You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
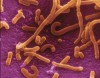
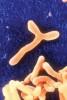
Probiotics are defined as “live microorganisms, which when administered in adequate amounts confer a health benefit on the host.”1 The most commonly studied genera that fulfill this definition are Lactobacillus and Bifidobacterium (Figure 1 and Figure 2). This beneficial role of the selected bacteria was first observed by Eli Metchnikoff, who proposed that Lactobacillus bulgaricus could displace pathological intestinal microbiota. He theorized that because intestinal microbiota depend on food, it might be possible to replace the harmful microbes with useful microbes.2
In contrast, prebiotics are defined as “not digestible food ingredients that beneficially affect the host by selectively stimulating the growth and/or activity of one or a limited number of bacterial species already established in the colon, and thus in effect improve host health.”3 Examples of prebiotics are inulin, fructo-oligosaccharides, galacto-oligosaccharides, and lactulose, all of which can be found in wheat and onions.4
In combination, probiotics and prebiotics may be beneficial; this is known as the symbiotic concept. Symbiotics are defined as “mixtures of probiotics and prebiotics that beneficially affect the host by improving the survival and implantation of live microbial dietary supplements in the gastrointestinal tract of the host.”5
Periodontal disease is a chronic, inflammatory disease affecting the supporting structures of the teeth, ie, the connective tissue attachment, periodontal ligament, and alveolar bone. It results from the interplay of a Gram-negative bacterial infection and the host response in susceptible individuals. The disease may result in bone loss, bleeding and erythema of the gingival tissue, and mobility of the teeth. Methods of treatment often include the mechanical removal of the bacteria with or without antibiotics in combination with improved oral hygiene techniques. Approximately 30% of adults in the United States have moderate forms of periodontitis, and 10% have severe types of the disease.6
Dental caries is also a bacterial disease, brought on by the production of organic acids resulting in the demineralization of tooth structure. It, too, is a multifaceted disease comprising the host, bacteria, and nutrients. The main bacterial cause is Streptococcus mutans through its ability to produce highly branched and water-insoluble glucan and mutan, which helps it become established in the oral biofilm. Together with its acidogenic properties and rapid metabolism of sugars, S. mutans creates a low pH, which shifts the homeostasis in the oral cavity in favor of bacteria that induce caries.7-9
Due to an increase in antibiotic resistance, and because both periodontal disease and dental caries are results of bacterial action, new treatment methods have been explored. Among them, probiotic approaches are being evaluated. This article examines studies that have been aimed at determining the potential of treating periodontal disease and caries management via probiotic mechanism. There are several mechanisms proposed as to how probiotics may work in the oral cavity, including the following10:
• competition with pathogenic bacteria for adhesion sites on dental surfaces
• modification of the environmental conditions of the oral cavity via pH and/or oxidation-reduction potential
• production of antimicrobial substances against oral pathogens
• stimulation of the nonspecific immunity response and modulation of the humoral and cellular immune response
Probiotics and Dental Caries
In order to fight dental caries, probiotics must be able to adhere to dental surfaces and become integrated into the biofilm environment and therein compete with and antagonize the cariogenic bacteria to prevent their proliferation and ability to metabolize sugars, resulting in low acid production.10 Lactobacillus rhamnosus GG was examined in several studies. Näse et al11 tested the dietary strain based on the in-vitro inhibition of a caries pathogen, Streptococcus sobrinus,12 and its effects on the gastrointestinal microbiota in a randomized, double-blind, placebo-controlled intervention study. Although the study did not show a significant reduction in caries prevalence between test (children drinking milk with low concentrations of live L. rhamnosus GG) and control (milk without the strain), the study authors did conclude a tendency for less caries development and lower salivary counts of S. mutans in the probiotic milk–drinking group for children ages 3 to 4 years old.
