You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
GLOSSARY
Anterior – towards the front; incisors and canines
Articulate – to bring the teeth in one arch together with the teeth in the opposite arch
Avulse – tooth loss due to trauma
Bilateral – on both sides of the mouth
Bruxism – habitual grinding of the teeth together
Buccal – surface of teeth towards the cheek
Congenitally missing – born without
Crepitus – crackling sound in the jaw joint
Deciduous – primary (baby) teeth
Distalize – movement posteriorally, away from the dental midline
Esthetic – pertaining to facial beauty, symmetry, balance, and proportion
Expose – to remove the tissue over a tooth that has not yet erupted
Extrusion – tooth movement directed occlusally and parallel to the long axis
Intrusive – tooth movement directed apically and parallel to the long axis
Labial – surface of anterior teeth closest to the lips
Lateral – towards the side
Lingual – surfaces and directions toward the tongue
Mandible – the lower jaw
Mandibular – referring to the lower jaw
Maxilla – the upper jaw
Maxillary – referring to the upper jaw
Mixed dentition – combination of primary and permanent teeth
Occlusal – chewing surface of posterior teeth
Orthognathic surgery – surgery performed to align the jaws
Osteoblast – a cell from which bone develops
Osteoclast – a cell that resorbs bony tissue
Palate – the roof of the mouth
Periodontium – referring to tissues surrounding the teeth
Posterior – toward the back; premolars and molars
Root resorption – shortening of the roots
Sagittal – pertaining to the suture joining the two parietal bones of the skull
Supernumerary teeth – teeth in excess of the normal number
Tongue thrust – thrusting of the tongue between the anterior teeth
Vertical – up and down
This article will introduce the reader to the fascinating world of orthodontics. Orthodontics is a technical and scientific area of dentistry that not only focuses on functional occlusion, but also can dramatically improve the quality of people’s lives by creating an esthetic, pleasing smile, which can increase self-esteem and self-confidence. Whether the patient is a child or adult, orthodontics is a relatively short-term investment for a lifetime of results.
Orthodontics
Orthodontics is a branch of dentistry that specializes in the diagnosis, prevention, and treatment of dental and facial irregularities. Many technical terms and names of biological structures are formed from Greek and Latin roots. “Ortho” means straight and “odont” means tooth.
The technical term for orthodontic problems is referred to as “malocclusion,” which means “bad bite.” The practice of orthodontics requires professional skill in the design, application and control of corrective appliances to bring teeth, lips and jaws into proper alignment and achieve facial balance. Orthodontic treatment achieves not only a correct bite, but also beautiful smiles, improved dental health and increased self-esteem and self-confidence.
An orthodontist is a dental specialist who after dental school completes an American Dental Association accredited post-doctoral course of at least two academic years in the area of orthodontics. Only dentists who have successfully completed an advanced specialty program may call themselves orthodontists. All orthodontists are dentists, but only about six percent of dentists are orthodontists.
Although the beginning of orthodontics can be traced back to the ancient Phoenicians and Egyptians, Dr. Edward Angle is considered “The Father of Modern Orthodontics” and was one of the first to emphasize occlusion in the natural dentition. His interest in creating proper occlusion in the late 1890s and early 1900s created the specialty of orthodontics. Dr. Angle also designed the classifications of malocclusion of the teeth, based on the first molar as the key to occlusion, which is still commonly used today.
Occlusion
Normal Occlusion
In normal occlusion, the mesiobuccal cusp of the maxillary first molar occludes with the buccal groove of the mandibular first molar.
Types of Malocclusion
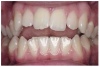
Angle Classifications: Class I malocclusion (Figure 1) has a normal molar relationship. Although the molars may be in ideal position, the other teeth may be crowded, rotated or have excess spacing.
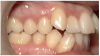
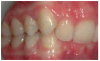
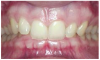
The maxillary first molar is forward of the normal molar relationship in Class II. The mesiobuccal cusp of the maxillary first molar is mesial to the buccal groove of the mandibular first molar. In Class II Division 1 (Figure 2), the maxillary incisors are in labio-version, or protruding. In Class II Division 2 (Figure 3), the maxillary central incisors are in linguo-version (retruded) and lateral incisors are protruded. In Class III the maxillary first molar is distal of the normal molar relationship. The mesiobuccal cusp of the maxillary first molar is distal to the buccal groove of the mandibular first molar.
