You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Many techniques and protocols are available to clinicians for the extraction of failing teeth and replacement with implant-supported restorations. However, identifying predictable treatment options in various clinical situations can be challenging. Extraction socket classifications and treatment protocols are designed to help guide clinicians through diagnosis and therapy. This article aims to present a straightforward, yet thorough, classification for the extraction sockets of single-rooted teeth while providing a roadmap to assist clinicians in selecting appropriate and predictable treatment. The proposed classification is unique in its scope, design, and foundation in wound healing.
This classification of extraction sockets focuses on the bone topography of the extraction socket, while the protocol for treatment of each socket type is based on the biologic foundations of wound healing. The protocol takes into account the shape of the remaining bone, the biotype, and the location of the socket whether it be in the mandible or maxilla. First, an overview of fundamentals that led to this classification and treatment protocol will be presented, then a description of the socket classifications and treatment protocol for each socket type is discussed (Figure 1).
Background
The basis of this classification is the hard tissue, as the presence and shape of the bone remaining after an extraction determines the foundational aspects of treatment. The bone topography of a socket determines the timing of implant placement and dictates the type of grafting techniques that may be needed, whether grafting in conjunction with implant placement, site preservation, or ridge augmentation. The bone topography of an extraction socket comprises the shape, contour, and 3-dimensional structure of the bone remaining following tooth extraction. It is determined by the shape of the alveolus apical to the extraction site, the level of interproximal bone, and the height, thickness, and quality of the buccal plate. Each of these aspects of the hard tissue affects the socket healing and treatment outcome, and these effects were considered when establishing this classification.
Bone Presence and Quality
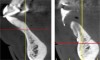
The shape and amount of bone present apical to the extraction socket is the apical topography and is important in treatment planning for both immediate and delayed implant placement. For immediate implant placement, the apical topography is significant, as 3 mm to 4 mm of native bone needs to be engaged for primary stability of the implant.1,2 If planning a 2-stage approach with site preservation and delayed implant placement, analysis of the apical topography is also essential. If a tooth with an apical concavity is extracted and a graft is placed only inside the socket, there may not be adequate bone following healing to place the implant in the proper position without additional surgical procedures3 (Figure 2). Teeth that do not have enough apical bone to provide the housing necessary for immediate implant placement or delayed implant placement with grafting inside the socket alone are defined as having inadequate apical topography. This inadequacy can be the result of periapical pathologies or the anatomy of the alveolus.
Interproximal bone levels influence the healing of the socket and the support of the interproximal soft tissue following implant placement. The presence or absence of papilla between an implant and a natural tooth is dependent on the level of interproximal bone. Therefore, the height of the interproximal bone plays a significant role in the final esthetic outcome when replacing a failing tooth with an implant-supported restoration.4,5
The interproximal bone affects the healing of an extraction socket, because this bone along with the buccal and lingual bone makes up the walls of a socket. After tooth extraction, a blood clot will form within the confines of the extraction socket walls; this blood clot will serve as the scaffold for bone formation, turning into woven and, then eventually, mature trabecular bone.6 As the interproximal, lingual, and buccal bone all support the initial blood clot, their height affects the dimension of the blood clot and, therefore, impacts the final bone morphology.
The quality of the bony walls present also affects the socket’s healing and, therefore, influences the morphology of the healed site. When the quality of the buccal plate is poor due to its being thin, made mostly of cortical bone, or dehisced, it is more likely to resorb and result in greater dimensional changes following socket healing.7 The dimensional changes that occur after tooth extraction related to the height and quality of the socket walls can be reduced through socket grafting or compensated for with the use of guided bone regeneration (GBR) simultaneous to tooth extraction.8,9 Grafting at the time of implant placement may also correct buccal plate loss; however, careful analysis of the quantity and quality of residual buccal plate must be made to achieve reproducible success.10,11
Principles of Periodontal Defect Repair
In this protocol, the principles observed in periodontal defect repair have been applied to extraction sockets. This is possible because of the similarities between sockets and periodontal defects: in both, the wound heals from the walls and continues to the center6; also, a completely intact socket is essentially a 4-wall defect within the alveolus, while a socket that is missing half of a buccal plate can be regarded as a three-and-a-half–wall defect, and one with no buccal plate can be considered a 3-wall defect. With periodontal defects, as the number and quality of bony walls decrease, so does the predictability of regeneration; therefore, each socket must be examined because the width of the defect, the number of walls, and the quality of the bone around it all impact the potential for regeneration.12-14 The authors have considered the variations in sockets that are possible following single-rooted tooth extraction and have divided these possibilities into 3 groups. The treatment protocol for each group considers the predictability of regeneration based on the principles of wound healing and tissue regeneration.
