You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Orthodontic treatment prior to orthognathic surgical correction is aimed primarily at removing interferences.1-3 Before surgery, proper decompensation enables the optimum skeletal correction with the best facial and occlusal outcome and minimizes surgical instability.1 Orthodontic preparation helps reduce anesthesia time by allowing for a straightforward surgical procedure with fewer required surgical cuts, reducing overall morbidity during orthognathic surgery.
Orthodontic tooth movements in preparation for the surgical intervention are in the contrary direction to nonsurgical traditional orthodontics.1,3 Crucial to a successful result is clear communication between the orthodontist and oral and maxillofacial surgeon to establish common treatment goals.2 During treatment planning, careful consideration should be given to the patient's motivation for surgery, a psychological evaluation of the patient may be warranted, and a determination needs to be made as to whether or not the patient's expectations are reasonable.4 Taking a logical step-by-step sequential approach can facilitate success. Surgical procedures that yield the most stable long-term results are preferred. Lifelong retention and follow-up should be incorporated into the treatment team protocols.5
In borderline cases (ie, those that are difficult to determine whether orthognathic surgery is necessary), camouflaging the defect may be attempted first. In such cases, tooth movements should be carried out without the use of irreversible procedures such as extractions to avoid complicating any future surgery.3 A disadvantage of the use of camouflage or orthodontic compensation of the malocclusion as compared to surgical orthodontics is that the facial changes they provide are of a lesser magnitute.1-3 When treating dentofacial deformities, orthodontists should consider facially driven treatments instead of dentally driven ones.
Orthognathic Surgery and Obstructive Sleep Apnea Management
Airway function has received considerable attention of late, and surgical orthodontics could be utilized as part of treating patients with obstructive sleep apnea (OSA) or other sleep-disordered breathing problems. Orthognathic surgery can potentially increase upper airway dimensions (more specifically, the nasopharynx and oropharynx). Although there is no doubt that specific surgical movements, such as advancements, maxillary expansion, and maxilla down-fracture, are more likely to increase specific upper airway dimensions, such increases do not automatically imply an improvement in breathing function because of the complex nature of breathing and the inconsistencies of upper airway anatomy.6-8
Nevertheless, maxillomandibular advancement surgery is one of the available management options for a selected subset of OSA patients. Patients with underlying skeletal discrepancies and severe OSA who cannot tolerate positive airway pressure or oral appliance therapy may be candidates for this surgical approach. The severity of the disease and the comorbid obesity degree have had a significant impact on the success. One study reported that when body mass index (BMI) was >32 or apnea-hypopnea index (AHI) was >70, the success rate of surgery was around 60%, while when BMI was <32 or AHI was <70, the success rate reached 90%.6 Regardless, such a surgical approach may potentially result in unfavorable postsurgery facial esthetics in patients with a straight or convex profile.6-8
Specific Aspects of Presurgical Orthodontics
General Principles Vs Individual Requirements
A general principle applies for every surgical case: bond second molars to avoid interferences from hanging cusps.1-3 Another general principle for use in cases of significant transverse discrepancies between the maxilla and mandible (>5 mm) is to perform a surgical-assisted or temporary anchorage device (TAD)-assisted expansion first, then execute the vertical and sagittal surgical correction. This initial step allows for coordination of the arches in the transverse dimension prior to the surgical correction of the other skeletal problems. Alternatively, if the transverse discrepancy present is <5 mm, a two-piece Le Fort I procedure can be considered for simultaneous correction of all three dimensions, thus enabling only one surgical procedure.9-11
Conversely, individual requirements are more specific to each case. For example, leveling the upper arch in three segments in an anterior open bite that will require surgery and using .036-in wires in a .045-in tube during postsurgical care may be necessary.2,3
Leveling the Curve of Spee
