ®, Ultradent Products, Inc) should be placed in custom whitening trays and worn daily for 1 hour during the week prior to the bleaching appointment and for 1 hour immediately following the procedure.9 These gels may also contain remineralization components that increase the enamel microhardness.10
Sensitivity during the bleaching procedure is likely caused by the penetration of the HP through the enamel and dentin and into the pulp, creating a reversible pulpitis.11 Sensitivity is transient,12 and an analgesic (ibuprofen 600 mg) should be administered at the onset of the procedure.13
Question 5: How Can Patients Be Made Aware They Need Whitening?
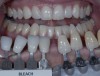
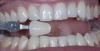
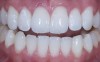
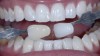
Dentists can provide a quick and easy shade assessment for each patient. Using a smart phone, a team member takes a preoperative photograph with the Vita shade guide (VITA, www.vitanorthamerica.com) next to the whitening shade guide, positioned at the lower lipline (Figure 1). The preoperative color is chosen and a second preoperative photographic image is recorded using only the single shade tab that matches the pre-existing darker color. It is placed on the left half of the photograph (the patient’s right side) (Figure 2).
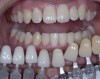
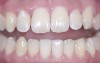
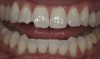
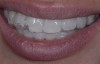
The whitening conversation begins with the dentist and patient reviewing the photographs together on a computer screen. The patient verifies his or her beginning shade and, for comparison, is then shown photographs of other patients who presented with a similar preoperative shade who completed whitening and bonding (Figure 3 through Figure 5). The appropriate whitening options for the patient’s particular clinical situation can then be discussed, with patients then choosing the product that they like best and most meets their esthetic expectations while fitting within their budget.
When the procedure is complete (either in-office or take-home), team members follow a checklist designed for the postoperative evaluation. A final postoperative photograph is taken using the original single shade tab that matched the pre-existing darker color on the left half of the photo (the patient’s right side) and the new single shade tab that matches the whitened teeth. This tab is placed on the right half of the photo (the patient’s left side) (Figure 6).
The dentist should use specific scripting when discussing the results with the patient, asking what shade of yellow the beginning shade was, followed by “What shade of yellow are the teeth now?” The team member could then point out that the teeth whitened all the way to the 010 whitening shade tab. The dentist and team should show excitement over the results, re-emphasize them, and show the patient the photographs. Patients are then told they will receive the photographs via email and are encouraged to share them with friends and post them on social media.
Case Report
A 30-year-old female patient presented with right lateral and central incisors that were fractured in a fall (Figure 7). Radiographs were taken and clinical testing revealed a fracture-free root and a vital pulp. Restorative options were presented that included porcelain and composite restorations. The patient desired to conserve tooth structure and chose direct composite restorations. Photographs of previous patients were reviewed and the whitening discussion began. She preferred the quickest solution to attain the whitest smile possible; therefore, in-office power bleaching (Philips Zoom WhiteSpeed) was chosen.
Clinical Protocol
The 25% HP bleaching gel was applied and repeated for three 15-minute cycles, for a total exposure time of 45 minutes. At-home trays were filled with desensitizing gel (Relief ACP Zoom), which also contains remineralization agents to increase the enamel microhardness7 (Figure 8).
The peroxide from the bleach decreases the bond strength to the tooth and it takes 14 days for the bond strength to return to normal[REF?] (Figure 9). Thus, 2 weeks later anesthesia was administered and all extrinsic stain on the teeth was removed with pumice on a soft prophy brush. Shade selection and mockup was immediately performed. Shade selection was accomplished by curing small increments of enamel shades (Filtek™ Supreme Ultra A1E and B1E, 3M ESPE; Premise™ B1E, Kerr Dental, www.kerrdental.com; and IPS Empress® Direct B1E, Ivoclar Vivadent, www.ivoclarvivadent.com) onto the teeth to be treated. In this case, IPS Empress Direct demonstrated the best match to the surrounding tooth structure.
To produce a seamless undetectable transition from tooth to restoration, an infinity bevel preparation was started with a medium-grit diamond bur (Brasseler M862-009, Brasseler USA, http://brasselerusadental.com) and placed 0.5 mm into the dentin. The bevel was carried 2 mm beyond the fracture lines. The lingual preparation requires a chamfer of 0.8 mm in thickness[REF?]; this allows a bulk of composite that will resist fracture with tooth flexure. The tooth was microetched (Microetcher® II, Danville Materials, www.danvillematerials.com), then rinsed. Because all the bonded surfaces were enamel, the total-etch technique was used and a 37% phosphoric etch was placed past the margins of the infinity bevel on to unprepared tooth and agitated with a microbrush for 15 seconds. The etch was rinsed off the tooth for 5 seconds followed by light air-drying with care to leave the preparation visually moist. A coat of universal adhesive containing 10-methacryloyloxydecyl dihydrogen phosphate (MDP) (All-Bond Universal®, Bisco, www.bisco.com) was scrubbed on the preparation with a microbrush for 15 seconds, followed by evaporating the excess solvent by thoroughly air-drying for 10 seconds. When the tooth appeared glossy, it was ready to be light-cured for 10 seconds. This total-etch and adhesive technique was used on all augmented surfaces of teeth Nos. 7 and 8.
