You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
CAMBRA (Caries Management by Risk Assessment) was introduced in the Journal of the California Dental Association1 in 2007, and recommendations for office protocols have been subsequently introduced.2 Many risk factors contribute to the development of dental caries.3,4 Some risk factors may mildly increase one’s risk, while some present an imminent risk. It is crucial to identify which risk factors are present, and having an understanding of how risk factors contribute to the disease process is highly useful to the practitioner.
Historically, it was understood that for caries to occur, a tooth, a fermentable carbohydrate, and bacteria must to be present.5 Recent research suggests that although this supposition is correct, as carbohydrates are metabolized by bacteria, the decrease in the pH will greatly contribute to the caries process.6
pH and Dental Caries
Marsh7 proposed the Ecological Plaque Hypothesis, which is a hybrid of the Non-specific and Specific Plaque Hypotheses.8 He stated that cariogenic bacteria may occur naturally in dental plaque. In the presence of a low pH, these potentially cariogenic bacteria become increasingly competitive. It is prudent for the dental practitioner to keep in mind that in health, the elements for disease (carbohydrate metabolism by potentially cariogenic bacteria) are continually present. Disease occurs when the environment shifts to facilitate the disease process. These environmental shifts are implications of an oral cavity with a low pH for a prolonged period of time and increased numbers of acidogenic bacteria. The increased acid due to the increased numbers of acid-producing bacteria will lead to demineralization and caries. Many risk factors predispose the oral cavity to increased levels of bacteria and a prolonged oral environment with a low pH.6
Caries Risk Assessment
Risk Assessment and Documentation
There are several risk assessment questionnaires available. These questionnaires are generally reviewed with the patient, who is subsequently assigned to a caries risk category.9 A simplified alternative to the risk assessment document is to assess a patient’s medial history, medications, habits, oral hygiene practices, and clinical presentation, and document the findings into the clinical record.10 Some factors contribute to a patient’s overall caries risk but do not place the patient at immediate risk. These factors include: diet high in fermentable carbohydrates, gingival recession, poor oral hygiene, deep pits and fissures (occlusal anatomy), and growing up without access to fluoride. Conversely, there are other risk factors that place a patient at an immediate risk for developing new dental caries. These include: xerostomia (including low salivary flow and/or poor quality of saliva), caries within 3 years, presence of incipient caries or demineralization, patients undergoing orthodontic treatment, recreational drug use, extensive restorations, removable partial dentures, fixed partial dentures, smoking, and direct contact with people with infectious bacteria (Table 1).
Adjuncts for Determining Caries Risk
Practitioners may utilize adjunctive tools for aiding in determining caries risk. These include: salivary flow tests,4 caries bacterial activity tests, pH tests,11 and plaque-disclosing agents. These tools not only aid the practitioner determine caries risk, but they may also motivate patients to improve their dietary habits, oral hygiene practices, or product choices to create an oral environment that is less favorable for the formation or progression of dental caries.
Caries Risk Factors
Medical Conditions and Medications
There are numerous medical conditions that contribute to one’s caries risk. The impact of the patient’s medical history on dentistry is extraordinarily important; however, the impact of dental health on a patient’s systemic health must also be considered. Many systemic conditions and medications can increase a patient’s risk for tooth decay. Conversely, research has discovered that cariogenic bacteria has a role in systemic disease, specifically upper respiratory infections, pneumonia,12 and cardiovascular disease.13
Many systemic conditions or their treatment cause low salivary flow, which leads to xerostomia, which greatly increases one’s risk for caries. Systemic conditions that lead to xerostomia include: diabetes mellitus, hypertension, anxiety, depression, Sjögrens syndrome, systemic lupus erythematosus, rheumatoid arthritis, bells palsy, scleroderma, and HIV. Many treatments will additionally lead to xerostomia, including, but not limited to, medications, chemotherapy, or radiation therapy.14 Additionally, digestive disorders such as helicobacter pylori,15 uncontrolled acid reflux,16 and the eating disorder bulimia nervosa17 greatly lower oral pH or erode the enamel surface, exposing dentin. Prolonged exposure to an acidic oral environment will allow cariogenic bacteria to thrive and will increase risk for demineralization or caries. Dentin is less resistant than enamel to the acid insult of cariogenic bacteria, and exposed dentin is more likely to develop caries than intact enamel.
