You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Introduction
Attention deficit/hyperactivity disorder (ADHD) is the most common behavioral disorder in school-aged children today. According to Friedlander, in 2007, ADHD affects 4 to 9% of children in the U.S.1 Prevalence of this neurologic disorder has been reported to be as widespread as 2 to 18% of the population.2 The characteristic features of ADHD can include excessive motor activity, developmentally inappropriate activity level, low frustration tolerance, impulsivity, poor organizational behavior, distractibility, and inability to sustain attention and concentration.1-9 Since more children are being diagnosed with ADHD today than ever before, causes and treatment of dental caries in children with ADHD are of great interest to the dental community and to the public.
Studies have been conducted that support the anecdotal evidence that children with ADHD have a signifi¬cantly higher prevalence of dental caries than children without ADHD.2-6 Since xerostomia (dry mouth) has been reported as a side-effect of methylphenidate, and dextroamphetamine medications and non-stimulant medications such as serotonin reuptake medicines and tricyclic antidepressants commonly used to manage the symptoms of ADHD, it is hypothesized that xerostomia may contribute to a higher prevalence of dental caries.2,7-9 Saliva production, the body’s natural protection system against dental caries, may be reduced by these medications. A reduction in saliva flow is considered to be a factor in dental caries risk.10
Healthy saliva plays many important functions in the prevention of dental caries. Reduction of salivary flow or changes in the composition of the saliva caused by medications in children with ADHD may have an effect on the risk of dental caries.7-9 In search of contributing factors to higher caries rates in children with ADHD, researchers have also investigated factors such as poor oral hygiene, high consumption of sugar-containing foods and beverages demographics, low IQ, low socioeconomic status of parents, dental anxiety, and pathophysiologic changes.2-9
Stimulant medications are effective in treating ADHD because they enhance the release of dopamine and norepinephrine, thereby allowing previously under-stimulated areas of the brain to regain their normal functionality.1 In the case of ADHD, these normal functions are the suppression of hyperactivity, impulsiveness, aggression and unusual distractibility.1
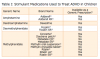
Although medical management brings about a 50 to 75% reduction in symptoms, a combination of pharmaco¬logical and behavioral therapy is generally more effective than either one alone.1 In 2002, Wender reported that stimulant medication is the medication of choice in the treatment of children with ADHD.11 Table I lists the names of some of the stimulant drugs used to treat ADHD. Medications used to treat ADHD that may also cause xerostomia are antidepressants, such as desipramine, imipramine and buporpion sold as Norpramin®, Tofranil® and Wellbutrin®.12,13
The focus of this review is to determine if stimulant medication used to treat the symptoms of ADHD in children increases the risk of dental caries by virtue of its effect on the reduction of salivary flow.
Methods and Materials
A PubMed/Medline search was performed using the terms “ADHD medications” and “dental caries” to discover a connection between the two. Additional sources were located using the search terms “attention deficit/hyperactivity disorder,” “dental caries,” “xerostomia and dental caries” and “saliva and dental caries.” Further information on pertinent articles was retrieved from the reference sections of these articles. Early studies were included that tested for a correlation between ADHD and dental caries.2-6,8
Studies were reviewed for data relevant to a connection between xerogenic medications used to treat symptoms of ADHD and the risk of dental caries. Only studies that either identified or examined the prevalence of dental caries in children with ADHD and/or those who discussed and/or used xerogenic medication as a variable were included in this review.
Studies Conducted to Establish a Relationship Between ADHD and Dental Caries
Most of the early research concerning dental caries and children with ADHD has been performed with small case studies to confirm the anecdotal evidence that children with ADHD have a significantly higher caries rate than children without ADHD. Broadbent et al conducted a regression analysis to determine if dental caries remained higher in children with ADHD and to quantify the role of confounding factors in any observed relationship between dental caries and ADHD.2 This study was one of the first to ask the question, “How might ADHD be associated with dental caries experience?”2 Four possible explana¬tions were offered. One idea was that characteristics of the disorder itself may lead to a lack of motivation to maintain good oral hygiene. Another possibility was that parents of a child with ADHD may be more likely to reward that child with cariogenic treats.2 Thirdly, medications used to treat the symptoms of ADHD have been reported to have the side effect of xerostomia which is often associated with increased frequency of consumption of soft drinks and poorer oral hygiene.2 A fourth suggestion was that parents/guardians of children with developmental disorders (including ADHD) may report the unmet need for oral health treatment than parents of children without developmental disorders.
