You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
As dentistry evolves, digital technology is becoming increasingly prevalent. Digital technologies have been embedded in dental implant workflows for many years. These workflows range from simple to more complex, allowing many treatments to be performed digitally. Digital technology can enable clinicians to effect more efficient workflows, attain more accurate results, and even explore new treatment avenues.
Some implant treatments require the utilization of a hybrid workflow in which conventional and digital procedures are both used due to digital limitations. It is important to remember that conventional workflows have served dentistry well for many decades, and they can benefit clinicians when used in conjunction with digital technologies. By employing a hybrid workflow, clinicians can use the "best of both worlds," so to speak. As such, clinicians should understand when to use a fully digital workflow versus a hybrid one.
General Considerations
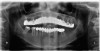
In a digital workflow, implant planning begins with the collection of basic data sets, including a digital imaging and communications in medicine (DICOM) file generated by a cone-beam computed tomography (CBCT) scan. CBCT use has become progressively commonplace as its availability increases and cost lowers, and because of its relatively low-dose radiation. In complex patient cases or challenging single-tooth implant cases, CBCT-based treatment planning has become a standard approach. Three-dimensional (3D) images can be obtained in any plane by reconstruction of the DICOM data. Abboud et al compared CBCT and CT on uniform objects and found reliable measurements for both imaging modalities.1 They noted that although there were differences between CT and CBCT in the distance measurements of the hard tissue of the human mandible, these differences were not clinically significant for most diagnostic purposes. With 3D radiography data all anatomic landmarks and tooth structures are able to be evaluated. CBCT detects bone volume present, bone deficiencies, furcations, crestal bone loss, fenestrations, and dehiscences.2
An intraoral optical scan (IOS) or an optically scanned model or impression can be utilized to accurately capture the tooth and soft-tissue anatomy.3 Most IOSs now function without the use of powder, and they create accurate prosthodontic data sets when used to scan single teeth or quadrants of teeth.4 Studies examining IOSs used for full-arch intraoral scans have yielded conflicting results. Keul and Güth showed that an IOS is a valid alternative to conventional impressions for complete arches.5 On the other hand, Ender et al presented data demonstrating that it was challenging to make complete-arch digital impressions using IOSs.6 They, however, showed that certain IOS devices were well within the required range for clinical quality. Conventional impressions, model casting, and optional digitization of the impression or cast with desktop optical scanners remain a safe workflow process for complete-arch patient cases. The data set created from an IOS is a standard triangulation language (STL) file.
Superimposition and matching of the DICOM and STL data sets allows visualization of the relationship between bone, teeth, and soft tissues with accurate anatomic representation. This is the ideal starting point for planning implant types, sizes, and positions virtually. Additionally, the face and/or smile of a patient can be captured and matched with existing data files. An STL file can be generated by specific devices, such as a scanner that provides photorealistic 3D digitization of patients' faces; alternatively, technologies have been developed that incorporate cameras into a CBCT scanner. The generation of a photorealistic 3D digitalized face aids in the creation and design of a highly esthetic restoration.
Based on the restorative design and the implant placement planning, "static" surgical guides can be fabricated for surgery. When indicated, prosthetic components, such as custom abutments and temporary crowns, can be manufactured prior to surgery. Static guides refer to the fabrication of tooth-, bone-, or mucosa-supported surgical templates. The virtual implant position(s) planned from the CBCT, IOS, and face-in data sets is reproduced in the guide. Implant-specific instrumentation is necessary to create osteotomies and guide the implants accurately in 3D. The guides can be printed, milled, or stereolithographically fabricated in an office or dental laboratory, or by a manufacturer.
Immediate loading procedures with provisional restorations allow patients to leave the dental/surgical office with esthetics and function. Research of immediately loaded implants has shown that the marginal bone level can be preserved from the time of implant placement. A provisional restoration with an ideal crown form can facilitate the formation of natural peri-implant mucosal contours.7 The results of finite element experiments also indicate that immediate loading of implants is a safe procedure, even for single-tooth implants, assuming correct loading criteria and control of loading forces are maintained.8
After implant insertion, a temporary crown can be produced in a chairside workflow. Numerous chairside solutions are available in the US market. They all allow the user to fabricate same-day crowns, inlays, onlays, bridges, and veneers. The restoration design and fabrication can be accomplished quickly and conveniently, although a learning curve is involved.