The palatal enamel walls of teeth Nos. 7 and 8 were developed freehand up to the height of the incisal edge with IPS Empress Direct BL-LE. To match the contralateral teeth, an additional 1 mm composite rope BL-XLD was placed on the incisal edge. The dentin shade B1-D was rolled into a ball and smoothed and feathered over the bevel. A second increment was used to form the lobe. It is important to view this layer from an incisal view and not build it too thick. Placing opalescent composite Trans 30 between the lobes created a desired halo affect (Figure 10). Shade B1E was placed as a final facial layer and light-cured for 20 seconds.
Using finishing and polishing discs (Sof-Lex™, 3M ESPE), primary anatomy was refined. When performing these adjustments, it is important to evaluate the results from all views and mimic the contralateral tooth in shape form and surface texture. A final luster was attained using spiral-finishing wheels (3M ESPE) followed by placing polishing paste (Enamelize™, Cosmedent, www.cosmedent.com) on a felt wheel (Figure 11 through Figure 13).
Conclusion
Smile transformations may happen on the outside, but there is no denying the overpowering effect they have on how patients feel on the inside. Whiter teeth can boost their confidence level. A wide gap exists between the wants and needs of patients regarding tooth whitening and the actual usage of it, and clinicians must better communicate its value. Implementing the tooth-whitening strategies outlined herein will help ensure patient retention, new patient generation, and increased revenue.
About the Author
Joyce L. Bassett, DDS
Private Practice
Scottsdale, Arizona
References
1. Talamas SN, Mavor KI, Perrett DI. Blinded by beauty: attractiveness bias and accurate perceptions of academic performance. PLoS One. 2016;11(2):e0148284.
2. Oral Care – US – May 2013. London, England: Mintel Group Ltd; 2013.
3. Philips Oral Care. Data on file. Whitening Usage & Attitude Survey. StrateSci Inc Marketing Research. Whittier, CA; 2012.
4. Li Y, Lee S, Kwon SR, et al. A randomized, parallel-design clinical trial to assess tooth bleaching efficacy and safety of light versus non-light activated chairside whitening. Philips website. Data on file, 2012. http://www.usa.philips.com/content/dam/b2c/category-pages/personal-care/POHC/resource-library-docs/A-Randomized-Parallel-Design-Clinical-Trial-to-Assess-Tooth-Bleaching-Efficacy-and-Safety-of-Light-versus-non-Light-Activated-Chairside.pdf. Accessed April 3, 2017.
5. Kwon SR, Wertz PW. Review of the mechanism of tooth whitening. J Esthet Restor Dent. 2015;27(5):240-257.
6. Ontiveros JC, Paravina RD. Color change of vital teeth exposed to bleaching performed with and without supplementary light. J Dent. 2009;37(11):840-847.
7. Lee SS, Kwon SR, Arambula M, et al. Assessment of whitening efficacy of two in-office professional bleaching regimes. Center for Dental Research, Loma Linda University. International Association for Dental Research. March 2013.
8. Young N, Fairley P, Mohan V, Jumeaux C. A study of hydrogen peroxide chemistry and photochemistry in tea stain solution with relevance to clinical tooth whitening. J Dent. 2012;40 suppl 2:e11-e16.
9. Haywood VB, Caughman WF, Fraizer KB, Myers ML. Tray delivery of potassium nitrate-fluoride to reduce bleaching sensitivity. Quintessence Int. 2001;32(2):105-109.
10. Ochiai K, Sung EC, Chung J, Caputo AA. Effect of remineralizing agents on enamel microhardness after bleaching. J Dent Res. 2007;86(spec iss A).
11. Park S, Kwon SR, Qian F, Wertz PW. The effect of delivery system and light activation on tooth whitening efficacy and hydrogen peroxide penetration. J Esthet Restor Dent. 2016;28(5):313-320.
12. Croll TP, Donly KJ. Tooth bleaching in children and teens. J Esthet Restor Dent. 2014;26(3):147-150.
13. Charakorn P, Cabanilla LL, Wagner WC, et al. The effect of preoperative ibuprofen on tooth sensitivity caused by in-office bleaching. Oper Dent. 2009;34(2):131-135.