You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Early studies on risks of infection from exposure to microbial pathogens focused primarily on medical healthcare workers. However, oral healthcare professionals face similar infection control concerns, especially since pathogens occur in oral tissues and oral fluids.1 Comprehensive infection control guidelines from the Centers for Disease Control and Prevention (CDC) include recommendations for personal protective equipment such as gloves, masks, eyewear, and protective clothing designed to protect oral healthcare workers in these environments.
Multiple investigations into medical and oral healthcare worker occupation-related infections indicate repeated exposures to microorganisms in blood and other secretions, resulting in higher infectious disease incidence among healthcare workers than in the general population.2 In this current study, the exposure to airborne microorganisms was not observed. Research indicates that only 40% to 50% of healthcare workers in the hospital setting comply with handwashing and hand disinfection recommendations.3,4 Noncompliance with hospital/medical standards in healthcare facilities increases the probability that infection will spread. Suggested reasons for poor hand hygiene among healthcare workers are diverse and inconclusive but may be related to time.5 On a more positive note, a 2008 survey conducted by Myers, et al., and cited by K. Erdman, limited due to sample size, found that only 6% of dentists reported that they did not practice recommended hand hygiene procedures at the beginning of the practice day, and only 11% of dental hygienists reported not performing hand hygiene between patients.6
In 2013, Garland examined the infection control knowledge level and practices in a sample of US dental hygienists. She found a high level of familiarity with the CDC guidelines, and a majority (52%) of respondents reported believing that if they followed the handwashing recommendations, their hands might be drier and subject to more skin damage.7 Though few studies examined oral health professional practices and compliance with infection control, this article uses the available research to review hand care procedures and glove recommendations including pre-treatment, treatment, and post-treatment procedures.
Before Patient Treatment
Prior to treatment, clinicians should select gloves that are protective and comfortable, and that permit good circulation and complete tactile sensitivity. Gloves acceptable for use in the oral healthcare setting generally include heavy-duty utility gloves, sterile surgeon's gloves, and nonsterile latex/nitrile exam gloves.
The glove should cover the whole length of the hand, reaching even slightly past the cuff. A proper fit will not cause tension that can lead to premature fatigue.
Gloves vary in terms of integrity, protection, resistance to chemical penetration, and potential to cause allergic reactions to their material. Glove selection should take the treatment procedure into consideration to make sure both protection and time-efficiency are maximized.
Each pair of gloves should be used only once, one pair per procedure, to avoid potential cross infection.8,9 Select FDA-approved gloves and note their expiration date. Gloves past their expiration can compromise protection. When ordering and using these products, keep all these aspects in mind. Having the correct single-use, personal protective equipment is worth the expense.10
For clinicians, hands are the most common area for disease transmission. Bacteria and microbes are easily removed by comprehensive, systematic hand washing and regular compliance with OSHA guidelines for safety. Soaps and hand sanitizers should be purchased in non-refillable containers in liquid form to prevent staff members refilling containers with expired liquids and still have an appropriate expiration date. Review the expiration date of all products prior to clinical use.11 Hand lotions that contain petroleum should not be used because they can weaken latex gloves and increase permeability. Only water-based lotions should be used during the workday. If the clinician is lubricating the patient's lips during the appointment, choose a non-petroleum product, such as cocoa butter.12
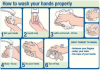
Handwashing should be accomplished with sensor-dispensed water, soap and disposable towels. Each handwashing session should consist of 20 seconds of regular scrubbing and cleansing of fingernails, under nails, between fingers including thumb and wrists, after which the hands should be rinsed and completely dried. Figure 1 illustrates proper handwashing technique.13
Hands should be clear of any jewelry or obstructions that could harbor bacteria. In a study of 40 dental hygienists, researchers found that those who wore rings were twice as likely to harbor potential pathogenic bacteria and almost five times more likely to harbor fungi than those who did not. In a clinical study of nurses, the results were similar. "In a sample of 84 nurses working in intensive care units, those who wore rings showed more gram-positive and gram-negative bacteria than those who did not, while no difference was found between nurses wearing plain wedding rings and those wearing rings with stones. Most importantly, samples were collected after hand cleansing with alcohol and rubbing for 30 seconds as recommended."14
