You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
For many years, technological advancements in the laboratory were heavily focused on the fixed prosthetic market. Milling equipment and zirconia product advancements received most of the research and development money, but as this market became more competitive, the industry experienced a definite shift to the rather neglected removables arena.
Initial printable polymers were less than ideal. They were translucent and brittle, printing times were slow, and the products required arduous hand processing to complete.1 After an initial rough start, printed dentures finally became a more feasible solution in 2019.2
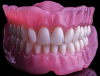
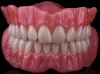
The release of Lucitone Digital Print (Dentsply Sirona) changed the direction of this polymer-based option (Figure 1). This material was initially processed exclusively on a Carbon® printing platform but has recently been validated for additional printing platforms. Today, other platforms have introduced their own material options, including Flexcera™ Smile (Desktop Health) for EnvisionTEC printers (Figure 2) and Trusana (Zahn Dental) for SprintRay and Asiga printers.
These new-world materials show exceptional monolithic denture base color and exhibit almost three times the strength of traditional hand-processed, high-impact acrylics.3 One of the greatest improvements over first-generation polymer materials is that current materials require very limited hand processing.
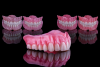
These materials facilitate many clinical and technical workflow upgrades, especially in design software options (Figure 3).4The advancements not only save today's dental laboratory technician from having to implement many arduous hand-processing techniques, but they also allow the clinician to restore a new denture in as few as two clinical appointments.
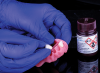
Another often overlooked advantage of digital dentistry is that digital design allows for an archivable record of the delivered prosthesis. This archived smile has the potential to greatly reduce the number of post-delivery appointments required to fabricate a replacement or new denture. Furthermore, once a patient's approved smile is archived, the clinical process of fabricating future dentures is greatly simplified and reduced to as few as two appointments. In case of a lost or broken denture, the clinician can now offer the patient a new, exact copy of the original without the need for any pre-delivery clinical appointments (Figure 4). The ability to order a new replacement denture by phone, without the need for any record taking such as impressions and bites, gives today's clinicians the ability to provide a patient with a new prosthesis in as little as 24 hours (Figure 5).
Despite these advantages, adoption rates have been slow for printed denture technology. This article will identify some myths that may discourage adoption and explain the corresponding truths.
Material Strength
Myth: Printed denture materials are not strong enough.
The biggest concern voiced by critics relates to the printable base material strength. Many technicians still believe hand processing a traditional high-impact acrylic yields higher material strength when compared to a printable polymer. At the author's laboratory, this is also still the most voiced concern from first-time clinical users.
Leading printable polymers are reported to have higher flexural strength, flexural modulus, and work of fracture at room temperature when compared to traditional denture base materials.5
The true advantage is seen once the material reaches body temperature. At a working temperature of 37°C, work of fracture resistance can double in a printed denture from 1,500 J/m² to more than 3,000 J/m², with some materials documented to reach as high as 3,667 J/m². This material class will likely see even more improvements as development progresses.
Tooth-to-Base Bonding
Myth: Teeth will de-bond from the printed base.
Some question whether the strength of the base is even relevant if the tooth de-bonds from the base prematurely (Figure 6). This argument is often used to question the validity of a printable denture material.
However, a fusing technique can be used to permanently link the tooth structure to the denture base. This fusing process utilizes the polymer's glass transition (Tg) property to facilitate fusing between the two materials. This "above glass transition" occurs when an amorphous material is either heated or cooled in a particular temperature range.6 As the material cools, it loses its flexibility and becomes brittle (hence the term "glass"); as it is heated, it becomes softer. This is what makes the glass transition important to thermoplastic polymers; above the glass transition region, a thermoplastic can be molded without breaking.
This is one of the key properties that makes thermoplastics so useful in the dental industry, and in this case, it is used to create a true fusing between the two structures.
Limited Patient Application
Myth: Digital dentures cannot be prescribed for all patients.
With the initial release of printed polymer materials, carded teeth were the only restorative tooth option available. This limited their use to only patients with adequate restorative clearance. Because printing is an additive process, carded teeth are fused into a predesigned receptacle area that pairs with the intaglio surface of the stock carded tooth. This means that carded teeth can only be used in their unaltered state in additive fabrication; if any adjustment to the vertical height of the tooth structure is required, additive technology cannot be utilized in conjunction with the carded teeth.
However, competition is often the biggest product development driver, and the evolution of printable polymers is no exception. Newer materials have been designed to allow for a printed base and customized, printed tooth structure (Figure 7).
Printing the tooth structure offers significant technical advantages over using carded teeth, but questions arose regarding wear rates and longevity. Multiple studies have shown amazing wear rate results, especially when compared to well known and trusted denture tooth brands. According to one study, "The mean vertical depth of wear for the 3D printed denture teeth (0.016 ± 0.010 mm) was statistically significantly less than the prefabricated denture teeth."7 Having access to a functional printable material allows the modern-day restorative team to produce a denture with a monolithic, interproximally connected tooth structure. This product produces a strong, lightweight, and very esthetic solution for patients with bruxism who experience high wear in their traditionally fabricated dentures.
Limiting Clinical Workflows
Myth: Traditional clinical record taking cannot be used.
