You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Identification of the Human Papillomavirus (HPV) as a causal agent for oropharyngeal cancers has prompted public health interests. The oral HPV infection prevalence among U.S. adults was estimated to be 6.9% in 2009-2010.1 Moreover, approximately 72% of oropharyngeal cancers are associated with HPV and 62% are attributed to HPV types 16 and 18.2,3 As a result, it is estimated that approximately 11,000 oropharyngeal cancers each year in the U.S. are attributed to HPV. From 2008 to 2012, oropharyngeal cancers were the second most common HPV-associated cancer in the U.S.4 Furthermore, evidence indicates that HPV-related oropharyngeal cancer rates are increasing and expected to surpass rates of HPV-related cervical cancer in the U.S. by 2020.5 The HPV vaccine is a primary prevention activity related to HPV and cancer. This vaccine, although not currently approved for the prevention of oropharyngeal cancer, is now recommended for routine vaccination of children between the ages of 11-to-12. It is also recommended for “catch-up” vaccination for females 13-to-26 years old, and for males 13-to-21 years old and 22-to-26 years old for “high-risk” populations.3,6
The American Dental Association advises dental providers “to educate themselves and their patients about the relationship between HPV and oropharyngeal cancer.”7 Given the evolving role of oral health care providers in the prevention of HPV and HPV-related oropharyngeal cancers,8,9 an assessment of oral health care providers’ current knowledge and communication skills is needed. One framework to assist this investigation is health literacy, which is the skill-based process of accessing, understanding, appraising and applying health information to make informed health decisions.10 Health literacy is not just knowledge regarding a topic; rather, it is the skills required to gather information, process it, and use it. Previous research has suggested that “health literacy is not just about individual patients, but also includes healthcare providers and other decision makers.”11 Furthermore, system-level factors can influence healthcare providers’ health literacy and decision-making. Thus, understanding and promoting the HPV-related health literacy of dental providers as agents and recipients of health literacy,12 can ultimately impact the health literacy of patients as well.
Dental hygienists, with their historical focus on prevention through the services they provide including screening examinations, preventive treatments and oral health education, are a unique group of oral health care providers. Dental hygienists can be part of the next group of health care providers involved in HPV-related cancer prevention programs and because of their training, have a unique position as educators and prevention specialists; however, little is known about dental hygienists’ HPV-related health literacy levels. The purpose of this qualitative study was to explore dental hygienists’ HPV-related health literacy as a means to inform the development of interventions promoting their unique ability to communicate HPV-related information to patients.
Methods and Materials
This study sample included dental hygienists licensed in the United States (U.S.) who were recruited via email to take part in focus groups conducted during a national dental hygiene conference in July 2015. Inclusion criteria included the following: (1) possess a current U.S. dental hygiene license; (2) be a graduate of an accredited dental hygiene program; (3) be in practice for more than one year; and, (4) be 21 years of age or older. The University of South Florida Institutional Review Board approved this study.
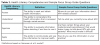
Focus groups13 were used to explore dental hygienists’ HPV-related health literacy. As such, the focus group guide was based on the following health literacy competencies as described by Sørensen and colleagues (2012): access; understand; appraise; and apply.10 Focus group questions addressed areas regarding HPV knowledge, sources of information, information usage, and barriers and facilitators to HPV discussion related to patients, practice and their profession (Table I). The focus group guide was reviewed for content validity by an expert panel composed of a dental hygienist, a dentist, and researchers with expertise in health literacy and HPV.
Each focus group was conducted with a trained moderator and a note-taker. Written informed consent was obtained from participants. A brief survey was administered to gather information on demographics (e.g., years in practice, gender, race/ethnicity, age). Each participant received a $100 gift card. All focus groups (N=4) were audio-recorded and transcribed verbatim. Focus groups lasted an average of 85 minutes.
When conducting focus groups, it is recommended to plan for three to four groups of similar composition, and to add more groups until saturation is reached.13 For this study, participants were recruited and focus groups were scheduled several months prior through the conference administrators; therefore, adding additional focus groups was not possible.