Nail care is another important aspect of maintaining asepsis. Nails should be clean and short with no adornment.6 Studies have found that nails with polish or gel or acrylic adhesive on them contributed to infection and cross-contamination of patients in healthcare settings.15 These adornments disrupt the natural nail, creating a harbor for pathogens. Artificial nails cannot be cleaned thoroughly by either alcohol-based sanitizer or rigorous scrubbing with soap and water.16
Immunocompromised patients are most at risk for cross-contamination. Of five separate cases studied in a hospital setting, at least one bacterial patient infection was linked to the clinician's fingernails. Infectious bacteria include Pseudomonas aeruginosa, Serratia marcescens, extended-spectrum beta-lactamase (ESBL) Klebsiella pneumoniae, and Candida osteomyelitis.17
During Treatment
Hands should be completely clean and dry prior to donning gloves. It is important to not trap moisture from soap or hand sanitizer in the glove during treatment. If hands are not fully dry, the resulting warm, moist environment permits growth of microorganisms on the hand and irritates sensitive skin, creating a rash that could affect the clinician later.18 Hand dermatitis is approximately 17% to 30% more common among medical and dental professionals than in the general population. Hand dermatitis is caused by exposure of skin to water, detergent, fragrances, antimicrobial agents, low humidity levels, frequent hand washing and repeated gloving.19 Affected people often complain of a feeling of dryness or burning; skin that feels "rough"; and erythema, scaling, or fissures.20 Skin should be well-moisturized and free of open cuts to prevent an infection in the clinician or the patient being treated. Following proper guidelines helps clinicians reduce the likelihood of dermatitis and skin irritation.
Use clean hands to remove gloves from the box to prevent contaminating the remaining gloves.21 An optimal time interval has not been established for glove changing during long procedures, although there is evidence that undetected micro perforations frequently develop in medical gloves somewhere between 30 minutes and three hours of use.22 For dental hygiene professionals, gloves typically deteriorate in less than 45 minutes, but the risk remains the same.
Cross contamination from reusing gloves is dangerous and unnecessary. Failures in infection control include the patient being touched intraorally by a contaminated glove that had been used extraorally, touching nonsterile materials before a treatment procedure, and washing a glove before using it for another function during treatment.23 Washing single-use gloves decreases the integrity of the material, and reusing them is not recommended.24
Post-Treatment
After treatment is complete, remove using the Beak Method: remove one soiled glove with the other, then slip a clean finger under the remaining glove edge to remove it. Consistent use of this method will help clinicians avoid contaminating their hands when removing gloves. Glove use should never be treated as a substitute for consistent and meticulous hand hygiene or as an infallible barrier. It is critical that hand hygiene be performed immediately after glove removal.25
Once contaminated gloves are removed, the clinician should diligently wash hands and/or disinfect with an alcohol-based sanitizing rinse for 30 seconds. When using the hand sanitizing alcohol rinse, the clinician must rub their hands until completely dry to ensure microbial inactivity. Alcohol-based hand sanitizers play a crucial role in preventing acquisition of pathogens, but they have no effectiveness against bacterial spores.26 Because of this, clinicians should practice thorough hand hygiene with soap and water in between patients to avoid bacterial transportation.
Studies report that dental hygienists were more likely to recommend use of stringent infection control procedures than dentists or dental assistants. Although dental hygienists recommended practices more frequently, none of these professionals were able to comply with standard infection control procedures.27
It is our responsibility as healthcare workers to systematically and consistently comply with all standards. CDC's website includes a checklist of expectations for safe care.28
References
1. Crawford JJ. Cross infection risks and their control in dentistry. An overview. CDA J. 1985;13(10):18-21.
2. Molinari J. Infection control: its evolution to the current standard precautions. J Am Dent Assoc. 2003;134(5):569-574.
3. Chatfield SL, Debois K, Nolan R, et al. Hand hygiene among healthcare workers: a qualitative meta summary using the Grade-CERqual process. J Infect Prev. 2017;18(3):104-120.
4. Pereira E. Evaluation of the multimodal strategy for improvement of hand hygiene as proposed by the World Health Organization. J Nurs Care Qual. 2017;32(2):E11-E19.
