You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Ensuring patient comfort during dental procedures is an essential aspect of oral health care, not only during treatments such as restorative procedures and more complex dental reconstructions, but also during simple diagnostic procedures such as imaging and impression taking. Providing comfort to the patient can involve addressing psychological as well as physical issues, as dental anxiety (ie, the stress or dread experienced before, during, or after dental treatment) is a common source of patient discomfort. Because it often leads to avoidance of dental treatment, dental anxiety may also indirectly contribute to increased oral and general health problems.1 Patient discomfort may additionally result from unpleasant physical sensations during dental procedures, such as gagging reflexes that may occur when bitewing radiographs are taken or with impression taking, which may, in turn, result in psychological distress during the dental visit.2 In the case of impression taking, gagging may also severely limit the ability of the dental practitioner to perform the procedure, which can compromise the accuracy and fit of the final restorations and, ultimately, the quality of care.3
Impression taking is one of the most essential procedures involved in the fabrication of restorations. Although the exact prevalence is unknown,4 unfortunately many patients experience gagging during impression taking, while anxiety and other forms of discomfort during the procedure are common.5Dental healthcare professionals should therefore employ various management strategies to address the gag reflex and anxiety that patients can experience during dental procedures. Practitioners should consider ways of mitigating aspects of impression taking that may contribute to these problems, such as the duration of the procedure. This article examines strategies and techniques to reduce dental anxiety and gagging during impression taking. It discusses ways to maximize patient comfort, such as by performing the procedure more efficiently and, when possible, with dental impression materials that minimize gagging and promote efficiency, thus creating a more comfortable experience for the patient.
Dental Anxiety
Many patients may feel uncomfortable, anxious, or fearful before, during, and even after dental procedures. This phenomenon, known as dental anxiety, is highly prevalent worldwide (approximately 25% of the population).1,6 However, while it is often assumed that perceptions or anticipation of pain cause dental anxiety, for some patients there are additional causes for their anxiety about dental treatments, which may be experienced even during "pain-free" procedures.6 It has been postulated that the origin of dental anxiety is multidimensional and includes both endogenous and exogenous causes; several psychological disorders (such as low self-esteem, general anxiety disorder, and alcohol dependence) have been reported in patients with dental anxiety.6 Many patients who have never had negative dental experiences have reported feelings of vulnerability and of "not being in control" as well as the perceived "unpredictability" of the procedures as reasons for their anxiety.7 Impression-taking procedures can potentially induce these feelings in some patients. Left unaddressed, dental anxiety can lead to avoidance of dental treatment, which can harm oral and general health.1
The Gag Reflex and Its Etiology
Gagging is an involuntary and unpleasant contraction of the soft palate or pharynx muscles that results in retching.8 As such, the gag reflex is the body's natural way to prevent potentially dangerous objects in the mouth from entering the throat and blocking the airway and thus helps prevent choking when the situation does not involve normal swallowing. According to a study published in The Lancet, about 37% of healthy adults do not have a gag reflex.9Conversely, 10% to 15% of people have a
hypersensitive gag response in which even the slightest sensation can trigger an involuntary throat contraction.10The remainder typically respond to non-swallowing sensations in the pharynx. Therefore, when taking dental impressions, dental healthcare professionals must consider the trigger that the impression material will cause during insertion.
Five areas of the oral cavity are trigger zones for gagging: the palate, uvula, base of the tongue, the fauces (leading to the pharynx), and the posterior pharyngeal wall.2,10 When any of these areas is stimulated by touch, afferent fibers from the trigeminal, glossopharyngeal, and vagus nerves pass to the medulla oblongata in the brain stem. This then signals the muscles in the back of the mouth to contract or push up, resulting in gagging.2 Also, neural pathways from the center of the medulla oblongata or the "gagging center" to the cerebral cortex allow the reflex to be modified by higher centers, allowing thoughts about stimulation to initiate the gagging in some instances.2 Therefore, in some patients, simply thinking about dental impressions (or other procedural stimuli) may stimulate this reflex.
