You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Until recent developments in dental science and technology, traditional materials for tooth restoration (eg, lithium disilicate, porcelain, amalgam, and gold) have been inert (ie, exhibit no interaction with the tooth structure) and have offered no biologic benefit to the surrounding tissues other than to "occupy the space" left after removal of decay and the completion of tooth preparation. New bioactive dental materials have emerged that increase the longevity of dental restorations and improve clinical outcomes after dental procedures.
The Benefits of Bioactive Dental Materials
For the past several decades, the concept of bioactivity in dentistry has been associated primarily with fluoride release and the conversion of hydroxyapatite to its stronger form, fluorapatite. Fluoride strengthens tooth enamel and makes it more resistant to acidity. Common applications of bioactivity have included fluoridated water and fluoride treatments.
Today, with the emergence of many new bioactive dental materials, the definition of bioactivity in dentistry is expanding. The ability of dental materials to contribute calcium and phosphate ions to help rebuild demineralized dentin has enabled a new treatment paradigm. Bioactive materials are considered to have "smart" behavior if they have the capacity to interact with living tissues or systems1 and if they can react to pH changes in the oral environment to foster advantageous changes in the properties of the dental material itself or the material-tooth complex.2
In this context, "biomineralization" refers to the exchange of calcium and phosphate ions with the tooth substance, forming new apatite or, in many cases, repairing existing demineralized apatite. Bioactivity also includes the precipitation of apatite crystals on the surface of the dental material in the presence of moisture (saliva). Bioactive dental materials have several benefits, including 1) stimulation of the natural remineralization process; 2) "moisture-friendly" properties that facilitate transport of water and other essential minerals vital to the natural remineralization process; and 3) the ability to form a layer of apatite and a natural bond between the restorative material and the tooth.3-5
Bioactive Cavity Liners and Bases
Traditional cavity liners include calcium hydroxide and resin-modified glass ionomer cements. However, use of calcium hydroxide is contraindicated under composite resins because it interferes with the set of the material. Also, many of the light-cured glass ionomer liners are resin reinforced, and depending on the resin content, this can limit any benefit from the release of fluoride. In addition, traditional resin-based cavity liners have been shown to be cytotoxic to odontoblast-like cells.6 Bioactive liners have dramatically changed the treatment of dental caries by helping replenish the missing calcium and phosphate ions that are lost as a result of acid attack (decay). It is important to remember that when caries are present, histologically there are two types of dentin: 1) infected dentin, which is demineralized and full of bacteria, and 2) affected dentin, which is demineralized but bacteria free. Affected dentin can be remineralized and converted back into healthy dentin, as shown in the study by Sauro and colleagues.7 However, although affected dentin may be "sticky" to the tactile touch, it should not necessarily be removed.
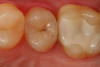
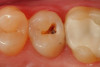
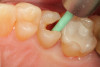
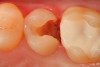
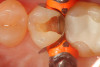
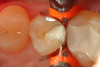
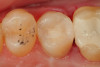
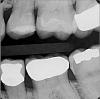
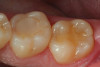
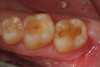
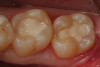
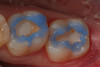
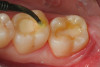
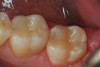
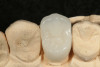
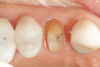
Use of round, polymer burs (Smart Bur II: SS White) that are fabricated at the specific Knoop hardness of healthy dentin (90) can be used to ensure that only infected dentin is removed during the excavation process. Placement of a bioactive liner can then help remineralize and rebuild the remaining affected dentin and restore it to healthy dentin (Figure 1 through Figure 8).
Examples of bioactive cavity liners that are currently available include TheraCal™ LC (Bisco Dental Products), ACTIVA™ BioACTIVE Base/Liner (Pulpdent Corporation), and Calcimol LC (VOCO). These products have all been shown to exhibit bioactive properties.