Ahola et al13 did a randomized, double-blind, controlled study with two parallel groups to examine if the short-term consumption of cheese containing L. rhamnosus GG and L. rhamnosus LC 705 would beneficially affect the oral cariogenic flora of young adults compared to a control and if these effects would persist afterwards. They found significantly more subjects in the probiotics group with a decreased S. mutans count during the post-treatment period. The study concluded that this may be useful in patients with high S. mutans counts. Montalto et al14 sought to learn whether there was a difference between taking probiotic lactobacilli in a liquid versus capsule form on S. mutans counts in a double-blind, randomized, placebo-controlled intervention study. They found that the salivary counts of lactobacilli increased regardless of the liquid or capsule form, but the S. mutans counts were not significantly modified.
Additionally, Nikawa et al15 studied the effects of Lactobacillus reuteri in yogurt on the oral carriage of mutans streptococci. They found reduced S. mutans levels in saliva in those eating the L. reuteri-containing yogurt daily for 2 weeks and that these reduced levels were maintained when the placebo yogurt was consumed afterwards. Calgar et al16 also studied L. reuteri on salivary S. mutans and lactobacilli in a randomized, placebo-controlled study design with parallel arms. They found a statistically significant reduction of the S. mutans levels after the ingestion of the probiotics either via straws or tablets versus the placebo groups (Table 1).
In addition to studies focused on lactobacilli and their possible benefits, other studies, including Calgar et al,17 examined bifidobacteria. The genus Bifidobacterium comprises Gram-positive, non-motile, often branced anaerobic bacteria that are ubiquitous, endosymbiotic inhabitants of the gastrointestinal tract and mouth. The data in the double-blind, randomized crossover design showed that there was a small but significant decrease in salivary S. mutans counts when bifidobacterium-containing yogurt was consumed, but the counts of lactobacillus were unaffected.
Lactobacilli may also be related to caries progression. Fitzgerald et al18 showed that 3 out of 50 lactobacillus strains isolated from the dental plaque of school children induced significant caries in conventional hamsters. This suggests that patients using probiotics with lactobacilli should be closely monitored for caries. Busscher et al19 and Petti et al20 could not detect an oral colonization of lactobacilli after yogurt consumption. It appears that probiotic lactobacilli do not colonize the oral cavity permanently and are eradicated within weeks after termination of probiotics treatment. Replacement therapy such as that described by Hillman et al21 may be a possibility where an effector strain can colonize the oral cavity and displace the indigenous wild type. They isolated a strain of S. mutans that was capable of killing almost all other strains of S. mutans against which it was tested by producing a bacteriocin (mutacin 1140). There is promising data with this strain; however, data from human trials is still needed. Phase 1 of clinical trials may begin in the near future because Hillman et al reported in 200722 on their construction of a BCS3-L1 mutant to test the safety of BCS3-L1 in humans. BCS3-L1 is an effector strain developed from Zymomonas mobilis that has no measurable lactic acid dehydrogenase activity and elevated levels of alcohol dehydrogenase activity relative to its parent (Table 1).
Probiotics and Periodontal Disease
Periodontal disease requires a susceptible host, pathogenic species, and a reduction or absence of “beneficial bacteria.” Probiotics might work by suppressing the endogenous pathogens or preventing the superinfection by exogenous pathogens and/or promoting a beneficial host response.23 In their review, Teughels et al24 summarized studies that were relevant. Hillman and Shivers25 studied gnotobiotic rats with an artificial oral Aggregatibacter actinomycetemcomitans (A.a.) infection in a parallel, open-label, placebo-controlled study and found that A.a. counts were significantly lower in the probiotic groups versus placebo, but there was no significant difference in the Streptococcus sanguinis—either the parent strain, hydrogen peroxide deficient mutant, or revertant of the mutant—between the groups. They had already identified that S. sanguinis and Streptococcus uberis could inhibit the growth of periodontopathogens. This was based on the production of hydrogen peroxide. However, because colonization of A.a. also decreased with the mutants, other mechanisms beside hydrogen peroxide must also be playing a role.
Ishikawa et al26 conducted two in-vivo studies examining the potential of a Lactobacillus salivarius strain to suppress periodontopathogens and improve periodontal health. They did not find significant changes in the total number of bacteria, mutans streptococci, or lactobacilli; but they did ascertain a significant reduction in numbers of black-pigmented anaerobic rods for the probiotics groups in their parallel open-label study. In their second double-blind, placebo-controlled, parallel study, they found a significant decrease in the total amount of subgingival bacteria, which persisted for up to 4 weeks after discontinuation of the tablets; and although it did not alter levels of subgingival Tannerella forsythensis, there was a significant decrease in Porphyromonas gingivalis immediately after stopping the probiotics treatment. However, this decrease did not persist.