Techniques to Reduce Gagging and Dental Anxiety During Impression Taking
Depending on the patient's gag reflex severity, techniques to reduce gagging can be introduced and incorporated into the dental visit. While there are many evidence-based approaches to reduce gagging before the office visit in a patient with a history of a gag reflex, including anti-nausea medicine, sedatives, local and general anesthetics, behavioral therapies, and acupuncture,2 these interventions are beyond the scope of this section, which focuses on simple, nonpharmaceutical strategies, many of which can be adopted during the office visit. Likewise, several management strategies exist to address dental anxiety, including pharmacologic and psychotherapeutic interventions, that are beyond the scope of this article.1 In this article, we will explore simple strategies that can be undertaken during or immediately before impression taking when anxiety is identified during the office visit.
Inspire Trust and Provide Reassurance
Experiencing occasional anxiety is a normal part of life. However, people with anxiety disorders frequently have intense, excessive, persistent worries and fears about everyday situations. Having an initial conversation with patients about their anxieties before taking impressions helps inspire trust and conveys sensitivity and understanding.11 Explaining the impression
taking procedure to patients, including the estimated time for placement and setting, can reassure patients and help them feel safe and in control. Additionally, answering patients' questions while encouraging them to share their anxieties helps reinforce their trust and confidence.12
When a dental impression material has been selected that minimizes the likelihood of gagging, as in the case of vinyl polysiloxane (VPS) (as discussed later in this article), the practitioner should explain the benefits of the dental impression material and how the material will improve the patient's comfort during the procedure; positive encouragement should always set the tone for every dental procedure, and by helping patients understand and know what to expect, their anxiety will be reduced.
Relaxation Techniques
Relaxation techniques that the patient can perform during the office visit include breathing exercises, which can both alleviate anxiety and reduce gagging.8To begin rhythmic breathing, the dental practitioner should ask patients to breathe through their noses. The practitioner should ask the patient to sit up straight in the chair and relax their shoulders. Next, the patient should be instructed to uncross their legs and tip their toes towards the practitioner. Because anxiety such as that caused by impression
taking may trigger faster breathing, patients should be told to continue breathing through their nose and to take deep breaths, as this will help increase how much oxygen is taken in. This may help slow breathing, reduce the heart rate, and alleviate the patient's anxiety.12The author recommends asking patients to practice first by closing their lips and inhaling slowly through the nose, letting the chest rise and fill with air; the practitioner can demonstrate this by practicing the exercise with the patient. Breathing deeply through the nose should be continued throughout the minutes required to take a good impression.
Keep a Tissue Handy
Always have a tissue handy in case the patient feels they are drooling. Provide a tissue to the patient so that they can allow saliva to drain out of the mouth. This may sometimes reduce the gag reflex.13
Acupressure
Although acupuncture has been shown to be successful in reducing gag reflex,8 this procedure can be performed only by a licensed therapist. Acupressure is very similar to acupuncture, utilizing the same pressure points, but it can be performed by anyone and without the use of needles. Because acupressure uses gentle-to-firm finger pressure alone to stimulate pressure points on the body, it is ideal for self-treatment wherever and whenever necessary. Evidence supports its use for reducing the gag reflex; in one study, researchers found that pressure applied to a specific point on the palm consistently altered the severity of the gag reflex (Figure 1).14In the author's experience, anecdotal evidence also suggests that if a person closes their left hand over their left thumb and applies gentle pressure, it may stop them from gagging. Another technique for suppressing the gag reflex that has been effective in the author's experience involves applying pressure to the concave point between the thumb and index finger (Figure 2).
