You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
When using digital technologies in restorative dentistry, clinicians must have a comprehensive understanding of traditional esthetic principles in order to attain successful results, especially when treating challenging esthetic cases. Even the use of contemporary digital tools requires a solid knowledge of basic tooth shape and form rules that have been discovered, honed, and documented over many years.1-4 There are a number of classical esthetic principles that clinicians need to follow beginning with a smile analysis, which encompasses all parameters of shape and form. These parameters include the midline, maxillary incisal length, tooth dimensions, variation of incisor tooth forms, illusions with tooth dimensions, surface texture, and transitional angles. This article will review these parameters and demonstrate their implementation in a challenging esthetic case.
Parameters of Tooth Shape and Form
Midline-The dental midline is an imaginary vertical line that runs from the nasion through the subnasal and interincisal points to the pogonion.5 Ideally, the papillae between the maxillary central incisors coincides with the midline of the face; however, research has shown that the maxillary midline coincides with the facial midline only 70% of the time, and slight deviations in the dental midline do not necessarily compromise esthetics.6
Maxillary incisal length-The average length of a central incisor is 10 mm to 11 mm.7 However, the patient's desired incisal length often differs from this average; therefore, patient input is critical when determining the final incisal edge location.
Tooth dimensions-In an esthetic smile, the central incisors are dominant in shape, size, and position, with an ideal width-to-length ratio of 75% to 80%.8 The lateral incisor width is approximately 60% the width of the adjacent central incisor. The canines represent the junction between the posterior and anterior segments of the dentition. Typically, only the mesial half of the canine is visualized from a frontal perspective. The distal half may be in line with the buccal surface of the maxillary posterior dentition. No standard measurements define tooth dimensions; however, the golden rule of proportion states that the ratios between the width of the maxillary anterior teeth should be 1.618 for a central incisor, 1 for a lateral incisor, and 0.618 for a canine. The term "golden proportion" is a mathematical theorem concerning the proportions of the dentition; it dictates only the width of the teeth.9,10 Thus, when viewed from the front, and looking anterior to posterior, each anterior tooth is approximately 60% of the size of the preceding adjacent tooth.
These principles are crucial for clinicians to understand. Strict application of these rules, however, may be too limiting, and the clinician must determine the appropriate sizes of the teeth in each individual patient taking into consideration the unique arch form, lip dynamics, and facial proportions.11
The theory of continuous proportion states that the same ratio of tooth widths established between the central and lateral incisors (not limited to 60% as in the golden proportion rule) can be used moving distally when designing the smile. The recurring esthetic dental proportion concept ratio allows the dentist to choose a proportion that best fits the patient. A constant, consistent proportion will be pleasing to the eye as one's gaze moves distally in the dentition.12
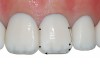
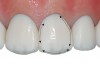
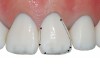
Variation of incisor tooth forms-There are three predominant incisor tooth forms: square, ovoid, and triangular.13 In a square type of tooth the mesial and distal outline forms are straight and parallel and present with a wide cervical volume. The incisal edge is straight or slightly curved (Figure 1). In an ovoid tooth form both mesial and distal outline forms are curved and present with a narrow cervical volume. The incisal edge is relatively narrow and occasionally rounded. The transition outline is smooth, with no lobes showing incisal and cervical convergence (Figure 2). In a triangular tooth form the distal outline is not parallel to the mesial outline but clearly inclined, defining a narrow cervical area with a wide incisal edge that is slightly curved. The tooth shows a straight outline with marked transition line angles. The lobes display the distal inclination of the distal outline (Figure 3).
Lateral incisors are half oval in shape and present with the gingival zenith centered with the long axis of the tooth. They differ from central incisors in that they are smaller in size and have more rounded mesioincisal line angles.14 They may present with a slight depression of the distal line angle at the cervical contour. Lateral incisors have the greatest variation in form among the anterior teeth and provide the personality of a smile.15 In an esthetic smile design, lateral incisors tend to not match each other identically.
