You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
The long-taught practice for composite restorations has been to place composite material incrementally in 2-mm layers. Part of the theory behind this teaching was that it would reduce the total amount of polymerization shrinkage of the composite. As one layer of composite is placed and cured, all surfaces of that composite layer not bonded to tooth structure could contract freely. In this way, stress relief could be achieved at each layer of cured composite, as opposed to a single cured layer with a bulk-filling technique. However, some researchers have questioned the benefits of using incremental filling to reduce the clinical effects of composite shrinkage.1 A more substantial claim for the 2-mm composite increment is the ability of a curing light to effectively polymerize a composite to this depth. Both polymerization shrinkage and depth of cure are important clinical parameters. Excessive polymerization shrinkage could lead to open margins, microleakage, and postoperative sensitivity or cuspal deflection and enamel fracture.2 Inadequate depth of cure could leave composite at apical margins soft and susceptible to wear, dissolution, or fracture.3
The impetus for bulk-filling composites is a desire to reduce the time required for composite placement and to eliminate the possibility of voids between composite layers. The time savings allowed by placing a single layer of composite can be appreciated by both the dentist and patient. In addition, an unwanted side effect of the incremental placement technique is the introduction of voids between composite layers. For universal handling composites, the stickiness of the composite to the placement instrument can make it difficult to completely adapt the new layer of composite to the previous layer. When placing additional layers of flowable composite, air can become trapped between layers. Internal voids may be innocuous in some clinical cases; however, in stress-bearing areas, a void may act as a site of stress concentration and eventual fracture.4 Voids or gaps present on the external surface of a composite restoration may be more prone to staining.
How Bulk-Fill Composites Work
In response to the clinical demand for materials compatible with bulk-filled placement, a new class of dental composites has been developed. In general, bulk-fill composite materials are characterized by lower shrinkage stress and a higher depth of cure than conventional composites. Shrinkage stress is defined as the amount of force per area exerted on the walls of a cavity preparation by a composite as it polymerizes. Volumetric shrinkage, on the other hand, is the difference in volume between an uncured and cured specimen of composite. Shrinkage stress is more clinically important than volumetric shrinkage because a material that shrinks substantially when cured on a countertop may not exert large forces when cured inside a bonded restoration.5
Methods that manufacturers may employ to produce composites that do not exert high stress during polymerization include increasing “flexibility” of polymer networks in the composite resin; incorporating “flexible” fillers in the composite; and slowing the polymerization reaction to allow polymers time to disperse prior to crosslinking.6-8 Many commercially available bulk-fill composites incorporate one or more of these techniques to reduce polymerization shrinkage. Several research studies have compared polymerization shrinkage of conventional composites and bulk-fill composites. Broadly, bulk-fill flowables have less polymerization shrinkage stress than conventional flowables, and high-viscosity bulk-fill composites demonstrate polymerization stress similar to or less than comparable conventional composites.7,9-11
Depth of Cure
Most bulk-fill materials are marketed with claims that they have 4 mm of curing depth. Depth of cure is commonly measured by measuring the hardness or the degree of double-bond conversion at the surface of a composite exposed to a curing light and comparing it with the degree of conversion at various depths of the restoration. Several studies have determined that bulk-fill composites have a degree of conversion (indicating adequate crosslinking) of at least 80% of their surface value at 4-mm depths.11-13 Other studies have determined that hardness values at 4 mm were at least 80% of the surface hardness for most bulk-fill materials.7,14-17 Some studies suggested that not all high-viscosity bulk-fill composites could achieve acceptable hardness all the way to 4 mm.13,15,17 All bulk-fill composites showed higher depths of cure than conventional composites used as a control.7,11,15-17
Manufacturers have achieved this depth of cure by modifying the translucency of the composite and including more effective light initiators. When a composite is light cured from the occlusal direction, light energy from the curing light must be transmitted through the bulk of the composite without being absorbed or deflected before reaching the bottom of the restoration. By adjusting the translucency of the composite or matching the refractive index of the filler and the resin, light can travel through an increased depth of a bulk-filled composite.18,19 A side effect of this modification is that several of these materials appear more visually translucent than tooth structure.
