You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Autism spectrum disorder (ASD) is a group of complex developmental conditions arising from central nervous system perturbations leading to declines in social interaction and communication skills (verbal and nonverbal), behavioral norms, sensory processing, and possibly cognitive performance.1,2 Degree of impairment varies from high-functioning autism to severe involvement.3 The prevalence of ASD within the United States has increased from 1.3% to 1.7% among children aged 4 years from 2010 to 2014. Prevalence also varies geographically, ranging from as low as 0.9% to 1.0% in Missouri to 2.0% to 2.8% in New Jersey.4 Early detection and intervention are key regimens for optimal learning and applicable behavioral guidance. Pooled data indicate that males are affected 2 to 3 times more frequently than females although this gender predilection may underrepresent some high-functioning females who are often diagnosed later in life.5 It has been determined that genetic factors play some role in the pathogenesis of ASD while the impact of various environmental contributions has been inconclusive.6
Oral healthcare professionals (OHCP) may be faced with increased challenges in rendering clinically acceptable radiographs in individuals with ASD. However, there is limited information in the literature regarding helpful behavioral modifications when taking radiographs on this cohort. In a pilot study of 20 autistic patients, Lowe and Lindemann reported a 50% success rate of completion of an initial oral examination including bitewing radiographs yet information regarding their treatment protocol had not been disclosed.7 The task of taking diagnostically acceptable radiographs on ASD-affected patients may be hindered by their difficulties with understanding instructions, lack of cooperative behavior, and other communication difficulties. The objective of this report is to provide a useful template of basic and advanced guidance techniques to employ during dental radiographic examinations for individuals with ASD.
Discussion
General features of autism
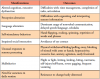
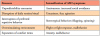
Stereotypical behavior. Individuals with ASD often manifest central nervous system (CNS) alterations (language expression, cognitive and sensory processing, executive dysfunction), and frequent engagement in repetitive or inappropriate behavior, any of which could hinder the completion of healthcare provider tasks and promote an unsuccessful and possible negative clinical experience. Individuals affected with ASD may also exhibit reduced tendencies to engage in a wide range of interests (Table I).5 ASD is also associated with anxieties and diminished coping skills to a variety of stressors, particularly regarding new experiences and surroundings, unfamiliar people, disruptions to routine behavior, anticipation of treatment, excess stimulation, and separation of objects that provide solace and familiarity (Table II). Various sensory hypersensitivities (visual, aural, olfactory, touch) may also impede the implementation of healthcare measures.
Self-stimulatory behavior, often initiated to alleviate extreme anxiety, may serve as a coping mechanism to counteract an overwhelming sensory environment.8-11 This may be observed as various repetitive actions (stimming) and may include hand-flapping, rocking, body spinning, obsessive handling of an object, and echolalia (repetitive and meaningless language).12 Patients with ASD may exhibit aggressive behavior, have a tendency for self-injury, and may resist establishing eye contact. Positive predictors for cooperation with autistic individuals take into consideration their reliance on nonverbal communication, minimal use and comprehension of language, and their inability to read and follow multistep instructions.
Sensory processing impairment. Sensory processing refers to actions in the CNS that determine interpretation of feedback from the body and environment.9 Atypical hyper- or hyposensitivities may be associated with ASD. Determining whether the patient is a hypo-responder (one who seeks sensory input) or a hyper-responder (one who avoids sensory input) is important when strategizing guidance techniques. Sensory defensiveness, a consequence of over-responsivity in individuals with a low threshold to sensations, may lead to averting or overreacting to environmental stimuli. Individuals who experience tactile defensiveness when touched by others may demonstrate impulsive "flight or fight" behaviors, as opposed to the "fight or flight" seen in a typical physiologic response, in addition to emotional outbursts, anxiety, anger, and self-injury (head banging).13 Observation of the patient's body language is critical in assessing their comfort. Early signs of distress include gaze avoidance, severe gagging or vomiting. Other avoidance actions include withdrawal, cowering, hiding, crying, and blocking the stimuli (covering ears or eyes).