TheraCal LC differs from the other bioactive cavity liners in that its calcium silicate chemistry enables it to be used on pulp exposures, as well.8-10 Expanding on the ability to use a calcium silicate product for direct pulp capping, TheraCal PT® (Bisco Dental Products) was developed to be used when vital pulp therapy, such as pulpotomy, is performed. This material is a dual-cured calcium and fluoride-releasing material that can be used when vital pulpectomies are performed on teeth that have carious exposures. TheraCal PT is particularly useful when vital pulpectomies are performed on deciduous teeth to help maintain the viability of the tooth until it is exfoliated. Biodentine® (Septodont) is a tricalcium silicate material, which can be used as a bioactive "build up" material when large areas of tooth structure are missing and a pulp exposure or root perforation may exist. Although some patients who undergo these "heroic" procedures may eventually require endodontic therapy, many cases will respond favorably, thus avoiding an additional procedure and preserving the vitality of the tooth. TheraBase® (Bisco Dental Products) is a dual-cure calcium- and fluoride-releasing self-adhesive base/liner material that can be placed alone (if there is no pulp exposure) or with a layer of TheraCal LC (if there is a pulp exposure). The hydrophilic resin matrix facilitates calcium release, making it a good dentin replacement that can then be layered with composite to complete the restoration (Figure 9 through Figure 14). Finally, mineral trioxide aggregate (MTA) is another option to use for pulp exposures and perforations of the root system. Mineral trioxide aggregate was developed for use as a dental root repair material. It has been successfully used clinically to create "apical plugs" during apexification, as well as repair root perforations and treat internal resorption, and as a direct pulp capping agent. Its high alkalinity and antimicrobial properties give MTA a high degree of biocompatibility.
Bioactive Restorative Materials
Bioactive restorative materials can protect as well as repair and help seal the marginal gap that exists around all dental restorations, thus helping to preserve the natural tooth and extend the longevity of the dental restoration. ACTIVA BioACTIVE Restorative (Pulpdent Corporation) is one such restorative material. It is particularly useful for patients with high caries indices and highly acidic oral environments, which can create extensive damage to teeth, as well as for pediatric patients who still have their primary teeth. The need to complete a procedure quickly in a less than "moisture-free" environment makes traditional composites and adhesives very difficult to use in pediatric patients.
One composite currently available on the market (Beautifil II and Beautifil Flow Plus, Shofu) has a glass filler called a Giomer, which is coated with a glass-ionomer phase with a protective coat over the top of that phase, allowing the slow release of ions over time. Although Giomers do not release calcium and phosphate ions, they do release many other basic ions that can help "buffer" the effects of the acid environment in the oral cavity, helping inhibit plaque accumulation on restorations and at the margins.11-13ACTIVA Presto™ (Pulpdent Corporation) is the first light cure, mineral-enriched composite that mimics the properties of natural tooth structure. This material also has the esthetic quality to match nanocomposite and microhybrid composite materials, and it can be used for all anterior and posterior applications.
Bioactive Dental Cements
In crown-and-bridge dentistry, an acceptable "restorative-tooth gap" or margin has long been reported to be 30 to 50 μ, Because a marginal gap that small is not perceptible to a sharp dental explorer, to the clinician this marginal space is considered "closed." However, the term "closed" is misleading. Bacteria that live in the oral cavity, in plaque, and around teeth and dental restorations can be less than 1 μ in diameter. During their normal metabolism, bacteria break down sugars and produce acid byproducts that can cause demineralization of tooth structure, leading to recurrent decay. This "low pH" environment can pose a constant danger to the maintenance of healthy teeth and dental restorations.
One recent type of dental cement can precipitate apatite on its surface, buffer the acidic pH of the tooth-restorative environment, and help reduce the adherence of plaque, all of which help to give a level of protection around crowns that is not realized with traditional crown-and-bridge cements. One of the first such dental cements that was brought to market was a calcium aluminate crown-and-bridge cement called Ceramir® Crown & Bridge (Doxa Dental). This was followed by self-etching resin cements that offered some of the same bioactive benefits. TheraCem® (Bisco Dental Products) is a dual-cured, calcium- and fluoride-releasing, self-adhesive resin cement indicated for luting crowns, bridges, inlays, onlays, and posts (prefabricated metal/nonmetal/fiber posts) (Figure 15 through Figure 20). Continuous release of calcium and fluoride and a high alkaline pH to buffer acid attack are attributes of this self-etching resin cement. Also, apatite can be seen precipitating on the surface of TheraCem. Conventional crown-and-bridge cements over time can potentially break down, leaving microscopic gaps where bacteria and biofilm can invade and cause further damage. Materials that can precipitate apatite on the surface have the ability to self-seal and protect from further damage.4 Other cements on the market in this category include ACTIVA BioACTIVE cement (Pulpdent Corporation), Calibra Bio (Dentsply Sirona), and BioCem® (NuSmile).