Based on all of these considerations, this article presents several different implant treatment scenarios and discusses whether a fully digital workflow is possible and/or beneficial for the clinician and patient in each situation. Each scenario includes the full-treatment sequence for immediately loaded implants. The authors acknowledge that immediate loading is not always the treatment of choice. However, from a descriptive standpoint, this presentation allows a direct comparison of different restorative and surgical implant workflows.
Immediately Loaded Single Implant Using Chairside CAD/CAM Systems
In this scenario the clinician uses an IOS to register the implant position by scanning an implant scanbody that is screwed into the implant. A second scan, of the opposing teeth, is then made, followed by a third scan of the patient's occlusal relationship. Computer-aided design/computer-aided manufacturing (CAD/CAM) software is then used to superimpose the three scans. The combined scans can then be sent to a dental laboratory, or the provider can design the patient case using the navigation and graphic tools embedded in the software. For single-tooth crowns or three-unit bridge restorations, most software programs are able to automatically position selected tooth templates to match the central grooves, cusp heights, and marginal ridges of the proximal dentition. This decreases chairside design time.
Once the design is completed, the software selects the location of the sprue, which the clinician can alter as needed. The clinician may also design the abutments for implant restorations and bridges, but some chairside systems presently do not offer in-office milling.
To mill a digitally designed restoration, the file is then sent to a milling machine. If an immediate restoration is being fabricated, blocks of various materials, such as polymethyl methacrylate (PMMA) or ultrafine zirconia-silica ceramic particles that reinforce a highly cross-linked polymeric matrix, are available for milling. If the definitive restoration is being fabricated, the clinician can choose from feldspar/glass ceramics, high-strength glass ceramics, hybrid ceramic, zirconium oxide, aluminum oxide, infiltration ceramics, polymers, and nonprecious metals. Different sized blocks are available for chairside milling of individual restorations or fixed partial dentures. Feldspathic or zirconia materials are available in multilayered blocks that allow for a very natural-looking appearance with a high degree of chroma in the cervical portion and good translucency in the incisal portion. Milling times for a crown are between 10 to 18 minutes depending on the CAM unit, crown design, and material used.9 After the milling is completed and the restoration is tried intraorally, final adjustments may be made as necessary. Some materials, like a lithium disilicate glass-ceramic for CAD, require crystallization, with or without glazing, while others, such as a fully crystallized glass-ceramic, require only polishing. To individualize restorations, surface stains are available for various materials. Numerous cements come in different shades and translucencies and vary from luting to adhesive cements.
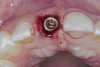
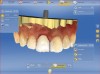
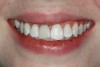
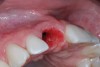
The workflow in this scenario can be executed fully digitally. It is predictable and efficient for the planning and fabricating of single crowns or small bridge units. The block size for many milling machines ends at 20 mm; larger, more expensive units may accommodate up to 40 mm. The clinician must determine how best to utilize time in this workflow. Often, a dental technician or skilled team member may be used in many aspects of the workflow. For in-office milling, sufficient time must be allotted in both the patient's and the practice's schedules to allow for fabrication, preparation, and delivery of the restoration. In the authors' experience, it typically takes 90 to 120 minutes to deliver an in-office milled crown and 70 to 90 minutes for an inlay or onlay. The advantage is that the treatment can be finished in one visit. An example of a patient case is shown in Figure 1 through Figure 6.
Immediately Loaded Implants Using Prefabricated Temporary Restorations, Multiple Units
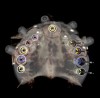
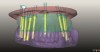
The multiple-unit workflow is similar to the scenario above except that the manufacturing of the temporary restoration is made prior to surgery. The most predictable method to execute this scenario is with CT guided surgery. Surgical guides are used to place implants into their virtually planned position(s) using a minimally invasive surgical technique. Flapless insertion of implants is possible, minimizing potential complications arising from soft-tissue elevation such as infection, dehiscence, and soft- and hard-tissue necrosis.10,11 Additionally, the use of guided surgery reduces the potential for injury to underlying anatomical structures during the implant osteotomy preparation and implant placement.12 It is important to use bite registrations to properly position surgical guides fabricated from guided surgical planning, as bite registrations hold the surgical guide in its correct planned position for stabilization with screws or pins. This is most important when the patient case involves multiple extractions or a mucosa-supported surgical guide. Surgical guide stabilization pins or screws should be used in all completely edentulous patient cases and most partially edentulous patient cases. Manufacturer-recommended implant-specific instrumentation and drilling protocols should be followed.