Krasse et al27 studied L. reuteri in the treatment of recurrent gingivitis via a parallel, double-blind, randomized, placebo-controlled study on adults with gingivitis. They found significantly higher reduction in gingivitis in one probiotic group (strain 1) and a significant reduction in plaque scores for both probiotic groups. The authors concluded that L. reuteri is effective in reducing gingivitis and plaque scores, but the differences are small. Kang et al28 found a significant reduction in plaque score for the probiotic group in their study of the ability of Weissella cibaria in vivo to reduce dental plaque. Earlier they had determined by isolating W. cibaria that it exhibited profound inhibitory effects on the formation of S. mutans biofilms and on the proliferation of S. mutans in vitro. Their results indicate that the W. cibaria may possess the ability to inhibit biofilm formation in vitro and in vivo.
Despite all of the studies on lactobacilli in periodontal infections, Kõll-Klais et al29 demonstrated that the composition of Lactobacillus spp. in the oral cavity differs in respect to periodontal health and habitat, with findings suggesting that lactobacilli rarely colonize subgingival sites but instead colonize the saliva more. Teughels et al30 examined seven presumed beneficial oral bacteria for their ability to interfere with the colonization of periodontopathogens. Among them were S. sanguinis KTH-4, S. salivarius TOVE, and S. mitis BMS, three bacterial spp. that appear to be effective in-vitro inhibitors of periodontopathogens partially caused by direct interbacterial interactions, environmental conditioning, and interaction with epithelial cells. The authors thought that the application of these three beneficial bacterial spp. after mechanical debridement would enhance the microbial shift away from periodontopathogens in an in-vivo Beagle dog model. They found the post-treatment attachment level was slightly lower but not statistically significant for the treatments, which included the application of the beneficial species; they attributed these findings to the lack of oral hygiene. Yet the difference between root planing alone and root planing with the application of the bacterial mixture for sites with bleeding on probing was statistically significant. This result suggests the promise of application of beneficial bacteria as an adjunct to root planing (Table 2).
In more recent studies, Shimauchi et al31 conducted a double-blind, randomized, placebo-controlled clinical trial in healthy volunteers without severe periodontitis in an effort to evaluate whether the oral administration of tablets containing L. salivarius would change the clinical parameters of periodontal tissues and the expression of salivary inflammatory markers. They found that periodontal clinical parameters improved in both groups after an 8-week intervention, and that current smokers in the test group showed a significantly greater improvement in plaque index and probing pocket depth as compared to the placebo group. Salivary lactoferrin was also significantly decreased in the test-group smokers. Zhu et al32 studied whether bio-yogurt and probiotics isolated from yogurt have antimicrobial activity against periodontal pathogens in vitro. They hypothesized that the improvement may be attributed to the direct and selective antimicrobial activity of probiotics against periodontal pathogens. The found that fresh yogurt inhibited all the periodontal pathogens studied, while heat-treated yogurt showed lower antimicrobial activity. Neither inhibited the “protective bacteria” S. sanguinis. Antimicrobial properties were reduced when both probiotics and periodontal pathogens were inoculated simultaneously versus when the probiotics were inoculated first. Slawik et al33 tested the hypothesis that the consumption of a probiotic product may reduce the risk of gingivitis. They found that bleeding upon probing and gingival crevicular fluid volume were lower in the test group. They concluded that the daily consumption of probiotic milk reduces the effects of plaque-induced gingival inflammation associated with a higher plaque score (Table 2).
