You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
According to the 2010 United States (US) census, the US continues to be more culturally diverse which subsequently creates an increasingly diverse population of patients for oral healthcare providers.1 In order to treat, counsel and communicate with diverse patient populations, oral healthcare providers must be culturally competent.2 As oral healthcare providers, dental hygiene students must have knowledge, understanding and appreciation for a wide variety of cultures, beliefs and customs in order to provide quality oral care for diverse populations.3
Dental hygiene, according to the US Bureau of Labor and Statistics, is one of the fastest growing professions in the US and the number of dental hygienists is projected to increase by approximately 38% between the years 2010-2020.4 In spite of this projected growth of the profession within an increasingly diverse general population, demographics on the current workforce indicate that dental hygiene is the least culturally diverse of all healthcare providers. According to data from the U.S. Department of Health and Human Services, 85% of dental hygienists are Caucasian and 97.2% are female; leaving the profession severely lacking in diversity.5 If this lack of diversity continues, the profession may be ill-prepared to treat patients of differing cultures.3 A more culturally diverse dental hygiene workforce has the potential of being both beneficial to the profession as well as the increasingly diverse population at large. While increasing the cultural diversity of the workforce may be part of a solution, promoting cultural competence within the dental hygiene workforce is essential. Failure to develop culturally competent oral healthcare providers may compromise the quality of and access to care, limit patient resources, threaten patient safety and perpetuate oral health disparities.2,3
Cultural Competence
Betancourt and colleagues define cultural competence as, “understanding the importance of social and cultural influences on patients' health beliefs and behaviors; considering how these factors interact at multiple levels of the health care delivery system (e.g., at the level of structural processes of care or clinical decision-making); and, finally, devising interventions that take these issues into account to assure quality health care delivery to diverse patient populations.”2
The dental hygiene profession has not ignored the growing need for cultural competence. A set of core competencies for graduate level dental hygiene programs established collaboratively by the American Dental Hygienists' Association (ADHA) and the American Dental Education Association (ADEA) addresses ability of graduate dental hygiene students to engage and interact with individuals and groups across and within diverse communities and cultures in an effective and respectful manner.6 Entry level education also includes a cultural competence knowledge base. The Commission on Dental Accreditation Standards for dental hygiene addresses the student's ability to treat diverse populations in Standard 2-15: “Dental hygienists should recognize the cultural influences impacting the delivery of health services to individuals and communities (i.e. health status, health services and health beliefs).”7 Dental hygiene education must include effective communication and treatment of patients of various cultures and backgrounds in their curriculum.
A recent survey of dental hygiene program directors showed that 92% of dental hygiene program respondents reported incorporating some form of cultural competency education into their curriculum; the most common form was via lectures. It is also noteworthy that while cultural competency is part of the curriculum, measurements of cultural competence outcome indicators are rarely evaluated.8 There are examples of cultural competency education in the literature. Doucette et al found that implementing a tobacco dependence education (TDE) curriculum with a cultural competence component increased dental hygiene students' cultural knowledge. However, while the study results indicated an increase in the student's knowledge of the culture of First Nations and Inuit peoples, it is unclear whether the students felt better prepared to provide TDE to this population and the authors acknowledged the need to implement additional learning experiences with cultural competence components to better facilitate student levels of preparedness.9 Dewald and Solomon assessed the cross-cultural adaptability of dental hygiene students by administering the Cross-Cultural Adaptability Inventory (CCAI) at the beginning and at the end of the 2-year dental hygiene curriculum and found no significant differences in the four skill areas assessed in the CCAI. Students did not receive any specific cultural competency training module intervention nor did they receive their CCAI results until after completing the dental hygiene program which may indicate that clinical experiences alone are not enough to increase cultural competence in students.10
Looking beyond examining the cultural competence of students, Behar-Horenstein et al, surveyed cultural competence of allied dental educators in Florida by administering the Knowledge, Efficacy and Practices Instrument (KEPI), a validated measure of cultural competence. Survey results demonstrated that while allied dental faculty have a greater awareness of sociocultural and linguistically diverse dental patients' oral health needs than that of dental faculty members, their scores in several areas of cultural competence indicated need of moderate to more intense training.11 Current literature indicates that further research in the areas of training and evaluation of cultural competence is warranted.
