You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
The comprehensive dental new patient examination has been elevated from a visual and tactile mirror/explorer and radiograph examination to a much more sophisticated assessment of the total oral cavity and airway space. Clinical dentists are using digital intraoral scanning, caries detection technology, and cone-beam computed tomography (CBCT) imaging to get a complete picture of a patient's oral condition.
Traditionally in dental school, many students were taught that a comprehensive examination for a new patient consisted of a visual examination, a tactile examination, and a full-mouth series of radiographs or a panoramic image and bitewings. Technology and improved diagnostics have made this traditional model almost obsolete. Similar to the way that restorative dentistry has changed from amalgam and porcelain-fused-to-metal crowns to minimally invasive restorations and strong ultrathin ceramics, diagnostics have moved from explorers and 2-dimensional (2D) radiographs to caries-detecting devices and CBCT scanning.
Offering advanced diagnostics will differentiate a modern, cutting-edge dental practice from traditional practices. Dentists face many challenges, with stagnant and decreasing insurance reimbursements, changing landscapes in practice management, increasing overheads, and now even direct-to-patient care. Patients are more informed and more demanding than ever before and have many choices when it comes to selecting their dental care. Incorporating technologies such as intraoral digital scanning, fluorescence and transillumination for caries detection, and CBCT technology elevates comprehensive diagnosis with increased information and increased patient acceptance.1,2
The Comprehensive Examination
Beginning each comprehensive examination with an intraoral digital scan records the complete visible condition of the dentition. CBCT allows dentists to gain a highly accurate 3D image of the patient's anatomy from a single scan so they can better diagnose and understand the true extent of dental disease. Traditional 2D radiographs for diagnosis and treatment planning typically require multiple images, and with them, multiple doses of radiation.
Another technological advancement has occurred with caries detection. Advanced caries detection diagnostic technology allows dental professionals to detect caries earlier and gives clinicians more information than they previously had access to with traditional methods.
The comprehensive examination includes assessing head and neck condition, occlusion, periodontal condition, temporomandibular joint (TMJ) health and function, airway functions, and dental hard-tissue condition. The process begins with proper communication from the front desk team when the patient makes the first appointment. It is important to convey that the first appointment is ultimately designed to gather information and to discuss concerns-it is not for a "cleaning." It will be centered entirely around the patient's needs, with a thorough assessment of the patient's condition and concerns. The following is a suggested sequence for a new patient visit with a comprehensive examination using today's technology:
1. Welcome and tour of office, introduction to team and treating doctor
2. Medical and dental history review
3. Visual assessment
4. Intraoral digital scan
5. Caries assessment with fluorescence and transillumination
6. Periodontal evaluation
7. 2D radiographs as needed
8. CBCT scan
9. Photographs for cosmetic concerns
After a tour of the office and introduction to the treating staff, the patient is seated and interviewed, and then medical and dental history are reviewed. The treating dentist then performs a visual assessment. Diagnostics are decided by the dentist-ie, radiographs, CBCT, or both. The dental assistant or dental hygienist records a digital intraoral scan. A team member then uses the caries detection technology, saving images of any positive findings. Next, a full periodontal chart is recorded. Radiographs and/or CBCT scans are taken. Digital photographs are taken. A digital smile mockup is performed if the patient has cosmetic concerns. Together, all information gathered gives the clinician the most complete diagnostic picture.
A Closer Look at Technology
Intraoral Scanning
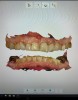
Records from the digital intraoral scan provide a complete picture of the hard tissue and existing restorations (Figure 1). Particularly worthy of mention is the versatile integration of digital impressions into diagnostic and treatment concepts to provide a customizable healthcare solution for the patient.3 Digital intraoral scans can be integrated into CBCT for implant planning and fully guided implant surgery. The digital intraoral scan can also be used to simulate orthodontic outcome and serial evaluation of orthodontic tooth movement.4 In fact, with optical impressions, patients feel more involved in their treatment and it becomes possible to establish more effective communication with them; this emotional involvement may have a positive impact on the overall treatment-for example, by improving patient compliance with oral hygiene. In addition, patients become interested in the technology and mention it to their acquaintances and friends, elevating their opinion of dental offices equipped with these modern technologies. Indirectly, intraoral scanning has become a powerful advertising and marketing tool.5
Fluorescence Caries Detection
Sharp explorers and radiographs have been the primary means of caries detection for many years. However, both tactile inspection and radiographs have limitations. Caries must become deep enough or large enough to be "seen" by the tip of the explorer or radiographically. Lesions, especially interproximal, typically advance so far that by the time they are visible on radiographs, they require restorative intervention.6,7
Fluorescence caries detection technology uses light that measures reflective differences between healthy tooth structure and demineralized tooth structure. The reflected light is analyzed by stage of caries progression and represented by color and number. Caries-producing bacteria will show as red; healthy enamel displays as green. Florescence technology provides a means for diagnosing early demineralization to deep decay in pits and fissures and on smooth surfaces and calibrating it by number.
