You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
The use of complete dentures as a means to restore function and appearance in an edentulous patient can be challenging for both the denture wearer and clinician. Although the rate of edentulism among adults in the United States continues to decline below the current estimated rate of 4.9%1 it is predicted that nearly 37.9 million adults will have one or two edentulous arches by 2020.2 This information suggests that clinicians will continue to implement treatment plans utilizing complete dentures. Furthermore, the rate of edentulism is positively correlated to age and lower socioeconomic standing.1 Clinicians are obligated to tailor their treatment plans to their patients and be prepared to address the unique needs of older, long-term edentulous, and/or economically disadvantaged patients using evidence-based treatment rationale with a predictable, superlative outcome.
Lack of retention or traumatic ulceration accounts for most denture wearers’ dissatisfaction with their prostheses and are the chief reasons why they seek new dentures.3 Patients are more often dissatisfied with their mandibular denture.3 Under the best of circumstances a well-made denture can mitigate these complications. Unfortunately, as evidenced by the denture-wearing demographic, many patients may have complicating factors such as limited bone support, poor soft-tissue anatomy, and/or comorbid medical conditions that negatively impact their denture-wearing experience. Regardless of the unique challenges presented by a patient, it is becoming increasingly apparent that the standard of care for edentulous patients is shifting away from traditional mandibular dentures and toward implant-retained mandibular prostheses.4
Implant-retained mandibular overdentures (IRMOD) can be configured in many ways and generally differ in the number of implants used and type of attachment present at the implant/denture interface. The use of two “standard” (>3.3 mm width) endosteal root-form implants placed intraforaminally with resilient attachments can be considered the minimum standard of care for most edentulous patients when possible.5 This benchmark two-implant IRMOD has been shown to provide patients with a significant and measurable improvement in oral health-related quality of life (OHRQoL).6 The placement of standard 3.3 mm or wider implants in the edentulous mandible may be complicated by reduced bone width and, therefore, may require additional surgery for augmentation. The leading reasons why denture wearers do not pursue an IRMOD is because it may be considered too expensive, invasive, or time-consuming.7
The use of small-diameter (2.7 mm to 3.3 mm) or “mini” (1.8 mm to 2.4 mm) dental implants in an IRMOD is increasingly being proven as an alternative to the minimum standard of care. In some respects both the patient and practitioner may consider mini implants to be superior to larger diameter options. In a recent study, the placement of two mini implants intraforaminally for denture retention/stability was shown to produce superior OHRQoL scores when compared to the two standard implant solution, while a four mini-implant-retained mandibular overdenture (mIRMOD) was superior to both.8 Implant survival rates were 89%, 82%, and 99% for four mini-implant, two mini-implant, and two standard implant overdentures, respectively.8 In these mIRMOD designs there is no use of a rigid bar connecting the implants.
By design, mini implants require less bone width for successful placement than standard implants due to their relatively smaller diameter.9 Implant surface textures, thread profiles, and implant width and length vary among mini-implant manufacturers. Histological studies of removed 1.8-mm-diameter implants used in a mIRMOD application showed successful osseointegration.10 This characteristic of needing less bone width is well suited to patients who have atrophic residual ridges that may otherwise require bone augmentation surgery. According to limited, retrospective data, the survival rates of mini implants in both fixed and removable scenarios may be >90%.11,12 Furthermore, provided adequate primary stability at the time of placement, immediate loading and early loading of implants in a mIRMOD has proven to be successful with 91.7% and 96.7% implant survival rates, respectively.13 A mIRMOD requires regular replacement of worn-out retentive o-rings found in the female implant attachment housings. Otherwise, maintenance is similar to that of a traditional denture in regards to worn teeth and the need for relines and other general repairs.14
Barriers to care regarding implant therapy in edentulous patients are significant. It is estimated that 1.7% of edentulous patients worldwide have received implant treatment.15 It is also estimated that as few as 13% of US general dentists place implants,16 although this appears to be trending upward. Cases planned for mIRMOD therapy may offer greater acceptance rates due to the treatment’s relatively lower cost and perceived minimal invasiveness. This, along with the growing body of evidence for its support at least in the short term or as interim treatment, should motivate more dentists to place mini implants and help edentulous patients overcome the problems associated with traditional lower dentures.
Case Presentation
A 62-year-old male patient presented seeking a new pair of dentures. He admitted that he had not worn his old dentures since they were delivered 6 years prior, immediately following the extraction of his remaining teeth. The timeline of the patient’s dental history was unclear, but he recalled having serial extractions beginning as a young man due to general neglect. He reported that his prostheses were ill fitting, which resulted in lack of retention, masticatory issues, and soreness. At his initial consult he mentioned seeing a television commercial for implants used to stabilize dentures and was interested in this treatment modality. He was chiefly concerned about cost and the invasiveness of surgical implant placement.