Assessing Cultural Knowledge and Competence
In April of 2014, the US Department of Health and Human Services (HHS), Office of Minority Health (OMH) launched a three-module online training program specifically for oral health professionals: The Think Cultural Health Initiative; a component of the Cultural Competency Program for Oral Health Professionals.12 The purpose of the free, self-paced online program is to provide oral health professionals with basic knowledge and skills related to cultural and linguistic competencies based on the HHS Office of Minority Health National Standards for culturally and linguistically appropriate services in health and health care (CLAS Standards). This training tool serves to inform oral health professionals about the variety of cultures, traditions, beliefs, and customs of the diverse population that they will encounter in practice and provide a respectful appreciation for all individuals regardless of culture.12 The program is broken down into three online modules consisting of a pretest, an information component and video followed by a post test. The three modules are as follows: Fundamentals of Culturally and Linguistically Appropriate Oral Health Care; Providing Culturally and Linguistically Appropriate Oral Health Care; Culturally and Linguistically Appropriate Communication and Messaging.12 The training modules have added features to enhance the learning experience including additional resources, questions, culturally specific information, and video vignettes. Participants achieving scores of 70% or higher on all three post-tests receive a certificate serving as proof of successful completion of the course which also provides the oral health professional with six hours of continuing education.12
Studies addressing cultural competence assessment in health care providers often use self-administered tools and with inconsistent measurements lacking validation.13 A systematic review of the literature documents over 45 variations of such instruments.13,14 The Inventory for Assessing the Process of Cultural Competency among Health Professionals- Student Version (IAPCC-SV) as developed and copyrighted by Campinha-Bacote is a 20-item pencil/paper validated self-assessment tool for measuring the healthcare student's self-perceived levels of cultural competence in five constructs.15,16 Cultural awareness as defined by Campinha-Bacotec is the process of conducting self-examination of one's own biases towards other cultures and an in-depth exploration of one's own cultural and professional background and one's own biases towards other cultures.15,16 Campinha-Bacotec describes cultural knowledge as the process in which the healthcare professional seeks out a sound knowledge base about culturally diverse groups while integrating the following as defined by Lavizzo-Mourey and MacKenzie: health related beliefs, practices and cultural values, disease incidence and prevalence of disease.15-17 Cultural skill, according to Campinha-Bacotec is the ability to conduct an assessment in order to collect relevant cultural data regarding the client's presenting problem in addition to conducting an accurate culturally-based physical assessment.15,17 Cultural encounters, are defined as the process by which the healthcare professional engages in face-to-face cultural interactions as well as other encounters with clients from culturally diverse backgrounds in an effort to modify any existing beliefs about a cultural group and to prevent stereotyping.15,17 The survey identifies cultural encounters as the pivotal construct of cultural competence.15,17 Lastly the fifth construct, cultural desire, is defined as the healthcare professional's desire to become freely engaged in the process of becoming culturally aware, knowledgeable and skillful in seeking cultural encounters.15,17
Oral health care providers must possess knowledge of cultural competence in order to meet the needs of diverse groups of patients and provide services in a culturally and linguistically appropriate manner. There is potential for HHS Think Cultural Health Initiative online course modules and the IAPCC-SV measurement tool to be used in dental hygiene education programs as parts of their cultural competence curriculum. Currently there are no published studies on the effectiveness of the HHS OMH modules for oral health care providers and knowledge of cultural competence. The purpose of this study was to measure the change in scores of self-perceived levels of cultural competence of senior level dental hygiene students after the implementation of an online training module designed to increase knowledge of cultural competence.
Methods
This study used a pre-test, post-test design with a prospective cohort. Participants were recruited from the 31 senior dental hygiene students at Ohio State University, School of Dentistry. The study received an exempt status from the University's Institutional Review Board. The students attended an informational session explaining the study. Following the informational session, students were invited to participate and informed consent was obtained from 28 out of 31 of the senior dental hygiene students. Students took the Inventory for Assessing the Process of Cultural Competency among Health Professionals- Student Version (IAPCC-SV), a 20-item, copyrighted, fee-based, survey instrument as a pre-test. The IAPCC-SV as developed by Campinha-Bacote is specifically designed to assess students' perceived cultural competence levels in five specific areas or constructs: Cultural Awareness, Cultural Knowledge, Cultural Skill, Cultural Encounter and Cultural Desire. Specific questions on the survey are related to each construct. The validity and reliability of this instrument has been established previously in the literature.15,16
The IAPCC-SV is designed so that specific questions are designed to assess the level of each of the specific constructs. Each response is given a point value. For questions 1-13 and 15-20 the values are as follows: strongly agree=4 Points, agree=3 Points, disagree=2 Points, strongly disagree=1 Point. Question 14 uses a reverse coding system and the point values are as follows: strongly disagree=4 Points, disagree=3 points, agree=2 Points, strongly agree=1 Point. Once a number value has been assessed for a student's responses, a level of cultural competence can be established. Culturally proficient is defined as a total score of 75-80, culturally competent 60-74, culturally aware 41-59 and culturally incompetent 20-40. The pre-test survey established a baseline level of knowledge and a level of cultural competence for each student.