One of the most important decisions is how and when to level the curve of Spee in surgical preparation.1-3 Is incisor intrusion or premolar extrusion going to be used to level it?2,3 While class II clockwise mandibular rotators (ie, patients who have an augmented lower facial height with a short mandibular ramus and presenting increased vertical patterns) require early leveling through lower incisor intrusion,1,3 class II brachyfacial patterns are better served by postsurgical premolar extrusion.2 In deep bite cases, if extractions are planned in presurgical orthodontics, good leveling mechanics are needed to avoid making the bite deeper. These cases require the use of a reverse curve of Spee incorporated into the archwires or auxiliary intrusion arches attached to a base arch.2 Most class III cases and asymmetries should have the curve of Spee also leveled before surgery.2,3
Overerupted maxillary or mandibular second molars and overerupted and undercorrected lower incisors are among the most common causes of instability due to a postsurgical occlusal fulcrum.2,3 Special considerations should be given to the first and last tooth in the lower arch to have a flat curve of Spee.2 Bracket repositioning before surgery is usually a prudent approach. This is generally done with the aid of presurgical mounted models, clinical photographs, and panoramic x-rays, all of which are used to ensure proper marginal ridge heights, the presence of no premature contacts, and adequate root parallelism.1,3,11
Staging Surgical Procedures in Severe 3-Dimensional Discrepancies
In cases with significant dentofacial deformities involving all three planes of space-transverse, vertical, and sagittal-presurgical orthodontics is modified to achieve a more stable long-term skeletal correction.9-11 The surgical procedure can be staged in these patients. Transverse discrepancies might be solved in the first stage through a surgically assisted rapid palatal expansion procedure.9-11 The third molars might be extracted during this first surgical procedure. After this, orthodontic decompensation is performed, and then the vertical and sagittal discrepancies might be corrected in a second surgical procedure. An advantage to this approach is that it allows healing from third molar removal for future osteotomies to restore the vertical and sagittal dimensions. The two procedures are usually done at least 8 months apart.9-11
For years it has been understood that transverse skeletal discrepancies should be measured through imaging and treated accordingly.12,13 Dental assessment (determining if there is a dental crossbite) is insufficient, and measuring the transverse skeletal discrepancy should be the standard of care.13
Use of Skeletal Anchorage in Presurgical Orthodontics
A major advantage of skeletal anchorage is the simplification of orthodontic movements.14,15 Limits in the transverse, vertical, and sagittal dimensions have been greatly expanded through the use of absolute anchorage, examples of which are shown in Figure 1 through Figure 7.14-16 Orthodontic decompensation can be done in a shorter amount of time with more predictable results with the support of skeletal anchorage.16-18 If the case allows it, surgical correction can be limited to one jaw, as absolute anchorage simplifies the surgical plan.13-16 Sometimes it is even possible to reduce the need for multiple-piece Le Fort osteotomies through better occlusal plane control.16-18
The clinician is faced with choices regarding the use of absolute anchorage. For example, miniscrews or miniplates are both sources of absolute skeletal anchorage. Miniplates, although they require a more invasive procedure for placement and removal, allow for better 3-dimensional control of specific tooth movements.19 All factors, including the extent of required correction, the possibility of an extra surgical procedure for miniplate placement, and the future orthognathic surgical plan, should be taken into account in the selection of absolute anchorage sources.
Patients With Special Periodontal or Prosthetic Considerations
Because many patients who require orthognathic surgery are adults, there are often either periodontal problems or prosthetic dentistry requirements to consider.20-22 Conditions commonly found are multiple missing or broken posterior and/or anterior teeth. This situation may require planning implant placement in the context of orthognathic surgery.22 Often a separate surgical procedure is planned for implant site preparation (eg, bone augmentation) and insertion, although sometimes all of the surgery can be done in one procedure, such as in cases of single implant placement as opposed to multiple implant placement with bone reconstruction.