When grafting is indicated, the choice of bone-graft material is left to the clinician’s preference. When a ridge-augmentation style of grafting is required, it is suggested that the principles of space maintenance, cell occlusion, and primary closure that allow for successful bone formation are followed.15,16 Note that performing ridge augmentation simultaneous to extraction with primary closure may cause disharmony in the mucogingival junction. These soft-tissue discrepancies can be corrected through soft-tissue repositioning or manipulation at the time of implant uncovery.
Thin vs. Thick Biotypes
The characteristics and quality of the soft tissue have a major impact on the final esthetic and treatment outcome, and, therefore, a patient’s biotype must be taken into account when performing tooth replacement with an implant-supported restoration. The biotype, which can be characterized as thick or thin, influences both how the soft tissue lays over the osseous structure and how it reacts to surgical handling. Compared with thin biotypes, thicker biotypes are more forgiving to surgical treatments such as tooth replacement with an implant-supported restoration. This forgiving nature is evident in the following characteristics: thicker biotypes are less likely to have tissue discoloration due to implant-body show-through, thick biotypes can achieve papilla fill with a greater distance from osseous crest to contact, thick biotypes have greater peri-implant mucosal dimensions, and they are not prone to the same recession suffered by their thin counterparts when subjected to surgical manipulation and mechanical injury.4,17-21
Thus, thick and thin biotype tissues need to be handled differently to achieve the same esthetic result. Thin biotypes need more support to attain the same contour as thick biotypes and require a more conservative treatment approach because of their susceptibility to recession. Hence, a biotype’s effect on esthetic outcome and its ability to tolerate surgical insult and injury were heavily weighed when this treatment protocol was created.
Atraumatic Flapless Technique
In all cases, treatment begins with atraumatic flapless extraction of the hopeless tooth, evaluation of the remaining osseous structure, apical topography, and interproximal bone, and identification of the biotype. Analysis of the bony topography should be done preoperatively through examination of radiographs and cone-beam computed tomography (CBCT) imaging and confirmed clinically following extractions. Atraumatic extraction technique is used to conserve as much of the surrounding hard and soft tissue as possible, and a flapless technique is utilized to maintain the blood supply between gingiva and the buccal plate, minimizing resorption.22 Once the extraction socket is classified and the biotype is identified, the presented protocol can be followed.
In specific cases of deficient bone and soft tissue, a clinician may choose to alter and enhance the bony topography and soft-tissue contour through orthodontic extrusion prior to extraction. Evaluation and classification of the site and choice of protocol should be made following completion of orthodontic treatment because of the ensuing changes in bone level and soft-tissue contour.23,24 The foresight provided to clinicians by observing these noted aspects of an extraction socket’s topography, through the use of the presented classification, will help lead to an appropriate treatment that is based on the biologic foundations of wound healing.
Classification and Treatment Protocol
Imagery depicting examples of single-rooted sockets showing periodontium status, socket conditions, and CBCT imaging is presented in Figure 2 through Figure 5.
Grade I
Grade I sockets are the most ideal. Following tooth extraction, a socket that has an intact buccal plate, adequate interproximal bone, and satisfactory apical topography will fall into this category. In this classification, an intact buccal plate is defined as having no fissures or dehiscences and less than 25% loss of height (Figure 4, left; Figure 5, left). This percentage of buccal plate loss was selected as the cutoff based on the average root length of single-rooted teeth, which is 14.2 mm,25 and the amount of buccal plate that can be reliably regenerated during immediate implant placement. Adequate apical topography is defined as enough bone present apical to the extraction site to allow for engagement of 3 mm to 4 mm of a properly positioned immediate dental implant (Figure 2).1,2 Adequate interproximal bone is defined as no or mild (up to 2 mm) periodontal bone loss on the adjacent teeth as to allow for support of the interproximal soft tissue and to enable placement of the platform of an immediate implant in the proper apical-coronal position relative to the adjacent teeth while still being bordered by bony walls on the mesial and distal aspects26 (Figure 3, left).
Grade I extraction sockets are treated with immediate implant placement with or without provisionalization depending on implant stability and the remaining gap between the implant and socket walls to be grafted.
Grade II
Grade II sockets are differentiated from Grade I by the amount and quality of the remaining buccal plate. A Grade II socket has a fissure, dehiscence, or deficiency of the buccal plate totaling a 25% to 50% loss. Like Grade I sockets, they have adequate interproximal bone and apical topography (Figure 3, left; Figure 4, center; Figure 5, center).