The other method that manufacturers have used to increase depth of cure is by incorporating more efficient and robust light initiators. Most dental composites polymerize by activating the photoinitiator camphorquinone (CQ). When the energy from a curing light excites CQ, it stimulates an amine co-initiator to release a free radical and initiate resin polymerization. Ivocerin®, a new germanium-based photoinitiator patented by Ivoclar Vivadent (www.ivoclarvivadent.us), does not require a co-initiator and requires less energy from a curing light to produce crosslinking of the resin composite.8,20 Therefore, composite at the bottom of a 4-mm layer requires less light to achieve sufficient mechanical and physical properties.
In addition, manufacturers have added blends of photoinitiators that are activated at different wavelengths of light to optimize the energy from a curing light. CQ is maximally stimulated at 468 nm. Ivocerin has a maximum absorption of 410 nm. The photoinitiators phenyl-propanedione (PPD) and Lucirin® TPO (BASF, www.basf.com) absorb a lower wavelength of light (385-400 nm) and have been used in light and translucent shades of composite because they do not exhibit the yellowing associated with CQ.
Effective Light Curing
The range of maximum of absorption of different photoinitiators has clinicians concerned that their curing lights do not have the spectral output to effectively polymerize these composites. For reference, a typical LED curing light has a spectral output of utilizable wavelength ranging from 430 to 480 nm. New polywave or multi-wavelength LEDs have expanded spectral outputs. These new lights include VALO® by Ultradent (www.ultradent.co) with a range of 395 to 480 nm and the Bluephase® 20i by Ivoclar Vivadent with a range of 385 to 515 nm. Testing by the author, however, has revealed that Tetric EvoCeram® Bulk Fill with Ivocerin (Ivoclar Vivadent) could be effectively cured to 4 mm with both a traditional and polyphase LED curing light (Figure 1). Because Tetric EvoCeram Bulk Fill is the only bulk-fill composite marketed with a new photoinitiator, the concern of composite and light compatibility may not be of clinical relevance with current materials.
Clinicians should be concerned, however, about the power output (also called irradiance) of their curing lights. The depth of cure of a bulk-fill composite measured in laboratory testing is typically determined with relatively new lights with power outputs greater than 600 mW/cm2. A recent study has shown that dental curing lights measured at 200 private practices had low outputs (200 mW/cm2 to 400 mW/cm2) and were covered with composite residue.21 Clinicians should monitor the output of their curing lights and keep their light tips clean with protective sleeves or acetone-based cleaners. Because every resin composite requires a minimum amount of energy, lights with lower outputs must be compensated by using longer exposure time.22
Types of Bulk-Fill Composites
Many manufacturers have entered the market with bulk-fill composites. SureFil® SDR® by DENTSPLY Caulk (www.caulk.com) was one of the first materials advertised for use with a 4-mm layer. This flowable composite is characterized by very low shrinkage stress and high translucency. Modifying the polymerization kinetics and allowing the material to flow during polymerization leads to low shrinkage stress. It must by “capped” with a more wear-resistant composite and is used primarily as a base in deep areas of preparations and proximal boxes. Filtek™ Bulk Fill Flowable was introduced by 3M ESPE (www.3mespe.com), followed shortly by the more highly filled Filtek™ Bulk Fill Posterior Restorative. The novel components of these materials are two monomers. One monomer can fragment in response to shrinkage stresses and rebond in a more relaxed position, and the other reduces the density of crosslinking.8
Ivoclar Vivadent released its highly filled material Tetric EvoCeram® Bulk Fill and later a flowable version, Tetric EvoFlow Bulk Fill. These materials contain the photoinitiator Ivocerin as well as stress-relieving “flexible” filler particles.6 Kerr’s SonicFill™ (www.kerrdental.com) utilizes sonic energy (vibrations within the audible frequency) to reduce the viscosity of a highly filled material and allow it to flow into a preparation. The sonic energy is supplied by a specific handpiece that attaches to an air hookup and is dispensed by pressing on a rheostat. After dispensing, the material returns to a sculptable state, allowing the clinician to contour the restoration. The high concentration of filler particles (83.5 wt%) reduces polymerization shrinkage of the composite as the resin, not the fillers, contract upon polymerization. The manufacturer does not explain how the increased depth of cure is obtained. Other bulk-fill composite materials include QuiXX® (DENTSPLY), Beautifil® (Shofu,www.shofu.com), Venus® Bulk Fill (Heraeus Kulzer, www.heraeus-kulzer.com), HyperFIL™ (Parkell Inc., www.parkell.com), X-tra Base and X-tra Fil (Voco, www.voco.com).
