You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Dentistry is a sedentary occupation with occasional lifting, prolonged sitting in awkward positions, minimal walking, little movement, and considerable standing. Together, these factors can produce muscle pain and likely musculoskeletal disorders (MSDs), including shoulder injuries, as well as poor posture or fatigue. Musculoskeletal pain commonly affects general dentists, followed by dental specialists, dental assistants, and dental technicians,1 with females being most affected.
The World Health Organization (WHO) defines MSD as "a disorder of the muscles, tendons, peripheral nerves, or vascular system not directly resulting from an acute or instantaneous event (eg, slips or falls)." MSDs are neuromuscular impairments due to increasing or repetitive movements at low-intensity loads.1 Repeated movements prevent the tissues from regenerating and cause micro-injuries in specific body parts. MSDs are the world's second-largest cause of disability, rapidly becoming a global healthcare issue.2
MSDs often occur due to incorrect posture, but awareness and early preventative practices may minimize injury.3 These disorders include regional neck and shoulder pain, shoulder tendonitis, neuropathy, tension neck syndrome, and trapezius myalgia.4 Other risk factors include the use of inadequate non-ergonomic equipment, muscle use and effort, and vibrating instruments.
Shoulder Injuries Among Dental Professionals
Dental professionals often work in a seated position, slouching and leaning forward, placing pressure on the shoulders and back. Rotator cuff muscle imbalance and strain may occur with shoulder pain and inflammation. Shoulder injuries due to poor posture and repetitive motions can occur, leading to strain on the shoulder joint, inflammation, and pain. Awkward positions may prevent dental professionals from attaining the correct angle to perform specific procedures and place additional stress on the shoulders. Shoulder joint strain also occurs when dental professionals reach over a patient's head when working on their upper teeth.
The types of shoulder injuries common in dentistry include trapezius myalgia, which results from static and prolonged shoulder elevation and forward head posture with pain symptoms and upper trapezius stiffness or tightness. Rotator cuff tendonitis occurs when dental professionals hold their elbow above waist level and the upper arm away from the body, causing shoulder area tendon inflammation, soft-tissue tearing, shoulder joint bone spurs or abnormalities, and poor shoulder posture. Thoracic outlet syndrome may result from nerve, arteries, and vein compression through the neck to the arm (thoracic outlet), causing neck, shoulder, arm, or hand pain, finger numbness or tingling, muscle weakness or fatigue, or cold sensations within the arm, hand, or fingers.
Shoulder joint area MSDs include diagnoses of rotator cuff syndrome due to dynamic heavy loads. Low external loads and repeated or sustained exertion pose upper shoulder problems. Dental professionals report an average pain level of 4 on a 7-point scale based on combinations of postures, force, frequency, duration, past injuries, and present discomfort.4
Shoulder Ergonomics
Ergonomics is the applied science of designing products and procedures for maximum efficiency and safety; it studies personnel, equipment, and work area environment relationships.5 Ergonomic factors address static postures that result in fatigue, the effect of instrument usage on upper extremity pain, repetition, forceful exertions (eg, tooth extraction), contact stress, improper work habits, and stance, all of which may cause significant muscle pain and skeletal disorders, including hand, elbow, shoulder, back, and head pain. Common dentistry MSDs include symptoms of pain or weakness, decreased range of motion, impaired coordination, and an impaired sense of touch as itching and/or numbness.6 Proper ergonomic design helps prevent repetitive strain injuries.
A dental professional's job performance may become significantly impacted by work-related shoulder injuries, resulting in decreased job productivity, a loss of earnings, and reduced daily activity performance. The ability to perform specific procedures or hold instruments may become affected by shoulder pain and inflammation, potentially leading to increased errors. Long-term effects may cause additional MSDs or shoulder injuries, require surgery, or force early retirement.
The critical factors of shoulder ergonomics include posture, force, and frequency. Awkward posture leads to non-neutral positions, preventing the body from being in a natural, relaxed position. During procedures, force is excessive weight, grip, or pressure on the body. Performing tasks that require excess force can produce muscle, tendon, joint, and/or soft-tissue damage, leading to fatigue and discomfort. An example would be holding small instruments for extended periods, which can create excess gripping force. Frequency refers to how often an action is performed.