More than 400 medications list xerostomia as a side effect. When a patient is on multiple medications, the severity of xerostomia increases exponentially. In 2003, Cassolato and Turnbull stated that the following medications reduce the output of the salivary glands due to the inhibition of signaling pathways: antipsychotics, tricyclic antidepressants, selective serotonin reuptake inhibitors, antihypertensives, sedatives, and antihistamines.18 It is worthwhile for the dental practitioner to investigate the side effects of any medication a patient is taking, as it often impacts dental treatment or predisposes the patient to have dental caries secondary to xerostomia.
Clinical Considerations for Minimization of Caries Risk
• A thorough medical history and an update of the patient’s health history, including medications or recreational drug use at each appointment: Exploring for the presence of potential side effects of prescribed, recreational, and over-the-counter medications will aid the practitioner in evaluating whether the use of medication is a contributing factor in caries risk.
• Evaluation of caries risk at each recare appointment: This is necessary because a patient’s medical history or list of prescribed medications may change between visits, which may result in changes in the patient’s caries risk classification.
Xerostomia
A patient’s subjective recognition of xerostomia may not be reliable. This condition may be a gradual process and go unnoticed for some patients, while others may experience a significantly diminished quality of life due to the discomfort of severe xerostomia. To counteract the discomfort, many patients opt for sugary candies, drinks, or snacks in an attempt to stimulate salivation. When a patient ingests food or a beverage with an acidic pH, the result is an acidic oral environment that is conducive to the progression of dental caries. A healthy salivary flow will help facilitate rebound of the pH back to neutral in approximately 30 minutes. In contrast, when someone with xerostomia eats or drinks, the pH will drop, but it may take 2 or more hours for the pH to rebound.19 Consider that when a patient with xerostomia is sipping on juice or using lozenges or candies to keep their mouth moist, these patients, in theory, may have an acidic oral environment for considerable of periods of time (Figure 1).
The role of saliva is important to consider, because saliva has immunoglobulins, buffering agents, calcium, and phosphate that will protect teeth against dental caries.20 In patients with normal salivary flow, the saliva can naturally help to remineralize teeth, especially when in the presence of fluoride, calcium, and phosphate. When patients do not have an adequate salivary flow, they do not have the natural reserve of calcium and phosphate, leaving them defenseless against the acid insult that occurs when eating or drinking substances that have a low pH or contain fermentable carbohydrates.
Lack of saliva also changes the consistency of dental plaque. When a patient has an inadequate salivary flow, the plaque becomes stickier, thicker, and more difficult to remove.21,22 If a patient with historically good oral hygiene presents to the office with an uncharacteristic amount of plaque on his or her teeth, it is prudent for the clinician to consider the onset of xerostomia, as well as inquiring about changes in oral hygiene practices.
Clinical Considerations for Minimization of Caries Risk
Patients that suffer from xerostomia can benefit from the following:
Nutritional counseling: The clinician can help guide patients to make diet selections that do not increase the risk for dental caries, including non-cariogenic food and snack selections and limiting sugar in the diet and drinks.
Xylitol: This naturally occurring sweetener is commonly found in chewing gum, mints, and oral sprays. Xylitol is recommended as an adjunct for caries management due to its bacteriostatic properties and ability to raise oral pH by stimulating salivation. For high- or extremely high-risk patients, 6 to 9 grams of xylitol is recommended daily.4 However, ingesting greater than the recommended dosage may contribute to gastric distress and should be discouraged. In addition, xylitol may be harmful to dogs,23 and patients should be encouraged to keep xylitol products away from pets.
Restoration of minerals: To restore the lost minerals that naturally occur in saliva, topical application of pastes containing fluoride, calcium, and phosphate can promote remineralization, halt the caries process, and prevent the occurrence of dental caries.24
pH neutralization strategies: The use of products that contain sodium bicarbonate is recommended to neutralize an acidic oral environment.
Poor Oral Hygiene
Most people have caries-causing bacteria in their dental plaque. In health, there tends to be low numbers of bacteria, and the frequent disturbance of the biofilm during tooth brushing and flossing will prevent demineralization or cavitation of a tooth. When large amounts of plaque are present due to inadequate oral hygiene, the number of anaerobic and acidogenic bacteria increases. According to Marsh, in the presence of a low pH, coupled with a fermentable carbohydrate, these bacteria thrive. The bacteria will produce acidic byproducts from the metabolism of the fermentable carbohydrate, and demineralization of a tooth can occur.6 Continuous demineralization of a tooth without equal remineralization will lead to cavitation.