Upon completion of the pre-test, students were instructed to complete the US Department of Health and Human Services (HHS) Office of Minority Health (OMH) Cultural Competency Program for Oral Health Professionals.13 Students were given two full weeks to complete the online training modules. Following the completion of the three modules and posttest, students received an email from the Office of Minority Health Cultural Competency Program confirming completion of the three-course program. To verify completion of the online training modules, the students sent their course confirmation email to the program director. Three weeks following the pre-test, the students completed the IAPCC-SV posttest survey, which was used to establish the level of knowledge of cultural competence following the completion of the HHS OMH online modules. Data was analyzed using JMP 10 (SAS Institute, Cary, NC). The IAPCC-SV pre-test and post-test results were analyzed using descriptive statistics, a paired t-test and Wilcoxon Signed-rank test.
Results
Twenty-eight (N=28) out of 31 senior dental hygiene students agreed to participate in the study. Individual demographic information was not asked of each participant but the class as a whole from which the sample was drawn had a mean age of 22 years with a range of 20-49 years. Ninety percent of the class was female and 87% of the class was Caucasian. Ninety-four percent of the class were domestic students (US citizens) and 6% indicated international citizenship. Twenty-eight surveys were distributed and completed for both the pre-test and the post-test. One participant's survey was missing a response on both the pre-test and the post-post. Therefore, for the specific constructs of Cultural Encounters and Cultural Knowledge, only 27 surveys were utilized.
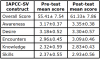
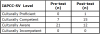
The average score on the pre-test was 55.41(±7.54) while the average score on the post-test was 61.33(± 7.86) (Table I). No students fell into the culturally incompetent category on either the pre-test or the post-test (Table II).
The mean change in overall score from pretest to post-test was 5.79. Two students had post-test scores that were lower than pre-test scores, but both stayed within the same level of cultural competency from pre-test to post-test despite the lower scores. There were also two students who scored equally on the pre- and post-tests. The greatest overall score increase was 17 points. Scores were also evaluated by construct (Table I).
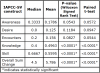
After assessing normality of the data, the paired t-test and the Wilcoxon signed rank tests were used to determine if there were differences in the level of knowledge of cultural competence before and after the modules were completed. There was a statistically significant difference in the pre-test to post-test scores in the constructs of knowledge (p<0.001), skill (p<0.001) and overall sum (p<0.001) (Table III).
Discussion
According to the results from the IAPCC-SV survey, the pre-test results indicated that the majority of the senior dental hygiene students started at the self-perceived level of being culturally aware. After completing the online HHS OMH training modules and then taking the post-test the students increased their self-perceived levels of cultural competency on the IAPCC-SV survey, with the majority of the students at the scoring level of culturally competent. One students score was rated at the highest level of cultural competency: culturally proficient.
The dental hygiene students' mean score for the pretest was 55.14, which falls within the level of culturally aware according to the scaling of the IAPCC-SV. This finding was not surprising as senior dental hygiene students have received some instruction in cultural competence at various points in the curriculum and have likely experienced interactions with patients from different cultural backgrounds than their own.
In a study by Hawala-Druy et al, health professions students including nursing, pharmacy and allied health were enrolled in an interdisciplinary course designed to provide the necessary knowledge and skills through transformative learning experiences to provide culturally appropriate team-based patient care to diverse populations.18 Student's levels of cultural awareness, competency and proficiency were measured with the IAPSS-SV both prior to and following the educational intervention. Additional evaluation measures included course evaluations, student feedback and portfolio reflections. Results from the pre and post IAPSS-SV surveys indicated a significant increase in the mean scores from the pre-test mean of 60.8 to the post test mean of 70.6.18 While Hawala-Druy et al and this study both used the IAPSS-SV instrument and demonstrated an increase in the mean scores of cultural competence, the change in the scores for the dental hygiene students was 5.79 as compared to a change of 10.8 points with health professions students.18 It is important to note that the single intervention for the dental hygiene students was the online HHS OMH training program administered over a two-week time period while the Hawala-Druy et al studied the effects of a semester-long, interprofessional education course.
In this study, the constructs of knowledge and skill showed the most significant increases in the comparison of the IAPSS-SV pre- and post-test mean scores, 0.496 and 0.560 respectively. Significant increases in these categories may be due to the focus of the HHS OMH online training modules on increasing the knowledge and skills of cultural competency with videos, information along with ways to communicate to achieve culturally and linguistically appropriate oral health care and services (CLAS).
