You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
With well-accepted data now linking oral and systemic inflammation and evidence that biofilm is the main etiology of periodontal disease, dental health care practitioners should select therapeutic and at home options that are most likely to affect the identified etiology to optimize treatment outcomes.1 Ultrasonic scaling and the use of prophy paste with a rubber cup polisher are two of the most widely used debridement methods to render the tooth surface free from microbial biofilm, calculus, and stain.2 These debridement methods help stave off the host inflammatory response and provide patients with an esthetically pleasing smile by eliminating the microbial biofilm and surface stain.2 However, evidence has long suggested that the tooth surface can be compromised after debridement procedures.
Polishing procedures contribute to the removal of biofilm and inadvertently, the fluoride-rich, outer layer of enamel, which can take up to three months to rebuild.3,4 Overzealous polishing can cause more damage by abrading the enamel surface and depositing debris into the microcavities created by the procedure.4 Certainly, improper manual and ultrasonic techniques during patient treatment can result in root surface wear and roughness.2 Both debridement and polishing procedures can make the tooth surface more vulnerable to demineralization, placing the patient at greater risk for developing dentinal hypersensitivity and caries.5 The use of fluoride varnish is a common and cost-effective treatment that helps to inhibit demineralization and enhance remineralization while also inhibiting the activity of some bacteria, offering the patient protection in between dental visits.6
Periodontal disease prevention and periodontal disease treatment success relies heavily on the patients accepting their role as co-therapist. For this reason, oral health education is critical during each patient appointment. Research indicates the importance of patient compliance on the success of periodontal therapy.7-9 Oral health education improves patient knowledge and plays a vital role in helping patients understand the oral-systemic benefits of good oral health, seeing value in preventative appointments, and adopting favorable oral health behaviors.7,10 Daily oral health care should include treatments that target microbial biofilm as well. In addition to brushing and interdental care, various home care items that contain hydrogen peroxide such as dentifrices, mouth rinses, and antiseptic gels have been used as an adjunctive therapy in periodontal disease treatment with a long-term safety record.11 In a 2012 study, Putt and Proskin11 demonstrated the effectiveness of using 1.7% hydrogen peroxide gel, locally administered in prescription customized trays to treat patients with moderate to advanced periodontitis.11 In this study, patients showed clinical improvements in pocket probing depth with the use of hydrogen peroxide gel over a three-month period.11 Although the use of whitening strips embedded with hydrogen peroxide has yet to be studied extensively as an adjunctive treatment for periodontal diseases, recommending the use of them could offer patients the benefit of obtaining a whiter smile while inhibiting microbial growth on the tooth surface and under the gumline. They could also serve as a compliance motivator to enhance treatment outcomes.
Worth noting, additional adjunctive therapies have demonstrated efficacy in the treatment of periodontal disease. The addition of Chlorhexidine, cetylpyridinium chloride (CPC), and essential oils to mouthrinses has demonstrated clinical efficacy for therapeutic benefits in the treatment of periodontal diseases when formulated at specific concentrations.12 Another promising adjunctive therapy is the use of oral probiotics, which favorably influence the oral microbiota and offer benefits to the oral ecosystem in periodontal diseases.13
Debride and Polish
While every dental hygiene visit is unique, there is still a wave of activity that occurs around each appointment that is consistent for most offices. During these appointments, clinical and microscopic etiology is removed from the tooth surface via debridement and polishing. The preferred instrument to debride the tooth surface is the ultrasonic scaler, of which there are two main systems used in dentistry: magnetostrictive systems, which operate within the range of 18 kHz to 45 kHz with an elliptical tip motion, and piezoelectric systems, which operate within the range of 25 kHz to 50 kHz with a linear motion.2 It is unclear which system is more efficient in debriding the tooth surface, according to a literature review conducted by Kamath and Umesh Nayak,14 highlighting the need for further research on the subject.2 An in vitro study conducted by Mahiroglu et al2 concluded that magnetostrictive and piezoelectric ultrasonic scalers result in similar wear and roughness effects, while other studies have established similar scaling efficiencies amongst both systems.2,14 What has been established in the literature is that application parameters (power setting, scaling tip design, and user technique) impact scaling efficiencies on the root surface.2,14,15 The key to effective and efficient use of ultrasonic debridement is to select the appropriate ultrasonic insert for the oral conditions, use the selected tip with appropriate power, and employ the correct technique, with an understanding that power settings and tip selections will vary depending on the phase of care and clinical scenario.16 A number of offices house magnetostrictive units that operate at either 25kHz or 30kHz. Most of these scalers require inserts that match their frequencies. This can pose a problem for clinicians who are unsure if they are using an Ultrasonic Scaling Insert (USI) operating at 25kHz or 30kHz. However, there are units that will accept both tips, such as the TurboSENSOR Ultrasonic Scaler (Parkell) and the ACCLEAN™ Ultrasonic Scaler (Henry Schein) (Figure 1).