A codebook based on the focus group guide and health literacy competencies was created a priori. Using constant comparison methods, two researchers independently coded all the transcripts and met to discuss the coding process with areas of disagreement resolved by discussion.13,14 Data were entered into Atlas-ti version 6.2, and analyzed using the health literacy framework whereby general themes (i.e., competencies) emerged. Additional findings were also noted that may not have been reported across all groups, but describe the variability of participants’ perceptions. Exemplary quotes were selected for each theme or sub-theme found for these data. Three quotes were selected per theme, and two researchers came to consensus of the most representative quotations for data presentation.
Results
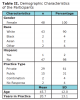
All participants (n=48) across the four focus groups were female, the majority Caucasian, and had an average of 20 years of experience (Table II). The health literacy skills based processes for making informed health decisions are presented according to each category.
Access
Participants were asked about sources from which they obtained information regarding HPV and HPV-related cancers. Participants mentioned a variety of sources where they get their information, including scholarly journals, continuing education courses, and during dental hygiene education. Dental hygienists who had been in practice longer reported they had not received information about HPV and HPV-related cancers during their training. Exemplary quotes are presented in Table III.
Participants in two focus groups mentioned using two well-known oral health advocacy websites as a source of information on both oral cancer and oral cancer screening. Similarly, other websites were mentioned in at least one focus group, including the websites of both the American Dental Hygienists’ Association and the Centers for Disease Control and Prevention. Other sources of information about HPV and HPV-related cancers that were less frequently discussed included the local news reports, magazines, social media and blogs, public service announcements, the participant’s personal medical doctors, and peers/colleagues. Participants in two of the focus groups mentioned the media coverage of the actor Michael Douglas’ revelation regarding his HPV-related oral cancer.
Understand
Dental hygienists were asked what they knew about HPV and the HPV vaccine. Participants discussed three thematic areas of understanding between HPV and oral cancer including: HPV infection, oral cancer and the connection to HPV, and knowledge of the HPV vaccine (Table III).
HPV infection. Regarding understanding HPV and the association to oral cancer, the majority of participants accurately described HPV as a sexually transmitted infection, oral sex as a mode of transmission, and the different strains of HPV. However, results revealed misunderstanding among participants about HPV treatment and cure, and the specific strains associated with oral cancer.
Oral cancer and the connection to HPV. Participants in all focus groups discussed the connection of the virus with oropharyngeal cancers. These discussions included the increased rates of HPV among young people who have less “traditional” risk factors (e.g., alcohol and tobacco use). Discussion in one group surrounded the perception that HPV-related cancers are more easily treated than “traditional” oral cancers attributable to smoking and alcohol.
Dental hygienists also discussed signs and symptoms associated with HPV-related oral cancers. Although participants accurately described that HPV lesions typically present farther back in the throat, making visual inspection difficult, the majority of participants in all groups reported a lack of knowledge in describing lesion appearance, triage, or referral sources.
The HPV vaccine. Whereas the existence of a vaccine to prevent HPV infection was acknowledged, participants in only three groups correctly identified that the vaccine is available for both males and females (participants in one group said the vaccine was approved only for females). Additionally, although it was not identified as a theme, two participants incorrectly reported the virus’ ability to “mutate,” impacting the vaccine’s ability to prevent HPV-related cancers.
Appraise
The appraisal process comprised a complex set of interrelated factors that dental hygienists consider prior to applying HPV-related information during discussions with patients. These factors were categorized into three broad levels: patient, practice, and professional (Table III).
Patient factors. Overall, dental hygienists mentioned that talking about sensitive topics depends on the individual patient. Patients’ age was the most common factor mentioned across all focus groups. Both younger and older age made it difficult for dental hygienists to engage in HPV-related communication. When referring to older patients, dental hygienists believed that the age difference tended to be a barrier for communication because older patients perceived the dental hygienist as inexperienced. Additionally, some dental hygienists felt uncomfortable engaging in “the sex talk” with older patients, while others felt that older patients need more education.
When dental hygienists referred to younger patients, their concerns were related to adolescents who they perceived as sexually active. Participants noted that discussing HPV-related oral cancer prevention with parents of underage patients raised two different concerns. First, parents of patients that they saw in clinic may believe that a discussion of any topic related to sexuality should be off-limits. Second, dental hygienists who work in school-based settings typically do not have contact with parents where they could engage in these types of conversations.
Another patient factor was specific risk status of the patient. For example, participants reported it was easier to talk about HPV and oral sex with people living with HIV, men who have sex with men, and homeless patients because dental hygienists perceived that these populations are concerned and interested in the information.