Implants should be placed through the surgical guide, to final depth and angulation, attached to appropriate guided surgery implant mounts. Computerized implant planning on 3D tomographic data (CT or CBCT), followed by image guided surgery, improves the accuracy of prosthodontic-driven implant positioning.13-15 Guided surgery with drill guides has been reported to increase implant placement precision and improve the transfer of 3D implant planning to patients.16,17 Drill guides are known to increase safety in dental implant placement compared to freehand techniques18 while being compatible with all aspects of implant surgery, including flapless methods.
Nevertheless, potential errors, which are additive, can be made in each step in the CT guided surgery workflow. In the authors' experience, consistent success with CT guided surgery requires an understanding of the rationale for all steps in the workflow, attention to detail, meticulous adherence to established recommended protocols, and a concerted effort to carry out all of the steps in the workflow and not omit any.
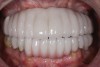
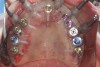
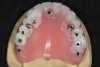
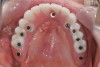
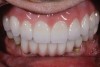
Obviously, a prefabricated restoration on multiple units made prior to surgery will fit imperfectly on implant abutments and require chairside adjustments and relining. Therefore, a fully digital workflow in this scenario is unrealistic. Practically every prefabricated temporary restoration needs to be relined and adjusted chairside to provide good fit and margin adaptation. A hybrid treatment that combines digital and conventional techniques will deliver the most consistent results. An example of a patient case is presented in Figure 7 through Figure 16.
Immediately Loaded Implants Using a Prefabricated Denture in an Edentulous Patient
The stabilization of existing dentures with dental implants is a common procedure. The creation of a well-fitting denture for edentulous patients is challenging using fully digital procedures because of soft-tissue resilience and movement. While intraoral scanners are excellent at scanning hard tissue, movement of vestibular tissues is difficult to capture with an IOS device. An IOS is a static impression. The dynamic changes of moveable and compressible mucosa cannot be captured.
In this scenario, the use of a traditional preliminary alginate or definitive impression is the better and more accurate choice. The fit and comfort of a denture is determined by how well the available space within the oral cavity is captured. Currently, border molding movements are utilized to best capture this restorative space. In many of the digital denture workflows, conventional impressions are digitized. Using scannable alginate or definitive impression material for the initial records gives the clinician the ability to scan the impression. This saves time and eliminates the potential for error introduced from scanning a stone cast. Before the final denture is delivered, a printed or milled denture try-in should be scheduled to evaluate for any necessary adjustments. This step cannot be executed fully digitally.
A simple and highly accurate technique for denture relining over dental implants is done chairside. Time and skill are the only requirements; increased skill will decrease the time required, and a proficient clinician can effectively complete a denture reline rapidly and easily, provided the proper material is selected. Current chairside reline materials have demonstrated properties that rival laboratory-processed relines.19 With a simple procedure, the entire denture relining process can be completed in one appointment. Using the direct hard relining concept, the denture is relined chairside with cold-curing acrylic resin material.19 Undercuts in the sulcular areas should be blocked out and plastic rings placed around the abutments. The temporary prosthesis is hollowed out chairside in the area of the implants, and the surgical field is covered with a rubber dam to protect the soft tissues during the restorative phase of treatment. The copings placed on the implants are "picked up" and the temporary fixed detachable prosthesis is modified and polished afterwards.
Similar to the second scenario above, a prefabricated denture cannot be adapted chairside to dental implants without the use of conventional restorative workflows. For the treatment of fully edentulous patients, a fully digital workflow is not predictably possible at this time.
Conclusion
Digital implant workflows are opening new and more accurate ways of implant treatment planning when compared to older analog techniques. The placement of implants using guided surgery (static or dynamic) follows this digital trend and presents multiple benefits for immediately restoring a patient functionally and esthetically with a provisional restoration. Small restorations can be produced chairside in a fully digital workflow. When patient cases exceed a quadrant or involve a complete-arch restoration, the fabrication and insertion of temporary restorations becomes the limiting factor in any attempt to utilize a fully digital workflow. In these cases, a hybrid workflow combining traditional and digital techniques is presently the optimal choice.