Using questionnaires and dental records of 128 case-controlled pairs (aged 11 to 13), cases and controls were matched on age, sex, ethnicity and socio-economic status. After controlling for fluoride history, medical problems, diet and self-reported oral hygiene, analysis showed children with ADHD had nearly 10 times the odds of having a high decayed, missing or filled teeth (DMFT) score than children who did not have ADHD. None of the other co-variants were significantly associated with the outcome of higher caries in the ADHD group. On the basis of the association between medication for ADHD and high DMFT, it was suggested that there may be some validity to the idea that medication might be a risk factor for the high rate of dental caries. But, given that medication was not studied as a possible risk factor in dental caries, there is no supporting evidence for this conclusion.13 In fact, the limitations of this study were that, in addition to its small sample size, treatment with medication was only used as a positive diagnosis of ADHD and 9 of 14 of the subjects with ADHD were medicated.
All other variables being constant, the outcome of a study of dental caries in children with ADHD could be influenced by the age of the children which correlates with the eruption sequence. Three clinical and retrospective, double-cohort studies (2006, 2007 and 2011) were conducted by Bloomqvist et al using subjects from the same population pool for all 3 studies.3-5 All 3 studies tested for dental caries experience in children with ADHD as compared to children without ADHD along with other factors. The 2006 study which tested for oral health, dental anxi¬ety and behavioral management problems studied both children with ADHD (n=25) and children with¬out ADHD (n=58). All of the children were 11 years of age.3 A significantly higher rate of dental caries was found in the ADHD subjects. The ADHD group was not found to have a higher degree of anxiety, but they did have more behavioral management problems than the control group. The 2007 study which tested for dental caries and oral health behavior did not find a significant difference in caries prevalence between a group of 13 year old children with ADHD (n=21) and control subjects (n=79).4 They did, however, find children with ADHD had poorer oral health behavior than the control group. The 2011 study considered caries experience and oral hygiene status in a group of 17 year olds.5 The ADHD group consisted of medicated (n=40) and non-medicated (n=40) subjects. Results found significantly higher decay rates in the ADHD group along with poor oral hygiene and an increased consumption of sugary foods.
It was postulated that the lack of caries among the 13 year old group may have been attributed to the shedding of deciduous teeth and the lack of time for caries development in the new dentition.4 Another study, by Chandra et al, found a similar difference.7 Children, aged 6 to 14 years of age with ADHD (n=80) were found to experience more caries (DMFT) in the primary dentition (p=0.002) than children not diagnosed with ADHD. However, in the same study, no such difference (p=0.144) was found in the permanent dentition (DMFT). This would appear to give credence to the theory that the newly erupted teeth had not been in the oral environment a sufficient length of time for caries to develop. These studies would seem to support the theory that children with ADHD have a tendency toward a higher rate of caries and generally poorer oral hygiene than children without ADHD. However, more research using a larger sample size is needed to confirm this finding.
Studies Using Medication as a Variable in ADHD and Dental Caries
Although medication has been used to diagnose subjects having ADHD, few studies have controlled for medication as a risk factor in dental caries. Proper investigation of any relationship of xerogenic drugs and dental caries among ADHD children would require using medication and saliva production as variables.13
A cross-sectional study to examine whether children with ADHD had the same caries experience as children without ADHD was conducted in by Grooms in 2005.7 Saliva flow was considered in this study to test for xerostomia in children with ADHD. Participants ranged in age from 6 to 10 years old, and were divided into 2 groups consisting of 38 subjects each (31 boys and 7 girls). One group was diagnosed with ADHD and taking medication. The other group was composed of healthy children who were not taking any medications. All 76 children were screened by 1 examiner for decayed, missing, filled surfaces (DMFS). A visual exam was conducted and subjects’ teeth were charted for their presence, car¬ies, restorations and sealants. At the same screening, the examiner collected a timed, quantitative, unstimulated, whole saliva sample for each partici¬pant. The weight of the saliva was measured to the nearest one-hundredth of a gram. Both a medical questionnaire and a questionnaire concerning each child’s oral health including diet, oral hygiene, dental care, fluoride exposure, and daily activities was completed by the parent/guardian.