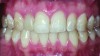
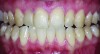
Optimal oral hygiene is challenged when a patient undergoes fixed orthodontic therapy; it is essential, therefore, that the patient receive oral hygiene education to prevent the accumulation of plaque and calculus on the teeth and around the orthodontic appliances. Excessive plaque around orthodontic appliances often results in the formation of white spots or demineralized areas of the enamel surface (Figure 2).
Clinical Considerations for Minimization of Caries Risk
Individualized oral hygiene instructions: Disruption of the colonies within the plaque biofilm will prohibit the formation of virulent complexes that can potentially destroy the tooth and periodontium.
Minimally invasive25 white spot removal: Demineralized enamel often presents as a white or brown “spot” on the tooth surface. Systematic treatment with pastes containing calcium and phosphate can remineralize these surfaces and result in the minimization or removal of the “spot”26 (Figure 3).
Gingival Recession
A patient is at an increased risk for caries when root surfaces are exposed to the oral cavity.27 Cementum is less mineralized then enamel and, therefore, less resistant to caries. Early demineralization of root surfaces may appear clinically as rough, dull, or discolored, whereas occult root caries may present with significant discoloration and cavitation of the root surface.28
Clinical Considerations for Minimization of Caries Risk
Fluoride varnish: According to the American Dental Association Council on Scientific Affairs, fluoride varnish treatments are more comfortable for patients, and the result is improved compliance.29 Fluoride varnishes offer a concentrated application of fluoride, calcium, and phosphate and have been shown to consistently reduce the risk for caries.30 Clinicians should be cognizant that the application recommendations vary for different products and that the manufacturer’s instructions should be reviewed.
Individualized oral hygiene instructions: It is essential for patients to be instructed to clean root surfaces without damaging cementum. Adjunct oral hygiene tools may be necessary for efficient plaque removal in areas with wide embrasures or teeth with furcation involvement.
Deep Occlusal Anatomy
A tooth with deep or well-defined occlusal anatomy presents a greater risk for caries, because it has a greater risk for plaque retention.4
Clinical Considerations for Minimization of Caries Risk
Sealants: It is well documented that glass ionomers offer a viable option for pit and fissure sealants.31-33 They have a similar longevity to their resin-based counterparts; however, glass-ionomer-based sealants offer the added benefit of 400 ppm fluoride release over 4 to 6 months.34,35 Moreover, glass-ionomer sealants are “rechargeable” and permeable to fluoride, calcium, and phosphate to the surface of the tooth. In addition, glass ionomer is an inherently hydrophilic material and is less technique-sensitive than resin-based sealants.36
Caries Incidence within 3 Years/Incipient Caries – Radiographic or Clinical
When a patient presents with caries within a 3-year period it is considered recent dental breakdown. Featherstone states that for a restoration placed within the past 3 years, clinical caries, radiographic interproximal lesions (into dentin or confined to enamel), and white spots on smooth surfaces are “strong indicators for future caries activity and unless there is nonsurgical therapeutic intervention, the likelihood of future cavities or the regression of existing lesions is very high.”4 After a patient is caries-free for 3 years and risk factors have been eliminated or controlled, a practitioner may consider classifying the patient into a lower risk category.
Clinical Considerations for Minimization of Caries Risk
• Fluoride varnish treatments.
• Pastes containing calcium and phosphate.
• Xylitol.
• pH neutralization strategies.
Extensive Restorative History/Fixed or Removable Prosthodontics
Patients with extensively restored teeth are at an increased risk for caries. Despite a practitioner’s best efforts, most restorations fail at the tooth–restoration interface, and when a patient is at an increased risk for dental caries it is likely that the lifespan of the restoration will be greatly diminished. In addition, patients that present with extensive dental treatment indicate a past history of deterioration of dental health, and if the dental disease was a recent occurrence there is a high likelihood of recurrence. Identification of caries risk factors and minimization of risk is essential to improve the lifespan of dental restorations and prevent recurrence of disease.
Removable Partial Dentures (RPDs)—Patients that wear removable partial dentures are at an increased risk for dental caries due to the increased likelihood that caries37 will develop along the surfaces on abutment teeth adjacent to the minor connectors and guide planes of the RPD framework. According to Budtz-Jörgensen and Isidor, the caries rate was six times higher for the RPD group than the control groups within their 5-year study.38,39
Fixed Partial Dentures (FPDs)—The average lifespan for fixed partial dentures is approximately 10 years, and the long-term prognosis of the FPD becomes less favorable as the span of the FPD increases.40 The most common mode of failure is dental caries41 around the margins of abutment teeth; therefore, it is essential to provide additional protection of the abutment teeth to minimize restorative failures due to dental caries.