Comorbid conditions. ASD is associated with a diversity of comorbidities, most notably epilepsy and sleep disturbances.12,14,15 For individuals who experience seizure activity, it is important to determine the specific type, existence and manifestation of a prodrome, seizure frequency and most recent episode. An estimated 86% of children diagnosed with ASD experience sleep deprivation almost daily.15 Disrupted and insufficient sleep may negatively affect daytime behavior, leading to lethargy, irritability, or poor coping skills. ASD is also associated with increased incidences of anxiety, depression, obsessive-compulsive disorder, psychosis, gastrointestinal disturbances, immune compromise, substance abuse, eating disorders, and oppositional behavior.5 Moreover, commonly prescribed medications for management of anxiety and stereotypic ASD-related behaviors (antipsychotics, antidepressants, anticonvulsants) may increase the risk for serious allergic reactions such as angioedema leading to swelling of the tongue and throat.16 Additional oral side effects include xerostomia and the subsequent risk for dental caries and periodontal disease.16
Clinical management techniques for patients with ASD
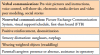
Due to social and communication impairments, individuals with ASD are often less able to respond appropriately to directions, prompting the basic guidance techniques outlined in Table III. In order to decrease patient anxiety and negative behavior, efforts should be undertaken to gain successful conveyance of information and instructions by providing anticipated and simplified multistep activities to address the patient's desires, feelings and preferences.11,17
The individual's unique communication challenges will determine the type and extent of information interchange. Healthcare practitioners should ask the parent/caregiver about any useful words or phrases for improving communication and consider use of pre-visit pictures, instructions, voice control, and tell-show-do. Another helpful method is the utilization of social stories (personalized, easy short narrations and illustrations) to simplify comprehension and preparation of appropriate responses to specific situations or events. When an individual is particularly apprehensive or uncooperative, holding personal comfort objects such as a favored toy or stuffed animal, squishy or squeeze ball may be consoling. One should also carefully weigh the consequences of separating these items from the patient. Some individuals may be calmed by allowing the use of an electronic screen media device to watch or listen to favorite video games and movies. It is also advantageous to ask the parent/caregiver regarding any stereotypic manifestations such as, "what type of behavioral problems does the patient have and how have you handled the situation?"
Video peer modeling (viewing a procedure on a video) and visual supports may be useful to explain anticipated behavior with a specific activity. Visual supports, substitute words and phrases with pictures and symbols, as exemplified by the Picture Exchange Communication System, visual schedules, and social stories. The Picture Exchange Communication System facilitates communication through pictures for individuals with minimal or no verbal capabilities. This method is widely used in the home and classroom and may be modified by using pictures with phrases to build visual schedules for patients with ASD. Visual scheduling is a systematic technique to improve learning and communication, particularly for incomprehensible language or echolalia.11 Social stories are typically individualized short narrations and illustrations written in a child's perspective to prepare appropriate responses to specific situations or events.
Positive reinforcement is important to promote the repetition of desired outcomes. Verbal reinforcers (rewards) may include positive voice modulation and appropriate physical demonstrations of praise. For example, communicating a direct response such as "Thank you for sitting still" is preferable to saying "Good job."
Nonverbal communication methods necessitate use of a visual support and schedule, sensory distraction (redirecting attention), and relying on the assistance of the parent/caregiver. To increase patient comprehension and compliance of planned activities, it may be helpful to use the first-then board (FTB) method, a fundamental language base that visually provides step-by-step instructions and sequencing of upcoming events.17 The "first" picture is characteristically a skill-building activity that the OHCP would want an individual to perform whereas the "then" activity symbolizes an exchange for patient compliance, leading to a reward.