With no data yet available on DMFS for children with ADHD, researchers proposed that a two-fold increase in DMFS among ADHD children would rep¬resent a clinically meaningful elevation in caries.7 Results revealed that children in the ADHD group had statistically more enamel carious lesions in the primary dentition (p=0.04) and significantly more enamel caries in the permanent dentition (p=0.01) than the control group.7 No differences were identi¬fied in key preventive practices such as tooth brush-ing, fluoride exposure and flossing and no differ¬ences in diet were reported between ADHD subjects and the control group. No significant differences (p=0.5) were found for the amount of saliva (0.5 g) produced in the ADHD group of subjects taking dif¬ferent types of medications and those in the control group. These findings lead researchers to conclude saliva flow is not significantly reduced in children prescribed medications for ADHD.7 A limitation of this study is that it did not perform a plaque index (PI) and therefore could not determine if oral self-care contributed to the higher caries experience in the ADHD group.
Although the previous study found children with ADHD did not have a significant reduction in saliva to cause xerostomia, it did not separate children with ADHD who were treated with medication from those with the disorder who were not treated. Without comparing the 2 distinct groups of children with ADHD, it is not clear if dental caries prevalence is related to ADHD itself or the medications.
In 2011 and 2012, Hidas et al published results of 2 individual studies that further investigated how saliva affects dental caries by studying the effect of children medicated for symptoms of ADHD as opposed to those not medicated.8,9 In both studies, researchers separated subjects into 3 groups according to their medication status. One group had ADHD and no pharmacologic intervention, another group had ADHD and was treated with methylphe¬nidate, and the control group consisted of healthy non-ADHD subjects taking no medications. The 3 groups in each study contained 31, 30 and 30 individuals, respectively. The aim of the 2011 study was to investigate the relationship between ADHD and the prevalence of caries in children, adolescents and young adults by focusing on salivary quality in terms of salivary flow rate, oral mucosal pH, PI, oral hygiene and dietary behavior.8 It was hypothesized that children medicated for ADHD would have lower unstimulated salivary flow rates (an outcome of the medicament) which would result in lower buffer capacity and higher bacterial count than those not treated.8
Data were collected including unstimulated salivary flow rate, oral mucosal pH, PI, DMFT index, oral hygiene and dietary behavior were compared between the 3 subject groups. It was found that the non-medicated ADHD group had the lowest mean unstimulated salivary flow (0.72 ml/min) and the control group had the greatest (1.13 ml/min). The medicated ADHD group had 0.85m/min, which was not significantly higher that the non-medicat¬ed ADHD group. Both subject groups with ADHD (medicated and non-medicated) had significantly lower unstimulated salivary flow than the control (p=0.016). However, it was noted that none of the children in any group had very low levels (<0.1 ml/min).9 No significant correlation between DMFT and unstimulated saliva flow was found among the 3 groups. Although PI scores were significantly higher (p<0.05) in the 2 ADHD groups combined than the control, no significant correlation was found between DMFT/dmft and PI. No significant differences were found among the groups for the other factors studied.9
Reduced salivary flow impairs buffering abilities and creates an oral environment that is more acidic.8 Mutans streptococci (MS) and lactobacillus (LB), the major caries pathogens, have been found to be higher in patients with more concentrated saliva.8 While the previous study investigated salivary flow and pH to establish a link between ADHD and dental caries,8 the 2012 study looked at the composition of the saliva, focusing on MS and LB levels, salivary buffer capacity and salivary flow rate along with oral hygiene and diet in 3 groups of children.9 It was hypothesized that lower salivary flow rates in medicated ADHD children (an outcome of the medicament) would result in lower buffer capacity and higher bacterial count.9
Three groups of children – ADHD1 (with no pharmacological intervention, n=31), ADHD2 (medicated with methylphenidate, Ritalin® or Concerta®, n=30) and a healthy group (n=30). Each group was composed of children between approximately 6 and 17 years of age (mean age 10.3+2.8 years). The main finding of this study was that despite a higher PI in the ADHD groups, no significant differences existed in salivary buffer capacity (p=1.00), LB and MS counts (p=0.579), or the DMFT index between children with ADHD (with or without phar¬macologic intervention) and the control group.9 As reported in questionnaires from parents/guardians of all subjects, there were no differences in diet and oral health behaviors between the 3 groups. Consumption of sugary sodas was associated with higher DMFT rates in all 3 groups (p =0.043).9 It was noted that significantly higher (p=0.024) levels of plaque were found in the 2 ADHD groups combined compared with the control group.