Subdivision: There can be classification of unilateral (one side) maloccluded positions. One side is Class I and the other side is either Class II or Class III.
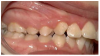
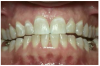
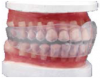
Discrepancies: In a deep bite (overbite) (Figure 4), the maxillary incisors vertically overlap the mandibular incisors excessively. (In severe cases, mandibular incisors may contact the palate or maxillary incisor may strike mandibular gingiva.) In an open bite, there are areas where the maxillary and mandibular teeth do not touch. A patient can have an anterior or posterior open bite (Figure 5 and Figure 6). (An anterior open bite can sometimes be attributed to thumb sucking or a tongue thrust. Other times the condition is a skeletal problem.) Overjet refers to the distance between the facial surfaces of the maxillary incisors and the facial surfaces of the mandibular incisors.
There are two types of crossbites. A buccal crossbite is a malocclusion characterized by any teeth of the maxillary jaw being located lingually (to the inside of) the teeth of the mandibular jaw. In an anterior crossbite, the maxillary incisors are lingual (behind) the mandibular incisors, usually with a Class III occlusion. Space between two teeth is called a diastema. This is most common between the maxillary central incisors.
Other conditions: Impacted teeth are prohibited from normal eruption due to their position in the bone or surrounding teeth. Ankylosed teeth occur when two hard tissues are fused together, preventing movement. When this happens to a tooth and the alveolar bone, the tooth partially erupts. In a growing child, an ankylosed tooth appears to be ‘submerged’ as adjacent unaffected teeth and alveolar bone continue their normal pattern of eruption.
Factors in Dental and Facial Problems
Heredity: Most orthodontic problems are hereditary. Inherited problems include crowding or spacing of teeth, missing or supernumerary teeth, cleft palate and a wide variety of other irregularities of the jaws and face. For example, a patient may inherit their mother’s small mandible, and their father’s large teeth; if this were the case, the child’s teeth would be too large to fit their mandible and result in malocclusion.
Missing and supernumerary (extra) teeth: Congenitally missing teeth are not uncommon. The maxillary permanent lateral incisors, mandibular second premolars and third molars are the teeth most commonly absent, either on one side or bilaterally. This can result in spacing, asymmetry (off-centeredness) and movement of other teeth. Supernumerary or extra teeth seldom erupt into the mouth. They may prevent normal teeth from erupting or cause abnormal eruption.
Acquired: Some orthodontic problems are acquired. Acquired malocclusions can be caused by thumb or finger sucking habits, tongue thrusting, mouth breathing, airway restriction from tonsils and adenoids, dental disease, malnutrition, trauma, or premature loss or prolonged retention of primary teeth. Whether inherited or acquired, many of these problems affect not only alignment of the teeth but facial appearance and self-esteem as well.
Habits: Thumb sucking and finger sucking can shift the teeth out of alignment, creating an open bite, protrusive maxillary incisors, overjet and Class II occlusion.
Tongue thrust and tongue posturing: The tongue pressing forward instead of into the roof of the mouth during speech and swallowing can also force the teeth out of alignment, sometimes causing an open bite.
Mouth breathing: People with severe respiratory problems such as chronic nasal congestion, asthma and bronchitis primarily breathe through their mouth. They often develop narrow maxillary arches, buccal crossbite, high palates and increased gingival display.
Disease: One can lose a tooth early due to dental caries or periodontal disease; leaving a space that allows other teeth to drift towards and into the space.
Malnutrition: Nutritional deficiencies can alter the growth of the jaws and teeth. Early childhood caries, also known as baby bottle caries, promotes early loss of primary teeth.
Trauma: If a tooth is lost due to an accident, then teeth may start to drift into the empty space if preventive measures are not taken.
Premature loss of primary teeth: One purpose of primary teeth is to maintain space for the permanent teeth, which will eventually replace them. Should a primary tooth be extracted or lost before it would be lost naturally, the permanent teeth distal to it can drift forward and the space for erupting teeth may be lost.