Additional studies cite the challenges of measuring cultural competency within the curriculum.19-21 Palombaro et al used the IAPSS-SV to measure the development of cultural competence in physical therapy students over a three-year curriculum with students participating in both mandatory and voluntary experiential learning opportunities that included experiences in a student-run pro bono clinic. Required didactic classroom presentations and activities were also integrated throughout the curriculum. Palombaro et al found that there was an overall improvement in self-assessed cultural competence as a result of a combination of curricular activities with a special emphasis on service learning and cultural encounters. These findings support the construct that the cultural encounters provide that foundation for each individual healthcare provider's journey towards cultural competence.19
Measuring and comparing cultural competence, even when similar instruments are used can be challenging. Studies conducted on the curricular integration and measurement of the development of cultural competency in physical therapy students do not differentiate between the various constructs and the changes in the pre- and post-test scores for each construct.19,20 Only the overall mean change is examined and reported.19-21 This limits the ability to compare previous study results with this study.
Limitations to this study include the sample was only comprised of 28 senior level dental hygiene students at one institution. This was a small, homogenous group and it is difficult to generalize the results as applicable to all dental hygiene programs. This study should be repeated in other dental hygiene programs to further validate the tool in improving cultural competence in the dental hygiene student population.
This pre-test, post-test design within one cohort of students did not allow for a control group. It is unclear whether the HHS OMH training modules or if time, experiences or other external factors over the two-week period influenced the levels of change in cultural competence. Future work should include a control group that does not complete the HHS OMH modules. While some cultural competency studies have tracked the longitudinal effects of specific interventions,21 this study only looked at the measurement of cultural competence changes over a two-week period of time. Tracking the students' levels of cultural competence over longer periods of time may show how the levels change with ongoing training and experience.
Another limitation was that there was no way to measure the amount of time the students spent on the HHS OMS website. The students were instructed to work on the online training modules independently outside of the classroom and submitted an email indicating completion of the training modules. If the students did not work through the information completely and just completed the post-test at the end of each module, the full impact of the training modules may not have been reflected in their overall scores. Using the training modules within the context of a course would help to ensure more complete participation in all aspects of the modules.
The authors of this study recognize that cultural competence is a multi-faceted construct and one online training program is not adequate to meet the needs of a very diverse patient population. Clinical and community experiences that students have throughout their curriculum also contribute to their levels of cultural competence and patient feedback and health outcomes are critical components of culturally competent oral health care. This study aimed to examine one novel program's effects and it is not suggested that this be the sole content for cultural competence in the dental hygiene curriculum. The HHS OMH training modules can serve as an ideal starting point for the topic are an excellent resource for dental and allied dental educators to address cultural competence in an oral health context.
Future research would include a larger, more diverse sample size, a control group and the ability to track the amount of time spent on the training modules possibly by incorporating the training modules into the dental hygiene curriculum.
Conclusion
Culturally competent dental hygiene care is becoming increasingly more important as the population of the United States becomes more diverse. Dental hygiene accreditation (CODA) standards required that students recognize cultural influences that impact the delivery of healthcare. This study examined the effects of knowledge acquired via the online HHS OMH Cultural Competency Program for Oral Health Professionals as compared to pre- and post-tests of self-perceived levels of cultural competence as measured by the Inventory for Assessing the Process of Cultural Competency among Health Professionals-Student Version (IAPCCSV). While this single HHS OMH training program and IAPCC-SV student post-tests do not serve as sole indicators of cultural competency, the results of this study demonstrate that the HHS OMH Cultural Competency Program for Oral Health Professionals was effective for increasing dental hygiene students' levels of knowledge of cultural competence.
About the Authors
Heather N. Daugherty, RDH, BSDH is the EFDA Clinical Coordinator and clinical dental hygiene instructor; Dental Hygiene Clinical instructor; Rachel C. Kearney RDH, MS is an assistant professor and chair; both in the Division of Dental Hygiene, The Ohio State University College of Dentistry, Columbus, OH.
Corresponding author: Rachel C. Kearney RDH, MS;
Kearney.19@osu.edu
References
1. U.S. Census Bureau. 2010 census shows America's diversity. [Internet]. Washington (DC): U.S. Census Bureau; 2011 March 25 [cited 2016 Aug 24]. Available from: https://www.census.gov/newsroom/releases/archives/2010_census/cb11-cn125.html.