Discussion
Current thought on the caries risk of children medicated for ADHD is due to the reported xerogenic effect of these medications. Most early studies were conducted to simply evaluate this theory by comparing the caries experience of children with ADHD to that of healthy children. Few studies have been conducted to evaluate the effect of ADHD medications on dental caries in children.7-9
Results of the Grooms7 and Hidas8,9 studies suggest reduced saliva flow from ADHD medications is not a factor in the rate of caries in children with ADHD.7-9 However, only the 2 Hidas studies have compared medicated and non-medicated ADHD subjects.8,9 The 2012 study provided preliminary evidence that children medicated for symptoms of ADHD were not at higher risk for caries than non-medicated ADHD children due to the side effect of the medication reducing the amount of saliva.9 However, due to the small sample size of both stud¬ies, more research is needed.
Although dental caries prevalence has been found to be higher in children with ADHD,2,3,5,7,9 decreased salivary flow as a side-effect of pharmacological treatment does not appear to be responsible.8,9 It has been suggested children with ADHD may be unable to perform regular routine activity like tooth brushing in an effective manner which may lead to improper oral hygiene practices due to their symptoms of inattention, hyperactivity and impulsivity.12 According to the studies, pharmacologic intervention should not be discontinued based on a fear of it contributing to dental caries. Medication is an effective and essential part of the management of behavioral symptoms associated with ADHD. As long as the medication is well tolerated by the child and effective in controlling symptoms, pharmacotherapy should go hand-in-hand with behavioral therapy.
It has been postulated that the child’s perception of xerostomia may increase the desire for sugar-filled candies, mints and sodas because sugar temporarily increases saliva flow.12 The increase in sugar along with the general finding of higher levels of plaque and poorer oral hygiene practices may have an effect on the higher prevalence of dental caries in children with ADHD.2 Quantitative, objective data regarding the capacity of medications to induce xerostomia are usually based on patient report in clinical drug trials.14
The flow rate of saliva varies greatly from person to person and xerostomia is a subjective sensa¬tion that may not be related to an actual reduction in salivary flow.15 The experience of dry mouth is usually considered to be minor when evaluating the side effects of a medication and is often listed in the information sheet along with other side-effects.15 Investigations to evaluate the actual flow rate of saliva are complex, expensive and rarely performed.15
Sodas containing sugar and several types of acid provide a compounded threat for dental caries by introducing refined carbohydrates into the oral environment and significantly reducing the oral pH.16 It is important to note that even artificially sweetened sodas contain the same amount of acid as sugar-sweetened sodas.16 The presence of sugar is not the only threat. Cariogenic oral bacteria thrive in an acidic environment.16 Saliva’s normal pH is 6.5 to 7.5. The pH required for enamel demineraliza¬tion is 4.5 to 5.5.16 A can of soda has a pH level of between 2.7 and 3.5.16 Perhaps the best method of preventing dental caries in children with ADHD is to encourage both children and parents to limit the consumption of cariogenic food and drinks. Parents/caregivers should be encouraged to not have them available and not use them for behavioral rewards.
Conclusion
Knowing that children diagnosed with ADHD may have a higher risk of dental caries2,3,5,7,9 and a tendency toward higher plaque formation,1,4,5,8,9 practicing dentists and dental hygienists need to be assertive in recommending shorter intervals between recare visits as well as nutritional counseling to include a non-cariogenic diet along with additional preventive measures such as topical fluoride and increased parental monitoring of the child’s daily oral hygiene practices. Although decreased salivary flow as a side-effect of pharmalogical treatment does not appear to be responsible for the increase in dental caries in children with ADHD,7-9 the role of saliva in the caries process still needs further study.