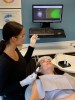
Interproximally, an infrared light beam can be used (Figure 2). Carious lesions absorb infrared light. Healthy tooth structure reflects the infrared light and appears transparent. Interproximal lesions can be diagnosed without ionizing radiation, and depth can be assessed. When demineralization is recognized at earlier stages in pits and fissures, smooth surfaces, and interproximally, the clinician can treat more conservatively and with minimally invasive techniques. Conserving tooth structure is better for the long-term dental health of the patient. Additionally, recent studies using light-microscopy have found that using a sharp dental probe for occlusal caries detection causes enamel defects, leading to the conclusion that dental explorer probing should not be considered as an appropriate procedure.8
Cone-Beam Computed Tomography
CBCT is a radiographic imaging method that allows accurate 3D imaging of hard-tissue structures. CBCT is capable of providing sub-millimeter resolution (2-line pair/mm) images of higher diagnostic quality, with shorter scanning times (~60 s). Radiation exposure dose from CBCT is 10 times less than from conventional CT scans during maxillofacial exposure (68 µSv compared with 600 µSv of conventional CT),1 and CBCT also has optimal dimensional accuracy (only about 2% magnification). Increasing availability of this technology now provides the dental clinician with an imaging modality that is capable of generating a 3D representation of the maxillofacial structures with minimal distortion and reduced radiation hazards.9
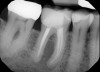
CBCT technology can be used for 3D location of jaw pathologies, to assess impacted teeth and supernumerary teeth, to assess the relation of the teeth to vital structures, to assess changes in the cortical and trabecular bone in cases of bisphosphonate-associated necrosis of the jaws, and to evaluate bone grafts. CBCT is also used to investigate the pathologies related to paranasal sinuses and to assess obstructive sleep apnea. CBCT technology also can be used to access endodontic lesions, root fractures, and resorption lesions (Figure 3 and Figure 4).10
Additionally, CBCT can be used to accurately assess periodontal condition, bone loss, and pathology. CBCT is a highly effective tool to define the true position of the condyle in the fossa, thereby revealing the possibility of dislocation of the disc in the joint and the extent of translation of the condyle in the fossa.8
CBCT technology is increasingly more affordable; therefore, more dental practices are able to incorporate this technology into general practice. Diagnostic information and treatment possibilities are enhanced with CBCT. As with any radiation exposure, risk versus benefit to the patient should be considered before using CBCT. CBCT can be indicated where 2D images are not sufficient or where technology such as guided surgery will improve patient management and restorative outcome.
Conclusion
After all the diagnostic information has been gathered, a full treatment plan can be formulated and presented to the patient. Not only does technology provide the dentist with complete information, it also empowers the patient to make informed decisions about his or her care.
About the Author
Susan McMahon DMD, AAACD
Private Practice
Pittsburgh, Pennsylvania
References
1. Muchhal M, Niraj LK, Chaudhary D, et al. Spanning the horizon of accuracy of different intraoral radiographic modalities: a systematic review. J Contemp Dent Pract. 2017;18(12):1206-1212.
2. Mansour S, Ajdaharian J, Nabelsi T, et al. Comparison of caries diagnostic modalities: a clinical study in 40 subjects. Lasers Surg Med. 2016;48(10):924-928.
3. Zimmermann M, Mehl A, Mörmann WH, Reich S. Intraoral scanning systems - a current overview. Int J Comput Dent.2015;18(2):101-129.
4. Yun D, Choi DS, Jang I, Cha BK. Clinical application of an intraoral scanner for serial evaluation of orthodontic tooth movement: a preliminary study. Korean J Orthod. 2018;48(4):262-267.
5. Mangano F, Gandolfi A, Luongo G, Logozzo S. Intraoral scanners in dentistry: a review of the current literature. BMC Oral Health. 2017;17(1):149.
6. Berg JH. Minimal intervention: motivating patients through caries risk assessment. Compend Contin Educ Dent. 2007;28(3):162,164.
7. Bozdemir E, Aktan AM, Ozsevik A, et al. Comparison of different caries detectors for approximal caries detection. J Dent Sci. 2016;11(3):293-298.
8. Kuhnisch J, Dietz W, Stosser L, et al. Effects of dental probing on occlusal surfaces--a scanning electron microscopy evaluation. Caries Res. 2007;41(1):43-48.
9. Kumar M, Shanavas M, Sidappa A, Kiran M. Cone-beam computed tomography - know its secrets. J Int Oral Health.2015;7(2):64-68.
10. Alamri HM, Sadrameli M, Alshalhoob M, et al. Applications of CBCT in dental practice: a review of the literature. Gen Dent. 2012;60(5):390-400.