You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Patients present with many deficiencies, including loss of vertical dimension, dental caries, esthetic and speech concerns, periodontal disease, and arch discrepancies. A thorough diagnosis and evaluation of their prognosis is pertinent to making the appropriate clinical treatment planning decisions. It is most important that the patient’s chief complaints are understood and that a good dialogue is established to highlight different treatment options and the potential effectiveness of these options.
Periodontal and prosthodontic treatment goals include working with an interdisciplinary team for diagnosis, the elimination of disease, and the restoration of esthetics and function.1-3 After a detailed intraoral exam, diagnostic records should include a photographic series of the face and lip profile, smile, centric occlusion, and all excursive movements of the anterior and posterior teeth. In addition, diagnostic casts should be made and mounted with a facebow on an Arcon articulator. Ideally, an electronic pantographic analysis is recorded to set the articulator accurately and record the functional potential of the mandibular condyles. With these casts, initial observation of the tooth position, mandibular movement, and plane of occlusion can be assessed, and changes in the vertical dimension can be contemplated.4 Once vertical dimension is established, a diagnostic wax-up is created. This diagnostic wax form can be discussed with the patient in light of the photographic series to have the patient better understand the treatment options and goals prior to initiating therapy. Once the treatment plan is determined, the diagnostic wax-up can be duplicated and a laboratory heat-processed provisional can be fabricated.
Complex prosthodontic care almost always requires an interdisciplinary approach. This entails allowing time for potential orthodontic therapy to place teeth and bone in more favorable positions, and periodontal therapy to eliminate disease, rebuild gingival and bone foundations, and place dental implants. In the past, the restorative dentist would prepare all the teeth and place provisional restorations as soon as possible, but today the complexities of modern therapies often require more time for wound healing, which may delay the completion of treatment. If there are preliminary surgical procedures with longer healing times, these may be considered prior to tooth preparation and placement of provisional restorations to reduce the duration of the provisional restorations and issues associated with long-term provisionals, which include cement washout and recurrent caries. Initial therapy should include control of active disease and dental caries, patient education, and oral hygiene; endodontic therapy should be performed as indicated. In addition, hopeless teeth should be extracted and nonsurgical periodontal therapy provided.
Interdisciplinary care requires a commitment to communication, not only directly with the patient but also between treating professionals to confirm the diagnosis, prognosis, and treatment plan.5 This report presents cases managed with varying levels of surgical and restorative coordination of care. The periodontal surgical therapy and prosthodontic care shown was directed by the diagnosis and treatment plan. The following case examples are included:
1. Maxillary full-coverage crown restorations for esthetic and functional occlusal rehabilitation.
2. Utilization of gingival ceramics to manage an esthetic defect of papilla loss.
3. Periodontal–prosthodontic–implant reconstruction with 10-year follow-up.
4. Full-mouth reconstruction of a patient presenting with partial edentulism, supra-eruption, and loss of vertical dimension.
Case 1
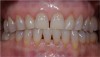
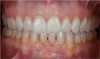
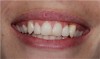
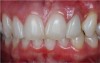
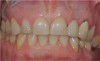
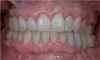
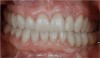
A 28-year-old woman in excellent health presented chiefly to enhance her dental esthetics and eliminate the central diastema (Figure 1 and Figure 2). While this seemed to be a potential veneer case, a comprehensive diagnosis—including the evaluation of mounted models on a fully adjustable articulator—confirmed the clinical findings of vertical dimension collapse and a lack of posterior occlusion on the left side. It was not possible to treat this occlusal factor with only veneer therapy or by limiting treatment to the anterior dentition. The treatment plan was for maxillary full-coverage crown restorations with lithium disilicate to maximize esthetics, strength, and wear of the opposing teeth.6 The periodontium was healthy and there was adequate gingival symmetry, so there was no need for periodontal surgical intervention.
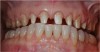
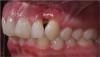
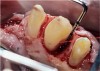
The teeth were prepared without violating the biologic width with intracrevicular preparations (Figure 3) and final impressions were made to establish master models, which were mounted using an electronic pantographic record. This record determined the condylar settings necessary to set an Arcon articulator. (There are now many articulators that are fully adjustable and easily programmable.) The master casts were made and mounted with a facebow to an Arcon articulator.
Creating an occlusion that conforms to the patient’s movements and that can minimize overloading and lateral forces on all of the prosthetic teeth is significant to the long-term survival of the prosthesis.7 This can be achieved with the sequential disclusion concept first described by the gnathological school.8,9 This concept maintains that occlusal anatomy and disclusive movements are determined by condylar guidance and are modified by incisal guidance. Therefore, in harmony with different anterior guide angles, the first molar would separate the second molar in all movements; then the second bicuspids would separate the molars, after which the first bicuspids would separate the teeth posterior to them; and, finally, the cuspids would separate all the posterior teeth. According to the theory, with time and wear, a protective and reverse pattern occurs, protecting the most vulnerable posterior teeth and ceramics. Using this approach, the electronic pantographic record program would determine the anterior disclusive angles of the anterior table; however, it should be noted that with some articulators, the angles are interpreted as inserts that are placed on the anterior table.