Sandra S. Rosenberg, RDH, MDH, is an Adjunct Professor at Sanford Brown College.
Sajeesh Kumar, PhD, is an Executive Director, Institute for Health Outcomes and Policy, Chair- PhD program, Associate Professor, Department of Health Informatics & Information Management at UTHSC-Memphis.
Nancy J.Williams, RDH, EdD, is a professor and graduate program director in the Department of Dental Hygiene at UTHSC.
References
1. Friedlander AH, Yagiela JA, Mahler ME, Rubin R. The pathophysiology, medical management and dental implications of adult attention-deficit/hyperactivity disorder. J Am Dent Assoc. 2007:138(4):475-482.
2. Broadbent JM, Ayers KM, Thomson WM. Is attention-deficit hyperactivity disorder a risk fac¬tor for dental caries? A case-control study. Caries Res. 2004:38(1):29-33.
3. Blomqvist M, Holmberg K, Fernell E, Ek U, Dahllöf G. Oral health, dental anxiety, and behavior management problems in children with attention deficit hyperactivity disorder. Euro J Oral Sci. 2006:114(5):385-390.
4. Blomqvist M, Holmberg K, Fernell E, Ek U, Dahllöf G. Dental caries and health behavior in children with attention deficit hyperactivity disorder. Euro J Oral Sci. 2007:115(3):186-189.
5. Blomqvist M, Ahadi S, Fernell E, Ek U, Dahllöf G. Dental caries in adolescents with attention deficit hyperactivity disorder: a population-based follow-up study. Euro J Oral Sci. 2011:119(5):381-385.
6. Chandra P, Anandakrishna L, Ray P. Caries experience and oral hygiene status of children suffering from attention deficit hyperactivity disorder. J Clin Pediatr Dent. 2009;34(1):25-29.
7. Grooms MT, Keels MA, Roberts MW, McIver FT. Caries experience associated with attention-deficit/hyperactivity disorder. J Clin Pediatr Dent. 2005;30(1):3-7.
8. Hidas A, Noy AF, Birman N, et al. Oral health status, salivary flow rate and salivary quality in children, adolescents and young adults with ADHD. Arch Oral Biol. 2011:38(1):29-33.
9. Hidas A, Birman N, Noy AF, et al. Salivary bacteria and oral health status in medicated and non-medicated children and adolescents with attention deficit hyperactivity disorder (ADHD). Clin Oral Investig. 2013;17(8):1863-1867.
10. Stookey GK. The effect of saliva on dental caries. J Am Dent Assoc. 2008;139 Suppl:11S-17S.
11. Wender PH. ADHD: Attention-Deficit Hyperactiv¬ity Disorder in Children and Adults. Oxford University Press: New York. 2000.
12. Kohlboeck G, Heitmueller D, Neumann C, et al. Is there a relationship between hyperactivity/inattention symptoms and poor oral health? Results from the GINIplus and LISAplus study. Clin Oral Investig. 2013;17(5):1329-1338
13. Rindal DB, Rush WA, Peters D, Maupomé G. Antidepressant xerogenic medications and resto¬ration rates. Community Dent Oral Epidemiol. 2005:33(1):74-80.
14. Maupome G. Diverse components of the oral environment in attention-deficit hyperactivity disorder (ADHD) make it difficult to establish whether ADHD is a risk factor for dental caries. J Evid Based Dent Pract. 2005:5(1):39-40.
15. William Wrigley Jr. Company. Dry Mouth and Salivary Flow. Drymouth.info [Internet]. 2013 March [cited 2014 January] Available from: http://www.drymouth.info/practitioner/salivaryFlow.asp
16. Bardow A, Nyvad B, Nauntofte B. Relationships between medication intake, complaints of dry mouth, salivary flow rate and composition, and the rate of tooth demineralization in situ. Arch Oral Biol. 2011:46(5):413-423.