You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
pproximately 97% of the US adult population experiences some form of tooth wear.1 Tooth wear, defined as the loss of tooth substance by a chemical or mechanical process that does not involve dental caries,2 is typically caused by any or a combination of three distinct processes: attrition, erosion, and abrasion. Abfraction, a further process that results in loss of tooth structure due to flexure of the tooth under occlusal loading, may potentiate wear by abrasion and/or erosion.3 Symptoms of tooth wear, which vary widely, include tooth sensitivity, difficulty chewing, and other functional problems, although many patients are asymptomatic.4 Changes in tooth shape, loss of surface characteristics, cingula, mamellons, smoothing of facial surfaces, thinning of enamel, rounding angles, and cupping and grooving on occlusal surfaces are some of the signs of tooth wear.5,6
A normal physiologic process that occurs throughout the lifespan of a tooth, tooth wear is a multifactorial problem, making it difficult to identify a single causative factor for a particular patient. One well-established cause of tooth wear is bruxism. Early diagnosis and treatment of bruxism and addressing the possible underlying causes of bruxism itself are important aspects of the management of tooth wear in affected patients. Malocclusion is another cause of attrition, and as such, requires corrective therapy.
ATTRITION AND BRUXISM
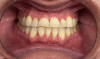
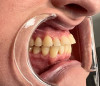
Whereas erosion is the result of chemical dissolution of tooth structure and abrasion is the loss of tooth structure caused by contact with external objects other than opposing teeth (eg, via vigorous toothbrushing), attrition is a wear process caused by direct tooth-to-tooth contact (Figure 1 and Figure 2).7 The most common cause of attrition is bruxism.8 Characterized by the involuntary gnashing, grinding, or clenching of teeth, bruxism is usually an unconscious activity, which may occur both during sleep (sleep bruxism) or when the individual is awake (awake bruxism).9-11 According to the American Dental Association, severe bruxing can cause extensive damage to the teeth and supporting structures.12
Prevalence and Etiology of Bruxism
Bruxism can begin at any age after the eruption of the deciduous teeth and occurs in all age groups. However, the exact data on bruxism prevalence are much more elusive. A wide range in prevalence has been reported in both children (6% to 50%),13and the general population (5% to 30%).9 The onset of sleep bruxism can occur as early as age 1 year.14 In studies, the prevalence of bruxism in study participants has been found to be 22.1% to 31% when the participants were awake and approximately 12.8% when they were asleep.15 However, these findings are from studies based on self-reported data, which are typically considered to be less reliable than other forms of clinical data.
Bruxism is generally accepted to have multiple causes, including psychosocial factors such as anxiety, pathophysiological factors that involve neurotransmitters or the basal ganglia, occlusal interferences, as well as several local, systemic, and other factors (Table 1).16-22Anxiety and emotional stress are believed to be the most common triggers in patients with awake bruxism.11,19 Malocclusion is also believed to be a possible pre- disposing factor of bruxism.11 Occlusal interferences are one of the most probable causes of bruxism and eccentric occlusion,20with eccentric occlusion resulting in premature contact of teeth. According to a study by Safari et al, evaluation of occlusal contacts in patients with bruxism can be useful in the assessment of causative factors.20
Complications and Sequelae
Teeth grinding involves the forceful closure of opposing dentition in a dynamic maxillomandibular relationship as the mandibular arch moves through areas of excessive position. Teeth clenching is the forceful closure of the opposite dentition in a static relationship of the mandible to the maxilla in either maximum intercuspation or an eccentric position.22 The lateral movement of the mandible during grinding often exceeds the edge-to-edge relation of the canines.23 Bite forces during sleep bruxism events can exceed the amplitude of maximum voluntary bite force when awake.24 Protective neuromuscular reflexes that are operational during waking hours appear to be suppressed during sleep, and this can lead to significant loading of teeth, the perio- dontium, and TMJ, as well as muscles of mastication. It has been estimated that loading of more than 20 g over periods of 2.5 seconds of clenching may occur during bruxing.25
Over time, these high-intensity occlusal forces overcome the body's adaptive capacity, resulting not only in tooth attrition, but in detrimental effects on the periodontium, the TMJ, and the masticatory muscles, as well pulp exposure, tooth mobility, tooth fractures, and abfraction lesions.11,25 Recurrent failure of and damage to dental restorations and implants may also occur. With eccentric occlusion, often the patient will try to adjust to the new habitual position caused by the occlusal interference26; this usually has a destructive effect on the surrounding structures.