Other patient factors that hindered HPV-related communication include the conservative or religious background of the patient, some patients’ unwillingness to pay for some dental services, and language differences between the dental hygienist and the patient. However, dental hygienists also mentioned that there are patients that want to talk and establish a provider-patient relationship with them, thus making it easier for them to engage in HPV-related or sensitive topic conversations.
Practice factors. Practice factors discussed in the focus groups represent characteristics of the work environment that affect the dental hygienist’s ability to discuss HPV-related oropharyngeal cancer with patients, including: the dentist control of the office, characteristics of the dentist, and the physical setting of the office. Overall, participants in all groups mentioned the influence of the dentist in the practice and the need for their support.
In many cases, dental hygienists mentioned that the dentist is in control of the office, and this may have an impact on the discussion of HPV with their patients. For example, as one hygienist who had been in a dental practice for 10 years stated, “… it depends on your boss too, and the protocol, how the office runs.”
Another factor influencing the information discussed with patients is the age of the dentist, which may impact the information provided within the practice setting. Dental hygienists mentioned that young dentists more often support hygienists in educating their patients on HPV and performing oral cancer exams.
Another practice factor that may negatively influence discussion of HPV and HPV-related cancer with patients is a lack of privacy within the office setting. Participants in two focus groups mentioned the open layout of the office creating a situation where patients can overhear conversations. As a result, the lack of privacy, which they perceived as a patient’s concern, is a barrier to discussing sensitive topics.
Professional factors. Professional factors are those that relate to the dental hygiene profession in general. The discussion centered on improving perceptions of the dental hygiene profession and the need to be recognized as experts in oral healthcare. This conversation included the public’s perceptions of the hygienist’s role as a “cleaning lady” (mentioned in three groups) or a “mouth janitor” (mentioned in one focus group), and not being viewed as a healthcare professional.
Additionally, an unsolicited finding noted from these conversations is that of dental hygienists’ self-described role as “prevention specialists.” Across all four focus groups, dental hygienists discussed their role in the dental profession as that of prevention. The role includes a range of prevention behaviors, patient education, and secondary prevention of oropharyngeal cancers through oral cancer screenings.
Apply
Participants reported they used the information gathered from information sources with their patients. However, as noted above, most felt uncomfortable talking to their patients about the link between oral cancer, HPV, and sexual behaviors. This resulted in most participants not engaging in conversations with their patients to discuss HPV, HPV-related cancers, or HPV vaccine information. The few participants who did discuss this with their patients were more likely to do so during an oral cancer screening. During one of the focus group discussions, participants expressed they would be willing to talk and encourage HPV vaccination because it is related to prevention.
Participants felt confident doing the secondary prevention behavior of oral cancer screenings and were willing to take the time to educate their patients about HPV risks factors and overall health-related information. Some even provided suggestions about what to do and say while screening for oral cancer (Table III).
All groups discussed the necessity of the oral cancer screening at dental visits and suggested that this prevention behavior is of a higher importance than “cleaning teeth.” Additionally, many mentioned the need to change patients’ perceptions of the hygiene visit to focus on the oral cancer exam rather than just a dental cleaning.
Some dental hygienists reported questions from patients as to why they had never had an oral cancer exam performed before and why it was necessary. Dental hygienists stated that they used this opportunity to educate the patient on the exam’s importance, how it was performed, and general risk factors for oral cancer, without discussing specific risks.
Discussion
The results from this study present a baseline description of the current health literacy of dental hygienists in relation to HPV. As dental hygienists are among providers who can be both agents and recipients of health literacy, these focus groups helped to better understand the current health literacy process. Overall, dental hygienists reported mixed experiences when accessing, understanding, appraising, and applying information about HPV prevention with their patients.