2. Betancourt JR, Green AR, Carrillo JE, et al. Defining cultural competence: a practical framework for addressing racial/ethnic disparities in health and health care. Public health reports. 2016 Nov 15;118(4):293-302.
3. Newcomb TL, Sokolik TL. Cultural competence: How to incorporate different cultural beliefs and practices into the dental hygiene process of care. Dimensions. 2012 Apr;10(4):58-61.
4. U.S. Bureau of Labor Statistics. Dental hygienists: occupational outlook handbook [Internet]. Washington (DC): US Bureau of Labor Statistics; 2015 Dec 17 [cited 2016 Aug 24]. Available from: https://www.bls.gov/ooh/healthcare/dentalhygienists.htm.
5. U.S. Department of Health and Human Services. The U.S. health workforce chartbook part I: clinicians [Internet]. Rockville (MD): US Department of Health and Human Services; 2013 Nov [cited 2016 Aug 24]. Available from: https://bhw.hrsa.gov/sites/default/files/bhw/nchwa/chartbookpart1.pdf.
6. American Dental Hygienists Association. Core competencies for graduate dental hygiene education [Internet]. Chicago (IL): American Dental Hygienists Association; 2011[cited 2016 Aug 24]. Available from: https://www.adha.org/resources-docs/72610_Core_Competencies_for_Graduate_DH_Education.pdf.
7. Commission on Dental Accreditation. Accreditation standards for dental hygiene education programs [Internet]. Chicago (IL): 2016 [cited 2016 Aug 24]. Available from: http://www.ada.org/~/media/CODA/Files/dental_hygiene_standards.pdf?la=en.
8. Ocegueda DR, Van Ness CJ, Hanson CL, et al. Cultural competency in dental hygiene curricula. J Dent Hyg 2016 Jun;90 Suppl 1:5-14.
9. Doucette HJ, Maillet PJ, Brillant MG, et al. Dental hygiene students' perceptions of a cultural competence component in a tobacco dependence education curriculum: a pilot study. J Dent Educ. 2015 Jun;79(6):680-5.
10. DeWald JP, Solomon ES. Use of the cross-cultural adaptability inventory to measure cultural competence in a dental hygiene program. J Dent Hyg. 2009 Jun; 83(3):106-10.
11. Behar-Horenstein LS, Garvan CW, Catalanotto FA, et al. Assessing cultural competence among Florida's allied dental faculty. J Dent Hyg. 2016 Jun; 90(3):192-6.
12. U.S. Department of Health and Human Services. Think cultural health: cultural competency program for oral health professionals [Internet]. Rockville (MD): U.S. Department of Health and Human Services; 2015 [cited 2016 Aug 24]. Available from: https://oralhealth.thinkculturalhealth.hhs.gov/.
13. Gozu A, Beach MC, Price EG, et al. Self-administered instruments to measure cultural competence of health professionals: a systematic review. Teach Learn Med. 2007 May 25;19(2):180-90.
14. Lin CJ, Lee CK, Huang MC. Cultural competence of healthcare providers: a systematic review of assessment instruments. J Nurs Res. 2017 Jun 1;25(3):174-86.
15. Campinha-Bacote, J. Inventory for assessing the process of cultural competence among healthcare professionals – student version [Internet]. Cincinnati (OH): Transcultural C.A.R.E Associates; 2015 [cited 2016 August 24]. Available from: http://transculturalcare.net/iapcc-sv/.
16. Capinha-Bacote, J. The process of cultural competence in the delivery of healthcare services; a model of care. J Transcult Nurs. 2002 Jul; 13(3):181-4.
17. Lavizzo-Mourey, RJ, MacKenzie E. Cultural competence—an essential hybrid for delivering high quality care in the 1990's and beyond. Tran Am Clin Climatol Assoc. 1996; 107:226-35.
18. Hawala-Druy S, Hill MH. Interdisciplinary: Cultural competency and culturally congruent education for millennials in health professions. Nurse Educ Today. 2012 Oct 31;32(7):772-8.
19. Palombaro KM, Black JD, Dole RL, et al. Curricular integration and measurement of cultural competency development in a group of physical therapy students. Journal of the Scholarship of Teaching and Learning. 2015 Oct 31;15(5):82-96.
20. Okere SD, Gleeson P, Mitchell K, et al. The effects of a cultural competence education module on the cultural competence of student physical therapists: A double-blind, randomized controlled trial. Paper presented at: American Physical Therapy Association Annual Conference and Exposition;2012 Tampa, FL.
21. Sanner S, McAllister LE. A longitudinal study of cultural competence among health science faculty. J Cult Divers. 2010 Jul 1;17(2):68.