Simple Distractions
Distraction techniques have been reported to reduce anxiety and gagging.8 The dental practitioner should provide the patient with something to hold. Stress balls can reduce stress, enhance mood, and induce relaxation. A stress ball diverts the patient's attention from negative thoughts towards those that are more pleasant and promotes relaxation. Talking to the patient or even singing (for example, singing along with the radio in the operatory) can provide simple distractions that will help take the patient's mind off the procedure.8
Selection of Impression Materials
The choice of impression materials is also essential in providing a more comfortable experience and reducing gagging for patients during impression taking.15 Alginate is an irreversible elastic hydrocolloid (Figure 3) that has various applications in dentistry. The applications of alginates include making impressions of edentulous and partially edentulous arches, duplication of casts, and study models. Alginates possess numerous vital properties such as
hydrophilicity, the ability to record finer details, and elastic recovery, and because it is inexpensive, this material is widely used in dentistry. Unfortunately, alginate impression materials historically have demonstrated a low tear strength and inconsistent setting and working times.16 Because of their delicate nature, impressions made from alginate materials have not been used for multiple pours; alginate impressions typically must be poured immediately to avoid losing accuracy due to dehydration.17
Although VPS impression material is slightly more expensive, it has several advantages, particularly in term of ensuring efficiency and decreased procedural time during impression taking. It produces great detail reproduction, has stability over time, and high tear strength and elastic recovery.18 However, because VPS is a hydrophobic substance, proper moisture control must be maintained to achieve accuracy and a high-quality impression.18
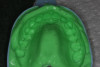
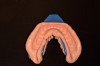
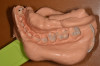
These anatomical impressions made from VPS reproduce the dental and mucosal structure of the patient's oral cavity (Figure 4 and Figure 5) and are used to create orthodontic models, opposing models, temporaries, night guards/splints, and custom bleaching trays (Figure 6). An impression made from VPS can withstand numerous pours; this allows the impression to be used to make multiple models for the patient, if necessary. With an alginate impression, only one model can be made, and duplicates will need to made with a unique material. Repeating the impression taking clearly adds to the overall procedural time, which increases the likelihood of discomfort for patients with a history of dental anxiety or gagging. VPS also creates less mess and reduces the likelihood of seepage of the material toward the back of their throat.
The efficiency of the impression-taking procedure can be largely driven by the dental impression material. With VPS impression material, impressions can be poured immediately-or when convenient, so provisional fabrication can begin as soon as the impression is removed from the patient's mouth. Other impression materials can require 20 minutes of waiting before pouring. The use of VPS impression material thus results in a shorter and more convenient appointment for patients. Shorter procedural durations reduce the opportunities for anxiety to develop, and patients will be less anxious about future impression-taking procedures, as they will remember their last experience in a positive light.
Finally, the accuracy of the dental impression is a crucial aspect of ensuring patient comfort, as the final successful outcome of the restoration promotes confidence in the patient and allays anxiety about requiring further dental treatment for the restored tooth. Also, when dental impressions are found to be inaccurate, unstable, or deformed, dental impressions will need to be retaken. As already mentioned, when proper moisture control is ensured, the use of VPS impression material provides fine detail and accuracy in impressions.18Furthermore, VPS material demonstrates low dimensional changes and retains its shape upon setting for months without needing special storage.19 The material also can be disinfected without concerns about affecting dimensional stability. As a result, impressions can be used again in the future, avoiding the need for repeating the impression taking. Patients' future needs and concerns can thus be addressed quickly and efficiently, even in emergencies. Providing patients with the assurance that impression taking will not need to be repeated creates a positive experience for the patient, which in turn helps reduce future dental anxiety.
With impressions made from VPS, a provisional restoration that needs adjustment or becomes dislodged can be remade using the initial impression. Even after final restorations are delivered, temporary crowns may again be needed.18 For example, patients who undergo gingival surgery or implant placement may be in provisionals for several months, during which time the temporaries may need to be replaced. If alginate impressions were taken, the patient would require another impression procedure. With VPS, the initial impression can be used and a new provisional easily created, without the need for a repeated impression-taking procedure.
Conclusion
Dental anxiety is a multidimensional phenomenon, and dental healthcare professionals may sometimes be limited in their ability to fully address this problem in certain patients. Never-
theless, much can be done to ensure that patients are as comfortable as possible during dental treatments and procedures, and dental anxiety can be ameliorated in most cases by employing some simple techniques during the office visit. Likewise, gagging, which is by definition an involuntary reflex, can be prevented and reduced at the time of or immediately before the procedure through interventions such as acupressure, breathing exercises, and distraction techniques. Selection of impression materials, such as vinyl polysiloxane (VPS), can also help reduce gagging and anxiety during impression taking. Advancements in material science and the handling characteristics, accuracy, stability, and setting times of VPS have helped provide efficient, short-
duration procedures and accurate and high-quality impressions, which are crucial for successful outcomes and avoid the need for retaking impressions. By following these simple strategies, dental practitioners can ensure patient comfort both during impression taking and beyond, by creating a positive experience that will carry over to future dental visits.