For a patient with a thick biotype, an immediate implant can be placed in a Grade II extraction socket. The implant should not be temporized, and the remaining defect surrounding the implant should be grafted and contained by a barrier membrane. For a patient with a thin biotype, delayed implant placement with site preservation is recommended. If the extraction site is located in the maxilla, the rotated pedicle palatal connective-tissue flap technique should be used to enhance the thin soft-tissue profile and to allow for a more esthetic outcome following delayed implant placement.20 In this case, the location of the extraction site must be considered because if it is in the maxilla, keratinized tissue can easily be borrowed through rotated pedicle grafting to increase tissue.27 If the extraction socket is in the mandible, site preservation with delayed implant placement is recommended. This more conservative approach is recommended because of the characteristics of a thin biotype and its susceptibility to recession during surgical manipulation and mechanical injury.18,20 Discrepancies in the mucogingival line that may result from primary closure in the area of an extraction socket or any noted deficiencies in the soft tissue can be corrected during implant uncovery.
Grade III
Grade III sockets are the most deficient and include any socket with inadequate apical topography, insufficient interproximal bone, or more than 50% loss of buccal plate. Inadequate apical topography is defined as not enough bone present apical to the extraction site to allow for implant placement and may be the result of bone loss caused by periapical lesions or concavities due to existing anatomy of the alveolus (Figure 4, right; Figure 5, right). Insufficient interproximal bone is defined as moderate-to-severe periodontal bone loss—greater than 2 mm on one or both of the adjacent teeth.
Grade III sockets are further divided into those with inadequate apical topography and those that have interproximal bone loss with or without buccal plate loss. If the socket is Grade III due to inadequate apical topography, the extraction socket should be treated with a ridge-augmentation type of GBR to correct the inadequate apical topography and delayed implant placement.
In a Grade III extraction socket with adequate apical topography and interproximal bone loss regardless of biotype, the protocol will be the same as for a Grade II with thin biotype (Figure 1). Here again, delayed implant placement with site preservation is recommended. If the extraction site is located in the maxilla, the rotated pedicle palatal connective-tissue flap technique should be used; if the extraction socket is located in the mandible, site preservation with delayed implant placement is recommended.
In specific cases, a clinician may choose to use forced eruption as a means of correcting inadequacies in the interproximal bone. If forced eruption is employed, the socket should be reevaluated after completion of orthodontic treatment. Classification and selection of treatment protocol must be made following forced eruption because of the changes in the hard- and soft-tissue contours that can result.
Conclusion
A unique classification and treatment protocol for the extraction sockets of single-rooted teeth to be replaced by implants has been presented. This classification is based on the amount and quality of the buccal plate present, the level of interproximal bone, and the apical topography. The presented treatment protocol takes into consideration the bone topography of the extraction socket, the biotype, and the socket location. The percentages for buccal-plate loss that serve to distinguish the socket groups and the listed cutoff points to characterize interproximal bone loss are suggestions. Each case a clinician encounters is unique, and this classification system serves to divide a spectrum of possibilities into distinct groups to aid in the selection of a treatment protocol.
Other treatment options for the described situations can be successful, but the techniques advised here were chosen based on predictability and the biologic foundations of wound healing. Further analysis of bone levels prior to and following treatment as well as esthetic outcomes using the suggested protocol should be the aim of future studies. None of the techniques suggested are novel or unique; only the method of choosing when to employ them is.
About the Authors
Edgard El Chaar, DDS, MS
Clinical Associate Professor and Director
Postgraduate Periodontics
New York University College of Dentistry
New York, New York
Sarah Oshman, DMD
Postgraduate Periodontics
New York University College of Dentistry
New York, New York
Pooria Fallah Abed, DDS
Postgraduate Periodontics
New York University College of Dentistry
New York, New York
Queries to the authors regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Nemcovsky CE, Artzi Z, Moses O, Gelernter I. Healing of marginal defects at implants placed in fresh extraction sockets or after 4-6 weeks of healing. A comparative study. Clin Oral Implants Res. 2002;13(4):410-419.
2. Juodzbalys G. Instrument for extraction socket measurement in immediate implant installation. Clin Oral Implants Res. 2003;14(2):144-149.
3. Grunder U, Gracis S, Capelli M. Influence of the 3-D bone-to-implant relationship on esthetics. Int J Periodontics Restorative Dent. 2005;25(2):113-119.
4. Kan JY, Rungcharassaeng K, Umezu K, Kois JC. Dimensions of peri-implant mucosa: an evaluation of maxillary anterior single implants in humans. J Periodontol. 2003;74(4):557-562.