Medically, this patient could be classified as a physical score class 3 according to the American Society of Anesthesiologists (ASA PS 3),17 indicating that he had severe systemic disease. His medical history was significant for hypertension, “minor” cerebrovascular accident (CVA) or stroke in 2014, chronic pain from a disabling back injury with other musculoskeletal pain disorders, and generalized anxiety, all of which were being treated pharmacologically. The patient had a partial knee replacement in the mid-1970s, was not currently anticoagulated for his history of CVA, and had an allergy to penicillin. No antibiotic prophylaxis was indicated in this situation.
He had a social history significant for alcohol and tobacco use. Although complex, this patient’s medical history did not present any absolute contraindications to implant placement.18 The patient’s systemic conditions were well controlled; however, invasiveness and postoperative morbidity of implant placement must be considered when choosing an appropriate treatment modality. Additionally, patients must be informed of the potential risks associated with surgical implant procedures and whether or not potential improvements in overall quality of life outweigh the risks.19
The patient was presented with several treatment options before he decided on a traditional complete maxillary denture and a mIRMOD utilizing four mini implants with o-ball type attachments. Other options presented included the use of traditional dentures without implants, any combination of maxillary or mandibular overdenture using various styles of implants and attachments, and an implant-supported fixed bridge option that may have required minor adjunctive osseous surgery. He was informed that because he presented with adequate bone volume the standard-of-care implant solution could be performed. The patient’s final decision-making was based on cost, treatment timelines, and perceived invasiveness of surgery. He scheduled surgery 1 week after his consult. He was uninterested in using his existing dentures while new prostheses were fabricated. His unwillingness to wear a healing denture resulted in an unorthodox prosthetic approach that was easily overcome. The exposed supragingival portion of the implants would be protected by o-ring–retained attachment housings while his prostheses were being fabricated. The use of a surgical guide is not demonstrated in this case but can certainly be implemented.
Preoperative Imaging and Assessment
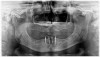
A panoramic radiograph was taken at the start of the consultation appointment. The radiograph revealed an edentulous maxilla and mandible with no remarkable pathology. Bone height was generally good and well suited for the placement of implants. The anterior mandible would serve as a suitable site for four mini implants. The panoramic radiograph served as a screening tool, which could be used to develop the early stages of an implant treatment plan at a consultation.
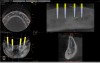
In a statement of position, the American Academy of Oral and Maxillofacial Radiology recommends that a form of cross-sectional imaging be used to guide surgical implant placement.20 In this case a small-volume cone-beam computed tomography (CBCT) scan was taken of the anterior mandible to further develop the surgical plan. From these images the position of the mental foramen and any anterior loop of the mental nerve was established (Figure 1). Given the length and width of bone, four 2.4-mm-wide by 13-mm-long implants were chosen for this case. The position of the two distal implants would allow for a margin of safety in regards to the mental nerve but would be placed as far posterior to the two most anterior implants as allowable. Maximizing the anterior-posterior, or A-P, spread of the implants would minimize any cantilevering forces acting on the denture.
An evaluation of the soft tissue showed no remarkable pathology. The muscle attachments were evaluated to assess the depth of all vestibular areas and any unfavorable frenal attachments. There was some remaining attached keratinized mucosa overlying the crest of the mandibular ridge, which was ideal for implant placement though not necessary for success.21
Surgical Phase
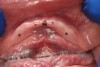
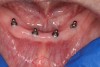
A sterile operating environment was established. Prior to administering anesthesia the location of the mental foramen and the exiting neurovascular bundle was established by palpating the facial aspect of the mandible; this procedure was performed in conjunction with the cross-sectional CBCT imaging. If this technique is inadequate, a radiographic splint can be used to further verify the position of the mental foramen; often, a patient’s existing mandibular denture can be modified for this purpose. A surgical marker was used to mark the proposed implant positions with at least 3-mm inter-implant spacing (Figure 2). Establishing the position of the mental nerve prior to administering local anesthesia is necessary, because the injection site will become filled with anesthetic solution, and/or submucosal hematoma will interfere with accurate palpation. Sufficient pain control was achieved via infiltration of local anesthetic in the area of the mental foramen as well as along the crest of the anterior mandible. Care was taken to minimize the patient’s exposure to epinephrine.