The canines are elliptical in shape and present thicker labiolingually. The canine gingival zenith is positioned distal to the long axis of the tooth. The mesial outline is convex resembling the lateral incisor while the distal outline is flat or concave and resembles the premolar.
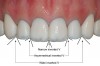
Illusions with tooth dimensions-Teeth can be made to appear narrower or wider using a variety of techniques. If the distal aspect of the tooth is lingualized, the tooth will appear narrower when viewed from the facial. Interincisal angles are illustrated in Figure 4. Mesioincisal and distoincisal angles define the negative dark space behind the teeth that is present when patients open their mouth or separate their teeth. These angles may be manipulated to create desired illusions of tooth width. Rounding the incisal corners opens the interincisal embrasure, thereby creating more negative dark space and giving the tooth a narrower appearance. Closing the incisal embrasure produces the illusion of a wider tooth when viewed from the front, with the mouth opened as when the patient is laughing.
Surface texture-Surface texture is the amount of graininess or roughness present on the tooth. As the roughness increases, more light is reflected and the tooth may appear brighter. The direction of the texture lines can create the illusion of long, thin teeth or short, wide teeth.13 Parallel horizontal lines, called lines of Retzius or perikymata, make a tooth appear wider and shorter. Vertical lines and grooves that segment the developmental lobes cause a tooth to appear thinner and longer.
Transitional angles-Incisor shape is related to the anatomy of the interproximal ridges, which are also called transitional line edges.13 These lines are slightly curved and vertically oriented, and represent the intersection of the facial surface and the reflective surface emerging from interproximal contact.14 Line angles can be placed strategically to change how light reflects off the tooth. The teeth will appear longer if the mesiofacial and distofacial line angles are moved toward the center of the tooth. If the line angles are placed with a wider trajectory, the tooth will be perceived as shorter and wider.
When viewing the tooth from an incisal perspective, if the facial contour between these transitional line angles is concave, the tooth will appear thinner. If the facial contour between these transitional line angles is convex, the tooth will appear wider (Figure 5).
Case Presentation
This case illustrates the diagnosis, planning, and clinical execution used to mask a congenitally missing lateral incisor while preserving the natural dentition on the contralateral side. Using the principles of both symmetry (creating a mirror image around the midline) and harmony (creating a recurring theme from left to right), the goal was to create a smile where the restorative dentistry would be imperceptible while protecting the remaining dentition from structural compromise. It was critical for the clinician to understand the esthetic principles outlined above in order to handle the severe discrepancies in shape and form between the patient's right and left sides.
Patient history, evaluation, diagnosis, and treatment planning
A 40-year-old woman presented for a thorough assessment of her dental condition. A comprehensive examination was completed, including a full-mouth series of radiographs, periodontal evaluation, and diagnostic photographs (Figure 6). Her medical history was noncontributory.
The patient was congenitally missing her maxillary left lateral incisor and mandibular left central incisor, and was unhappy with the lack of symmetry in her dentition, broken edges on her front teeth, and unappealing teeth coloring. The maxillary left canine was positioned in the left lateral incisor space and had been restored with unsightly bonding to close the gap. Her maxillary left second premolar was rotated 90 degrees, and her maxillary and mandibular incisal edges were broken and worn (Figure 7).
The gingival zeniths are positioned at the most apical points of the clinical crowns.16 When assessing gingival display, it is important to use the patient's Duchenne smile, in which maximum lip dynamics occur as both the zygomatic major and orbicularis oculi muscles are engaged16; it is considered to be an authentic expression of happiness. In the patient's Duchenne smile in the present case, only the gingival zenith on the maxillary right lateral incisor was revealed, with the remaining teeth displaying a medium smile line, revealing the interproximal papillae but not the gingival zeniths. From a frontal perspective her smile was wide. On the right side, the distal of the maxillary right first molar was visible, but the left side presented with a dark buccal corridor. The center of her Cupid's bow was not coincident with the midline of her triangular-shaped central incisors. Her maxillary right canine had a round shape and was facially prominent and very attractive.