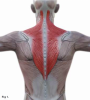
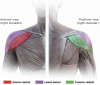
The goals of shoulder ergonomics include the prevention of work-related MSDs and MSD conditions, increased safety and productivity, enhanced performance by eliminating unnecessary effort, and improved patient standards of care.7 Without appropriate ergonomic support, dental professionals are commonly affected by pain or discomfort in the upper trapezius (Figure 1), lateral deltoid, and anterior deltoid (Figure 2) muscles when performing repeated actions on the dominant side.8
Chronic disorders and permanent career-ending injuries may occur if dental professionals ignore back, neck, shoulder, or arm pain symptoms. Studies have found that up to 81% of dental operators experience pain in these areas.9 A study by the American Dental Association revealed that two-thirds of responding dentists reported neck and lower back pain, with half describing the pain as moderate or severe.10 Dental professionals must balance maintaining a natural and comfortable posture while providing the most accurate and optimal treatment to the patient without sacrificing proper body ergonomics to attain better procedural vision. Repetitive movements over the long term require adequate visibility and replicated upper limb activity.
Ergonomic Assessment Tools
Advancements like ergonomically designed equipment and professional workplace assessments aim to reduce dentistry's toll on the body; however, making adjustments before pain begins remains challenging for dental clinicians.11 Many assessment tools are available to help identify muscle fatigue, injury, or pain. These include pain scales and functional assessments (eg, the Quebec back pain disability scale and the disabilities of the arm, shoulder, and hand [DASH] questionnaire), shoulder and cervical range of motion tests, motion analyses, muscle activity assessments, posture assessment instruments, and the modified-dental operator posture assessment instrument.
In addition, the rapid upper limbs assessment (RULA) uses a kinematic approach to evaluate the neck, shoulders, trunk, and hands. RULA identifies posture and ergonomic risks in dental professionals regarding muscle fatigue and pain.12 The rapid entire body assessment (REBA) is a systematic process to evaluate whole-body postural MSDs and job-related risks.13 REBA studies showed that 90% of dentists have unfavorable working postures and are susceptible to moderate to high risk of future MSDs. Lastly, the baseline risk identification of ergonomics factor (BRIEF) surveys a nonspecific body part, considering posture, force, duration, physical ergonomics, and load related to upper limb disorders and shoulder pain among dental professionals.14
Ideal Posture for Dental Professionals
Factors that cause poor posture include5: performing procedures while the neck is in flexion and tilted to one side (Figure 3), elevated shoulders, left or right side bending, excessive twisting, forward bending or overreaching at the waist, flexed and abducted shoulders, flexing the elbows more than 90 degrees, flexed or deviated wrists when grasping, hyperextension of the thumb, maintaining a position for more than 40 minutes per patient, and obesity.15
A static posture may increase the risk of MSDs and shoulder injuries. Static postures occur when more than half of the muscles contract during a motionless position against gravity, requiring more effort. A prolonged static posture causes muscle fatigue and imbalance. In addition, a prolonged static posture can elongate and weaken the stabilizing shoulder muscles, such as the middle and lower trapezius, rhomboid, and serratus anterior muscles. The long-term effect reinforces pulling the shoulder blades away from the spine and causes a rounded shoulder. The muscle adapts to the new position, and returning to the correct position becomes uncomfortable. Although dental professionals need to sit for most treatment purposes, a standing posture is best to reduce pressure on the back.16 Therefore, dental professionals should alternate between sitting and standing while utilizing optimal ergonomic techniques and promoting positive patient outcomes.
Improper and static posture also places pressure on nerves and blood vessels, leading to excessive muscle strain, decreased oxygen circulation, and wear on joint structures.15,16Rounding the shoulders may compress nerves, arteries, and veins, leading to upper extremity symptoms. Oxygen intake becomes limited with poor thoracic alignment. Diminished oxygen produces fatigue and loss of concentration. The dentist and dental assistant should participate in the four-handed dentistry approach, working together carefully and deliberately.17The dental chair arrangement and work area for the dental assistant is critical, as the assistant plays a vital role in four-handed dentistry, handing instruments to the dentist while the dentist performs the procedure. The four-handed dentistry approach enables the dentist to maintain a position around the operating field with limited hand, arm, and body movement and confine eye focus to the working field.17 Ergonomically, over-the-head and over-the-patient delivery systems better allow dental assistants to access handpieces.
Dental professionals should maintain the body posturing guidelines outlined in Table 1 and a neutral posture at the 11-12 o'clock position.18-20 Also, there needs to be sufficient workspace, and awkward bending, twisting, and reaching should be avoided to prevent discomfort.
