You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
The American College of Prosthodontists reports that about 178 million men and women are missing at least one tooth and about 40 million adults have no natural teeth.1 The most common reasons for losing a tooth, multiple teeth, or an entire set of teeth are dental decay (cavities), gum and bone disease, and trauma.1 Today, a dental implant is the first choice of treatment because it is predictable and offers a long-lasting solution. Unlike removable dentures that rest on the gum line, dental implants are a long-term treatment that is surgically implanted into the jaw. The implanted, artificial teeth look like real teeth and have the same functionality as real teeth. They are a more permanent solution to ordinary dentures and bridgework. When properly placed, dental implants have a very high success rate, about 98%.1 This article will help restorative dentists gain a thorough understanding of some of the best practices for achieving functionally esthetic implant restorations. It will focus in particular on the author's method of using a "restorative address."
Data from the National Health and Nutrition Examination Survey found that nearly 19% of adults aged 65 and older were edentulous, with a similar rate of prevalence in both men (18%) and women (19%).2 An obvious reason that people lose teeth is the presence of severe rampant caries. Periodontal disease is one of the most common reasons for adults in the United States to lose their teeth. According to the World Health Organization, severe periodontal disease is found in 15% to 20% of middle-aged (35 to 44 years) adults.3 Understanding the cause of the decay, whether it be trauma, diet issues, hygiene issues, or systemic or metabolic issues, is a critical first step. If an implant is made before the cause of the decay is taken into account, the success of the implant is at risk.
The Fundamentals of Implants
There are many reasons for a patient to get an implant. Replacing a tooth, or teeth, can provide a patient with the confidence to smile and the ability to eat normally again. Implants may also help preserve bone and prevent further deterioration of the facial structure. Alternatives to implants, such as dentures and bridges, may interfere with day-to-day activity.4 Dental implants are a long-term, cost-effective solution that, with proper care and periodic adjustments, can last a lifetime when placed properly. More than 1,300 types of dental implants are now available with different materials, shapes, sizes, lengths, and surface characteristics or coatings.5
Bone quality and quantity, implant geometry, and the chosen surgical technique adopted may significantly influence primary stability and the overall success rate of dental implants.6 Implants immediately placed into fresh extraction sockets and healed ridges have similar survival rates.7,8 Overall success rates differ, and the range is not entirely random. Patients with a history of periodontitis may have lower implant survival rates than patients without a history of periodontitis, and they are more prone to biologic complications such as peri-implant mucositis and peri-implantitis.9 Much of the success is in the hands of the dentist and oral surgeon.
For any implant procedure, successful implant integration is a prerequisite. This criterion depends on a series of procedure-related and patient-dependent measures.10 From a clinical standpoint, successful osseointegration is a measure of implant stability that occurs after implant integration.11 Primary stability is associated with the mechanical engagement of an implant with the surrounding bone. Secondary stability is determined by bone regeneration and remodeling.12 The extent of implant stability may also depend on the quality of surrounding tissue.13 Therefore, bone quantity and quality, implant geometry, and the surgical technique adopted are among the predominant clinical factors that affect primary stability.14 The author's method takes these factors into consideration and focuses on developing the best plan to approach implants.
Restorative Address 73-422
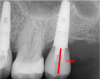
The author teaches "restorative address 73-422," a metaphorical street address, as the best method to help navigate an implant start to finish, where each number corresponds to a significant measurement. These measurements can be viewed by looking at the cross-section of a cone-beam computed tomography (CBCT) scan. The first number in the address, "7," represents the distance that the restorative platform should be from the desired occlusal table (Figure 1). An abutment 5 mm in length will minimize the chances of the restoration dislodging from the abutment. Then, above coronal to the abutment, there should be 2 mm of restorative material to ensure a strong restoration that will not fracture or break. Together, the abutment length of 5 mm plus the 2 mm of restorative material equals 7 mm. If the distance between the restorative platform of the implant abutment and the desired occlusal table is less than 7 mm, it will be difficult to mask out the screw-access hole and may result in an unsightly gray dot in the middle of the implant restoration (Figure 2). If the distance is slightly greater than 7 mm, that is acceptable, but it should not be less.