Loss of permanent teeth: If a permanent tooth is lost, the adjacent teeth drift or tip towards the space. When teeth have no maxillary or mandibular opposition, they will over (or super) erupt into that opposing space. This can result in root exposure and possible avulsion.
Prolonged retention of primary teeth: When the root of a primary tooth does not resorb as it should, the erupting permanent tooth beneath will either be deflected in another direction or remain impacted.
Importance of Orthodontic Treatment
Esthetics: An attractive smile contributes to one’s self esteem and self-confidence. Orthodontics is a short-term investment with long-term benefits. Many products such as whiteners or bonding treatments fade and need replaced. Straight teeth and a pleasant smile offer lifetime benefits.
Dental, general health, and function: Teeth in malocclusion are hard to clean and maintain and may lead to periodontal disease, tooth decay, and tooth loss. Other orthodontic problems can cause abnormal wear of tooth surfaces, speech problems, difficulty in chewing, or undesirable wear of the temporomandibular joints. Some malocclusions, such as maxillary teeth that protrude, can increase the possibility of fracture due to trauma.
When should treatment begin?: Because every child is different, there is not a standard answer to this question. The American Association of Orthodontics recommends that every child get an orthodontic checkup by age 7—or earlier if an orthodontic problem is detected by parents, the family dentist or the child’s physician. In some cases, early intervention utilizing the patient’s growth can often make corrective treatment faster and easier.
Adult treatment: Orthodontic treatment for individuals who have healthy teeth, gingiva and supporting bone can be successful at any age. Many adults are choosing orthodontic treatment to improve their smile, and/or increase function to support good oral health.
Tooth Movement
Orthodontic tooth movement occurs due to the pressure applied to the teeth by orthodontic appliances. This pressure is transmitted to the clinical crown of the tooth, down to the root, and ultimately to the periodontal ligament (the tissue that attaches the tooth to the bone) and alveolar bone surrounding the root.
Generally speaking, slow, continuous force provides the most efficient tooth movement. Excessive force destroys the periodontium. On the surface of the tooth in the direction where the tooth is being moved, the periodontal membrane is squeezed, resulting in compression of the periodontal fibers within the membrane. The bone surface contacting the periodontal membrane begins to resorb due to the activation of cells called osteoclasts.
On the surface of the root from which the tooth moves, the periodontal membrane becomes stretched. This activates cells called osteoblasts. These cells regenerate new alveolar bone in the area where the tooth was once located. That is why teeth may be slightly loose during orthodontic treatment. Once the movement has stopped, the ligaments are no longer stretched or squeezed and the bone regenerates and fills in around the periodontal ligament, causing the tooth to be more secure in the bone. Even though the tooth is more secure in the bone, retainers are required to hold the teeth in their new position once appliances are removed.
Types of Orthodontic Movement
Types of orthodontic movement include the following:
• Orthopedic forces - forces used to affect the shape and growth of the facial bones.
• Orthodontic forces - forces used to move teeth within the arches.
• Extrude – to move a tooth in the direction away from the gingiva.
• Intrude – to move a tooth in the direction toward the gingiva.
• Rotate – to move a tooth by spinning the tooth on its axis.
• Torque – force causing movement of a root either buccally or lingually.
• Tip - movement of a tooth/root mesially or distally.
• Retraction - moving teeth distally to close space.
• Advancing - moving teeth forward.
Length of Treatment
In general, active treatment time with orthodontic appliances ranges from one to three years. The actual time depends on the growth of the patient’s mouth and face, the cooperation of the patient, and the severity of the problem. Mild problems may require less time, and some individuals respond to treatment faster than others.
In some cases, patients are treated in two-phase treatment. The first phase of orthodontics occurs before all the permanent teeth have erupted. One goal of early treatment is to manipulate the current condition of the patient to allow for teeth to erupt into Class I position. According to Dr. William Proffit, this phase can be loosely described as preventive (preventing problems from occurring), or interceptive (reducing the severity of the problem). However, it is very rare for early orthodontic treatment to fully correct malocclusion on its own. Most children will require Phase II comprehensive orthodontic treatment after all their permanent teeth erupt.
After active treatment is completed, a patient will have to wear retainers to keep the teeth in their new positions. The need for a retainer and the length of time it will be worn are determined by the orthodontist.
The Patient’s Role in Orthodontics
Successful orthodontic treatment is a partnership of effort among the orthodontic team, family dentist and patient (and parent if applicable).