To achieve bilateral symmetry, an orthodontic consultation was recommended. The orthodontic treatment goal would have been to equalize the right and left spacing by moving the left canine into its proper position and creating space for placement of a single-tooth implant in the No. 10 site. The patient had the orthodontic consult but rejected any orthodontic treatment, primarily because of the extended amount of time it would have required.
She returned for a second restorative consultation to explore a solution that would be quicker than orthodontic therapy, albeit not ideal. She accepted the treatment goal as stated above, ie, modifying her smile using the principles of symmetry and harmony. Complete records were taken, including diagnostic models, occlusal records, and a facebow.
Digital smile design
The first step in the smile design process is to take a full-face photograph with the patient looking straight into the camera lens with a full, natural smile. Landmarks on the photograph are then correlated with landmarks on the digital design, and the midline and canting are evaluated. Outlining the preoperative tooth forms using smile design software allows the ceramist and dentist to visualize any dissimilarities, or inconsistencies, from the patient's right to left (Figure 8). This step is critical for any case with a significant space and size discrepancy so the existing tooth forms and inconsistencies can be identified.
Employing the continuous proportion theory, when designing the smile the clinician can use the ratio of the width established between the central and lateral incisors while progressing distally.12 In this case, using the smile design software the outline form of the patient's teeth on the right side was mirrored and digitally placed over the teeth on the left side (Figure 9). This evaluation revealed that the midline needed to be moved to the patient's left in order to equalize the right-to-left space discrepancy (Figure 10). Once the midline was moved, the maxillary right lateral incisor could be widened, the maxillary right central incisor could be repositioned to the patient's left, and the maxillary left canine could be slenderized.
The templates on the patient's left side were then fitted onto the teeth at the gingival margins (Figure 11). Lengthening the lateral incisors (thus, creating less dark space when the mouth is open) followed by closing the mesioincisal and distoincisal embrasures of tooth No. 7 would create the illusion of a wider tooth on the right lateral incisor. Rounding and opening the distoincisal of the left canine would create an illusion of a slenderized tooth (Figure 12).
The digital design from the preoperative photograph was accurately aligned and synced with the 3D model using blue landmarks (Figure 13). The final result of the preoperative alignment appears in gray in the digital design proposal, with exposed natural tooth structure visible as white areas (Figure 14). Final outlines are mimicked in white from the patient's right to left as close to the 3D model as possible, with respect given to the emergence of the restorations from the existing free gingival margin of the clinical crowns. The clinician can then analyze the relationship of the design proposal and the original preoperative condition and determine if the digital design is feasible to implement and whether it will meet the stated goals.
These 2D images are then entered into the 3D design as overlays (Figure 15). This step creates the final 3D design proposal (Figure 16).
The digital prototypes were virtually placed into the full-face photograph using the landmarks to allow the ceramist and dentist to perform a virtual try-in. The design can then be modified and developed to optimize integration of facially generated esthetics while minimizing tooth structure removal (Figure 17).
Upon completion of the digital try-in, a polymethyl methacrylate (PMMA) overlay may be milled or white wax can be milled and glued to a model to use as a diagnostic wax-up. Surface morphology and contours may be refined either by the ceramist at this time or by the dentist during the composite prototype phase.
Preparation appointment
At the preparation appointment, local anesthetic was administered. The incisal putty matrix (Sil-Tech®, Ivoclar Vivadent) fabricated from the digital design was used to dictate the contacts that were to be opened. When moving midlines and changing widths, it is necessary to open up contacts during the preparation phase. In this case the mesial of No. 7, distal of No. 8, and mesial of Nos. 8 and 9 were opened. The right central incisor distal contact was the first contact to be opened. This provided the room necessary to slenderize and change the outline form of the central incisors from triangular-shaped to square and created space for the right lateral incisor to be widened (Figure 18). Next, the contact between the central incisors was opened so the midline could be moved to the patient's left.