The Future of Bioactive Dental Materials
The future of bioactive dental materials is promising. New innovations continue to emerge that reinforce existing technologies and set new paradigms for treating dental disease and restoring broken dentitions. Dental restorations and adjunctive materials will no longer simply "occupy space" between themselves and the surrounding tooth but will help repair and sustain healthy tooth structure, allowing our patients to have a better chance to enjoy healthy dentition throughout their lifetime.
As Jack L. Ferracane, PhD, of the Department of Restorative Dentistry at the Oregon Health & Science University noted, "In the future, the desire for a biomaterial to be inert and nonharmful to the patient, while still relevant and necessary, will no longer be considered sufficient. New materials, currently being introduced, under development, or simply envisioned, are expected to be bioactive, in that they will be intended to interact in some positive way with the oral environment. These materials will provide a wide range of diverse functions, including the routine inhibition of bacterial biofilm formation, remineralization of lost dentin and enamel, and the regeneration of diseased pulp, bone, and soft tissues."14
References
1. Comisi JC. Using bioactive materials to achieve proactive dental care. www.oralhealthgroup.com/features/using-bioactive-materials-to-achieve-proactive-dental-care. December 1, 2011. Accessed June 2, 2021.
2. McCabe JF, Yan Z, Al Naimi OT, Mahmoud G, Rolland SL. Smart materials in dentistry. Aust Dent J. 2011; 56(Suppl 1):3-10.
3. Hench LL, Paschall HA. Direct chemical bond of bioactive glass ceramic materials to bone and muscle. Biomed Mater Res. 1973;7(3):25-42.
4. Jefferies SR, Fuller AE, Boston DW. Preliminary evidence that bioactive cements occlude artificial margin gaps. J Esthet Restor Dent. 2014;26(1):14-26.
5. Cao W, Hench LL. Bioactive materials. Ceram Int. 1996;22:493-507
6. Hebling J, Lessa FC, Noqueira I, Carvalho RM, Costa CA. Cytotoxicity of resin-based light-cured liners. Am J Dent. 2009; 22(3):137-142.
7. Sauro S, Pashley DH. Strategies to stabilise dentine-bonded interfaces through remineralising operative approaches - State of The Art. Int J Adhesion and Adhesives. 2016;69:39-57.
8. Gandolfi MG, Siboni F, Taddei P, Modena E, Prati C. Apatite-forming ability of TheraCal pulp-capping material, J Dent Res.2011;90 (Spec Iss A); abstract 2520.
9. Peskersoy C, Lukarcanin J, Turkun M. Efficacy of different calcium silicate materials as pulp-capping agents: randomized clinical trial. J Dent Sci. 2021;16(2):723-731.
10. Rodrigues NS, França CM, Tahayeri A, et al. Biomaterial and biofilm interactions with the pulp-dentin complex-on-a-chip [published online ahead of print May 23, 2021]. J Dent Res. doi: 10.1177/00220345211016429.
11. Nakamura N, Yamada A, Iwamoto T, et al. Two-year clinical evaluation of flowable composite resin containing pre-reacted glass-ionomer. Pediatr Dent J. 2009;19(1):89-97.
12. Tamura D, Saku S, Yamamoto K, Hotta M. Saliva protein which adsorbs to composite resin containing S-PRG filler. The Japanese Society of Conservative Dentistry. 2010;53(2):191-206.
13. Saku S, Kotake H, Scougall-Vilchis RJ, et al. Antibacterial activity of composite resin with glass-ionomer filler particles. Dent Mater J.2010;29(2): 193-198.
14. Ferracane JL, Pfeifer CS, Bertasson LE. Biomaterials for oral health. Dent Clin North Am. 2017;61(4):xi-xii.