Participants accessed HPV-related information from a variety of sources. When discussing the information received during their training, length of time in practice impacted the amount of HPV information they received during their program. With virtually every state requiring graduation from an accredited dental hygiene program and completion of a national written examination for licensure,15,16 interventions to improve access to HPV-related information should be incorporated into the dental hygiene curricula of the more than 300 accredited hygiene programs across the country.17 Employment of dental hygienists is expected to increase by almost 20% in the next ten years, and the number of dental hygiene education programs is expected to increase to meet those needs.17 Including access to information about emerging oral health topics in curricula is crucial. Additionally, there is an opportunity to include the topic of HPV prevention in regional, state, and national boards. For dental hygienists currently in practice, approaches to increase the level of HPV health literacy might be best facilitated through professional journals or continuing education courses, as these lectures have been shown to significantly increase knowledge of prevention-related topics.18
Overall, dental hygienists reported a mix of correct and incorrect knowledge about HPV and HPV-related cancers. Traditionally, oropharyngeal cancers have been associated with smoking and alcohol; however, it is now understood that HPV is an emerging causal factor in oropharyngeal cancer. Dental hygienists possess the baseline knowledge of oral cancers and they clearly expressed a desire to learn more and have accurate information before they begin to educate their patients. These findings complement a study conducted among Maryland dental hygienists, which identified a lack of awareness of oral cancer rates and an interest in additional training in this area.<sup>19</sup> This presents an opportunity to increase dental hygienists’ knowledge by including information on HPV and risk factors through the common sources mentioned previously.
Dental hygienists reported appraising multiple interrelated factors prior to discussing HPV-related information with patients. Commonly mentioned factors included the sensitive nature of the topic and characteristics of the patient (e.g., age). Again, participants reported they would greatly benefit from additional skills and training on beginning the discussion with patients. To meet this need, education should be provided in a variety of modalities, including personalized techniques to meet the needs of individual patients, materials to improve communication skills and HPV-related health literacy,20 and passive materials to educate patients on HPV (e.g., videos in waiting room, pamphlets). Such materials are available through the Centers for Disease Control and Prevention website and provide education on HPV, cancer prevention, and sexually transmitted infections. Additionally, other professional development options to improve self-efficacy for communication may include techniques such as motivational interviewing and active listening.
One emerging finding from this study is that dental hygienists are self-described as being “prevention specialists.” This finding was salient and unsolicited across all focus groups. Currently, few dental hygienists are applying their HPV-related knowledge with patients; however, they consistently reported performing oral cancer screenings to detect oropharyngeal cancer. As self-perceived “prevention specialists,” a crucial role within the dental hygiene profession, the ideal standard of care would involve the combination of educating patients about HPV and the HPV vaccine (i.e., primordial/primary prevention), and oral cancer screenings (i.e., secondary prevention).
Moreover, this view aligns with the professional identity of dental hygienists and presents an opportunity to build upon this perception by the inclusion of HPV-related education. Dental hygienists view themselves as having a professional focus on prevention and currently possess a skill-set as well as a relationship with their patients that facilitates patient education. The discussion of HPV and recommendation of the HPV vaccine as primary prevention would directly integrate into this perceived role. Previous research has suggested that dental hygienists should seek to increase their scope of practice,21 and that the role of dental hygienists is evolving,22,23 both of which present an opportunity to incorporate discussion of the HPV vaccine with their patients. Both dentists and dental hygienists report positive attitudes toward expanding the scope of practice.24 To facilitate this additional role, educational opportunities should be developed. More specifically, the development of targeted patient messages, continuing education opportunities, and dissemination of information on this topic could support dental hygienists in their role as “prevention specialists” as it is applied to HPV prevention.
Currently dental hygienists have a focus on primary prevention and providing preventive procedures, such as dental sealants and the application of fluorides. There is potential to include HPV information and the HPV vaccine within the education provided to their patients. Linking their perceived role as prevention specialists with the HPV vaccine is crucial, as dental hygienists may not conceptualize the ways in which the HPV vaccine fits in with their role. Similar practice behaviors, such as tobacco cessation counseling and oral cancer screenings, have been shown to increase among dental hygienists after they have received education about the topics.18 By increasing the dental hygienists’ knowledge base in various types of primary prevention, they may recognize that incorporating the HPV vaccine into their patient visits adds to the prevention opportunities. While the vaccine is not currently part of their current prevention behaviors, dental hygienists view themselves as “prevention specialists”; therefore, future studies should evaluate how dental hygienists view the role of “prevention specialist” as it relates to describing the benefits of and recommending the HPV vaccine to their patients.
The findings from this study describe the ways in which dental hygienists currently process HPV-related information in their practice. In the process of health literacy, dental hygienists report that they clearly have a role in HPV prevention, but there are issues throughout this process that impact the implementation of this role into practice. The access points that dental hygienists discussed for information should provide more clear and practical information about HPV vaccination. There are opportunities to further develop and expand the meaning of prevention within the dental hygiene profession by broadening the number of topics that fall under the scope of prevention.