The orthodontist provides the expertise, the treatment plan and the appliances to straighten teeth. The clinical staff provides the instructions and encouragement. The patient must follow the orthodontic team’s instructions carefully so that the teeth move in the appropriate manner.
Patients who brush thoroughly and use floss and flossing aids properly greatly reduce possible decay. Also, those patients that avoid hard or sticky foods, wear their elastics and/or other removable appliances as instructed, and keep their scheduled appointments usually finish treatment on time with good results.
Regular visits to the family dentist for prophylaxis and exams are very important during orthodontic treatment. Also, proper nutrition and keeping sugars and sodas to a minimum are essential for successful treatment.
Orthodontic Appliances
Orthodontic appliances are designed according to the problem being treated. They may be removable or fixed (cemented and/or bonded). They may be made of metal, ceramic or plastic. They can be placed on the labial or lingual surfaces of the teeth (or in some situations, both). All orthodontic appliances have one goal -- to use gentle pressure to move teeth into their proper positions. The body then builds new bone to support the new positions of the teeth.
New techniques and materials contribute to fewer office visits and reduced treatment time in addition to reducing the discomfort of orthodontic treatment. Advancements in technology have made brackets smaller and stronger than before. NASA developed one of the late 20th century’s most dramatic orthodontic breakthroughs, heat-activated nickel-titanium alloy wires. At room temperature, heat-activated nickel-titanium wires are very flexible. As they warm to body temperature they become active and gradually move the teeth to the shape of the archwire. These wires retain their shape, making them more effective for a longer period of time.
Types of Orthodontic Braces
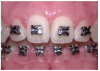
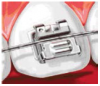
Brackets: Brackets are the small squares that are bonded directly to each tooth with a special dental bonding agent or are attached to orthodontic bands (Figure 7). Brackets act like handles, holding the arch wires that move the teeth. Brackets can be metal or clear, designed for the labial or lingual surface of the teeth.
Metal bands: Orthodontic bands are stainless steel rings that are cemented to the teeth. They wrap around each tooth to provide an anchor for the brackets. Separators are usually necessary to provide space for banding.
Separators: Separators, also known as spacers, are elastic rings or metal springs that fit between teeth to create a small space prior to placement of orthodontic bands.
Archwires: Archwires are wires of various dimensions and materials, such as stainless steel or titanium, which are held into the brackets and act as tracks to guide the movement of the teeth (Figure 8).
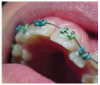
Elastic tie: The elastic tie is a tiny rubber ring that holds the archwire in place (Figure 9). These come in a variety of colors, offering fun choices for patients. (Some brackets are “self-ligating,” [Figure 10] which means that they do not need the elastics to hold the arch-wire onto the brackets.)
Ligature tie: The ligature tie or lig tie (also called steel tie or metal tie) is a fine wire that holds the archwire in place.
Examples of Other Auxiliaries
Power chain or C chain: The power chain is a continuous elastic chain used to close space (Figure 11).
Springs: Springs may be placed on the arch wires between brackets to push, pull, open or close the spaces between teeth.
Elastics: Elastics, or rubber bands, attach to hooks on brackets and are worn between the maxillary and mandibular teeth in various ways. They apply pressure to move the maxillary teeth against the mandibular teeth to achieve a perfect fit of individual teeth.
Orthodontic Appliances Other Than Brackets/Bands
There are many appliances available in the orthodontist’s repertoire. The following are other types of common orthodontic appliances.
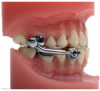
Functional appliances: Functional appliances are designed to stimulate growth of one arch and slow down the growth of another. The Herbst (Figure 12) is a fixed appliance used in treating a growing patient with Class II malocclusions and underdeveloped lower mandible. It is designed to hold the mandible in a forward position to stimulate faster growth of the mandible than the maxilla, therefore reducing overjet and enhancing the patient’s profile.
The sagittal appliance expands the arch and distalizes the buccal segments using three screws (one in the front and one on each side). The twin block is used to stimulate the forward growth of the mandible while restraining the forward growth of the maxilla.