Body Mechanics, Stretching, and Exercising
Correct body mechanics help prevent shoulder injuries. Dental professionals should understand how to maintain proper posture while using procedures with the least force possible. One can retrain one's shoulders and arms to position the hands to avoid forceful movements of the fingers. Dental professionals must avoid excessive wrist movements and adjust their body to a neutral position by alternating work positions between sitting, standing, and performing procedures on the opposite side of the patient. Shifting positions alters muscle stress to other muscles and allows relaxation.
Stretching and exercising can help prevent muscle imbalances and reduce injury risk. Dental professionals should perform whole-body stretching and body strengthening exercises for 15 to 30 seconds after each patient's treatment and at the end of the workday. Frequent breaks throughout the day help avoid muscle stress and shoulder injury.
Benefits of stretching include increased muscle blood flow, increased joint synovial fluid production, reduction of trigger point formation, maintenance of normal joint range of motion, increased vertebral disk nutrient supply, a central nervous system relaxation response, warming up of muscles before procedures, and identification of tight structures before injury predisposition.21,22
Shoulder rotation shrugging stretches the shoulder muscles. Other exercise-related activities beneficial to staying pain-free and reducing pain include weight training, cardiovascular exercise for 30 minutes at least three times a week, daily foam rolling, stretching, and weekly yoga. Healthy exercise and stretching habits promote easier ergonomic changes in the office to reduce MSD or shoulder injury risk.11
Patient Positioning
The patient should be positioned supinely according to the dental professional's natural posture to prevent physical stress. Conversely, when the patient is supine, positioning the oral cavity above the clinician's mid-chest level will limit the visual field and increase the rate of shoulder fatigue.9
The clinician should maintain a neutral position when positioning the patient by keeping the upper arms close to the body, supporting the elbow/forearm angle close to 90 degrees, and ensuring that the wrists align with the forearm, with no more than 20- to 30-degree extension.
Workstation Setup
Dental professionals' workstations should promote neutral positions, reduce position-related stress, and lessen shoulder strain. Ergonomists recommend the workstation be close to the dental professional, at a distance of about the length of the forearms, or 10 inches away, to protect the shoulders, neck, and back.9
Elements of an improper workstation setup include: the clinician's chair being too high or low; a lack of lumbar, thoracic, or arm support on the chair; improper positioning of the instrument table; inadequate lighting; the workstation or table having sharp or uncomfortable edges; and a damp or cold work environment.
Seating, Chairs, and Stools
The clinician's dental chair or stool should have five wheels, a supportive backrest, and a seat that prevents falling back.6 A dental stool must be compact to not impede the actions of the feet, foot controls, or the patient's chair but must be wide enough to allow movement. The patient's chair should have foot control to prevent accidental chair movements.23 The clinician's chair must have a rigid cast frame construction to sustain repeated stress throughout continuous use.
A chair should have adjustable height, adequate width, tilting capability, a backrest, seat pan, and armrest features. The armrests should be adjusted according to height and operator comfort to decrease back and shoulder fatigue, support the elbows, and stabilize the lower back curve.16 The clinician's spine and thighs should angle 90 to 110 degrees when the feet rest flat on the floor, and the buttocks should be snug against the back of the chair. The angle of the chair should be altered depending on the clinician's shoe variations, whether heels or flats. Adjusting the chair to a comfortable height can prevent shoulder elevation, and positioning the chair close to the patient minimizes forward bending or excessive leaning over the patient. Clinicians must also account for their height and determine their seat adjustment accordingly. Regarding height, they should function with their thighs parallel to the floor and fully supporting their legs.
Using an appropriate ergonomic chair or stool aids lower muscle activity and better posture by reducing the flexion of the spine.8 Dental stools should have elbow rests below the seated elbow height to prevent shoulder elevation. During frequent dental procedures, elbow rests may reduce upper trapezius muscle load, frequency, and arm abduction range. Individuals typically work with their legs slightly separated, with the sole of their feet resting on the stool.6
The patient chair should have a flat surface, be stable, and have appropriate drop-down armrests, headrests, neck, wrist, and forearm support.16
Instrument Tray and Tool/Equipment Selection
The instrument tray or table should be positioned close to and higher than the patient and the patient's chair to prevent the clinician from overextending the back, shoulders, and arms to reach the instruments. Also, the instrument tray or table should be placed on the clinician's dominant side to avoid twisting the body (Figure 4). Automatic handpieces should be utilized instead of manual instruments to reduce prolonged periods of grasping small instruments. Frequently used instruments should be placed closer to the operator, typically within 22 to 26 inches, to prevent reaching.