The provisional putty splint fabricated from the digital design was filled with a temporary composite material (B1 shade) (Luxatemp®, DMG America) and placed in the mouth. The patient previewed and approved the design, and depth-cut diamonds (Brasseler RWMIN 0.3/0.5/0.7 mm, Brasseler USA) were placed across the facial and established the facial reduction.17 Depth cuts on the incisal aspect were used to guide 2 mm of removal from the definitive postoperative incisal edge. Preparation of six teeth was finalized, followed by polyvinylsiloxane impression-taking (Honigum, DMG America) and recording of maximum intercuspation bite registration with a scannable material (Virtual® CADbite Registration, Ivoclar Vivadent). Stump shade photographs were taken for color documentation. The provisional restorations were fabricated with the B1 temporary composite (Luxatemp, DMG America), cemented with temporary cement (TempoCem®ID, DMG America), and documented with photographs.
The patient returned 3 days later for an esthetic re-evaluation and occlusal analysis. She requested that the left lateral incisor be made thinner and the maxillary left posterior teeth be more visible. As a result, the distal of the left lateral incisor was tucked in so it would appear thinner, and the buccal corridor of the left side was built out by increasing the volume on the canine and premolars using flowable composite (Beautifil® Flow, Shofu). Surface morphology and contours were refined using the line angle protocols discussed previously. A detailed laboratory prescription with final color, surface texture, and incisal translucency was generated. Photographs and approved provisional models were sent to the ceramist.
A HT BL2 lithium-disilicate ceramic ingot (IPS e.max®, Ivoclar Vivadent) was chosen for strength and esthetics to obtain the final desired color to match the patient's existing dentition.18The ceramist used distinct shade transitions and horizontal and vertical tertiary surface texture on the porcelain to create a symmetrical illusion from the patient's right to left (Figure 19).
Laboratory fabrication
The ceramist used the diagnostic model as a guide to make a silicone matrix to inject wax onto the working model. She then finalized the wax design by hand, separated it, sealed the margins, invested it, and pressed it out of the HT BL2 ingot. After it was cooled and devested, composite dies were made of the pressed restorations.
Typically, the ceramist would only layer teeth Nos. 7 through 10; cuspids generally are not layered for strength purposes. In this case, No. 6 was not restored, and it needed to be matched to the natural dentition on the patient's right side, so a surface stain was added to match.
The case was then adjusted and seated on the model, and the porcelain was adjusted to final contour and anatomy. The ceramist then made an incisal-edge matrix after finalizing the contour. Then, a cutback was made of teeth Nos. 7 through 10 and checked inside the matrix.
Next, a foundation firing was made with stain and glaze to add some effects for incisal translucency. After the initial firing, the ceramist strategically added brighter porcelains on the mesial and distal areas-small pieces for internal effects-and fired that. After checking it in the matrix again, she performed the final incisal layering with IPS e.max Impulse Opal Effect 1 (Ivoclar Vivadent) to achieve incisal translucency. That was then built up to contour and fired; either one or two firings may be necessary to achieve the exact desired appearance. With that completed, the ceramist performed the final contour, connecting all anatomy and ensuring that everything was nice and smooth, and that the contour was exactly where it needed to be.
For the final staining procedure, the ceramist assembled the restorations onto the composite dies and then added stains and effects, such as white highlights; she then held it up against the shade guide to confirm the final shade. The restorations were then fired using a lower-temperature stain set program. Once satisfied with the shade, the ceramist performed the glaze firing. Once she was satisfied with the glaze, the restorations were placed back on the model to check contacts, making adjustments where necessary. The completed restorations were then surface polished to achieve the desired texture and gloss. A drop of etching gel (IPS Ceramic Etching Gel, Ivoclar Vivadent) was then placed on the inside surface of each sandblasted restoration and etched for 20 seconds, rinsed, and cleaned. The restorations were then ready for delivery (Figure 20 through Figure 23).