5. dos Santos RP, Konkewicz LR, Nagel FM, et al. Changes in hand hygiene compliance after a multimodal intervention and seasonality variation. Am J Infect Control. 2013;41(11):1012-1016.
6. Erdman K. Nail hygiene: maintaining healthy fingernails is key to reducing microbial transmission in the dental setting. DDH. 2014;12(3):28-32.
7. Garland KV. A survey of United States dental hygienists' knowledge, attitudes, and practices with infection control guidelines. J Dent Hyg. 2013;87(3):140-151.
8. Seavey R. Moving beyond the wild, wild west of reprocessing. Communique. 2012;9:70-71.
9. Schrubbe K, Roth K. The price of safety. Dimensions Dent Hyg. 2013;11(1):36-40.
10. Cuny E. Best practices for personal protective equipment: the effective use of these infection control tools makes all the difference in ensuring clinician and patient health and safety. Dimensions Dent Hyg. 2016;14(6):36-42.
11. Saskatchewan Infection Control Program Hand Hygiene Working Group. Infection Prevention and Control Recommendations for Hand Hygiene in All Healthcare Settings. Government of Saskatchewan, February 2017.
12. Goodwin N. The evolution of gloves. Dimensions Dent Hyg. 2014;12(9):30-36.
13. Montana DPHHS. School of nursing hand washing chart. http://dphhs.mt.gov/schoolhealth/schoolnurse/schoolnursetipsforahealthyschoolyear. Accessed January 5, 2018.
14. Messano G. Bacterial and fungal contamination of dental hygienists' hands with and without finger rings. Acta Stomatologica Naissi. 2013;29:1260.
15. Arrowsmith VA, Taylor R. Removal of nail polish and finger rings to prevent surgical infection. Cochrane Database System Rev. 2012;5:CD003325.
16. Alberta Health Services. Artificial nails in the healthcare environment: why we care. 2017.
17. Moolenaar RL, Crutcher JM, San Joaquin VH, et al. A prolonged outbreak of Pseudomonas aeruginosa in a neonatal intensive care unit: did staff fingernails play a role in disease transmission? Infect Control Hosp Epidemiol. 2000;21(2):80-85.
18. Garland K. Brush up on the basics of PPE: the appropriate use of personal protective equipment is integral to the safe provision of oral health care services. Dimensions Dent Hyg. 2017;15(10):23-26.
19. Anjum Shah M. Maintaining skin integrity. Dimensions Dent Hyg. 2014;12(7):19-25.
20. Centers for Disease Control and Prevention. Guidelines for hand hygiene in health-care settings. MMWR. 2002.
21. Eveillard M. Wearing gloves: the worst enemy of hand hygiene? Future Microbiol. 2011;6(8):835-837.
22. Partecke LI, Goerdt AM, Langner I, et al. Incidence of microperforation for surgical gloves depends on duration of wear. Infect Control Hosp Epidemiol. 2009;30(5):409-414.
23. Loveday H, Lynam S, Singleton J, Wilson J. Clinical glove use: healthcare workers' actions and perceptions. J Hosp Infect. 2014;86(2):110-116.
24. WHO Patient Safety: Gloves use information leaflet. World Health Organization, 2009. http://www.who.int/gpsc/5may/Glove_Use_Information_Leaflet.pdf. Accessed January 5, 2018.
25. Globus. How to safely remove disposable gloves. https://www.globus.co.uk/how-to-safely-remove-disposable-gloves. Accessed January 5, 2018.
26. Nerandzic M, Sankar T, Setlow P, Donskey C. A cumulative spore killing approach: synergistic sporicidal activity of dilute peracetic acid and ethanol at low pH against Clostridium difficile and Bacillus subtilis spores. Open Forum Infect Dis. 2016;3(1):ofv206.
27. King TB, Muzzin KB. A national survey of dental hygienists' infection control attitudes and practices. J Dent Hyg. 2005;79(2):1-13.
28. Centers for Disease Control and Prevention. Summary of infection prevention practices in dental settings: basic expectations for safe care. CDC, 2016. https://www.cdc.gov/oralhealth/infectioncontrol/pdf/safe-care2.pdf. Accessed January 12, 2018.