About the Author
Shannon Pace Brinker, CDA, CDD
Private Practice
Virginia Beach, Virginia
References
1. Hoffman B, Erwood K, Ncomanzi S, Fischer V, O'Brien D, Lee A. Management strategies for adult patients with dental anxiety in the dental clinic: a systematic review. Aust Dent J. 2022;67(Suppl 1):S3-S13.
2. Eachempati P, Kumbargere Nagraj S, Kiran Kumar
Krishanappa S, George RP, Soe HHK, Karanth L. Management of gag reflex for patients undergoing dental treatment. Cochrane Database Syst Rev. 2019;2019(11): CD011116.
3. Dickinson CM, Fiske J. A review of gagging problems in dentistry: 2. Clinical assessment and management. SADJ. 2006;61(6):258-262, 266.
4. Mangano A, Beretta M, Luongo G, Mangano C, Mangano F. Conventional vs digital impressions: acceptability, treatment comfort and stress among young orthodontic patients. Open Dent J. 2018;12:118-124.
5. Yilmaz H, Konca FA, Aydin MN. An updated comparison of current impression techniques regarding time, comfort, anxiety, and preference: a randomized crossover trial. Turk J Orthod. 2021;34(4):227-233.
6. Facco E, Zanette G. The odyssey of dental anxiety: from prehistory to the present. a narrative review. Front Psychol. 2017;8:1155.
7. Armfield JM. Towards a better understanding of dental anxiety and fear: cognitions vs. experiences. Eur J Oral Sci. 2010;118(3):259-264.
8. Forbes-Haley C, Blewitt I, Puryer J. Dental management of the ‘gagging' patient - an update. Int J Dental Health Sciences. 2015;3(2):424-431.
9. Davies AE, Stone SP, Kidd D, MacMahon J. Pharyngeal sensation and gag reflex in healthy subjects. Lancet. 1995;345(8948):487-488.
10. Cox L, Brindley J. Exploring alternative methods of gag reflex control. Part 2: acupuncture. BDJ Team. 2017;4:17139.
11. Hashim MJ. MD patient-centered communication: basic skills. Am Fam Physician.2017;95(1):29-34.
12. Yang X-J, Jiang H-M, Hou X-H, Song J. Anxiety and depression in patients with gastroesophageal reflux disease and their effect on quality of life. World J Gastroenterol. 2015;21(14):4302-4309.
13. Alhajj M, Babos M. Physiology, Salivation. In: StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing; 2021. Available from: https://www.ncbi.nlm.nih.gov/books/NBK542251/. Accessed February 4, 2022.
14. Scarborough D, Bailey-Van Kuren M, Hughes M. Altering the gag reflex via a palm pressure point. J Am Dent Assoc. 2008;139(10):1365-1372.
15. Farrier S, Pretty IA, Lynch CD, Addy LD. Gagging during impression making: techniques for reduction. Dent Update. 2011;38(3):171-172, 174-176.
16. Massad J, Lobel W, Garcia L, Monarres A, Hammesfahr PD. Building the edentulous impression-a layering technique. Compend Contin Educ Dent. 2006;27(8):
446-451.
17. Kurtzman G. Creating great dental impressions. Inside Dental Assisting. 2012;8(1):42-45.
18. Heboyan AG, Muradyan RG. Impression material selection and soft tissue management in contemporary fixed prosthodontics. Int Acad Journal Web of Scholar. 2019; 5(35). doi: 10.31435/4sglobal_wos/31052019/6499
19. Wassell RW, Barker D, Walls AWG. Crowns and other extra-coronal restorations: impression materials and technique. Br Dent J. 2002;192(12):679-684, 687-690.