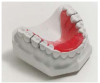
Other removable appliances: A bite plate (Figure 13) is an acrylic appliance that reduces a deep bite by preventing the posterior teeth from touching. A lip bumper (Figure 14) is a 0.036” size buccal wire that fits into the tubes on the mandibular molar bands. Pressure from the lips creates space along the dental arch. A splint is used for the treatment of TMD and facial pain. They may be designed for either arch depending on the treatment objectives. A tooth positioner (Figure 15) is worn after the braces are removed to achieve minor tooth movement and set the occlusion.
Invisalign® is an orthodontic treatment system that works to straighten teeth through the use of a series of clear plastic aligners. Invisalign eliminates the brackets and archwires that is characteristic of traditional orthodontic braces. The orthodontist uses 3-dimensional computer imaging system to design a treatment plan and order a series of clear retainers. Each aligner uses gentle pressure to move the teeth to their target alignments.
The number of Invisalign trays used will depend on each individual case but the average is between 18 and 30. Each clear Invisalign retainer is removable and worn for two weeks (24 hours a day, except during meals) and then the next aligner is used. This process is repeated until the teeth are in the desired position.
Invisalign was traditionally used only for adults. Invisalign for teens is now available. Features include an aligner wear indicator to help gauge patient compliance and specially engineered aligner features to address the natural eruption of key teeth and root control issues common in patients age 13 to 19.
Headgear is an apparatus that is used to deliver force to the teeth from outside the oral cavity. A headgear consists of three parts: a facebow, a headgear force module and a neck strap or headcap. Two bands on the maxillary teeth have headgear tubes on them for insertion of the facebow of the headgear. Examples of heargear include: Cervical headgear pulls from the back of the neck (cervical) to provide a low angle force either to move the maxillary first molars posteriorly to create more space or to anchor the first molars during treatment. This type of headgear has a slight extrusive force on the molars. Hi-pull headgear pulls from the top of the head to give a high angle force to move the maxillary first molars up and posteriorly using the headcap as anchorage. It holds the growth of the maxilla. This type of headgear has a slight intrusive force on the molars. The reverse-pull face mask is used in Class III cases to control growth of the mandible by pulling the maxilla and teeth forward.
Expansion or distalization appliances: A rapid palatal expander is used to widen the maxillary arch to align the maxillary and mandibular arches or make room for crowded teeth. The expanding action of the appliance gently separates the palatal suture (elastic membrane) in the center of the maxillary arch. Once the palate has been expanded, new bone fills the space. The widening of the palate usually causes a diastema to develop between the anterior teeth. (The space closes later.) This appliance can be designed to be banded or bonded to the teeth.
The quad helix (Figure 16) is an appliance using bands with a lingual wire and 4 loops (hence, its name). This appliance is designed to expand the maxillary arch to gain the space needed to correct a cross-bite.
The pendulum is an appliance that moves the maxillary molars posteriorly. The advantage of this appliance is that it replaces the need for headgear by rapidly distalizing the maxillary first molars. The appliance fits into the lingual tubes of the maxillary first molars and is bonded to the occlusal of the upper first premolars. Once the molars are moved posteriorly, a holding appliance is used (such as a Nance) to prevent the teeth from drifting forward.
The pendex is similar to the pendulum except that it additionally expands the maxillary arch simultaneously.
Holding arches: The lingual arch (Figure 17) is a wire bar bonded with bands on the lingual surface of an arch and is designed to prevent forward drifting of the molars.
The Nance is a lingual wire with an acrylic pad on the anterior part of the palate. This is used to hold position of maxillary first molars.
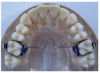
The transpalatal arch (Figure 18) is a lingual wire, either soldered or removable, that crosses from the first molar on one side directly across the palate to the other first molar to hold the molars in position. This appliance can also be adjusted to expand or rotate the maxillary molars.
The space maintainer is an appliance that utilizes a band and open loop. This loop maintains the space between teeth so a permanent tooth has room to erupt.
Retainers: Teeth are never completely stable and always have a tendency to move. After orthodontic treatment, retainers must to be worn to stabilize and hold the teeth in their new positions.
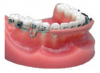
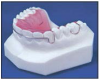
The Hawley retainer (Figure 19) is a removable appliance made of acrylic and a labial bow designed to hold the teeth in their present position or to achieve very minor tooth movement.