Techniques and Applications
The placement techniques for bulk-fill composites vary for flowable and higher viscosity materials. Bulk-fill flowable composites are primarily used for deep bases and interproximal boxes under conventional composites. Interproximal boxes can easily reach depths beyond 4 mm, and therefore at least two increments of composite are needed. To reinforce this point, it is important to note that bulk-fill does not mean one increment up to the occlusal surface. Instead, it implies increments up to 4 mm in depth. Even for shallow preparations of 4 mm or less, flowable bulk-fill composites are not indicated for the final occlusal layer. The two main reasons these materials are not placed up to the occlusal surface of a restoration are their low wear resistance and high translucency.
A study of several flowable bulk-fill composites showed that all flowables had significantly more wear than the control (Z100™, 3M ESPE); more wear was seen for SureFil SDR (0.04 mm3) than Venus Bulk Fill (0.024 mm3) or Filtek Bulk Fill (0.012 mm3). In addition, flowable bulk-fill composites tend to have a very high translucency that prevents them from blending with natural tooth structure. For this reason, manufacturers recommend covering or “capping” these materials with a conventional posterior composite.
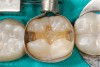
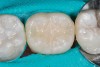
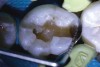
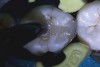
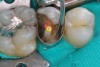
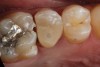
Higher viscosity bulk-fill composites can be used up to the occlusal surface, however. Two clinical cases using the bulk-fill composites Tetric EvoCeram Bulk Fill and SonicFill are presented in Figure 2 through Figure 6. Limitations when placing a high-viscosity bulk-fill composite include difficulty of condensing and esthetic restraints. Condensing a high-viscosity resin composite ensures adequate adaptation to the tooth preparation and sufficient interproximal contacts. Condensing 4 mm of composite is more difficult than condensing 2 mm. To ensure adequate interproximal contacts, a sectional or circumferential matrix with an inciso-gingival curvature can be used to obtain a tight area of contact gingival to the marginal ridge. A ring should be used to help separate the teeth and improve the tightness of the contact area.
An esthetic limitation of bulk-fill composites is that most materials are available in a small selection of shades. In addition, some of these materials have slightly higher translucency than conventional posterior composites. The esthetics achieved by these composites should be sufficient for posterior restorations for most patients.
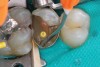
Another possible clinical application of bulk-fill composites is for use as a core build-up material. A clinical case demonstrating this technique is presented in Figure 7 through Figure 9. Build-ups are often placed into large, deep preparations with pins or a post. Therefore, important characteristics to consider for these materials are their shrinkage stress, depth of cure, flow, and toughness/strength. Flowable bulk-fill composites are desirable materials to use for build-ups because they have appropriate flow to adapt to a post or pin, low shrinkage stress, and high depth of cure, allowing them to be placed in bulk with the strength and toughness of a resin composite.
Conclusions
Bulk-fill composites are a new class of material with scientific evidence for claims of low polymerization shrinkage and 4-mm depths of cure. The appearance, handling, and mechanical properties of bulk-fill composites vary between flowable and high-viscosity materials. In general, flowable materials have a deeper depth of cure; however, high-viscosity materials have better wear resistance and less transparency. The handling and esthetic limitations of these materials may not be sufficient for use in anterior restorations; however, bulk-fill materials are a good solution for efficient posterior restorations and possibly core build-ups.
Author Information
Nathaniel Lawson, DMD, PhD, is an assistant professor in the division of biomaterials at the University of Alabama at Birmingham (UAB). He started his education as a biomedical engineering student at Tulane University. He completed his DMD at the UAB School of Dentistry and his MS and PhD in the department of biomedical engineering at UAB. Following graduation, he worked in private practice in Alabama and Illinois. Dr. Lawson is passionate about testing new materials and techniques in the laboratory. His main research focus involves testing the strength, color, wear, roughness and bond strength of ceramics, composites, cements, impression materials, and adhesives.
References
1. Versluis A, Douglas WH, Cross M, Sakaguchi RL. Does an incremental filling technique reduce polymerization shrinkage stresses? J Dent Res. 1996;75(3):871-878.