The appropriate time for patients to state their preferences regarding the esthetic design is before the final ceramic restorations are designed. This is accomplished with a treatment wax with a complete white wax-up of the case (Figure 4 and Figure 5), which can be inserted so the patient and clinician can evaluate function and esthetics. There must be symmetry between the restorations and the facial planes. The effect of the wax-up on speech—for example, F and V sounds—and the lip support for the nasolabial folds are checked. The patient has a chance to input the design of the tooth form and size at a stage when it can be easily altered chairside or returned to the laboratory for major corrections and a second wax try-in. Once the wax-up is approved, the fabrication of the final restorations can proceed.
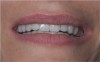
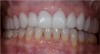
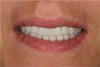
The occlusion is not just how the teeth “come together;” it is functional in centric and excursive movements. By using a fully adjustable articulator, the forced moments on the ceramics can be diminished to reduce overloading and the potential for failure. The final result meets the patient’s treatment goals (Figure 6 and Figure 7) with closure of the diastema and symmetry between the dental and facial esthetics.
Case 2
A 26-year-old woman presented with a history of previous biopsy of a squamous odontogenic cyst at the distal interproximal of the maxillary left lateral incisor. There was recurrence of the lesion and a 7-mm probing depth, recession, and loss of interdental papilla. A regenerative procedure was desired for both the periodontal support and esthetics; however, the recurrence of the lesion was an indication for further biopsy. The site was surgically evaluated with biopsy, which confirmed benign pathology, and regenerative therapy. Due to the limited papillary tissues, there was secondary intention healing at the site, which was monitored for approximately 12 months and evaluated for further treatment options.
At this phase, there were multiple treatment options. The clinical photographs demonstrate the extent of the esthetic defect (Figure 8 and Figure 9) with loss of the interdental bone and soft tissues. There was a guarded prognosis for the maxillary left lateral incisor. The patient was presented with the following treatment options:
1. Regenerative surgical treatment
2. Orthodontic extrusion followed by:
a. crown restoration
b. extraction of the lateral incisor and replacement with:
• a cantilever prosthesis extending from the maxillary left canine
• dental implant replacement
c. extraction of the maxillary left canine and lateral incisor, and a dental implant–supported cantilever prosthesis with the implant at the site of the canine.
3. Crown restoration of the lateral incisor with gingival ceramics to solve the esthetic deficiency
These options were thoroughly presented to the patient and she selected to proceed with the prosthodontic solution.
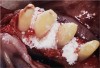
A single crown was designed with gingival ceramics onto the papilla site to solve the esthetic problem that clearly existed for her (Figure 10 and Figure 11).10 The treatment solution, as evidenced in the postoperative radiograph (Figure 12), kept the other treatment options open in the event of recurrent disease for the lateral incisor.
In complex treatment, patients have often lost significant bone and soft-tissue support, and grafting procedures may not be able to restore the arch to its ideal form. The loss of tissue can be both horizontal and vertical. A removable prosthesis can, with a gingival acrylic flange, restore some of the tissue and create better lip form. In fixed prosthodontics, gingival ceramics—with or without dental implants—can be used to restore esthetics and arch form. Gingival ceramics can correct gingival residual ridge defects and can restore gingival/tooth symmetry. This can be applied to a full-arch prosthesis or a single-tooth restoration, as in this case example.
As her high smile line had this large triangle, there was a significant psychological deficit for her. Her goal to have this remedied was significant. However, this is an area where regenerating that amount of papillae is very unpredictable, and other options were fairly unpredictable. In this case, using a pure prosthetic solution, it was possible to satisfy her needs and reach an endpoint more quickly. This case demonstrated how using the prosthetic in addition to growing tissue surgically allowed for a more predictable approach with a very esthetic result for gingival ceramics. The treatment result, which afforded adequate access for oral hygiene with flossing around the prosthesis, had a significantly positive psychological impact for the patient, who had been extremely self-conscious about the “black triangle.”