Hearing loss, maxillofacial problems, and even facial deformation have been reported in patients with bruxism.27 In certain patients, capitulum mandibulae may change, and loss of the vertical dimension and mandibular displacement on the maximum intercuspidal position may develop.28 Bruxism may also have a psychological impact, as the esthetic appearance of the teeth caused by tooth wear can be troubling for many patients.
Diagnosis of Bruxism
Early diagnosis of bruxism is of great importance because timely treatment will help prevent the consequences of long-term tooth wear and other sequelae of the condition that impact quality of life. The diagnosis is generally made clinically based on the patient's history and on identification of signs and symptoms.19A history is obtained from the patient and/or spouse/partner, which may include oral history taking as well as questionnaires, and a clinical evaluation or examination should be performed. Evaluation for bruxism can also include measurement of the bite force weighed down on the intraoral appliances (such as a brux core plate).10
Patients will often report a history of grinding, usually noted by the patient's bed partner. Symptoms of bruxism that patients may report include pain or discomfort in the TMJ and/or in the masticatory and cervical muscles, hypersensitive teeth, frequent headaches (especially in the temporomandibular region), fatigue (due to poor-quality sleep),19 hypertrophic facial muscles, and reduced capacity to open the mouth after waking.29Symptoms of tooth wear, as described earlier, may also be present.
Common signs of bruxism are mobility of teeth, tooth fractures, and fractures or breakage of dental restorations (eg, fillings and prosthetic restorations such as crowns, bridges, or dentures), as well as signs of tooth wear (as described earlier).19 Evaluation of tooth wear includes the use of study casts and digital analyzers20 and assessment of the wear facets on intraoral appliances.10
Because research has shown that there is a relationship between certain types of occlusal interferences and bruxism, occlusal contacts should be evaluated in patients with bruxism to identify any probable causative occlusal factors.20
Electromyographic and polysomnographic assessments can support the diagnosis,30 but the activity patterns demonstrated by these studies only infer bruxism and do not provide a definitive diagnosis.9
According to international research criteria, sleep bruxism consists of the following: four or more episodes of increased activity per hour; more than six bursts of activity per episode and/or 25 activity bursts per hour of sleep; and at least two episodes of grinding sounds in a research environment.10 Individuals who have more than four sleep bruxism episodes per hour of sleep are considered severe sleep bruxers.31
According to the international research group that provided a consensus definition of and diagnostic grading system for bruxism in 2013, diagnosis may be divided into three categories: 1) sleep or awake bruxism is possible when it is based on self-report only; 2) sleep or awake bruxism is probable when it is based on self-report plus clinical examination; and 3) sleep bruxism is definite when it is based on self-reporting, clinical inspection, and polysomnographic recording, ideally accompanied by audio and video recordings.32
Treatment
Any of several treatments can be used for bruxism. Occlusal equilibration is one of the most common treatments for correcting occlusal interferences.33 Occlusal equilibration, or occlusal adjustment, is the planned alteration of the occlusal surface of teeth to provide stable jaw relationships with stable simultaneous interocclusal contacts and smooth excursive movements without occlusal interferences.34 An occlusal adjustment allows all of the patient's teeth to come into contact simultaneously. Occlusal adjustments are used to obtain a stable occlusal relationship and reduce stress in certain areas of your mouth. This is usually carried out in two stages. Stage one includes the alteration of occlusal contacts in the intercuspal position. In Stage two, the stable interocclusal and ideal maxillary and mandibular jaw relationship are achieved.35
According to Bandodkar et al,36 in order to effectively manage bruxism in patients, an ideal relationship between maximum inter- cuspation and centric relation is required.
Overall treatment objectives are to address the causes of bruxism and prevent and treat the complications and sequelae of the condition, including tooth wear. For some patients, the treatment of bruxism can require a multidisciplinary approach, including psychotherapy and speech therapy.10 Reducing physical and mental stress and identifying sources of anxiety are key, as stress and anxiety are the primary triggers of bruxism in patients with awake bruxism.19 In these patients, early treatment involves reducing psychological stress through the use of relaxation methods such as exercises, massages, and physiotherapy.These patients may also be counseled to reduce caffeine intake and quit smoking. Comprehensive treatment may include occlusal therapy, pharmacological therapy, behavioral therapy, and biofeedback.