Digital denture protocols have created a world where a new denture can be restored predictably in two or three clinical appointments. This is done by using the patient's existing (old) denture as a custom tray and prototype starting point for a digital diagnostic wax-up. Although this updated clinical workflow has proven to be an absolute game changer for many clinicians who are tired of dealing with a traditional bite rim to set a sometimes-elusive vertical dimension of occlusion, many clinicians still choose to control the data gathering process with a more traditional workflow-and many of these clinicians have been told their preferred proven workflows cannot be used when restoring a digital denture.
Fortunately, most of the manufacturing upgrades are found in the fabrication and design processes; this means a digital denture can be restored just as effectively with a traditional or upgraded digital restorative workflow. The digital denture design software allows the design technician to import either an existing denture STL scan or a traditional bite rim (Figure 8) with documented landmarks as the starting point.
Accuracy and Longevity
Myth: Printed dentures are not as accurate as hand processed.
Many technicians and clinicians still believe that traditional hand processing techniques produce a better fitting and more accurate final prosthesis.
The author's laboratory initially switched from analog to digital denture processing in late 2019 and started implementing newer materials in mid-2021. Over a 26-month period, more than 2,250 digitally processed dentures were successfully delivered (Figure 9 and Figure 10). Post-delivery issues such as tooth shifting and bite changes caused by processing errors were completely eradicated.
The accuracy of digitally processed dentures was also compared with that of a hand-processed version in a study by Tasaka et al, which found that, on maxillary dentures, the amount of tooth displacement for the heat-cured dentures and for the 3D printed dentures ranged from -0.08 mm to +0.06 mm and from -0.25 mm to +0.06 mm, respectively.8 The discrepancies found on maxillary dentures were statistically negligible on mandibular dentures.8
A delivery success rate (patient acceptance/comfort) when using a digitally designed prototype try-in workflow was documented at 98% in the author's laboratory. Similar results were found in a retrospective comparison of 637 dentures reported by Kim et al in January 2021.9
Perhaps the most impressive documented statistic from the author's laboratory involves the negligible post-delivery material issues experienced with some of these new materials. Over a 6- to 26-month period, tooth-to-base debonding was reported on only three dentures, and base fractures were only reported (returned for remake) on 23 of the 2,250 delivered dentures.
As expected, carded tooth fracture rates were comparable with traditional dentures. At the time of this publication, even though no post-delivery issues were reported, the author considers it too early to accurately judge the functionality of printed tooth structures.
Conclusion
Even though the esthetics and functionality of first-generation digital denture materials hindered adoption rates, the clinical workflow advantages have proven extremely efficient for the modern-day clinician and patient. Now, printable polymer materials have finally caught up, and these products are proving their value in the removable arena.
With a rapidly aging removable technician demographic and labor shortages becoming major concerns for dental laboratory owners, the industry needed an updated protocol for survival. Even though the adoption of this groundbreaking product has been slower than expected, the combination of a very efficient clinical workflow, highly esthetic/stronger materials, and streamlined processing will ultimately be the driving force behind mass implementation.
Acknowledgements
The author would like to acknowledge the exceptional efforts of Chris Love, Kate Johnson, and Steve Lombardi of the Absolute Dental Acrylics team. Together, they implemented new digital protocols and established clinical adoption through guidance and education.
About the Author
Conrad J. Rensburg, ND, NHD
CEO and Head of Implant Division
Absolute Dental Services
Durham, North Carolina
References
1. Gad MM, Fouda SM, Abualsaud R, et al. Strength and surface properties of a 3d‐printed denture base polymer. J Prosthodont. August 2021. doi:10.1111/jopr.13413
2. Wagner SA, Kreyer R. Digitally fabricated removable complete denture clinical workflows using additive manufacturing techniques. J Prosthodont. 2021;30(S2):133-138. doi:10.1111/jopr.13318
3. Baba NZ, Goodacre BJ, Goodacre CJ, Müller F, Wagner S. CAD/CAM complete denture systems and physical properties: A review of the literature. J Prosthodont. 2021;30(S2):113-124. doi:10.1111/jopr.13243
4. Clark WA, Duqum I, Kowalski BJ. The digitally replicated denture technique: A case report. J Esthet Restor Dent. 2019;31(1):20-25. doi:10.1111/jerd.12447
5. Sun B, Ammon D, Ghergulescu C, Young A, Kelkar S, Mota E. Development of a high impact DLP 3D printing denture resin. lecture presented at the: IADR/AADR/CADR General Session; 2020.
6. Ibrahim M, Zheng F. The effect of glass transition on the bond strength at the interface between denture teeth and denture base. Dent Oral Biol Craniofacial Res. 2018;1(3):2-4. doi:10.31487/j.dobcr.2018.03.001
7. Pham DM, Gonzalez MD, Ontiveros JC, Kasper FK, Frey GN, Belles DM. Wear resistance of 3D printed and prefabricated denture teeth opposing zirconia. J Prosthodont. 2021;30(9):804-810. doi:10.1111/jopr.13339
8. Tasaka A, Okano H, Odaka K, et al. Comparison of artificial tooth position in dentures fabricated by heat curing and additive manufacturing. Aust Dent J. 2021;66(2):182-187. doi:10.1111/adj.12817
9. Kim TH, Huh JB, Lee J, Bae EB, Park CJ. Retrospective comparison of postinsertion maintenances between conventional and 3D printed complete dentures fabricated in a predoctoral clinic. J Prosthodont. 2021;30(S2):158-162. doi:10.1111/jopr.13322