About the Authors
Marcus Abboud, DMD, PhD
Adjunct Professor, College of Engineering and Applied Sciences, Stony Brook University, Stony Brook, New York
Sinead McEnhill, BDS, MSc
Clinical Director of Private Practice specializing in Dental Implants and Facial Esthetics, Enniskillen, County Fermanagh, Northern Ireland; Fellow, International College of Dentists
Gary Orentlicher, DMD
Section Chief, Oral and Maxillofacial Surgery, White Plains Hospital, White Plains, New York; Private Practice specializing in Oral, Maxillofacial, and Implant Surgery, Scarsdale, New York
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Abboud M, Calvo-Guirado JL, Orentlicher G, Wahl G. Comparison of the accuracy of cone beam computed tomography and medical computed tomography: implications for clinical diagnostics with guided surgery. Int J Oral Maxillofac Implants. 2013;28(2):536-542.
2. Shukla S, Chug A, Afrashtehfar KI. Role of cone beam computed tomography in diagnosis and treatment planning in dentistry: an update. J Int Soc Prev Community Dent. 2017;7(suppl 3):S125-S136.
3. Michelinakis G, Apostolakis D, Pavlakis E, et al. Accuracy of IOS in full-arch dentate patients compared to CBCT cast-scanning. An in-vivo study. Eur J Prosthodont Restor Dent. 2019;27(3):122-130.
4. Wesemann C, Muallah J, Mah J, Bumann A. Accuracy and efficiency of full-arch digitalization and 3D printing: a comparison between desktop model scanners, an intraoral scanner, a CBCT model scan, and stereolithographic 3D printing. Quintessence Int. 2017;48(1):41-50.
5. Keul C, Güth JF. Accuracy of full-arch digital impressions: an in vitro and in vivo comparison. Clin Oral Investig. 2020;24(2):735-745.
6. Ender A, Zimmermann M, Mehl A. Accuracy of complete- and partial-arch impressions of actual intraoral scanning systems in vitro. Int J Comput Dent. 2019;22(1):11-19.
7. Abboud M, Koeck B, Stark H, et al. Immediate loading of single-tooth implants in the posterior region. Int J Oral Maxillofac Implants. 2005;20
(1):61-68.
8. Abboud MF. Immediately loaded implants-clinical and biomechanical analysis. J Oral Maxillofac Surg. 2009;67(9 suppl):57-58.
9. Zaruba M, Mehl A. Chairside systems: a current review. Int J Comput Dent. 2017;20(2):123-149.
10. Arisan V, N. Bölükbaşı N, Öksüz L. Computer-assisted flapless implant placement reduces the incidence of surgery-related bacteremia. Clin Oral Investig. 2013;17(9):1985-1993.
11. Arisan V, Karabuda CZ, Ozdemir T. Implant surgery using bone- and mucosa-supported stereolithographic guides in totally edentulous jaws: surgical and post-operative outcomes of computer-aided vs. standard techniques. Clin Oral Implants Res. 2010;21(9):980-988.
12. Orentlicher G, Abboud M. Guided surgery for implant therapy. Dent Clin North Am. 2011;55(4):715-744.
13. Vrielinck L, Politis C, Schepers S, et al. Image-based planning and clinical validation of zygoma and pterygoid implant placement in patients with severe bone atrophy using customized drill guides. Preliminary results from a prospective clinical follow-up study. Int J Oral Maxillofac Surg. 2003;32(1):7-14.
14. Van Assche N, Vercruyssen M, Coucke W, et al. Accuracy of computer-aided implant placement. Clin Oral Implants Res. 2012;23(suppl 6):112-123.
15. Rosenfeld AL, Mandelaris GA, Tardieu PB. Prosthetically directed implant placement using computer software to ensure precise placement and predictable prosthetic outcomes. Part 3: stereolithographic drilling guides that do not require bone exposure and the immediate delivery of teeth. Int J Periodontics Restorative Dent. 2006;26(5):493-499.
16. Cassetta M, Stefanelli LV, Giansanti M, Calasso S. Accuracy of implant placement with a stereolithographic surgical template. Int J Oral Maxillofac Implants. 2012;27(3):655-663.
17. Abduo J, Lau D. Accuracy of static computer-assisted implant placement in anterior and posterior sites by clinicians new to implant dentistry: in vitro comparison of fully guided, pilot-guided, and freehand protocols. Int J Implant Dent. 2020;6(1):10.
18. Alevizakos V, Mitov G, Stoetzer, von See C. A retrospective study of the accuracy of template-guided versus freehand implant placement: a nonradiologic method. Oral Surg Oral Med Oral Pathol Oral Radiol. 2019;
128(3):220-226.
19. Tewary S, Pawashe KG. Evaluation of linear dimensional accuracy of hard chairside and laboratory heat cure reline resins at different time intervals after processing. Indian J Dent Res. 2014;25(6):686-691.