This study had several limitations. First, the study sample was derived from convenience sampling at a national dental hygiene conference. This may introduce sampling bias as persons attending the conference may be more likely to receive novel information regarding this topic. Moreover, this sample was homogenous, as the majority were Caucasian, all were women, with an average of 20 years in practice. Thus, additional research is needed to expand the generalizability of these findings to more diverse populations of dental hygienists. Given that these data were collected in a focus group, there is the possibility for social desirability bias influencing responses to questions in this group environment. Finally, while data saturation was reached for major health literacy themes, not all findings were consistent across all focus groups. Nonetheless, this formative study elicited both emerging themes and specific, unsolicited responses that propel the need for greater exploration of this complex topic.
Conclusions
Health literacy is a useful framework that can be used for patients as well as health care providers to understand HPV, a complex, emerging public health issue. Dental hygienists view prevention of HPV-related oropharyngeal cancer through screening and vaccine recommendation as being consistent with their professional perception of being prevention specialists. However, important practice and professional barriers (e.g., lack of self-efficacy, training and resources) among this population of oral healthcare providers remain. Public health efforts should facilitate opportunities for health literacy interventions among dental hygienists, with the ultimate goal of preventing HPV-related cancers morbidity and mortality.
Acknowledgements
This study was funded by the National Institute of Dental and Craniofacial Research (NIDCR) of the National Institutes of Health under award number 5R21DE024272.
The funding organization had no role in the design and conduct of the study; in the collection, analysis, and interpretation of the data; and in the preparation, review, or approval of the manuscript.
Conflict of Interest
Ellen Daley has served on the U.S. HPV Vaccine Advisory Board for Merck Pharmaceuticals. All other authors have no conflict of interest to report.
About the Authors
Erika L. Thompson, MPH, PhD is a postdoctoral fellow; Ellen M. Daley, MPH, PhD is a professor and associate dean of research and practice; Cheryl A. Vamos, MPH, PhD is an assistant professor; all in the Department of Community and Family Health and at the Chiles Center, College of Public Health, University of South Florida, Tampa, FL.
Alice M. Horowitz, RDH, PhD is a research associate professor, Department of Behavioral and Community Health, Horowitz Center for Health Literacy, School of Public Health, University of Maryland, College Park, MD.
Frank Catalanotto, DMD is professor and chair, Department of Community Dentistry and Behavioral Science, College of Dentistry, University of Florida, Gainesville, FL.
Rita Debate, MPH, PhD is the associate vice president of health and wellness and professor in the Department of Health Policy and Management, College of Public Health, University of South Florida, Tampa, FL.
Laura Merrell, MPH, PhD is an assistant professor, Department of Health Sciences, James Madison University, Harrisonburg, VA.
Stacey Griner, RDH, MPH is a doctoral research assistant; Coralia Vázquez-Otero, JD, MPH, is a doctoral research assistant; both are in the Department of Community and Family Health, College of Public Health, University of South Florida.
Nolan Kline, MPH, PhD is an assistant professor, Department of Anthropology, Rollins College, Winter Park, FL.
Corresponding author: Erika L. Thompson, MPH, PhD, ethomps1@health.usf.edu
References
1. Gillison ML, Broutian T, Pickard RK, et al. Prevalence of oral HPV infection in the United States, 2009-2010. JAMA. 2012 Feb; 307(7):693-703.
2. Steinau M, Saraiya M, Goodman MT, et al. Human papillomavirus prevalence in oropharyngeal cancer before vaccine introduction, United States. Emerg Infect Dis. 2014 May;20(5)822-828.
3. Markowitz LE, Dunne EF, Saraiya M, et al. Human papillomavirus vaccination: recommendations of the advisory committee on immunization practices (ACIP). MMWR Recomm Rep. 2014 Aug;63(RR-05):1-30.
4. Viens LI, Henley SJ, Watson M, et al. Human papillomavirus – associated cancers – United States, 2008 – 2012. MMWR Morb Mortal Wkly Rep. 2016 Aug;65(26)661-6.
5. Chaturvedi AK, Engels EA, Pfeiffer Rm, et al. Human papillomavirus and rising incidence in the United States. J Clin Oncol. 2011 Oct;29(32):4294-301.