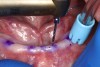
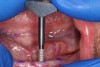
A surgical handpiece was used to perforate the mucosa and develop the osteotomy. The use of a transmucosal or “flapless” osteotomy is a well-established approach for the placement of narrow-diameter implants.22 If needed, as in the case of a surgical complication, a full-thickness mucoperiosteal flap can be developed, which will aid in visualizing the mandible. This requires great care so as not to disturb underlying structures. In this case a 1.2-mm-diameter twist drill running at 1200 rpm brought the osteotomy to a depth of 10 mm (Figure 3), which was dictated by the size of the selected implants. With practice, the clinician can create osteotomies that do not perforate the lingual or buccal cortical plates. This is done by assessing the vertical orientation of the bone by using a free hand to detect its buccal angulation. Interpreting the cross-sectional images is essential. If this is beyond the capabilities of the clinician or if the risk of perforation is great, a pre-drilled surgical guide of a flapped approach can be used for this step. Angulation pins or semi-inserted implants can be placed in shallow osteotomies to verify their orientation and check inter-implant parallelism.
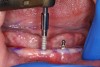
The implant was removed from its sterile packaging (Figure 4) and initially inserted into the osteotomy with a knurled thumb-driver (Figure 5). Alternatively, a surgical handpiece could be used, set to 50 rpm and 30 Ncm torque (Figure 6). The threads of the implant will advance it through the osteotomy. If insertion is performed manually, a T-shaped driver or ratchet would be used to develop more torque as the implant advances (Figure 7). The final depth of the implant is achieved when all threads are at or below bone level. In a “flapless” approach the thickness of the overlying mucosa must be accounted for and can be assessed by ridge mapping using a periodontal probe or by noting the thickness of tissue penetrated by the osteotomy. Final advancement to depth is achieved with a torque wrench to verify initial implant stability; in this case it was >40 Ncm (Figure 7). The final implant position was evaluated clinically (Figure 8), and a postoperative radiograph was taken to verify the implants’ final positioning (Figure 9).
Immediate postoperative instructions were given to the patient. Due to the patient’s history of chronic pain management with opiates he was not prescribed anything for postoperative pain. A prescription was written for an azithromycin 250-mg dose pack. Follow-up intervals were established at 2 weeks to coincide with prosthesis fabrication appointments.
Prosthetic Phase
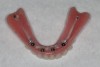
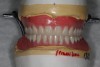
Fabrication of a mIRMOD and opposing maxillary denture does not differ greatly from traditional dentures. Final impressions were taken immediately following implant placement. An appropriate “stock” thermoplastic impression tray was chosen and a two-stage impression technique applied. In this technique, a vinyl polysiloxane (VPS) putty was first used to fill the impression tray, which was inserted into the mouth, and border molding was completed. The putty-lined impression tray was removed before setting and inspected to ensure that all borders and muscle attachments were captured. While soft, the putty impression was washed with light-body VPS and carefully reinserted, and border molding was repeated. The final impression was removed and inspected when it had completely set (Figure 10). The use of impression copings was contraindicated; the laboratory would place implant analogues directly into the cavities created by the implants before pouring the master casts(Figure 11). For patient comfort, removable implant attachments retained by resilient o-rings were placed over the mini-implant o-ball retentive feature between appointments.
Specific instructions were given to the laboratory to fabricate a cobalt-chromium framework that would add strength and rigidity to the largely acrylic mIRMOD. When fabricating the mIRMOD the laboratory was asked to invest and process the denture base, framework, and female attachment components as a first step. This processed denture base would be used in conjunction with a maxillary denture base, usually made of gutta percha, and wax bite rims to capture jaw relation records. This approach was useful because it allowed for retention of the mIRMOD as records were taken and the subsequent try-in appointments were completed (Figure 12 and Figure 13).
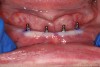
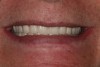
At 6 weeks post-surgery the implants showed proper healing (Figure 14) and the denture was delivered (Figure 15). Overpressurized areas that create sore spots were identified and adjusted as needed.
Follow-up
The follow-up protocol used in a mIRMOD case is based on the date of surgery and the date of prosthesis delivery. In the time directly following implant placement, the patient is generally seen at 2-week intervals for prosthesis fabrication; these appointments are also used to verify proper healing. The patient is scheduled to be seen 1 month after delivery of the prosthesis; often patients will be seen for adjustments before this date. Healing is then checked at 3 months after implant placement. Finally, annual follow-up appointments with radiographs are recommended. The patient is informed that the resilient o-rings inside the female attachments may need replacement every 6 to 12 months.
Conclusion
The use of a mIRMOD should be considered whenever restoration of an edentulous mandible is treatment planned. A mIRMOD has specific indications for patients who present with reduced bone volume or who seek a minimally invasive, relatively low-cost treatment option that predictably increases their oral health-related quality of life.