Pharmacologic management may include the use of anti- anxiety medications and muscle relaxants, as well as tricyclic antidepressants to inhibit the amount of rapid eye movement (REM) sleep.11 Botulinum toxin has been used based on the premise that the action of the toxin will lessen the ability to forcefully clench the teeth.19
Occlusal Guards and Splints
Worn on the maxilla or mandible and covering the occlusal surfaces of all the teeth, occlusal guards and splints are often considered the first line of management for preventing dental grinding and tooth wear in these patients. Also known as bite guards and bite plates, occlusal splints act as a biomechanical stress relaxer and reduce deformation and deviations in the TMJ.37 These appliances stabilize occlusion by minimizing gradual changes to the positions of the teeth, and reduce muscle strain by allowing easier movement of the upper and lower jaw in relation to each other.19
Occlusal splints may be worn both at night and during the daytime. A myriad of splint designs/types are available, varying with regard to their rigidity and resiliency and the extent of occlusal coverage that they offer.38 These splints may be fabricated in the dental office or a laboratory from either hard or soft materials. It has been suggested that splints made from hard materials may be more effective than those made from soft materials, whereas soft materials may be more difficult to adjust.11
Compliance with both daytime and nighttime usage of occlusal splints can be a challenge.39 Compliance is greater with combination guards because they offer a soft comfortable inner surface along with a hard durable outer surface.40
By protecting the teeth from the clenching and grinding of the teeth, use of occlusal guards has been consistently reported to be an effective approach to preventing and reducing the symptoms and sequelae of bruxism, including tooth wear.41 However, there is inadequate evidence that use of occlusal appliances reduces bruxism itself.38
Orthodontic Treatment
Because it has been proposed that malocclusion may be one of the causes of bruxism, orthodontic treatment may be a viable treatment strategy to prevent tooth wear in these patients.11 Malocclusion itself, both in the presence and absence of bruxism, is a major cause of tooth wear caused by attrition,42 although it has also been reported that the association between malocclusion is observed in children but not in adults.43Although currently no evidence supports orthodontic treatment to manage bruxism itself or masticatory muscle activity during sleep,44 orthodontic therapy is one of the most common treatments for correcting malocclusion and may be useful in preventing attrition-related tooth wear.
Clear aligner systems are a popular choice through which patients can receive a dentist-prescribed and -monitored orthodontic treatment plan that can be completed at home by means of a teledentistry platform. Clear aligner systems are an excellent option to help achieve esthetic results for mild to moderate mal- occlusion cases. Clear aligners are preferred by many patients because they are more esthetically pleasing during treatment than fixed orthodontic appliances, and they have as advantages segmented movement of teeth and shortened treatment duration.44Fixed orthodontics, on the other hand, are more suitable for cases that require more complex tooth movements, such as extrusion or correction of severe rotations.45In addition, because of the mechanical stress and additional forces exerted through bruxism on the bonded teeth, fixed orthodontic retainers are at greater risk for failure in patients who are bruxers.43
Patients tend to have greater compliance with clear aligner systems that incorporate non-contact communication between patients and dentists, because of the convenience that tele- dentistry provides. Recent studies found that adult men are slightly more likely than women to be compliant with clear aligner therapy, while age and pretreatment satisfaction with one's own smile have not been associated with compliance.46 Interestingly, patients who had previous orthodontic treatment with removable appliances were found to be more compliant than the patients who had previous fixed orthodontic treatment.46
After orthodontic treatment has been completed to correct a patient's malocclusion, an occlusal guard can be fabricated to further protect the teeth from attrition in patients with bruxism, as bruxism has causes other than poor occlusion and may continue after misalignment of teeth has been addressed.
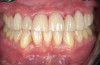
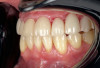
In addition, teeth affected by attrition will require restoration, and clear aligner therapy additionally provides the necessary tooth alignment to facilitate the fabrication of restorations (Figure 3 and Figure 4).
Conclusion
Tooth wear is a common and multifactorial condition with a complex etiology, which may be the result of one or a combination of chemical or mechanical processes (erosion, abrasion, and attrition). An important aspect in preventing tooth wear is identifying and managing its potential causes, such as bruxism. Along with several other treatment strategies that may be utilized as part of a comprehensive treatment plan, the use of occlusal guards and orthodontic treatment with clear aligners are suitable approaches to managing the symptoms and sequelae of bruxism and malocclusion, respectively. Reports on the general effectiveness of occlusal appliances in protecting the teeth from the grinding that occurs have been consistent. However, while occlusal splints play a role in protecting teeth from attrition, there is insufficient evidence that bruxism episodes themselves are reduced with this treatment. Because malocclusion has been proposed by some to be a potential underlying cause of bruxism, correction of malocclusion by means of orthodontic treatment such as clear aligner therapy may be another viable strategy to prevent tooth wear caused by bruxism. Clear aligner therapy is a highly effective solution to correct mild to moderate cases of malocclusion, thus preventing attrition-related tooth wear. Ultimately, teeth affected by attrition will require restoration, and clear aligner therapy additionally provides the necessary tooth alignment to facilitate the fabrication of restorations for anterior teeth.