Hypo-responders may be comforted by swaddling or by applying deep pressure to the chest and abdomen.9,10 Individuals who are hyper-responders may be overly sensitive to bright light, certain sounds or loud noise, touch, pressure, texture, taste, smell, and proprioceptive body movement.9,12,13,18,19 Desensitization gradually acquaints an anxious individual with aspects of a perceived unpleasant stimulus (object or place) to diminish emotional responsiveness.20
Dental radiographic management techniques
Preparation for the dental visit. Prior to the dental appointment, the OHCP should seek parent/caregiver input to consider the best approach to affect the patient's ability to self-regulate and adapt to change, sit or stand for a predetermined length of time, tolerate others touching their mouth with gloved hands, and follow a simple instruction. At the start of the dental visit, OHCP should assess the patient's anxiety level and ability to cope, and anticipate whether there may be challenges to the overall dental visit, particularly taking radiographs. Individuals with ASD have a strong need for continuity, as even small changes in routine may easily provoke undesirable behavior.23 Other impediments to dental care include hyperactivity and resistive movements. Early recognition of stereotypic behaviors and an individual's potential triggers may lessen protest behaviors such as crying, refusing to open the mouth, and aggression, any of which are usually consequent to fear and the need for self-protection.
Dental management should incorporate basic clinical techniques with modification strategies specifically relevant to the desired task (Table IV). Patients who have been uncooperative or overwhelmed by the dental experience may benefit from desensitization as a pre-visit activity. An example of a desensitization activity would be a "radiographic practice kit" for home use containing a disposable receptor holder. The patient could rehearse holding the receptor in their mouth while the parent/caregiver counts aloud as a distractor or use a sand or liquid motion timer as a visual incentive to denote the time interval of the practice and actual radiographic activity. Visually, the liquid timer may also have a calming effect.
Patients may be comforted by applying one or two weighted blankets or radiographic aprons on their chest and abdomen. Sunglasses should be available for patients affected with photosensitivity from operatory lighting. Auditory sensory processing impairments are also common with ASD. Creating a calm, quiet environment is important to those patients who have an intolerance to loud or shrill noises; intermittent sounds, such as bells or timers, may be distressing or even painful. Soft foam earplugs may ameliorate the high-pitched sound arising from panoramic devices. Occlusal and lateral jaw projections have a shorter exposure time and no automated moving parts and may serve as a suitable alternative. Motion of the panoramic receptor and x-ray source might be distracting and trigger an abrupt change in patient behavior.
Recently, handheld dental x-ray devices have gained in availability and usage. They offer increased portability and are specifically designed to allow the operator to remain chairside during the taking of radiographs on fearful or challenging patients. State laws may vary individually and OHCP would be advised to check their own regulatory agencies regarding permissibility and standards.21
On subsequent dental appointments, the risk of overwhelming patients with ASD may be reduced by maintaining similarity, scheduling them with the same OHCP on the same day, operatory, and dental chair.23
Visual schedule. Use of a visual schedule provides instructions to follow during a radiographic procedure and might include pictorials of the patient wearing a radiographic apron, placing hands on their stomach, opening their mouth, biting on a bite block, and listening to the sound of the "beep" emitted from the x-ray source. Inclusion of the FTB method may also motivate the patient to cooperate with these activities. To improve understanding, it may be helpful to show the patient an illustration of a visual schedule. An example is "first" sitting in the dental chair draped with a radiographic apron, and "then" play video games (Figure 1A and Figure 1B).
Visual incentives. Many individuals with ASD have an inherent preference for visual stimuli.16 Use of portable electronic screen media for communication and visual teaching may serve as a distractor to improve coping skills and reduce the fear of the radiographic examination, minimizing patient movement for improved image quality and ensuring patient safety.22
Social stories. Use of a social story may be helpful to communicate the desired tasks needed to conduct the radiographic examination. Social stories may be facilitated by using pictures and narratives such as "when I go to the dentist I will sit in a big chair that goes up and down," "keep my hands on my stomach," "sit quiet in a chair," "open my mouth wide for the hygienist or dentist to look at my teeth," "bite down on the toy block" (radiographic receptor holder), "get a prize when I am all done," "say goodbye," and "go home."