The wrap-around retainer is a removable appliance made of acrylic and a labial bow that goes around the entire arch, designed to hold the teeth in their present position or to achieve very minor tooth movement.
A clear retainer is a nearly invisible retainer to esthetically hold the teeth in their present position.
The bonded 3-3 retainer is a wire retainer bonded to the lingual surfaces of the canines or sometimes all mandibular anteriors. In some cases, a wire retainer can be bonded to the lingual of the maxillary central and lateral incisors. This is used to esthetically retain teeth in their correct position for an extended period of time. Special oral hygiene instructions must be given for flossing around this type of retainer.
Diagnosis and Treatment Planning
The patient’s initial visit to an orthodontic office typically consists of an examination and a discussion of possible treatment options and best timing for treatment. Initial orthodontic records are the next step in the process of treatment. The orthodontic assistant is usually delegated the responsibility for obtaining the various records the orthodontist must have to make the diagnosis. Make sure the state dental practice act allows for the duties to be delegated. The laws regarding the delegation of duties vary from state to state. Once all records have been completed the orthodontist analyzes the records to confirm or make a diagnosis for the best treatment options.
The following explains the individual records commonly taken and their purpose.
Photographs or digital imaging: A series of frontal and side facial photographs in addition to intraoral photographs or digital images make up the initial photography record. The facial pictures serve as visual aids for bony and soft tissue analysis so that the facial aspects of treatment can be thoroughly evaluated. Intraoral photos offer a color record of the patient’s initial condition.
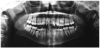
Panoramic radiograph: The panoramic radiograph (Figure 20) is a composite radiograph of the teeth and jaws to look for the normal number of teeth, third molars, missing teeth, impacted teeth or supernumerary teeth. This radiographic image also shows bone support and root length.
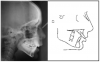
Cephalometric (lateral skull) radiograph: A lateral view of the skull, the cephalometric radiograph is used to study the relationship of the bones, teeth and jaws to the face and skull (Figure 21). The orthodontist obtains measurements then compares them to a standard reference group.
Cephalometric radiographic images taken before, during, and after treatment can be superimposed to study changes in jaw and tooth position. Although the main purpose of taking radiographic images is not for pathology screening, they can sometimes reveal changes or anomalies in the cervical spine, skull, jaws, or cranial base.
Study models: Maxillary and mandibular impressions are obtained from every patient to make a study model used during pre-treatment planning and for reference of the dental problems as they existed at the beginning of treatment.
Surgical Intervention in Orthodontic Problems
Some malocclusions require surgical intervention to achieve a high-quality result. The following outlines the techniques available in maxillofacial surgery to aid the orthodontist. Depending on the procedure, these can be accomplished in coordination with the patient’s general dentist or by an oral surgeon.
Surgical exposure of impacted teeth: Sometimes a tooth will develop laterally instead of vertically. This situation requires the need for surgical intervention to “expose” the tooth, allowing an orthodontic appliance to be attached to gently guide the tooth into the correct position.
Orthognathic surgery: The purpose of orthognathic surgery is to correct functional and esthetic problems that are due to underlying skeletal deformities. Orthognathic surgery is often the treatment solution in cases where the bite abnormality is so severe that braces alone cannot correct the problem, or where orthodontics alone would compromise facial appearance. Surgery may be avoided in some adolescents through growth modification and orthodontic appliances that correct the growth pattern during the remaining growth period.
Extraction of teeth: In some cases, extractions are necessary to create space for proper alignment and tooth movement. The following are different extraction scenarios:
Deciduous teeth (serial extraction) - In some cases, the planned extraction of deciduous teeth will assist the eruption of permanent teeth in the correct sequence.
Permanent teeth - Sometimes there is not enough room in the mouth or necessary bone support for all of the patient’s teeth once treatment has been completed. The most common teeth chosen for extraction are first premolars.
Supernumerary teeth - In some cases there are erupted supernumerary teeth that may hinder successful orthodontic treatment and will need to be removed.
Impacted teeth - The orthodontist primarily decides on the removal of impacted teeth as an adjunct to the orthodontic treatment. The teeth usually removed are the third molars (wisdom teeth) or impacted supernumeraries. These teeth are often removed to prevent future complications or re-malalignment of the teeth.