Other common problems are tooth size discrepancies, such as peg-shaped lateral incisors, and/or missing anterior teeth (mostly maxillary lateral incisors or mandibular second premolars).21 These issues generally are addressed during presurgical orthodontics. Proper space is planned in advance for these situations if replacement is considered or if space closure is the procedure of choice, as this is generally done presurgically.3,21
Postsurgical Considerations
Assuming the case was properly set up in presurgical orthodontics and all surgical goals and objectives were accomplished, postsurgical care will consist of interdigitation and working up the sequence to finishing wires. Stability of the correction is dependent on proper respect given to the muscular balance, the temporomandibular joints (TMJs), and the periodontium.5,10,23-25
Range of motion exercises, implemented utilizing a physical therapist, should be started early in the postsurgical period, perhaps as early as within 2 days of orthognathic surgery, to aid the patient in gaining sufficient mouth opening. In the authors' practices the minimum acceptable mouth opening postsurgically is the equivalent of three fingers. As soon as possible and feasible the patient should be given a diet of adequate consistency (ie, soft solid food). Irrigation devices might be used by the patient in the early postoperative period to assist with oral hygiene.
Box elastics, either 5/16 medium or 1/4 heavy, are used against braided rectangular or .018-in round stainless-steel wires to allow cusp seating. The purpose of elastics is to achieve ideal intercuspation after surgery. A good cusp-to-fossae relationship is critical for postsurgical stability.2,3,5 Individual torques are usually refined as is final arch coordination. First and second order bends might be added to finishing wires to detail the case.
Retention of the Case and Long-term Follow-up
Surgical cases are typically retained using either a Hawley or a wraparound retainer in the maxillary arch (depending on whether the case is an extraction or non-extraction case) and a fixed bonded lingual retainer from cuspid to cuspid in the mandibular arch. Patients often prefer clear retainers, which are acceptable assuming they do not interfere with the occlusion.
Patients are seen 6 weeks after fixed appliance removal. Subsequent follow-ups are typically at the 12-week and 6-month intervals. After this, patients are called annually for a check-up. These appointments are intended to ensure that the mandibular cuspid-to-cuspid lingual retainer and the maxillary removable appliance are well fitting.
Further Considerations
In his classic books, Proffit et al stressed that treatment sequence is of the utmost importance.1,23 Simply put, who does what and when? Combining the benefits of orthodontic therapy and orthognathic surgery allows for a result that can greatly impact individual specialty care. Patient satisfaction and achieving esthetic and functional goals are the drivers in facially driven, rather than dentally driven, treatment planning in orthodontics.
If the patient has specific malocclusion characteristics, conventional surgical orthodontics can perhaps be modified for a "surgery first" or "early surgery" approach. This approach enables a shorter treatment time.15-17
Current technology and various computer planning programs available to the multidisciplinary team play a role in improved communication among professionals and in presenting treatment options to the patient. This allows patients to have comprehensive information vital for committing to treatment, including any additional costs, risks, and time required to recover from surgery as compared with conventional orthodontics.
As presented in the first part of this two-article series,26 the advent of virtual planning allows increased surgical precision to make orthognathic surgery as comfortable and pleasant to the patient as possible.27 The surgery has become more minimally invasive than in the past, and rigid fixation can be customized in many instances.28,29 These advances are shaping orthognathic surgery for the benefit of patients and allowing orthodontists to offer orthognathic surgery more frequently as such treatment becomes more patient-friendly.
The sequence in patients presenting active TMJ disorders varies. These patients should normally first receive an occlusal splint for pain management. The splint is also diagnostic in these situations, as it helps reveal the actual amount of skeletal discrepancy. Usually, the discrepancy in class II patients becomes more severe after the condyle is seated in its correct orthopedic position through splint usage. Treatment time in these situations is usually increased by about 6 months as the occlusal splint is worn before fixed appliances are placed for presurgical preparation.30-32 Ambulatory or one-night stay orthognathic surgery has permitted many patients to benefit from combined corrections.
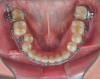
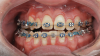
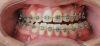
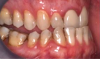
As previously mentioned, adult patients requiring orthognathic surgery often have esthetic dentistry and/or prosthodontic requirements. These are usually addressed after the surgical orthodontic correction has been completed and many times complemented through periodontal plastic surgery to improve the gingival architecture. A case report depicting this type of situation is presented in Figure 8 through Figure 20. In many instances the orthodontist is required to lead the interdisciplinary team and make appropriate coordinations with other dental specialties.1,11
Conclusions
Dentofacial deformities can affect many functions of a patient, including but not limited to airways. Bone position determines facial morphology, and functions such as breathing and feeding are affected by the 3-dimensional relationship of the upper and lower jaw relative to each other and to the craniofacial structures.