6. Petrosky E, Boccihi Jr JA, Hariri S, et al. Use of 9-valent human papillomavirus (HPV) vaccine: updated HPV vaccination recommendations of the advisory committee on immunization practices. MMWR Morb Mortal Wkly Rep. 2015 Mar;64(11)300-4.
7. American Dental Association Council on Scientific Affairs. Statement on human papillomavirus and cancers of the oral cavity and oropharynx [Internet]. Chicago (IL): American DentalAssociation; 2012 Nov [cited 2013 May 22]. Available from: http://www.ada.org/1749.aspx.
8. Daley E, DeBate R, Dodd V, et al. Exploring awareness, attitudes, and perceived role among oral health providers regarding HPV-related oral cancers. J Public Health Dent. 2011 Spring;71(2):136-42.
9. Daley EM, Vamos CA, Thompson EL, et al. Are dentists and dental hygienists the next line of prevention against HPV-related cancers? [abstract]. Paper presented at: Oral health section. 144th American Public Health Association Conference; 2016 Nov; Denver, CO.
10. Sørensen K, Van den Broucke S, Fullam J, et al. Health literacy and public health: a systematic review and integration of definitions and models. BMC Public Health. 2012 Jan;12(1):80.
11. Horowitz AM, Kleinman DV. Oral health literacy: The new imperative to better oral health. Dent Clin North Am. 2008 Apr;52(2):333-44.
12. Vamos CA. Applying a health literacy lens to preventative children’s oral health programming. Umwelt und Gesundheit. 2011;4:30-4.
13. Kreuger Ra, Casey MA. Focus groups: A practical guide for applied research. 5th ed. USA. SAGE Publications; 2015.
14. Morrison-Beedy D, Cote-Arsenault D, Feinstein NF. Maximizing results with focus groups: Moderator and analysis issues. Appl Nurs Res. 2001 Feb;14(1):48-53.
15. American Dental Hygienists’ Association. Education & Careers: Licensure [Internet]. Chicago (IL): American Dental Hygienist Association; c2012-2017. [cited 2016 December 12]. Available from: http://www.adha.org/licensure.
16. American Dental Hygienists’ Association. Standards for Clinical Dental Hygiene Practice [Internet]. Chicago (IL): American Dental Hygienist Association; 2016 [cited 2016 December 12]. Available from: https://www.adha.org/resources-docs/2016-Revised-Standards-for-Clinical-Dental-Hygiene-Practice.pdf.
17. Bureau of Labor Statistics, U.S. Department of Labor. Occupational outlook handbook, 2016-17 edition, dental hygienists [Internet]. Washington (DC): U.S. Bureau of Labor Statistics; 2016 [updated 2015 December 17; cited 2016 December 12]. Available from: http://www.bls.gov/ooh/healthcare/dental-hygienists.htm.
18. Walsh MM, Rankin KV, Silverman S. Influence of continuing education on dental hygienists’ knowledge and behavior related to oral cancer screening and tobacco cessation. J Dent Hyg. 2013 Apr;87(2):95-105.
19. Horowitz AM, Siriphant P, Canto MT, Child WL. Maryland dental hygienists’ views of oral cancer prevention and early detection. J Dent Hyg. 2002 Summer;76(3):186-92.
20. Horowitz AM, Clovis JC, Wang MQ, Kleinman DV. Use of recommended communication techniques by Maryland dental hygienists. J Am Dent Hyg. 2013 Aug 1;87(4):212-23.
21. Rock LD, Takach EA, Laronde DM. Oral cancer screening: Dental hygienists’ responsibility, scope of practice, and referral pathway. Can J Dent Hyg. 2014 Feb;48(1):42-6.
22. McComas MJ, Inglehart MR. Dental, dental hygiene, and graduate students’ and faculty perspectives on dental hygienists’ professional role and the potential contribution of a peer teaching program. J Dent Educ. 2016 Sept;80(9):1049-61.
23. Boyd L. Educating dental hygienists to meet future health care need and roles of the profession. J Dent Educ. 2016 Sept;80(9):1031-2.
24. Reinders JJ, Krijnen WP, Onclin P, et al. Attitudes among dentists and dental hygienists towards extended scope and independent practice of dental hygienists. Int Dent J. 2017 Feb;67(1):46-58.