Primary dentition: In the primary dentition, the Palmer Notation System uses uppercase letters instead of numbers. Following the same order as for adult teeth, children’s 20 primary teeth are lettered “A” through “E” in each quadrant: A = central incisor; B = lateral incisor; C = canine; D = first molar; E = second molar. The same symbols are used to identify the quadrants as in the permanent dentition.
It is important that the orthodontic assistant also understanding the Universal Numbering System used in general practices. Both systems must be understood to communication between orthodontic and general dental practices.
Career Opportunities in Orthodontics
The orthodontic field is full of opportunities. A career choice in orthodontics means you are a member of a special team that helps to produce better oral health, enhanced self-esteem and beautiful smiles.
The following are examples of duties that are typically preformed by orthodontic assistants. Depending on the size of your practice these responsibilities may be performed by separate assistants or all the duties may be performed by one assistant.
Orthodontic Clinical Assistant
Typical responsibilities: actively assists the orthodontist with treatment by preparing teeth for the placement of brackets and bands, prepares and secures orthodontic wires. (Responsibility varies by state.) The clinical orthodontic assistant also educates patients on oral hygiene and appliance care and motivates patients in order to achieve the very best results from orthodontic treatment. The clinical orthodontic assistant also serves as a key communication link between the patient and the orthodontist.
Requirements: communication skills, excellent eye-hand coordination, organizational skills, basic computer skills, attention to detail, time management skills and being a team player while often working independently.
Orthodontic Radiography Technician
Typical responsibilities: takes orthodontic records including radiographic images, photographs and study models. The dental radiography technician is often the first clinical assistant a new patient will encounter. This individual sets the tone of the patient’s orthodontic experience.
Requirements: a dental radiography license required in most states (check with your state dental practice act), communication skills, organizational skills, and attention to detail.
Orthodontic Laboratory Technician
Typical responsibilities: creates retainers and other orthodontic appliances, and prepares orthodontic study models.
Requirements: excellent eye-hand coordination, attention to detail, time management skills, and ability to work independently.
Orthodontic New Patient Coordinator
Typical responsibilities: the liaison between the new patient and the orthodontist and practice, enhances the patient experience of the initial exam; prepares financial arrangements for patients; coordinates treatment. In some offices, this individual is also responsible for external marketing.
Requirements: exceptional interpersonal communication and listening skills, basic understanding of orthodontics, sales training and/or experience ideal, organizational skills, computer skills and in some cases, a dental radiographer’s license.
Orthodontic Scheduling Coordinator
Typical responsibilities: schedules appointments; clerical duties; phone contact with patients, family dentists, and other dental specialists; customer service relations.
Requirements: excellent verbal and written communication ability, computer skills, knowledge of basic orthodontic and dental terminology and nomenclature.
Orthodontic Financial Coordinator
Typical responsibilities: oversees patient financial arrangements and payments, files and coordinates insurance payments, obtains computer statistical reports.
Requirements: excellent verbal and written communication ability, computer skills, basic understanding of insurance filing, and ability to obtain accounts receivables information.
This is just a sample of orthodontic careers. Some practices have a marketing coordinator, a sterilization technician, office manager and or business assistant.
Summary
Basic knowledge of malocclusion and tooth movement must be understood when being a part of an orthodontic dental practice. Becoming a member of the orthodontic team requires a unique combination of skills, a steadfast commitment to long-term goals and a desire to excel. All positions require individuals who thrive on delivering an excellent patient experience and a quality result. If you like to help people and if you would enjoy the respect that comes with being a member of a highly regarded health-care profession that has the capacity to change people’s lives, then, consider a career in orthodontics!
ABOUT THE AUTHOR
Lori Parker, RDAEF, MAOM
Lori Garland Parker is a clinical consultant and co-founder of Consulting Network, a leading orthodontic management and training organization. She coaches orthodontic practices on maximizing the talents of the clinical team, implementing systems to enhance clinical efficiency and productivity along with continuity of care, and teaches communication skills and patient motivation. She also designed and teaches the “Train the Trainer” program, lectures extensively in the U.S. and abroad, and has written a line of customizable procedure manuals to support successful new employee integration into the practice. Lori holds a Bachelors in Business and a Masters in Organizational Management. She is also a RDAEF in California.