References
1. Suchetha A, Sravani K, Mundinamane DB, Chandran N. Tooth wear - a literature review. Indian J Dent Sci. 2014; 6 (5):116-120.
2. Cunha-Cruz J, Pashova H, Packard JD, Zhou L, Hilton TJ; for Northwest PRECEDENT. Tooth wear: prevalence and associated factors in general practice patients. Community Dent Oral Epidemiol. 2010;38(3):228-234.
3. Addy M, Shellis RP. Interaction between attrition, abrasion and erosion in tooth wear. Mongr Oral Sci. 2006;20:17-31.
4. El Wazani B, Dodd MN, Milosevic A. The signs and symptoms of tooth wear in a referred group of patients. Br Dent J. 2012;213:E10.
5. Bartlett D, O'Toole S. Tooth wear and aging. Aust Dent J. 2019;64(S1):S59-S62.
6. Lussi A, Hellwig, Domenick Z, Jaeggi T. Erosive tooth wear: diagnosis, risk factors and prevention. Am J Dent. 2006;19(6):319-325.
7. Warreth A, Abuhijleh E, Almaghribi MA, Mahwal G, Ashawish A. Tooth surface loss: a review of literature. Saudi Dent J. 202032(2):53-60.
8. Green J. Prevention and management of tooth wear: the role of dental technology. Prim Dent J. 2016;5(3):30-33.
9. Thayer MLT, Ali R. The dental demolition derby: bruxism and its impact - part 1: background. Br J Dent.2022;232(8): 515-521.
10. Lobbezoo F, van der Zaag J, van Selms MK, Hamburger HL, Naeije M. Principles for the management of bruxism. J Oral Rehabil.2008;35:509-523.
11. Lal SJ, Webber KK. Bruxism Management. [Updated October 12 2022]. In: StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing, 2022.
12. American Dental Association. Mouthhealthy™ website. Teeth grinding and jaw pain. https://www.mouthhealthy.org/all-topics-a-z/teeth-grinding/. Accessed June 5, 2023.
13. Machado E, Dal-Fabbro C, Cunali PA, Kaizer OB. Preva- lence of sleep bruxism in children: a systematic review. Dental Press J Orthod. 2014;19(6):54-61. 14. Sari S, Sonmez H. The relationship between occlusal factors and bruxism in permanent and mixed dentition in Turkish children. J Clin Pediatr Dent. 2001;25(3):191-194.
15. Goldstein G, DeSantis L, Goodacre C. Bruxism: best evidence consensus statement. J Prosthodont. 2021;30(S1): 91-101.
16. Alves AC, Alchieri JC, Barbosa GA. Bruxism: masticatory implications and anxiety. Acta Odontológica Latinoamericana.2013;26(1):15-22.
17. Lobbezoo F, Naeije M. Bruxism is mainly regulated centrally, not peripherally. J Oral Rehabi.2001;28(12): 1085-1091.
18. Ohayon MM, Li KK, Guilleminault C. Risk factors for sleep bruxism in the general population. Chest.2001; 119(1):53-61.
19. Murali RV, Rangarajan P, Mounissamy A. Bruxism: conceptual discussion and review. J Pharm Bioallied Sci. 2015;7(Suppl 1):S265-S270.
20. Safari A, Jowkar Z, Farzin M. Evaluation of the relationship between bruxism and premature occlusal contacts. J Contemp Dent Pract. 2013;14(4):616-621.
21. Shetty S, Pitti V, Satish Babu CL, Surendra Kumar GP, Deepthi BC. Bruxism: a literature review. J Indian Prosthodont Soc. 2010;10(3):141-148.
22. Reddy SV, Kumar MP, Sravanthi D, Mohsin AH, Anuhya V. Bruxism: a literature review. J Int Oral Health. 2014;6(6):105-109.
23. Yap AU. Effects of stabilization appliances on nocturnal parafunctional activities in patients with and without signs of temporomandibular disorders. J Oral Rehabil.1998;25:64-68.