Clinical Considerations for Minimization of Caries Risk
Individualized oral hygiene instruction, specifically around abutment teeth for RPDs and around the margins of fixed prosthetics.
Frequent recare42 visits to evaluate for demineralization of abutment teeth or around margins of fixed restorations.
Paste containing calcium and phosphate.
Fluoride varnish treatments at recare visits.
Conclusion
Providing restorations that have long-lasting outcomes requires more than exceptional clinical skills. The assessment of factors that contribute to a patient’s disease process and the minimization of risk will aid the practitioner in providing restorations with the most favorable outcome. Additionally, this approach to patient care promotes cooperation between the dental practitioner and patient and can thereby aid in achieving optimal oral health.
ABOUT THE AUTHOR
Pamela Maragliano-Muniz, DMD
Assistant Clinical Professor,
Tufts University School of Dental Medicine,
Boston, Massachusetts;
Private Practice specializing in Prosthodontics,
Boston, Massachusetts
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
REFERENCES
1. Young DA, Featherstone JD, Roth JR. Curing the silent epidemic: caries management in the 21st century and beyond. J Calif Dent Assoc. 2007;35(10):681-685.
2. Kutsch VK, Milicich G, Domb W, et al. How to integrate CAMBRA into private practice. J Calif Dent Assoc. 2007;35(11):778-785.
3. Ramos-Gomez FJ, Crall J, Gansky SA, et al. Caries risk assessment appropriate for the age 1 visit (infants and toddlers). J Calif Dent Assoc. 2007;35(10):687-702.
4. Featherstone JD, Domejean-Orliaguet S, Jenson L, et al. Caries risk assessment in practice for age 6 through adult. J Calif Dent Assoc. 2007;35(10):703-713.
5. Harris NO. Carious lesions. In: Harris NO, Garcia-Godoy F, Nathe CN, eds. Primary Preventive Dentistry. 7th ed. New York, NY: Prentice Hall; 2008.
6. Marsh PD. Dental plaque as a biofilm and microbial community - implications for health and disease. BMC Oral Health. 2006;15(6 suppl 1):S14.
7. Marsh PD. Are dental diseases examples of ecological catastrophes? Microbiology. 2003;149(pt 2):279-294.
8. Loesche WJ. Clinical and microbiological aspects of chemotherapeutic agents used according to the specific plaque hypothesis. J Dent Res. 1979;58(12):2404-2412.
9. Jenson L, Budenz AW, Featherstone JD, et al. Clinical protocols for caries management by risk assessment. J Calif Dent Assoc. 2007;35(10):714-723.
10. Maragliano-Muniz PM, Roberts DR, Chapman RJ. Trends in dental hygiene. RDH Magazine. 2012;32(12):56-59,74-75.
11. Larmas M. Saliva and dental caries: diagnostic tests for normal dental practice. Int Dent J. 1992;42(4);199-208.
12. Department of Health, United Kingdom. Meeting the challenges of oral health for older people: a strategic review. Gerodontology. 2005;22(suppl 1):3-48.
13. Kossioni AE, Dontas AS. The stomatognathic system in the elderly. Useful information for the medical practitioner. Clin Interv Aging. 2007;2(4):591-597.
14. Papas AS, Joshi A, MacDonald SL, et al. Caries prevalence in xerostomic individuals. J Can Dent Assoc. 1993;59(2):171-174,177-179.
15. Moseeva MV, Belova EV, Vakhrushev IaM. Helicobacter pylori in the development of dental caries [in Russian]. Eksp Klin Gastroenterol. 2010;(2):19-21.
16. Corrêa MC, Lerco MM, Cunha Mde L, Henry MA. Salivary parameters and teeth erosions in patients with gastroesophageal reflux disease. Arg Gastroenterol. 2012;49(3):214-218.
17. Johansson AK, Norring C, Unell L, Johansson A. Eating disorders and oral health: a matched case-control study. Eur J Oral Sci. 2012;120(1):61-68.
18. Cassolato SF, Turnbull RS. Xerostomia: clinical aspects and treatment. Gerodontology. 2003;20(2):64-77.
19. Stephan Curves: The Basics. Newcastle University website. http://www.ncl.ac.uk/dental/oralbiol/oralenv/tutorials/stephancurves1.htm. Accessed August 29, 2013.