Advanced behavior guidance
The American Academy of Pediatric Dentistry has recognized clinical circumstances when a dental radiographic examination may be indicated but a diagnostic image may not be readily obtainable.24 Patient noncompliance may be attributable to fear, excessive anxiety, hyperactivity, repetitive behavior, physical disability, anatomic malformation, lack of comprehension of the requested task, or sensory hypersensitivity.12,19,25-28 When utilization of basic behavioral guidance techniques has been unsatisfactory, pharmacologic intervention may be necessary including the use of nitrous oxide/oxygen analgesia, anxiolysis, sedation and general anesthesia.24,29 In select cases, protective stabilization with physical restraints may be considered however this practice remains controversial or objectionable.24,30
Oral and maxillofacial impediments. A variety of oral anomalous features may pose challenges with radiographic examinations on patients with ASD including macroglossia, impaired tongue function, mouth breathing, drooling, malocclusion (high-arched palate, maxillary overjet), and hyper-gag reflex. Para-functional habits (bruxism, tongue thrusting, nonnutritive chewing) and atypical oral habits (mouthing, chinning, biting others, self-biting) also occur in this population and may potentiate the need for behavioral management strategies.12
Mouthing, the habitual manipulation of non-food items in the mouth, may result in fractured or mobile teeth, posing a problem biting on the radiographic bite block or receptor holder. Chinning refers to an individual's tendency to press the chin into an object or person's extremity, often resulting in increased pressure to the mandible to relieve the symptoms of exfoliating teeth, gingival inflammation, or dental caries. Another concern with treating patients with ASD, particularly those that are poor communicators, is the increased risk of the OHCP being bitten.12
Conclusion
Oral healthcare providers will be faced with an array of clinical challenges in providing comprehensive care for the growing number of individuals with ASD, particularly in the acquisition of dental radiographs. Unique patient needs, communication barriers, and atypical sensory issues along with appropriate behavioral techniques must be taken into consideration for successful patient outcomes with radiographic imaging. Anticipation of the patient's level of cooperation prior to acquiring dental radiographs should include an assessment by the dental hygienist and other dental staff members. Modification of radiographic techniques with patients with ASD may reduce stressors and increase cooperation resulting in diagnostically adequate imaging and improved clinical outcomes.
About the Authors
Jacqueline C. Dailey, RDH, MS is a clinical assistant professor, John K. Brooks, DDS is a clinical professor; both in the Department of Oncology and Diagnostic Sciences, University of Maryland School of Dentistry, Baltimore, MD.
Corresponding author: Jacqueline C. Dailey, RDH, MS; jdailey@umaryland.edu
References
1. Rapin I, Tuchman RF. Autism: definition, neurobiology, screening, diagnosis. Pediatr Clin North Am. 2008 Oct;55(5):1129-46.
2. Lord C, Elsabbagh M, Baird G, Veenstra-Vanderweele J. Autism spectrum disorder. Lancet 2018 Aug;392(10146):508-20.
3. de Giambattista C, Ventura P, Trerotoli P, et al. Subtyping the autism spectrum disorder: comparison of children with high functioning autism and Asperger syndrome. J Autism Dec Disord 2019 Jan;49(1):138-50.
4. Christensen DL, Maenner MJ, Bilder D, et al. Prevalence and characteristics of autism spectrum disorder among children aged 4 years - Early autism and developmental disabilities monitoring network, seven sites, United States, 2010, 2012, and 2014. MMWR Surveill Summ 2019 Apr;68(2):1-19.
5. Lai MC, Lombardo MV, Baron-Cohen S. Autism. Lancet 2014 Mar;383(9920):896-910.
6. Chaste P, Leboyer M. Autism risk factors: genes, environment, and gene-environment interactions. Diaglogues Clin Neurosci. 2012 Sep;14(3):281-92.
7. Lowe O, Lindemann R. Assessment of the autistic patient's dental needs and ability to undergo dental examination. ASDC J Dent Child.1985 Jan-Feb;52(1):29-35.
8. Lai B, Milano M, Roberts MW, Hooper SR. Unmet dental needs and barriers to dental care among children with autism spectrum disorders. J Autism Dev Disord. 2012 Jul;42(7):1294-303.
9. Kuhaneck HM, Chisholm EC. Improving dental visits for individuals with autism spectrum disorders through an understanding of sensory processing. Spec Care Dentist. 2012 Nov-Dec;32(6):229-33.
10. Delli K, Reichart PA, Bornstein MM, Livas C. Management of children with autism spectrum disorder in the dental setting: concerns, behavioural approaches and recommendations. Med Oral Pathol Oral Cir Bucal. 2013 Nov;18(6):e862-e8.