5. Salama H, Salama MA, Garber D, Adar P. The interproximal height of bone: a guidepost to predictable aesthetic strategies and soft tissue contours in anterior tooth replacement. Pract Periodontics Aesthet Dent. 1998;10(9):1131-1141.
6. Cardaropoli G, Araujo M, Lindhe J. Dynamics of bone tissue formation in tooth extraction sites. An experimental study in dogs. J Clin Periodontol. 2003;30(9):809-818.
7. Nevins M, Camelo M, De Paoli S, et al. A study of the fate of the buccal wall of extraction sockets of teeth with prominent roots. Int J Periodontics Restorative Dent. 2006;26(1):19-29.
8. Iasella JM, Greenwell H, Miller RL, et al. Ridge preservation with freeze-dried bone allograft and a collagen membrane compared to extraction alone for implant site development: a clinical and histologic study in humans. J Periodontol. 2003;74(7):990-999.
9. Vignoletti F, Matesanz P, Rodrigo D, et al. Surgical protocols for ridge preservation after tooth extraction. A systematic review. Clin Oral Implants Res. 2012;23 suppl 5:22-38.
10. Juodzbalys G, Wang HL. Soft and hard tissue assessment of immediate implant placement: a case series. Clin Oral Implants Res. 2007;18(2):237-243.
11. Ferrus J, Cecchinato D, Pjetursson EB, et al. Factors influencing ridge alterations following immediate implant placement into extraction sockets. Clin Oral Implants Res. 2010;21(1):22-29.
12. Kim CS, Choi SH, Chai JK, et al. Periodontal repair in surgically created intrabony defects in dogs: influence of the number of bone walls on healing response. J Periodontol. 2004;75(2):229-235.
13. Cortellini P, Tonetti M. Radiographic defect angle influences the outcome of GTR therapy in intrabony defects. J Dent Res. 1999;78:381.
14. Schenk RK, Buser D, Hardwick WR, Dahlin C. Healing pattern of bone regeneration in membrane-protected defects: a histologic study in the canine mandible. Int J Oral Maxillofac Implants. 1994;9(1):13-29.
15. Buser D, Dula K, Hirt HP, Schenk RK. Lateral ridge augmentation using autografts and barrier membranes: a clinical study with 40 partially edentulous patients. J Oral Maxillofac Surg. 1996;54(4):420-433.
16. von Arx T, Buser D. Horizontal ridge augmentation using autogenous block grafts and the guided bone regeneration technique with collagen membranes: a clinical study with 42 patients. Clin Oral Implants Res. 2006;17(4):359-366.
17. Kois JC. Predictable single tooth peri-implant esthetics: five diagnostic keys. Compend Contin Educ Dent. 2001;22(3):199-206.
18. Muller HP, Heinecke A, Schaller N, Eger T. Masticatory mucosa in subjects with different periodontal phenotypes. J Clin Periodontol. 2000;27(9):621-626.
19. Sanavi F, Weisgold AS, Rose LF. Biologic width and its relation to periodontal biotypes. J Esthet Dent. 1998;10(3):157-163.
20. Kois JC, Vakay RT. Relationship of the periodontium to impression procedures. Compend Contin Educ Dent. 2000;21(8):684-690.
21. Jansen CE, Weisgold A. Presurgical treatment planning for the anterior single-tooth implant restoration. Compend Contin Educ Dent. 1995;16(8):746-754.
22. Fickl S, Zuhr O, Wachtel H, et al. Tissue alterations after tooth extraction with and without surgical trauma: a volumetric study in the beagle dog. J Clin Periodontol. 2008;35(4):356-363.
23. Mantzikos T, Shamus I. Forced eruption and implant site development: an osteophysiologic response. Am J Orthod Dentofacial Orthop. 1999;115(5):583-591.
24. Ingber JS. Forced eruption: alteration of soft tissue cosmetic deformities. Int J Periodontics Restorative Dent. 1989;9(6):416-425.
25. Wheeler RC. A Textbook of Dental Anatomy and Physiology. Philadelphia, PA: WB Saunders; 1950.
26. Cooper LF, Raes F, Reside GJ, et al. Comparison of radiographic and clinical outcomes following immediate provisionalization of single-tooth dental implants placed in healed alveolar ridges and extraction sockets. Int J Oral Maxillofac Implants. 2010;25(6):1222-1232.
27. El Chaar ES. Soft tissue closure of grafted extraction sockets in the posterior maxilla: the rotated pedicle palatal connective tissue flap technique. Implant Dent. 2010;19(5):370-377.