Delivery appointment
The six maxillary prototype units were removed and the restorations were placed intraorally for esthetic evaluation using try-in gel (Choice 2, Bisco). The patient gave written approval of the restorations, and they were thus cemented following standard protocols using selective etching (Selective HV Etch, Bisco), a universal bonding agent (All-Bond Universal, Bisco), and adhesive cement (Duo-Link Universal, Bisco) (Figure 24).
Conclusion
Utilizing classical esthetic principles in combination with state-of-the-art technology allowed the clinician to efficiently evaluate all tooth placement and size options virtually. This digital evaluation also ensured that the chosen esthetic plan was minimally invasive and did not compromise tooth or supporting structures. The resultant successful, predictable outcome both pleased the patient and demonstrated that the perceived size of a tooth may matter more than the actual size of the tooth.
Acknowledgements
The author thanks Jean Martin, DDS, for editing. These concepts are based on the teachings of the Kois Center and the American Academy of Cosmetic Dentistry.
About the Authors
Joyce Bassett, DDS
Private Practice
Scottsdale, Arizona
Karsten Klimmek, MDT
MicroDental Laboratories
Troy, Michigan
Sandy Cook, CDT, AAACD
MicroDental Laboratories
Livermore, California
(Formerly CMR Dental Lab, Idaho Falls, ID)
References
1. Magne P, Versluis A, Douglas WH. Rationalization of incisor shape: experimental-numerical analysis. J Prosthet Dent. 1999;81(3):345-355.
2. Rufenacht CR. Fundamentals of Esthetics. Berlin: Quintessence Publishing; 1990:67-134.
3. Chiche GJ, Pinault A. Artistic and scientific principles applied to esthetic dentistry. In: Chiche GJ, Pinault A, eds. Esthetics of Anterior Fixed Prosthodontics. Chicago, IL: Quintessence Publishing; 1994:13-32.
4. Sieber C. Voyage: Visions in Color and Form. Berlin: Quintessence Publishing; 1994.
5. Gürel G. The Science and Art of Porcelain Laminate Veneers. Hanover Park, IL: Quintessence Publishing; 2003:61.
6. Johnston CD, Burden DJ, Stevenson MR. The influence of dental midline discrepancies on dental attractiveness ratings. Eur J Orthod. 1999;21(5):517-522.
7. Gillen RJ, Schwartz RS, Hilton TJ, Evans DB. An analysis of selected normative tooth proportions. Int J Prosthodont. 1994;7(5):410-417.
8. Allen EP. Use of mucogingival surgical procedures to enhance esthetics. Dent Clin North Am. 1988;32(2):307-330.
9. Heymann HO. The artistry of conservative esthetic dentistry. J Am Dent Assoc. 1987;spec no:14E-23E.
10. Levin EI. Dental esthetics and the golden proportion. J Prosthet Dent. 1978;40(3):244-252.
11. Lombardi RE. The principles of visual perception and their clinical application to dental esthetics. J Prosthet Dent. 1973;29(4):358-382.
12. Ward DH. Proportional smile design using the recurring esthetic dental (red) proportion. Dent Clin North Am. 2001;45(1):143-154.
13. Magne P, Belser U. Bonded Porcelain Restorations in the Anterior Dentition: A Biometric Approach. Hanover Park, IL: Quintessence Publishing; 2002.
14. Sesemann MR. Understanding and providing appropriate line angles to optimize smile design restorations. J Cosmet Dent. 2017;33(3):66-75.
15. Wells DJ. The lateral incisor: the unsung hero in smile design. AACD Journal. 1999;15(3):38-46.
16. Duchenne de Boulogne GB. The Mechanism of Human Facial Expression. Cambridge, UK: Cambridge University Press; 1990.
17. Magne P, Belser UC. Novel porcelain laminate preparation approach driven by a diagnostic mock-up. J Esthet Restor Dent. 2004;16(1):7-18.
18. IPS e.max® Press Scientific Documentation. Schaan, Liechtenstein: Ivoclar Vivadent AG; 2011.