Case 3
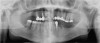
A 57-year-old man presented in 2000, when full-mouth radiographs were available (Figure 13). This case represents many of the principles encountered on a daily basis while attempting to provide periodontal-prosthetic reconstruction. Most patients desire to keep their natural teeth healthy. Traditional periodontal–prosthodontic concepts include rehabilitation with a second bicuspid occlusion.1,2 In this patient, who had functioned with missing molar teeth, the second bicuspid (mandibular left first molar) was restored. Before deciding on dental implant treatment, periodontal disease was treated with the goal of regenerating the damaged periodontal support to establish periodontal health and maintain natural teeth in a healthy environment, as it is necessary to maintain optimal health before proceeding with prosthetic rehabilitation. In this case, implant restoration was limited to the maxillary left quadrant; regenerative therapy was provided in the mandibular right quadrant, a root section for the mandibular left first molar, and a fixed partial denture (FPD) was placed in the maxillary right quadrant. All of the remaining natural teeth were maintained, with the exception of the maxillary right lateral incisor, the mandibular right central incisor, and the left central incisors, which were extracted.
Periodontal health must be established prior to beginning final prosthodontic therapy. The guidelines for treatment include pocket elimination and establishing an adequate zone of attached gingiva for the abutments.3,11,12 This patient followed a 3-month periodontal health maintenance program, as without a plan for maintenance and oral hygiene for the patient, the overall success would be compromised.
The necessity for pocket reduction is increased at sites receiving prosthodontic treatment and especially for strategic abutments for a long-span FPD.3 It is also known that sites with angular defects are likely to progress over time if not treated.13 The plan in this case was to use a periodontal regenerative procedure to treat the 5-mm interdental defect on the distal mandibular right canine, which extended to a 5-mm to 6-mm circumferential defect on the lingual surface (Figure 14). This was treated with a combination of a mineral collagen bone substitute,14 a xenograft in a collagen matrix, combined with enamel matrix derivative (Figure 15).15
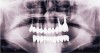
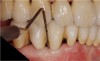
The 10-year postoperative panoramic radiograph (Figure 16) demonstrates the success of the reconstruction and the periodontal and dental implant foundation. The implants for the maxillary left quadrant are supported in regenerated bone where sinus grafting was performed, and the mandibular right canine and bicuspids have been stable with gain of clinical attachment and radiographic suggestion of bone fill after the periodontal surgical care. There is mild recession, especially for the maxillary anterior abutments, after 10 years of maintenance; however, the case is remarkably stable and healthy radiographically and clinically (Figure 17). There is minimal sulcular depth for the previously deep pocket on the distal aspect of the mandibular right canine (Figure 18). The results demonstrate the potential for longevity following periodontal-prosthodontic principles of treatment.
Case 4
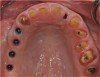
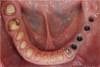
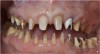
This patient previously presented with esthetic concerns but was reluctant to proceed with reconstructive dental treatment (Figure 19 and Figure 20). She had been monitored for several years and advised of the benefits of an interdisciplinary treatment plan including periodontal, dental implant, and prosthodontic therapy. The diagnosis included occlusal trauma, loss of vertical dimension, lack of posterior tooth support, and supra-eruption. There was also gingival asymmetry, lack of attached gingiva, lateral ridge defect for the mandibular left molar region, pneumatization of the maxillary right sinus, and alloy tattoo of the gingiva for the maxillary right bicuspids. Eventually the mandibular left second bicuspid, which was an abutment for a fixed partial denture, fractured, resulting in an abscess and significant bone loss localized to this abutment tooth (Figure 21). At this point, given the need for extraction and now more limited posterior chewing capability, the patient requested a comprehensive consultation and treatment plan for the reconstructive therapy she had previously elected to postpone.
The first step was the emergent management of the fractured mandibular left bicuspid. This tooth was extracted and a ridge preservation procedure was performed for this site. There was advanced bone loss with the intrabony defect adjacent to the fractured root extending 6 mm. The site was grafted with a growth factor-enhanced bone matrix combining freeze-dried bone allograft (RegenerOss™, Biomet 3i, http://biomet3i.com) with recombinant human platelet-derived growth factor-BB (GEM 21S®, Osteohealth, www.osteohealth.com) protected by an absorbable collagen membrane (Bio-Gide®, Osteohealth).16,17 After the site had healed and further consultation with the patient, a comprehensive treatment plan with the sequential steps for the coordinated therapy was accepted by the patient and allowed to proceed as directed.