Probiotics and Prebiotics
The role of prebiotics is also being considered when combined with probiotics. Prebiotics’ effects are caused by the metabolism of the bacteria they promote. They must be able to escape digestion in the upper gastrointestinal tract to reach the lower gastrointestinal tract and be used by the bacteria in the colon, ie, bifidobacteria and lactobacilli. Their effects depend on the solubility, distribution and branching, and length of chains of the molecules.34 Prebiotic fermentation results in the production of increased levels of hydrogen and carbon dioxide and of bacterial cell mass.35 Prebiotics do not undergo any changes during cooking. Clinical trials have shown that prebiotics can modify the composition of the intestinal microbiota into a more protective intestinal bacteria and alter the systemic and mucosal immune responses of the host.36-38 However, there are no studies investigating whether prebiotics have any function in enhancing probiotic activity in the oral cavity.39
Although the authors do not believe that prebiotics alone could add benefit when used in the mouth, they suggest that consuming them may stimulate the putative probiotic strains to remain longer in the mouth and thereby confer benefits. Clearly, the role of prebiotics in the oral cavity needs further exploration.
Probiotics Products
A variety of probiotic products for oral care are available in Asia, Europe, and the United States from different manufacturers. These include: PerioBalance® lozenges (GUM®, www.periobalance.com), which are said to promote healthy teeth and gums, reduce plaque, and fight bad breath; several different products from Oragenics (www.oragenics.com), including ProBiora3®, which the company claims promotes fresh breath, whiter teeth, and gum and tooth health, as well as consumer products EvoraPlus (for adults), EvoraPro (professional use), EvoraKids (for children), and EvoraPets (for dogs and cats); Compete50 Probiotic mouthwash (Denteme, www.denteme.com), which is claimed to reduce plaque formation; KForce Breath Guard mouthwash and lozenges (BreezeCare, www.breezecare.com), which the company says offers protection against halitosis and tongue coating; and various probiotic forms of BLISK12 (BLISK12, www.blisk12.com).
In addition, there are traditional remedies said to have probiotic properties. These include: kombucha, a fermented tea thought to originate in Russia or China; water kefir, which is also known as tibicos or Japanese water crystals, and is a probiotic beverage similar to kombucha; and ginger beer, a traditional culture of bacteria and yeast with powdered ginger and sugar.40
Conclusion
Probiotics, which are now commonly used for gastrointestinal health, may also have a role to play in the promotion of oral health. However, recommendations made for the gastrointestinal tract are not necessarily applicable to the oral cavity, whose complex microbial ecosystem makes it potentially difficult to target. Numerous studies have been undertaken to explore the use of probiotics to treat or change the microbial makeup of infectious diseases in the mouth, ie, periodontal disease and dental caries. The in-vitro potential of probiotics needs to be established and then clinical testing can begin.
Some considerations proposed by Teughels et al41 include: 1) examining pre-treatment to reduce levels of oral indigenous microbiota; 2) exploring the existence of probiotics in the indigenous microbiota, not just concentrating on lactobacilli; 3) not using probiotic therapy to permanently alter the oral microbiota; and 4) making clinicians and patients aware that probiotics are not regulated as rigorously as medications, and therefore may be ineffective or contain varying amounts of bacteria.
Despite the studies that have explored the use of probiotics in oral healthcare, it is still premature to make a conclusion on the existing results. Future research in better-designed clinical trials is needed to elucidate the role of probiotics in the oral cavity. With a better understanding of probiotics’ role in oral healthcare, it may be possible that over-the-counter products can be incorporated into practice. Together with good oral hygiene practices, probiotics use may become another useful method to help promote gingival and tooth health.
DISCLOSURE
The authors report no affiliation with any of the companies mentioned in this article.
ABOUT THE AUTHORS
Suellan Go Yao, DMD
Clinical Instructor, Columbia University College of Dental Medicine, Department of Periodontics, New York, New York; Private Practice, New York, New York
James Burke Fine, DMD
Associate Dean for Postdoctoral Education, Professor of Clinical Dentistry and Postdoctoral Director of the Division of Periodontics, Columbia University College of Dental Medicine, New York, New York; Attending Dental Surgeon, Presbyterian Hospital Dental Service, New York, New York; Private Practice, limited to Periodontics, Hoboken, New Jersey; faculty practice, Columbia University
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
REFERENCES
1. FAO/WHO. Health and nutritional properties of probiotics in food including powder milk with live Lactic Acid Bacteria. Report of a Joint FAO/WHO expert consultation on evaluation of health and nutritional properties of probiotics in food including powder milk with live lactic acid bacteria. London, Ontario, Canada: Food and Agriculture Organization/World Health Organization; 2001.