11. Zink AG, Diniz MB, Rodrigues dos Sanantos MT, Guaré RO. Use of a picture exchange communication system for preventive procedures in individuals with autism spectrum disorder: pilot study. Spec Care Dentist. 2016 Sep;36(5):254-9.
12. Green D, Flanagan D. Understanding the autistic dental patient. Gen Dent. 2008 Mar-Apr;56(2):167-71.
13. Stein Ll, Polido JC, Mailloux Z, et al. Oral care and sensory sensitivities in children with autism spectrum disorders. Spec Care Dentist. 2011 May-Jun;31(3):102-10.
14. Hara H. Autism and epilepsy: a retrospective follow-up study. Brain Dev. 2007 Sep;29(8):486-90.
15. DeVincent CJ, Gadow KD, Delosh D, Geller L. Sleep disturbance and its relation to DSM-IV psychiatric symptoms in preschool-age children with pervasive developmental disorder and community controls. J Child Neurol. 2007 Feb;22(2):161-9.
16. Chandrashekhar S, S Bommangoudar J. Management of autistic patients in dental office: a clinical update. Int J Clin Pediatr Dent. 2018 May-Jun;11(3):219-27.
17. Chebuhar A, McCarthy AM, Bosch J, Baker S. Using picture schedules in medical settings for patients with an autism spectrum disorder. J Pediatr Nurs. 2013 Apr;28(2):125-34.
18. Stein Ll, Polido JC, Cermak SA. Oral care and sensory over-responsivity in children with autism spectrum disorders. Pediatr Dent. 2013 May-Jun;35(3):230-5.
19. Marshall J, Sheller B, Williams BJ, et al. Cooperation predictors for dental patients with autism. Pediatr Dent. 2007 Sep-Oct;29(5):369-76.
20. Nelson T, Chim A, Sheller BL, et al. Predicting successful dental examinations for children with autism spectrum disorder in the context of a dental desensitization program. J Am Dent Assoc. 2017 Jul;148(7):485-92.
21. Berkhout WE, Suomalainen A, Brüllmann D, et al. Justification and good practice in using handheld portable dental X-ray equipment: a position paper prepared by the European Academy of DentoMaxilloFacial Radiology (EADMFR). Dentomaxillofac Radiol. 2015 Feb;44(6):20140343.
22. Isong IA, Rao SR, Holifield C, et al. Addressing dental fear in children with autism spectrum disorders: a randomized controlled pilot study using electric screen media. Clin Pediatr (Phila). 2014 Mar;53(3):230-7.
23. Klein U, Nowak AJ. Characteristics of patients with autistic disorder (AD) presenting for dental treatment: a survey and chart review. Spec Care Dentist.1999 Sep- Oct;19(5):200-7.
24. American Academy of Pediatric Dentistry. Guideline on behavior guidance for the pediatric dental patient. Pediatr Dent. 2016 Oct;38(6):185-98.
25. Maskey M, Warnell F, Parr JR, et al. Emotional and behavioural problems in children with autism spectrum disorder. J Autism Dev Disord. 2013 Apr;43(4):851-9.
26. Barry S, O'Sullivan EA, Toumba KJ. Barriers to dental care for children with autism spectrum disorder. Eur Arch Paediatr Dent. 2014 Apr;15(2):127-34.
27. Limeres-Posse J, Castano-Novaa P, Abeleira-Pazos M, Ramos-Barbosa I. Behavioural aspects of patients with autism spectrum disorders (ASD) that affect their dental management. Med Oral Patol Oral Cir Bucal. 2014 Sep;19(5):e467-72.
28. Gandhi RP, Klein U. Autism spectrum disorders: an update on oral health management. J Evid Based Dent Pract. 2014 Jun;14 Suppl:115-26.
29. Loo CY, Graham RM, Hughes CV. Behaviour guidance in dental treatment of patients with autism spectrum disorder. Int J Paediatr Dent. 2009 Nov;19(6):390-8.
30. Capozza LE, Bimstein E. Preferences of parents of children with autism spectrum disorders concerning oral health and dental treatment. Pediatr Dent. 2012 Nov- Dec;34(7):480-4.