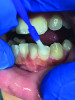
As a final step postdebridement, polishing serves to remove biofilm and stain, reduce surface roughness by smoothening the surface of the tooth, minimize the deposition of plaque, and appease the patient.2,17,18 This method is commonly accomplished by incorporating the use of a rubber cup and applying a paste to the tooth surface.2 It is prudent for dental healthcare providers to be aware of clinical and systemic contraindications for polishing and to consider essential selective polishing, which helps the clinician select polishing agents according to the individual patient's needs.19 Far too often, unethical polishing practices are performed, such as using one polishing grit for all polishing procedures.19 Having polishing agents with a variety of grits available to use in the office minimizes the chance of clinicians engaging in unethical polishing practices. A fine grit is suitable for younger patients and patients with minimal deposits. A medium grit is appropriate for most cleaning procedures where a high level of polish is desired, whereas a coarse grit is ideal for patients with heavy stain due to smoking or excessive intake of chromogenic beverages and foods. It is equally important to have different variations of rubber cups available to use in the office. Prophy cups are more commonly used. Firm cups should be used for heavy stain removal, while soft cups for light to moderate stain, and a tapered brush for removal of pit-and-fissure stain and for use around orthodontic appliances. Like ultrasonics, the armamentarium selected for a polishing procedure will vary depending on the phase of care and clinical scenario. The wide selection of prophy angles includes products such as 2pro® Disposable Prophy Angle (Premier Dental), ACCLEAN® Disposable Prophy Angles (Henry Schein), and Ultrapro Tx disposable prophy angles (Ultradent), while prophy pastes are available in different options to support individual patient needs, such as 3M™ Clinpro™ Prophy Paste (3M Oral Care), ProphyCare® (Directa Dental), and ACCLEAN® Prophy Paste (Henry Schein) (Figure 2 through Figure 4).
Treat and Protect
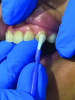
A thin fluoride-rich layer of enamel is compromised during debridement and polishing procedures. This layer can take upwards of 3 months to regenerate, leaving the tooth susceptible to daily sugar and acid attacks, which can result in a number of dental conditions such as caries and dentinal hypersensitivity. It is prudent for the clinician to treat and protect the compromised surfaces. As a preferred quick and easy in-office treatment, fluoride varnish is one of the most common dental products on the market to help protect vulnerable tooth surfaces until patients return for their next recare visit. Most varnish materials are comprised of a concentrated form of sodium fluoride (NaF) suspended in an alcohol- and resin-based solution with some additional additives, including a film-forming agent, flavors, sweetener such as xylitol (which has therapeutic benefits as well), and additives that aid in remineralization20,21 (Figure 5 through Figure 7). Examples include products such as Colgate® PreviDent® Varnish (Colgate Oral Health), FluoroDose® (Centrix), and ACCLEAN® 5% Sodium Fluoride Varnish (Henry Schein).
Once varnish is applied to the tooth surface, fluoride ions are attracted to the demineralized areas and integrate with hydroxyapatite to begin reforming the fluoride-rich enamel layer on the tooth surface.21 Most varnish products have a solubility profile that permits sustained release of fluoride over a specified period of time, offering teeth even greater protection over a longer duration.
Motivate Home Care
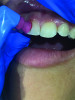
The patient plays a vital role in periodontal disease prevention and management. Therefore, the clinician must allot sufficient time to oral health education during each appointment to ensure that patients have the knowledge they need to function as an effective co-therapist for their oral healthcare needs. It can be difficult to keep patients motivated to perform their home care routines. However, patients who whiten their teeth have been found to be more compliant with treatment plans and regularly scheduled appointments. Approximately $1.4 billion is spent each year on over-the-counter whitening products, but patients should be getting whitening recommendations from their providers. Clinicians can help patients stay motivated to maintain their oral health by recommending the use of whitening strips embedded with hydrogen peroxide. Patients then get the benefit of a white smile and the therapeutic benefit from the antimicrobial effect as a result of the oxygenating action of the hydrogen peroxide. Recommended products are formulated with 10% hydrogen peroxide, which is one of the highest over-the-counter percentages available to consumers. The strips are also dissolvable within just 15 minutes, making them a desirable option for use as a patient motivator and adjunctive therapy (Figure 8 through Figure 10). Examples include LumiSmile® White Dissolving Strips (Oral ProCare) and ACCLEAN™ Professional Dissolvable Teeth Whitening Strips (Henry Schein), for example.