Respecting general surgical orthodontic principles is crucial to achieving pre- and postsurgical orthodontic goals. However, patient individuality prompts different situations in almost all cases. The orthodontist must have the flexibility to accommodate and satisfy all presurgical requirements to simplify the surgical procedure, as well as the skill to achieve good interdigitation and case detailing. In this sense, the orthodontist when moving teeth into the most ideal position is a facilitator for the surgical procedure.
The advent of skeletal anchorage has increased the envelope of possible orthodontic movements. This, in turn, has made surgery simpler and more efficient, often enabling fewer surgical cuts to be made to achieve the desired corrections.
About the Authors
Miguel Hirschhaut, DDS
Private Practice limited to Orthodontics, Caracas, Venezuela
Carlos Flores-Mir, DDS, DSc
Professor, Division of Orthodontics, Department of Dentistry, University of Alberta, Edmonton, Alberta, Canada; Part-time Private Practice limited to Orthodontics, Edmonton, Alberta, Canada
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Proffit WR, White RP Jr. Combining surgery and orthodontics: who does what, when? In: Proffit WR, White RP Jr., Sarver DM, eds. Contemporary Treatment of Dentofacial Deformity. St Louis, MO: Mosby; 2003:245-267.
2. Sabri R. Orthodontic objectives in orthognathic surgery: state of the art today. World J Orthod. 2006;7(2):177-191.
3. Larson BE. Orthodontic preparation for orthognathic surgery. Oral Maxillofac Surg Clin North Am. 2014;26(4):441-458.
4. Williams AC, Shah H, Sandy JR, Travess HC. Patients' motivations for treatment and their experiences of orthodontic preparation for orthognathic surgery. J Orthod. 2005;32(3):191-202.
5. Bailey LJ, Cevidanes LH, Proffit WR. Stability and predictability of orthognathic surgery. Am J Orthod Dentofacial Orthop. 2004;126(3):273-277.
6. Kent D, Stanley J, Aurora RN, et al. Referral of adults with obstructive sleep apnea for surgical consultation: an American Academy of Sleep Medicine systematic review, meta-analysis, and GRADE assessment. J Clin Sleep Med. 2021;17(12):2507-2531.
7. Zhou N, Ho JTF, Huang Z, et al. Maxillomandibular advancement versus multilevel surgery for treatment of obstructive sleep apnea: a systematic review and meta-analysis. Sleep Med Rev. 2021;57:1101471. doi: 10.1016/j.smrv.2021.101471.
8. Giralt-Hernando M, Valls-Ontañón A, Guijarro-Martínez R, et al. Impact of surgical maxillomandibular advancement upon pharyngeal airway volume and the apnoea-hypopnoea index in the treatment of obstructive sleep apnoea: systematic review and meta-analysis. BMJ Open Respir Res. 2019;6(1):e000402.
9. Betts NJ, Vanarsdall RL, Barber HD, et al. Diagnosis and treatment of transverse maxillary deficiency. Int J Adult Orthodon Orthognath Surg. 1995;10(2):75-96.
10. Vanarsdall RL Jr. Transverse dimension and long-term stability. Semin Orthod. 1999;5(3):171-180.
11. Vanarsdall RL Jr. Presurgical orthodontics for orthognathic surgery. Atlas Oral Maxillofac Surg Clin North Am. 2001;9(1):75-93.
12. Ricketts RM. Introducing Computerized Cephalometrics. Denver, CO: Rocky Mountain Data Systems; 1969.
13. Tamburrino RK, Boucher NS, Vanarsdall RL, Secchi AG. The transverse dimension: diagnosis and relevance to functional occlusion. RWISO J. 2010;2(1);13-21.