Using instruments that reduce forceful exertion should help the clinician maintain a neutral posture and a position of comfort. The use of color coding may help to identify instruments quickly. Among the difficulties of using dental instruments is the small diameter of the handles (usually between 3/16" to 4/16" in diameter); often, a fitted-grip instrument provides sufficient hold.15 Ergonomically advantageous features of hand instruments include7,17: hollow or resin handles for lighter weight and better grip; a positive locking feature to prevent spinning of the handle, such as found on Mathieu pliers, which allows the operator to maintain an upright position without requiring shoulder stress to hold, place, or tie ligatures and elastics; round, knurled, or compressible handles to reduce pinch grip force, muscular stress, and digital nerve compression; and carbon steel construction for sharp-edged instruments. In addition, dull instruments should be replaced to minimize the application of excess force.
Automated instruments, such as high-speed or low-speed handpieces, belt-driven drills, lasers, ultrasonic scalers, and endodontic handpieces, should be considered instead of manual hand instruments. Such instruments should be lightweight, well-balanced in weight (preferably cordless), and have sufficient power and built-in light sources. Angled design is preferred versus straight-shank. Hoses should be pliable and lightweight, and extra length should be avoided as this adds weight, may influence muscle fatigue, and can become coiled. Instruments should have easy activation, such as with a foot pedal or handle turn, to avoid sustaining a pinch grip for prolonged periods. Swivel mechanisms are also ergonomically beneficial.
Light, Magnification Lenses, and Loupes
Adjust the position of the dental light to avoid neck strain or shoulder injury. The light can be positioned behind the dental professional's head and parallel to their visibility line or within 15 degrees of inclination to avoid a shadow effect (Figure 5).24
The use of both a magnification lens and an ergonomic stool creates a significant decrease in muscle activity.8 However, although adequate magnification and lighting reduce movement and enable longer work without a break, it leads to a static position.25 Static positions should be avoided to minimize fatigue, pain, or physical damage by taking frequent stretching breaks and using ergonomic tools effectively. A loupe allows dental professionals to maintain an upright posture and reduces neck flexion (Figure 6). Additionally, improving the field of vision reduces the need to bend forward and lessens trunk flexion. Using lights, magnification lenses, and loupes helps maintain a comfortable working distance and reduces an awkward working position.
Other Considerations
Environment.The work area should be warm enough to avoid decreased circulation and extremity blood flow. The presence of reduced nutrient and oxygen supply with lactic acid and other accumulation of metabolites results in fatigue, pain, and tissue damage.9 The operator's hand temperature should be maintained at a minimum of 77°F to optimize dexterity and grip strength; thus, the work environment should not be too cold.
Scheduling.Appointments should be scheduled according to difficulty and time requirements with appropriate breaks to prevent MSDs and allow recovery. Buffer intervals should alternate between easy and challenging procedures.
Training.Shoulder ergonomics and injury prevention require the training of dental professionals to include workplace hazards and implementation for improvement. Dental schools are showing a growing awareness of the need to provide students with adequate teaching and training in ergonomics.26 Dental students and professionals must understand the ill effects of bad posture and poor ergonomics to prevent shoulder injuries.27
Conclusion
Dental professionals risk musculoskeletal disorders and shoulder injuries due to the repetitious and passive aspects of dentistry. Using adequate ergonomic tools correctly can help relieve fatigue, prevent painful tension on frequently used muscle groups, and promote a longer dental career. Clinicians must utilize shoulder ergonomic tools, such as appropriate body mechanics and posture, stretching, exercise, patient positioning, instrument tray positioning, equipment selection processes, light magnification, and workstation improvements, including the chair and stool. Acknowledging the necessity of dental ergonomics promotes the well-being of dental professionals and improves patient safety.
About the Author
Valerie Smith, ADN
Registered Nurse, Prisma Health Greenville Memorial Hospital, Greenville,
South Carolina
Queries regarding course may be submitted to authorqueries@broadcastmed.com.
References
1. Šćepanović D, Klavs T, Verdenik I, Oblak Č. The prevalence of musculoskeletal pain of dental workers employed in Slovenia. Workplace Health Saf. 2019;67(9):461-469.
2. Datkar D, Sibal A, Kale B. Ergonomics in dentistry: a review. JResMedDentSci. 2022;10(7):87-91.
3. Sakzewski L, Naser-ud-Din S. Work-related musculoskeletal disorders in dentists and orthodontists: a review of the literature. Work. 2014;48 (1):37-45.
4. Morse T, Bruneau H, Michalak-Turcotte C, et al. Musculoskeletal disorders of the neck and shoulder in dental hygienists and dental hygiene students. J Dent Hyg. 2007;81(1):10.