It is important to consider multiple factors in the timing of treatment. For this patient, it was decided to commence with mucogingival surgery, bone augmentation procedures, and the first phase of dental implant treatment before placing provisional restorations:
• Free gingival grafting on teeth Nos. 19 through 22 and 27 through 29
• Maxillary labial frenectomy
• Maxillary right sinus augmentation
• Mandibular left lateral ridge augmentation on teeth Nos. 18 and 19
• Implant placement in teeth site Nos. 2, 3, 18, 19, 20, and 21
Once this surgical phase of treatment was completed, the next step was to proceed with the placement of provisional FPDs following the diagnostic wax-up. This was followed by the majority of the remaining surgical therapy, which was conducted in one procedure with the adjunctive use of conscious sedation to avoid multiple surgical visits:
• Extraction of tooth No. 4
• Implant placement in teeth sites Nos. 4, 5, and 10
• Connective tissue graft ridge augmentation of tooth No. 10
• Alloy tattoo removal/free gingival graft of teeth Nos. 4 and 5
• Pre-prosthetic crown lengthening/apically repositioned periodontal surgery on teeth Nos. 6 through 9, 12 through 15, and 22 through 31
Once the healing was complete for the periodontal and dental implant procedures (Figure 22 and Figure 23), the final tooth preparations were completed and final impressions were made; records, including the electronic pantographic record, were then obtained. The treatment wax was used (Figure 24) to secure the patient’s approval of the esthetic design and to evaluate the esthetics and plan for the final prosthesis, including the cross-bite. The vertical dimension was raised, the facial anatomy was checked, and her speech and esthetics were checked by filming the patient and viewing facial profiles. Next, the implant abutments were made (Figure 25). In this case, metal–ceramic abutments were chosen; they were tried on before beginning the fabrication of the final restorations. These monolithic ceramic materials use lithium disilicate, which can result in a restoration with excellent biomechanical and esthetic properties (Figure 26 and Figure 27). The restorations were observed; the radiographs show the implants placed in the regenerated bone (Figure 28).
Conclusion
Periodontics and prosthodontics working together can provide interdisciplinary care for dental rehabilitation. The treatment should be guided by accurate diagnosis, prognosis evaluation, and coordinated treatment planning. Utilization of modern technology and surgical and restorative biomaterials enhances the therapeutic result for patients.
References
1. Amsterdam M. Periodontal prosthesis. Twenty-five years in retrospect. Alpha Omegan. 1974;67(3):8-52.
2. Nyman S, Lindhe J. Prosthetic rehabilitation of patients with advanced periodontal disease. J Clin Periodontol. 1976;3(3):135-147
3. Nevins M, Skurow HM. Periodontics and restorative dentistry: the clinical interrelationship. CDA J. 1984;12(4):101-105.
4. Malament KA. Pietrobon N, Neeser S. The interdisciplinary relationship between prosthodontics and dental technology. Int J Prosthodont. 1996;9(4):341-354.
5. Malament KA. Periodontics and prosthodontics: goals, objectives, and clinical reality. J Prosthet Dent. 1992;67(2):259-263.
6. Culp L, McLaren EA. Lithium disilicate: the restorative material of multiple options. Compend Contin Educ Dent. 2010;31(9):716-725.
7. Malament KA. Achieving quality esthetic dentistry and integrated comprehensive care with new generation techniques and materials. J Okla Dent Assoc. 2005;95(7):26-29.
8. McCollum BB, Stuart CE. A Research Report. South Pasadena, CA: Scientific Press; 1955.
9. McCollum BB, Evans RL. The gnathological concepts of Charles E. Stuart, Beverly B. McCollum and Harvey Stallard. Georgetown Dent J. 1970;36(1):12-20.
10. Malament KA, Neeser S. Prosthodontic management of ridge deficiencies. Dent Clin North Am. 2004;48(3):735-744.
11. Nevins M, Skurow HM. The intracrevicular restorative margin, the biologic width, and the maintenance of the gingival margin. Int J Periodontics Restorative Dent. 1984;4(3):30-49.
12. Wilson RD, Maynard G. Intracrevicular restorative dentistry. Int J Periodontics Restorative Dent. 1981;1(4):34-49.
13. Papapanou PN, Wennström JL. The angular bony defect as indicator of further alveolar bone loss. J Clin Periodontol. 1991;18(5):317-322.
14. Nevins ML, Camelo M, Lynch SE, et al. Evaluation of periodontal regeneration following grafting intrabony defects with bio-oss collagen: a human histologic report. Int J Periodontics Restorative Dent. 2003;23(1):9-17.
15. Giannobile WV, Somerman MJ. Growth and amelogenin-like factors in periodontal wound healing. A systematic review. Ann Periodontol. 2003;8(1):193-204.
16. Lynch SE, Wisner-Lynch L, Nevins M, Nevins ML. A new era in periodontal and periimplant regeneration: use of growth-factor enhanced matrices incorporating rhPDGF. Compend Contin Educ Dent. 2006;27(12):672-8.
17. Nevins ML, Reynolds MA. Tissue engineering with recombinant human platelet-derived growth factor BB for implant site development. Compend Contin Educ Dent. 2011;32(2):18, 20-27.
About the Authors
Kenneth A. Malament, DDS, MScD
Boston Prosthodontics Dental Group
Boston, Massachusetts
Marc L. Nevins, DMD, MMSc
Boston Periodontics & Dental Implants
Boston, Massachusetts
Thomas Singh, MDT
Boston Prosthodontics Dental Group
Boston, Massachusetts