24. Nishigawa K, Bando E, Nakano M. Quantitative study of bite force during sleep associated bruxism. J Oral Rehabil.2001;28:485-491.
25. Toyama N, Ekuni D, Taniguchi-Tabata A, et al. Awareness of clenching and underweight are risk factors for onset of crowding in young adults: a prospective 3-Year cohort study. Int J Environ Res Public Health. 2019;16(5):690.
26. Koos B, Godt A, Schille C, Gernot Göz G. Precision of an instrumentation-based method of analyzing occlusion and its resulting distribution of forces in the dental arch. J Orofac Orthop. 2010;71(6):403-410.
27. Kitsoulis P, Marini A, Iliou K, Galani V, Zimpis A, Kanavaros P, Paraskevas G. Signs and symptoms of temporomandibular joint disorders related to the degree of mouth opening and hearing loss. BMC Ear Nose Throat Disord. 2011;11(1):5.
28. Alóe F. Sleep bruxism treatment. Sleep Sci.2009:
2(1):49-54. 29. Aguilera SB, Brown L, Perico V. Aesthetic treatment of bruxism. J Clin Aesthet Dermatol.2017;10(5):49-55.
30. Lavigne GJ, Montplaisir JV. Bruxism: epidemiology, diagnosis, pathophysiology, and pharmacology. In: Fricton JR, Dubner R, eds. Orofacial Pain and Temporomandibular Disorders: Advances in Pain Research and Therapy. New York: Raven Press; 1995:387-404.
31. Rompré PH, Daigle-Landry D, Guitard F, Montplaisir JY, Lavigne GJ. Identification of a sleep bruxism subgroup with a higher risk of pain. J Dent Res. 2007;86(9):837-842.
32. Lobbezoo F, Ahlber J, Glaros AG, et al. Bruxism defined and graded: an international consensus. J Oral Rehabil.2013;40:2-4.
33. Butler JH. Occlusal adjustment. Dent Dig.1970;76: 422-426.
34. Woods WD. Occlusal equlibration [letter]. J Am Dent Assoc. 2005;136(7):850.
35. Stefanac SJ, Nesbit SP. Diagnosis and Treatment Planning in Dentistry. 3rd ed. St. Louis, MO: Elsevier; 2017: 432-446.
36. Bandodkar S, Tripathi S, Chand P, et al. A study to evaluate psychological and occlusal parameters in bruxism. J Oral Biol Craniofac Res. 2022;12(1):38-41.
37. Gholampour S, Gholampour H, Khanmohammadi H. Finite element analysis of occlusal splint therapy in patients with bruxism. BMC Oral Health. 2019;19:205.
38. Demjaha G, Kapusevska B, Pejkovska-Shahpaska B. Bruxism unconscious oral habit in everyday life. Open Access Maced J Med Sci. 2019;7(5):876-881.
39. Hassan KA, Salwa EK. Awake bruxism intensified during COVID-19 pandemic by cumulative stress-an overview. J Clin Res Dent . 2020;3(1):1-3.
40. Al-Abdallah M, Hamdan M, Dar-Odeh N. Traditional vs digital communication channels for improving compliance with fixed orthodontic treatment: a randomized controlled trial. Angle Orthod.2021;91(2):227-235.
41. Melo G, Duarte J, Pauletto P. Bruxism: an umbrella review of systematic reviews. J Oral Rehabil. 2019;46(7): 666-690.
42. Raj A, Ranjan R, Kumar A, Kumar M, Mala N, Ramesh K. Evaluation of Dental Status in Relation to Excessive Horizontal and Vertical Overlap in North Indian Population. J Pharm Bioallied Sci. 2021;13(Suppl 1):S276-S279.
43. Labuneț A, Objelean A, Almășan O, Kui A, Buduru S, Sava S. Bruxism's implications on fixed orthodontic retainer adhesion. Dent J (Basel). 2022;10(8):141.
44. Ke Y, Zhu Y, Zhu M. A comparison of treatment effectiveness between clear aligner and fixed appliance therapies. BMC Oral Health. 2019;19(1):24.
45. Rossini G, Parrini S, Castroflorio T, Deregibus A, Debernardi CL. Efficacy of clear aligners in controlling orthodontic tooth movement: a systematic review. Angle Orthod.2015;85(5):881-889.
46. Timm LH, Farrag G, Baxmann M, Schwendicke F. Factors influencing patient compliance during clear aligner therapy: a retrospective cohort study. J Clin Med. 2021; 14;10(14):3103.