5. Sarkar PA, Shigli AL. Ergonomics in general dental practice. People'sJSciRes. 2012;5(1):56-60.
6. Aghahi RH, Darabi R, Hashemipour MA. Neck, back, and shoulder pains and ergonomic factors among dental students. J Educ Health Prom. 2018;7:40.
7. Khatri P, Chhajed S, Patel N. Ergonomics in dentistry. IntJResearchTrendsandInnovation. 2022;7(10):86-89.
8. García-Vidal JA, López-Nicolás M, Sánchez-Sobrado AC, et al. The combination of different ergonomic supports during dental procedures reduces the muscle activity of the neck and shoulder. J Clin Med. 2019;8(8):1230.
9. Ramdurg P, Mendigeri V, Puranik S. An ounce of prevention is worth a pound of cure: ergonomics in dental practice. J Postgraduate Med Educ Res. 2015;49(1):37-42.
10. ADA survey: ergonomic risks in dentistry. OSHA Review website. January 29, 2018. https://oshareview.com/2018/01/ada-survey-ergonomic-risks-in-dentistry/. Accessed November 29, 2023.
11. Rehan K. The physical toll of dentistry. Ontario Academy of General Dentistry website. September 19, 2022. https://agd.org/constituent/news/2022/09/19/the-physical-toll-of-dentistry. Accessed July 31, 2023.
12. Blume KS, Holzgreve F, Fraeulin L, et al. Ergonomic risk assessment of dental students - RULA applied to objective kinematic data. Int J EnvironPublic Health. 2021;18(19):10550.
13. Jahanimoghadam F, Horri A, Hasheminejad N, et al. Ergonomic evaluation of dental professionals as determined by rapid entire body assessment method in 2014. JDent(Shiraz). 2018;19(2):155-158.
14. Chaiklieng S, Suggaravetsiri P. Ergonomics risk and neck shoulder back pain among dental professionals. Procedia Manufacturing. 2015;3:4900-4905.
15. Thakkar R, Katragadda HV, Shah F, et al. Ignorance of ergonomics in dental practice: systematic review. Int J Current Advanced Res. 2018; 7(3(L)):11251-11259.
16. Deshmuk RC, Gomes SR, Acharya SS, Khanapure SC. An overview of ergonomics in dentistry. Indian J Oral Health Res. 2019;5(2):40-45.
17. Gupta A, Bhat M, Mohammed T, et al. Ergonomics in dentistry. Int J Pediatr Dent. 2014;7(1):30-34.
18. Health and Safety Task Team. Ergonomics and Posture Guidelines for Oral Health Professionals. FDI World Dental Federation. 2021. https://www.fdiworlddental.org/ergonomics-and-posture-guidelines-oral-health-professionals. Accessed November 29, 2023.
19. Tyagi N, Sareen M, Rathore S, et al. Dental ergonomics - a questionnaire based cross sectional study. IOSR J Dent Med Sci. 2022;21(13):6-9.
20. Partido BB, Henderson R. Impact of ergonomic training on posture utilizing photography and self-assessments among dental hygiene students and practitioners. J Dent Hyg. 2021;95(3):33-41.
21. Kim ES, Jo ED, Han GS. Effects of stretching intervention on musculoskeletal pain in dental professionals. J Occup Health. 2023;65(1):e12413.
22. Sanders MJ. The benefits of stretching... Dentistry IQ website. January 1, 2007. https://www.dentistryiq.com/dental-hygiene/salaries/article/16351437/the-benefits-of-stretching-. Accessed December 20, 2023.
23. Chavan KA, Radha G, Rekha R. Insights of ergonomics in dentistry. IntJDentMedSciRes. 2021;3(1):364-372.
24. De Sio S, Traversini V, Rinaldo F, et al. Ergonomic risk and preventive measures of musculoskeletal disorders in the dentistry environment: an umbrella review. PeerJ. 2018;6:e4154.
25. Pejčić N, Petrović V, Dimitrijević-Jovanović N, et al. Ergonomics problems in dental profession-dentists working position. Balkan J Dent Med. 2022;26(3):154-160.
26. Katrova LG. Teaching dental ergonomics to undergraduate dental students. Why and how? The experience of the Faculty of Dental Medicine of Sofia, Bulgaria. Stomatological Disease and Science. 2017;1:69-75.
27. Andrew R, Narang S, Aggarwal S, Thongam S. Evaluating knowledge, awareness and behaviour among dental interns regarding ergonomics in dentistry: a cross-sectional survey. Int Healthcare Res J. 2020;4(7):OR1-OR4.