DISCLOSURE
Dr. Oppenheimer is a key opinion leader and clinical consultant for Sterngold, a company that produces mini dental implants and related armamentarium. He is also a key opinion leader and clinical consultant for Apex Dental Solutions, a group that specializes in training dentists how to place and market dental implants. Dr. Oppenheimer is part owner of Pro-Esthetics Dental Laboratory, which is the dental laboratory used in this case study.
Dr. Hauer is an associate doctor at Concierge Dental Group, a practice owned by Dr. Oppenheimer, and is also a clinical consultant at Pro-Esthetics Dental Laboratory.
ABOUT THE AUTHORS
Benjamin D. Oppenheimer, DDS
Private Practice, Buffalo, New York
Benjamin E. Hauer, DDS
Private Practice, Buffalo, New York
REFERENCES
1. Slade GD, Akinkugbe AA, Sanders AE. Projections of U.S. edentulism prevalence following 5 decades of decline. J Dent Res. 2014;93(10):959-965.
2. Douglass CW, Shih A, Ostry L. Will there be a need for complete dentures in the United States in 2020? J Prosthet Dent. 2002;87(1):5-8.
3. Bilhan H, Geckili O, Ergin S, et al. Evaluation of satisfaction and complications in patients with existing complete dentures. J Oral Sci. 2013;55(1):29-37.
4. Das KP, Jahangiri L, Katz RV. The first-choice standard of care for an edentulous mandible: a Delphi method survey of academic prosthodontists in the United States. J Am Dent Assoc. 2012;143(8):881-889.
5. Thomason JM, Kelly SA, Bendkowski A, Ellis JS. Two implant retained overdentures—a review of the literature supporting the McGill and York consensus statements. J Dent. 2012;40(1):22-34.
6. Emami E, Heydecke G, Rompré PH, et al. Impact of implant support for mandibular dentures on satisfaction, oral and general health-related quality of life: a meta-analysis of randomized-controlled trials. Clin Oral Implants Res. 2009;20(6):533-544.
7. Al-Dwairi ZN, El Masoud BM, Al-Afifi SA, et al. Awareness, attitude, and expectations toward dental implants among removable prostheses wearers. J Prosthodont. 2014;23(3):192-197.
8. de Souza RF, Ribeiro AB, Della Vecchia MP, et al. Mini vs. standard implants for mandibular overdentures: a randomized trial. J Dent Res. 2015;94(10):1376-1384.
9. Davarpanah M, Martinez H, Tecucianu JF, et al. Small-diameter implants: indications and contraindications. J Esthet Dent. 2000;12(4):186-194.
10. Balkin BE, Steflik DE, Naval F. Mini-dental implant insertion with the auto-advance technique for ongoing applications. J Oral Implantol. 2001;27(1):32-37.
11. Shatkin TE, Shatkin S, Oppenheimer BD, Oppenheimer AJ. Mini dental implants for long-term fixed and removable prosthetics: a retrospective analysis of 2514 implants placed over a five-year period. Compend Contin Educ Dent. 2007;28(2):92-99.
12. Sohrabi K, Mushantat A, Esfandiari S, Feine J. How successful are small-diameter implants? a literature review. Clin Oral Implants Res. 2012;23(5):515-525.
13. Maryod WH, Ali SM, Shawky AF. Immediate versus early loading of mini-implants supporting mandibular overdentures: a preliminary 3-year clinical outcome report. Int J Prosthodont. 2014;27(6):553-560.
14. Elsyad MA. Patient satisfaction and prosthetic aspects with mini-implants retained mandibular overdentures. A 5-year prospective study. Clin Oral Implants Res. 2016;27(7):926-933.
15. Carlsson GE, Omar R. The future of complete dentures in oral rehabilitation. A critical review. J Oral Rehabil. 2010;37(2):143-156.
16. Crawford JF, McQuistan MR, Williamson AE, et al. Should endodontists place dental implants? A national survey of general dentists. J Endod. 2011;37(10):1365-1369.
17. Jolly DE. Evaluation of the medical history. Anesth Prog. 1995;42(3-4):84-89.
18. Hwang D, Wang HL. Medical contraindications to implant therapy: part I: absolute contraindications. Implant Dent. 2006;15(4):353-360.
19. Diz P, Scully C, Sanz M. Dental implants in the medically compromised patient. J Dent. 2013;41(3):195-206.
20. Tyndall DA, Brooks SL. Selection criteria for dental implant site imaging: a position paper of the American Academy of Oral and Maxillofacial radiology. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2000;89(5):630-637.
21. Misch CE. Dental Implant Prosthetics. St. Louis, MO: Elsevier Mosby; 2014:59-62.
22. Scherer MD, Ingel AP, Rathi N. Flapped or flapless surgery for narrow-diameter implant placement for overdentures: advantages, disadvantages, indications, and clinical rationale. Int J Periodontics Restorative Dent. 2014;34 suppl 3:s89-s95.