Conclusion
As the growing body of evidence continues to show the integral link between oral health and systemic health, patients should be informed of this association and motivated to improve their oral health. Oral health is compromised by several factors, namely microbial biofilm. Clinicians and patients need to work together as therapist and co-therapist to identify and remove clinical and microscopic etiology for periodontal disease prevention and management, and each phase of care- debride and polish, treat and protect, and home care-must be equally attended to in order to address all periodontal etiologic factors.
Ultrasonic scaling and the use of prophy paste with a rubber cup polisher are two in-office treatment strategies used to render the tooth surface free from microbial biofilm, calculus, and stain to stave off the host inflammatory response. Incorporating the use of various tips and power settings along with proper technique can increase scaling efficiency. Having access to various polishing grits and prophy angles will allow the clinician to treat the unique needs of each patient and avoid unethical polishing practices.
Fluoride varnish is a quick and efficient method to protect the tooth surface after it is compromised during debridement and polishing procedures. Clinicians must dedicate time and effort during oral health education so that patients are not only aware of the oral-systemic connection but are equipped with the knowledge to perform effective biofilm removal at home. Motivating patients to take part in the care of their oral cavity can be challenging. Incorporating the use of at home whitening strips can not only serve as a patient motivator to perform routine home care but can also serve as an adjunctive therapy for periodontal disease management. Understanding the importance of periodontal disease prevention and management, and the significance of each phase of care, products and tools have been developed for the clinician and patient to achieve optimal oral health.
About the Authors
Joy D. Void-Holmes, RDH, BSDH, DHSc
Dental Hygiene Program Chair
Fortis College
Landover, Maryland
Adjunct Faculty
American Denturist College
Eugene, Oregon
Founder and CEO
Dr. Joy RDH
Washington, DC
References
1. Donley T. Rethinking the goal of patient-driven and therapist-provided debridement. Compend Contin Educ Dent. 2020;41(5):290-291.
2. Mahiroglu MB, Kahramanoglu E, Ay M, et al. Comparison of root surface wear and roughness resulted from different ultrasonic scalers and polishing devices applied on human teeth: an in-vitro study. Healthcare (Basel). 2020;8(1):55.
3. Sawai MA, Bhardwaj A, Jafri Z, et al. Tooth polishing: the current status. J Indian Soc Periodontol. 2015;19(4):375-380.
4. Camboni S, Donnet M. Tooth surface comparison after air polishing and rubber cup: a scanning electron microscopy study. J Clin Dent. 2016;27(1):13-18.
5. Vicente A, Ortiz Ruiz AJ, González Paz BM, et al. Efficacy of fluoride varnishes for preventing enamel demineralization after interproximal enamel reduction. Qualitative and quantitative evaluation. PLoS One. 2017;12(4):e0176389.
6. Arifa MK, Ephraim R, Rajamani T. Recent advances in dental hard tissue remineralization: a review of literature. Int J Clin Pediatr Dent. 2019;12(2):139-144.
7. Shah R, Thomas R, Bhandari S, Mehta DS. Influence of various factors on patient compliance after periodontal therapy: a pilot study. J Indian Soc Periodontol. 2017;21(1):50-54.
8. Lee CT, Huang HY, Sun TC, Karimbux N. Impact of patient compliance on tooth loss during supportive periodontal therapy: a systematic review and meta-analysis. J Dent Res. 2015;94(6):777-786.
9. Oliveira Costa F, Miranda Cota LO, Pereira Lages EJ, et al. Progression of periodontitis in a sample of regular and irregular compliers under maintenance therapy: a 3-year follow-up study. J Periodontol. 2011;82(9):1279-1287.
10. Nakre PD, Harikiran AG. Effectiveness of oral health education programs: a systematic review. J Int Soc Prev Community Dent. 2013;3(2):103-115.