2. Metchnikoff E. Lactic acid as inhibiting intestinal putrefaction. In: Metchnikoff E, Mitchell PC, eds. The Prolongation of Life: Optimistic Studies. London: W. Heinemann; 1907:161-183.
3. Gibson GR, Roberforid MB. Dietary modulation of the human colonic microbiota: introducing the concept of prebiotics. J Nutr. 1995;125(6):1401-1412.
4. Moshfegh AJ, Friday JE, Goldman JP, Ahuja JK. Presence of inulin and oligofructose in the diets of Americans. J Nutr. 1999;129(7 suppl):1407S-1411S.
5. Andersson H, Asp NG, Bruce A, et al. Heath effects of probiotics and prebiotics: a literature review on human studies. Scan J Nutr. 2001;45:58-75.
6. Papapanou PN. Epidemiology of periodontal diseases: an update. J Int Acad Periodontol. 1999;1(4):110-116.
7. Miller WD. Micro-Organisms of the Human Mouth. Philadelphia, PA: SS White Dental MFG Co; 1890.
8. Beighton D. The complex oral microflora of high-risk individuals and groups and its role in caries process. Community Dent Oral Epidemiol. 2005;33(4):248-255.
9. Hedberg M, Hasslof P, Sjöström I, et al. Sugar fermentation in probiotic bacteria—an in vitro study. Oral Microbiol Immunol. 2008;23(6):482-485.
10. Bonifait L, Chandad F, Grenier D. Probiotics for oral health: myth or reality? J Can Dent Assoc. 2009;75(8):585-590.
11. Näse L, Hatakka K, Savilahti E, et al. Effect of long-term consumption of a probiotic bacterium, Lactobacillus rhamnosus GG, in milk on dental caries and caries risk in children. Caries Res. 2001;35(6):412-420.
12. Meurman JH, Antila H, Korhonen A, Salminen S. Effect of Lactobacillus rhamnosus strain GG (ATCC 53103) on the growth of Streptococcus sobrinus in vitro. Eur J Oral Sci. 1995;103(4):253-258.
13. Ahola AJ, Yli-Knuuttila H, Suomalainen T, et al. Short-term consumption of probiotic-containing cheese and its effect on dental caries risk factors. Arch Oral Biol. 2002;47(11):799-804.
14. Montalto M, Vastola M, Marigo L, et al. Probiotic treatment increases salivary counts of lactobacilli: a double-blind, randomized, controlled study. Digestion. 2004;69(1):53-56.
15. Nikawa H, Makihira S, Fukushima H, et al. Lactobacillus reuteri in bovine milk fermented decreases the oral carriage of mutans streptococci. Int J Food Microbiol. 2004;95(2):219-223.
16. Calgar E, Cildir SK, Ergeneli S, et al. Salivary mutans streptococci and lactobacilli levels after ingestion of the probiotic bacterium Lactobacillus reuteri ATCC 55730 by straws or tablets. Acta Odontol Scand. 2006;64(5):314-318.
17. Calgar E, Sandalli N, Twetman S, et al. Effect of yogurt with Bifidobacterium DN-173 010 on salivary mutans streptococci and lactobacilli in young adults. Acta Odontol Scand. 2005;63(6):317-320.
18. Fitzgerald RJ, Fitzgerald DB, Adams BO, Duany LF. Cariogenicity of human oral lactobacilli in hamsters. J Dent Res. 1980;59(5):832-837.
19. Busscher HJ, Mulder AF, Van der Mei HC. In vitro adhesion to enamel and in vivo colonization of tooth surfaces by Lactobacilli from a bio-yoghurt. Caries Res. 1999;33(5):403-404.
20. Petti S. Tarsitani G, D’Arca AS. A randomized clinical trial of the effect of yoghurt on the human salivary microflora. Arch Oral Biol. 2001;46(8):705-712.