2. Giachetti L, Russo DS, Bambi C, Grandini R. A review of polymerization shrinkage stress: current techniques for posterior direct resin restorations. J Contemp Dent Pract. 2006;7(4).
3. Shortall AC. Depth of cure of radiation-activated composite restoratives--influence of shade and opacity. J Oral Rehabil. 1995;22(5):337-342.
4. Purk JH, Dusevich V, Glaros A, Eick JD. Adhesive analysis of voids in Class II composite resin restorations at the axial and gingival cavity walls restored under in vivo versus in vitro conditions. Dent Mater. 2007; 23(7):871-877.
5. Kappler O, Weinmann W, Thalacker C, et al. Correlation of strain, shrinkage and E-modulus of modern filling composites [abstract 56]. Presented at: IADR General Session; April 1, 2009; Miami, FL.
6. Can Say E, Özel E, Yurdagüven H, Soyman M. Three-year clinical evaluation of a two-step self-etch adhesive with or without selective enamel etching in non-carious cervical sclerotic lesions. Clin Oral Investig. 2014;18(5):1427-1433.
7. El-Damanhoury H, Platt J. Polymerization shrinkage stress kinetics and related properties of bulk-fill resin composites. Oper Dent. 2014;39(4):374-382.
8. Ivoclar Vivadent Report No. 19. 2013;19:1-42.
9. Jang JH, Park SH, Hwang IN. Polymerization shrinkage and depth of cure of bulk-fill resin composites and highly filled flowable resin. Oper Dent. 2015;40(2):172-180.
10. Kim RJ, Kim YJ, Choi NS, Lee IB. Polymerization shrinkage, modulus, and shrinkage stress related to tooth-restoration interfacial debonding in bulk-fill composites. J Dent. 2015;43(4):430-439.
11. Marovic D, Tauböck TT, Attin T, et al. Monomer conversion and shrinkage force kinetics of low-viscosity bulk-fill resin composites. Acta Odontol Scand. 2015;73(6):474-480.
12. Czasch P, Ilie N. In vitro comparison of mechanical properties and degree of cure of bulk fill composites. Clin Oral Investig. 2013;17(1):227-235.
13.Tarle Z, Attin T, Marovic D, et al. Influence of irradiation time on subsurface degree of conversion and microhardness of high-viscosity bulk-fill resin composites. Clin Oral Investig. 2015;19(4):831-840.
14. Alrahlah A, Silikas N, Watts DC. Post-cure depth of cure of bulk fill dental resin-composites. Dent Mater. 2014;30(2):149-154.
15. Benetti AR, Havndrup-Pedersen C, Honoré D, et al. Bulk-fill resin composites: polymerization contraction, depth of cure, and gap formation. Oper Dent. 2015;40(2):190-200.
16. Do T, Church B, Veríssimo C, et al. Cuspal flexure, depth-of-cure, and bond integrity of bulk-fill composites. Pediatr Dent. 2014;36(7):468-473.
17. Flury S, Peutzfeldt A, Lussi A. Influence of increment thickness on microhardness and dentin bond strength of bulk fill resin composites. Dent Mater. 2014;30(10):1104-1112.
18. Bucuta S, Ilie N. Light transmittance and micro-mechanical properties of bulk fill vs. conventional resin based composites. Clin Oral Investig. 2014;18(8):1991-2000.
19. Fujita K, Nishiyama N, Nemoto K, et al. Effect of base monomer’s refractive index on curing depth and polymerization conversion of photo-cured resin composites. Dent Mater J. 2005;24(3):403-408.
20. Moszner N, Fischer UK, Ganster B, et al. Benzoyl germanium derivatives as novel visible light photoinitiators for dental materials. Dent Mater. 2008;24(7):901-907.
21. Hegde V, Jadhav S, Aher GB. A clinical survey of the output intensity of 200 light curing units in dental offices across Maharashtra. J Conserv Dent. 2009;12(3):105-108.
22. Roulet JF, Price R. Light curing—guidelines for practitioners—a consensus statement from the 2014 symposium on light curing in dentistry held at Dalhousie University, Halifax, Canada. J Adhes Dent. 2014;16(4):303-304.
23. Sawlani KK, Beck P, Ramp LC, et al. In vitro wear of eight bulk placed and cured composites [abstract 2441]. Presented at: IADR General Session; March 22, 2013; Seattle, WA.