14. Costello BJ, Ruiz RL, Petrone J, Sohn J. Temporary skeletal anchorage devices for orthodontics. Oral Maxillofac Surg Clin North Am. 2010;22(1):91-105.
15. Yu HB, Mao LX, Wang XD, et al. The surgery-first approach in orthognathic surgery: a retrospective study of 50 cases. Int J Oral Maxillofac Surg. 2015;44(12):1463-1467.
16. Villegas C, Uribe F, Sugawara J, Nanda R. Expedited correction of significant dentofacial asymmetry using a "surgery first" approach. J Clin Orthod. 2010;44(2):97-103.
17. Hernández-Alfaro F, Guijarro-Martínez R, Peiró-Guijarro MA. Surgery first in orthognathic surgery: what have we learned? A comprehensive workflow based on 45 consecutive cases. J Oral Maxillofac Surg. 2014;72(2):376-390.
18. Farret MM. Occlusal plane canting: a treatment alternative using skeletal anchorage. Dental Press J Orthod. 2019;24(1):88-105.
19. Chen YJ, Chang HH, Lin HY, et al. Stability of miniplates and miniscrews used for orthodontic anchorage: experience with 492 temporary anchorage devices. Clin Oral Implants Res. 2008;19(11):1188-1196.
20. Halimi A, Zaoui F. Surgical-orthodontic treatment of patients suffering from severe periodontal disorders - a clinical case study. Int Orthod. 2013;11(3):314-332.
21. Sperry TP, Worms FW, Isaacson RJ, Speidel TM. Tooth-size discrepancy in mandibular prognathism. Am J Orthod. 1977;72(2):183-190.
22. Lopes JF, Pinto JH, Lopes MM, et al. Interrelationship between implant and orthognathic surgery for the rehabilitation of edentulous cleft palate patients: a case report. J Appl Oral Sci. 2015;23(2):224-229.
23. Proffit WR, White RP. The search for truth: diagnosis. In: Proffit WR, White RP, eds. Surgical-Orthodontic Treatment. St. Louis, MO: Mosby;1991:96-141.
24. Van Sickels JE, Richardson DA. Stability of orthognathic surgery: a review of rigid fixation. Br J Oral Maxillofac Surg. 1996;34(4):279-285.
25. Sarver D, Proffit WR, Ackerman L. Diagnosis and treatment planning in orthodontics. In: Graber TM, Vanarsdall RL,eds. Orthodontics: Current Principles and Techniques. 3rd ed. St Louis, MO: Mosby; 2000:3-115.
26. Hirschhaut M, Flores-Mir C. Guidelines for orthodontic evaluation and preparation for orthognathic surgery patients. Compend Contin Educ Dent. 2022;43(2):82-88.
27. Stokbro K, Aagaard E, Torkov P, et al. Virtual planning in orthognathic surgery. Int J Oral Maxillofac Surg. 2014;43(8):957-965.
28. AlAsseri N, Swennen, G. Minimally invasive orthognathic surgery: a systematic review. Int J Oral Maxillofac Surg. 2018;47(10):1299-1310.
29. Carneiro Júnior JT, de Moraes PH, de Oliveira DV, Carneiro NCM. Custom-made titanium miniplates associated with ultrahigh-molecular-weight polyethylene graft in orthognathic surgery: an adjunct to maxillary advancement. J Oral Maxillofac Surg. 2018:76(5):1091.e1-1091.e8.
30. Jung HD, Kim SY, Park HS, Jung YS. Orthognathic surgery and temporomandibular joint symptoms. Maxillofac Plast Reconstr Surg. 2015;37(1):14.
31. Al-Moraissi EA, Farea R, Qasem KA, et al. Effectiveness of occlusal splint therapy in the management of temporomandibular disorders: network meta-analysis of randomized controlled trials. Int J Oral Maxillofac Surg. 2020;49(8):1042-1056.
32. Okeson JP. General considerations in occlusal therapy. In: Okeson JP, ed. Management of Temporomandibular Disorders and Occlusion. 8th ed. St. Louis, MO: Elsevier; 2019:433-441.