20. Humphrey SP, Williamson RT. A review of saliva: normal composition, flow, and function. J Prosthet Dent. 2001;85(2):162-169.
21. Navazesh M, Kumar SK. Xerostomia: prevalence, diagnosis, and management. Compend Contin Educ Dent. 2009;30(6):326-328,331-332.
22. Glore RJ, Spiteri-Staines K, Paleri V. A patient with dry mouth. Clin Otolaryngol. 2009;34(4):358-363.
23. Murphy LA, Coleman AE. Xylitol toxicosis in dogs. Vet Clin North Am Small Anim Pract. 2012;42(2):307-312.
24. Somasundaram P, Vimala N, Mandke LG. Protective potential of casein phosphopeptide amorphous calcium phosphate paste on enamel surfaces. J Conserv Dent. 2013;16(2):152-156.
25. Mickenautsch S. An introduction to minimum intervention dentistry. Singapore Dent J. 2005;27(1):1-6.
26. Bailey DL, Adams GG, Tsao CE, et al. Regression of post-orthodontic lesions by a remineralizing cream. J Dent Res. 2009;88(12):1148-1153.
27. Katz RV, Hazen SP, Chilton NW, Mumma RD Jr. Prevalence and intraoral distribution of root caries in an adult population. Caries Res. 1982;16(3):265-271.
28. Maragliano-Muniz PM, Roberts DR, Chapman RJ. Classification system for root-surface quality. Inside Dentistry. 2012;8(1):34-42.
29. American Dental Association Council on Scientific Affairs. Professionally applied topical fluoride. J Am Dent Assoc. 2006;137(8):1151-1159.
30. Tellez M, Gomez J, Kaur S, et al. Non-surgical management methods of noncavitated carious lesions [published online ahead of print December 18, 2012]. Community Dent Oral Epidemiol. 2012; doi 10.1111/cdoe.12028.
31. Beauchamp J, Caufield PW, Crall JJ, et al. Evidence-based clinical recommendations for the use of pit-and-fissure sealants: a report of the American Dental Association Council of Scientific Affairs. J Am Dent Assoc. 2008;139(3):257-268.
32. Niederman R. Glass ionomer and resin-based fissure sealants - equally effective? Evid Based Dent. 2010;11(1):10.
33. Yengopal V, Mickenautsch S, Bezerra AC, Leal SC. Caries-preventive effect of glass ionomer and resin-based fissure sealants on permanent teeth: a meta analysis. J Oral Sci. 2009;51(3):373-382.
34. Antonson SA, Antonson DE, Brener S, et al. Twenty-four month clinical evaluation of fissure sealants on partially erupted permanent first molars: glass ionomer versus resin-based sealant. J Am Dent Assoc. 2012;143(2):115-122.
35. Simonsen RJ. Retention and effectiveness of dental sealant after 15 years. J Am Dent Assoc. 1991;122(10):34-42.
36. Baseggio W, Naufel FS, Davidoff DC, et al. Caries-preventive efficacy and retention of a resin-modified glass ionomer cement and a resin-based fissure sealant: a 3-year split-mouth randomised clinical trial. Oral Health Prev Dent. 2010;8(3):261-268.
37. Mazurat NM, Mazurat RD. Discuss before fabricating: communicating the realities of partial denture therapy. Part II: clinical outcomes. J Can Dent Assoc. 2003;69(2):96-100.
38. Bergman B, Hugoson A, Olsson CO. Caries and periodontal status in patients fitted with removable partial dentures. J Clin Periodontol. 1977;4(2):134-146.
39. Budtz-Jørgensen E, Isidor F. A 5-year longitudinal study of cantilevered fixed partial dentures compared with removable partial dentures in a geriatric population. J Prosthet Dent. 1990;64(1):42-47.
40. Tan K, Pjetursson BE, Lang NP, Chan ES. A systematic review of the survival and complication of fixed partial dentures (FPDs) after an observation period of at least 5 years. Clin Oral Implants Res. 2004;15(6):654-666.
41. Libby G, Arcuri MR, LaVelle WE, Hebl L. Longevity of fixed partial dentures. J Prosthet Dent. 1997;78(2):127-131.
42. Budtz-Jörgensen E. Restoration of the partially edentulous mouth—a comparison of overdentures, removable partial dentures, fixed partial dentures and implant treatment. J Dent. 1996;24(4):237-244.