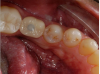
The next set of numbers is "3-4," which represents how far apically the restorative platform should be from the buccal-gingival margin. Measuring down 4 mm from the buccal-gingival margin helps get the implant into the desired position (Figure 3). However, a range of 3 to 4 mm is given because the measurement may vary depending on the condition of the site. In the case of a completely healed site, the restorative platform should be just 3 mm below the gingiva. But in a circumstance of immediate placement, 4 mm is better because, on average, 1 mm of bone on the buccal crest of the extraction site may be lost. Another reason for the distance of 3 to 4 mm is to allow room to create the right type of contour so that gingival tissue can be supported and a natural-looking soft-tissue esthetic can be created. When measuring the apical distance between a restorative platform and the buccal-gingival margin, it is better to err on the side of going slightly too deep because if too shallow, it will be difficult to create the type of subgingival contour that will support the tissue well. In other words, it would be difficult to get good esthetics. A ridge lap over the gingival margin is not a good idea because it may create an area that is difficult to properly clean and thus runs the risk of developing peri-implant mucositis or peri-implantitis. The situation could then result in the recession and loss of bone and/or terrible esthetic results. Furthermore, because many mechanical variables are present in the oral cavity, the proper measurement between the implant and the bone is important for treatment planning and longevity of the implant.15
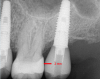
The next number is "2," which also refers to the distance between the restorative platform and the buccal-gingival margin, but for how far lingual the platform should be from the margin (Figure 4). With this measurement, similarly, it is better to err on the side of slightly greater than 2 mm as long as the trajectory of the implant is maintained to allow the screw access to come out of the central fossa. Too short a distance could result in an implant that has too little or no bone at all around the facial aspect of the implant. Such a situation would run the risk of having recession and ultimately even exposure of the implant and unpleasing long-term esthetics.
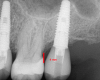
The final number "2" refers to the distance of the implant platform from adjacent teeth (Figure 5). According to the author, 2 mm is preferable here to the traditional distance of 1 to 1.5 mm taught in many schools because the goal is to create natural-looking soft tissue around the implant. Using a 2-mm distance allows the creation of contours that produce natural-looking papilla that can completely fill the gingival embrasure to avoid leaving a black triangle or food trap.
Additional Considerations
Although the main part of the address ends at this point, there is one more important number, a metaphorical apartment number: "4." The contact area should start within 4 mm of the crest of the bone between the two teeth (Figure 6). This is key to achieving quality tissue and thus esthetically pleasing restorations, whether the procedure is a veneer on anterior teeth or an implant.
It is important to note that many implant companies have changed their design to what is known as platform shifting or switching. Platform switching is a method for preserving crestal bone around the top of wide-diameter implants.16 It is used to account for changes in crestal bone height. Several theories exist as to the reason for the observed changes in crestal bone height after implant restoration. Some experts believe that when dental implants are placed into function, crestal bone remodels as a result of stress concentration at the coronal region of the implant.17 Others have suggested that post-restorative crestal bone remodeling occurs from localized inflammation within the soft tissue located at the implant-abutment interface as a result of the soft tissue's attempt to establish a mucosal barrier.18 Platform switching provides the clinician with additional surgical and prosthetic treatment options for use with wide-diameter implants. It alters the starting point from which the crestal bone remodeling occurs. As a result, the restorative address would change from 73-422 to 83-422 because the platform may shift about 1 mm, meaning the implant itself would need to be 8 mm apical to the desired occlusal table. A dental surgeon should be aware of this possibility, which is an example of the need to have clear, constant communication between the dentist and surgeon.
Communication Is Key
A dentist should have consistent, detailed communication with both the dental surgeon and the patient. There are three key steps to ensuring reliable communication. First, start with the why: why does the patient have occlusal disease or decay? Second, create a wax mock-up and use it to make a surgical guide for the surgeon using the restorative address. Third, be the leader in the implant process by using thorough, clear communication. When communicating with the surgeon, it is important to ask questions about the specifics of the dental implants and keep written documentation, using referral forms and surgical reports, of all the steps and idiosyncrasies being considered with each procedure. Providing the surgeon with a surgical guide is ideal.
The Value of a Surgical Guide
For those with access to CBCT technology and intraoral scanners, a 3-dimensional guide is easier to create. For those without the technology, it is still possible to create a simple analog surgical guide using the preoperative study models and a wax-up study model. A solid model duplicate of the wax-up model should be created along with a thermoplastic suck-down matrix over it. The latter should be trimmed, with extreme precision when trimming the buccal-gingival margin of the tooth that is going to replace the empty space. Then the central groove of the stent in the area of the wax-up tooth should be cut down. The lingual portion of the stent in that area should be removed so the surgeon can use the model by placing it in the patient's mouth. Not only can it assist in holding the flap of tissue back from the surgical site, it also enables the surgeon to use a periodontal probe to measure directly using the restorative address. By knowing exactly where the buccal-gingival margin is, the surgeon can measure 2 mm from that spot to understand where the buccal aspect of the implant platform should be. The surgeon can then measure vertically from the occlusal table and ensure the implant platform is placed deep enough to allow for functionally esthetic restoration. Thus, the restoration address is a tool for both the dentist and surgeon. It acts as a roadmap to avoid mistakes.