21. Hillman JD, Chen A, Duncan M, Lee SW. Evidence that L-(+)-lactate dehydrogenase deficiency is lethal in Streptococcus mutans. Infect Immun. 1994;62(1):60-64.
22. Hillman JD, Mo J, McDonell E, et al. Modification of an effector strain for replacement therapy of dental caries to enable clinical safety trials. J Appl Microbiol. 2007;102(5):1209-1219.
23. Roberts FA, Darveau RP. Beneficial bacteria of the periodontium. Periodontol 2000. 2002;30:40-50.
24. Teughels W, Van Essche M, Sliepen I, Quirynen M. Probiotics and oral healthcare. Periodontol 2000. 2008;48:111-147.
25. Hillman JD, Shivers M. Interaction between wild-type, mutant and revertant forms of the bacterium Streptococcus sanguis and the bacterium Actinobacillus actinomycetemcomitans in vitro and in the gnotobiotic rat. Arch Oral Biol. 1988;33(6):395-401.
26. Ishikawa H, Aiba Y, Nakanishi M, et al. Suppression of periodontal pathogenic bacteria in the saliva of humans by the administration of Lactobacillus salivarius TI 2711. J Jpn Soc Periodontol. 2003;45:105-112.
27. Krasse P, Carlsson B, Dahl C, et al. Decreased gum bleeding and reduced gingivitis by the probiotic Lactobacillus reuteri. Swed Dent J. 2005;30(2):55-60.
28. Kang MS, Chung J, Kim SM, et al. Effect of Weissella cibaria isolates on the formation of Streptococcus mutans biofilm. Caries Res. 2006;40(5):418-425.
29. Kõll-Klais P, Mandar R, Leibur E, et al. Oral lactobacilli in chronic periodontitis and periodontal health: species composition and antimicrobial activity. Oral Microbiol Immunol. 2005;20(6):354-361.
30. Teughels W, Newman MG, Coucke W, et al. Guided periodontal pocket recolonization: a proof of concept. J Dent Res. 2007;86(11):1078-1082.
31. Shimauchi H, Mayanagi G, Nakaya S, et al. Improvement of periodontal condition by probiotics with Lactobacillus salivarius WB21: a randomized, double-blind, placebo-controlled study. J Clin Periodontol. 2008;35(10):897-905.
32. Zhu Y, Xizo L, Shen D, Hao Y. Competition between yogurt probiotics and periodontal pathogens in vitro. Acta Odontol Scand. 2010;68(5):261-268.
33. Slawik S, Staufenbiel I, Schilke R, et al. Probiotics affect the clinical inflammatory parameters of experimental gingivitis in humans. Eur J Clin Nutr. 2011;65(7):857-863.
34. Rossi M, Corradini C, Amaretti A, et al. Fermentation of fructooligosaccharides and inulin by bifidobacteria: a comparative study of pure and fecal cultures. Appl Environ Microbiol. 2005;71(10):6150-6158.
35. Cummings JH, Macfarlane GT, Englyst HN. Prebiotic digestion and fermentation. Am J Clin Nutr. 2001;73(2 suppl):415S-420S.
36. Hedin C, Whelan K, Lindsay JO. Evidence for the use of probiotics and prebiotics in inflammatory bowel disease: a review of clinical trials. Proc Nutr Soc. 2007;66(3):307-315.
37. Leenen CH, Dieleman LA. Inulin and oligofructose in chronic inflammatory bowel disease. J Nutr. 2007;137(11 suppl):2572S-2575S.
38. Looijer-van Langen MA, Dieleman LA. Prebiotics in chronic intestinal inflammation. Inflamm Bowel Dis. 2009;15(3):454-462.
39. Stamatova I, Meurman JH. Probiotics and periodontal disease. Periodontol 2000. 2009;51:141-151.
40. Chatterjee A, Bhattacharya H, Kandwal A. Probiotics in periodontal health and disease. J Indian Soc Periodontol. 2011;15(1):23-28.
41. Teughels W. Loozen G, Quirynen M. Do probiotics offer opportunities to manipulate the periodontal oral microbiota? J Clin Periodontol. 2011;38(suppl 11):159-177.