Conclusion
The insertion of implants is usually associated with a low incidence of undesirable events. However, despite careful planning, surgical complications can arise: infection, intraoral hemorrhage, wound dehiscence, postoperative pain, lack of primary implant stability, inadvertent penetration into the maxillary sinus or nasal fossa, sinus-lift sequelae, neurosensory disturbances, injuries to adjacent teeth, tissue emphysema, and aspiration, or ingestion of surgical instruments.19 Proper presurgical planning can greatly reduce the risk of complications. The restorative address described above is a method designed to help secure a successful implant. Additionally, clear communication with the surgeon and postsurgical checkups with the patient help mitigate risks.
References
1. American College of Prosthodontists. Missing Teeth. https://www.prosthodontics.org/assets/1/7/ACP_Talking_points_for_Missing_Teeth_1-12-15.pdf. Accessed November 28, 2017.
2. Dye B, Thornton-Evans G, Li X, Iafolla T. Dental caries and tooth loss in adults in the United States, 2011-2012. NCHS Data Brief. 2015; No. 197.
3. World Health Organization. Oral health. Fact sheet No. 318. http://www.who.int/mediacentre/factsheets/fs318/en/.Published April 2012. Accessed November 28, 2017.
4. American Academy of Implant Dentistry. Dental Implants: Everything you need to know about dental implants. https://www.aaid-implant.org/about-dental-implants/what-are-the-benefits-of-dental-implants-over-other-treatments/. Published 2013. Accessed November 28, 2017.
5. Esposito M, Ardebili Y, Worthington HV. Interventions for replacing missing teeth: different types of dental implants. Cochrane Database of Systematic Reviews 2014, Issue 7. Art. No.: CD003815. doi: 10.1002/14651858.CD003815.pub4.
6. Romanos GE. Bone quality and the immediate loading of implants-critical aspects based on literature, research, and clinical experience. Implant Dent. 2009;18(3):203-209.
7.Lang NP, Pun L, Lau KY, et al. A systematic review on survival and success rates of implants placed immediately into fresh extraction sockets after at least 1 year. Clin Oral Implants Res. 2012;23(suppl 5):39-66.
8. Ortega-Martínez J, Pérez-Pascual T, Mareque-Bueno S, et al. Immediate implants following tooth extraction. A systematic review. Med Oral Patol Oral Cir Bucal. 2012;17(2):e251-e261.
9.Simonis P, Dufour T, Tenenbaum H. Long-term implant survival and success: a 10-16-year follow-up of non-submerged dental implants. Clin Oral Implants Res. 2010;21(7):772-777.
10. Javed F, Ahmed HB, Crespi R, Romanos GE. Role of primary stability for successful osseointegration of dental implants: Factors of influence and evaluation. Interv Med Appl Sci. 2013;5(4):162-167.
11. Natali AN, Carniel EL, Pavan PG. Investigation of viscoelastoplastic response of bone tissue in oral implants press fit process. J Biomet Mater Res B Appl Biomater. 2009;91(2):868-875.
12. Greenstein G, Cavallaro J, Romanos G, Tarnow D. Clinical recommendations for avoiding and managing surgical complications associated with implant dentistry: a review. J Periodontol. 2008;79(8):1317-1329.
13. Javed F, Almas K. Osseointegration of dental implants in patients undergoing bisphosphonate treatment: a literature review. J Periodontol. 2010;81(4): 479-484.
14. Romanos GE. Bone quality and the immediate loading of implants-critical aspects based on literature, research, and clinical experience. Implant Dent. 2009;18(3):203-209.
15. Suedam V, Moretti-Neto RT, Sousa EAC, Rubo JH. Effect of cantilever length and alloy framework on the stress distribution in peri-implant area of cantilevered implant-supported fixed partial dentures. J Appl Oral Sci. 2016;24(2):114-120.
16. Lazzara RJ, Porter SS. Platform switching: a new concept in implant dentistry for controlling postrestorative crestal bone levels. Int J Periodontics Restorative Dent. 2006;26(1):9-17.
17.Pilliar RM, Deporter DA, Watson PA, Valiquette N. Dental implant design--effect on bone remodeling. J Biomed Mater Res. 1991;25(4):467-483.
18. Erricson I, Persson LG, Berglundh T, et al. Different types of inflammatory reactions in peri-implant soft tissues. J Clin Periodontol. 1995;22(3):255-261.
19. Al-Faraje L. Surgical Complications in Oral Implantology: Etiology, Prevention, and Management.Quintessence Pub Co; 2011.