You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Tooth whitening or tooth bleaching is a popular dental treatment that continues to grow in response to public demand for esthetics. Despite its recent popularity, tooth whitening dates back 150 years. As early as 1848, non-vital tooth whitening was practiced. Vital teeth were also treated in-office as early as 1868. In 1877, Chapple first published a dental report on tooth whitening using oxalic acid.1 In 1918, Abbot used 35% hydrogen peroxide (HP) accelerated by heat from a light source, and this technique became well established.1 In 1968, orthodontist William Klusmier used Proxigel (10% carbamide peroxide [CP]), an oral antiseptic, with a custom-fitted tray overnight for 2 to 5 weeks.2 This concept was embraced by the profession in the late 1990s with the first publication on the technique by Haywood and Heymann.2
In-office treatment resurged in the early 2000s. Today, in-office systems are in demand due to their high-tech appeal and the manufacturers’ promises of excellent results in less time. Over-the-counter (OTC) whitening systems are in high demand due to their availability and low cost.
How Whitening Works
The tooth-whitening process is not fully understood. Research shows that the bleaching material penetrates through intact enamel and dentin into the pulp in 5 to 15 minutes.3 The whitening process is designed to enable the oxidizing agent to penetrate into the tooth to allow a chemical reaction to occur and dislodge or decolor the chromatic particles. The CP penetrates into the tooth, and it is broken down into urea and HP (Figure 1).1 The urea further breaks down into ammonia and carbon dioxide. The role of urea is to prolong the shelf-life of the product. The HP breaks down into oxygen and water and liberates the chemically reactive free radical perhydroxyl (HO2-) with great oxidative power. As shown in Figure 1, 10% CP corresponds to about 3.5% HP; therefore, 20% CP corresponds to 7% HP, and 30% CP corresponds to about 10% HP. The peroxide not only removes discoloration from within the tooth, it also changes the color of dentin itself.4
Indications and Prognosis
Tooth whitening can be indicated as a minimally invasive technique to treat both vital and non-vital discolored teeth. Tooth discolorations can be a result of enamel mottling, tetracycline staining, trauma, developmental hypoplasia, caries demineralization, age-related extrinsic enamel staining, thinning of enamel with subsequent dentin shine-through, and staining of teeth due to smoking or food and beverage ingestion.
Tooth discolorations are classified as either intrinsic (within the dentin) or extrinsic (on or within the surface of the enamel). Intrinsic discolorations are deep within the tooth, usually a dentin discoloration. Examples of intrinsic tooth discolorations are tetracycline staining of the teeth and endodontic staining. Extrinsic discolorations are superficial in the enamel. Fluorosis, enamel hypoplasia (“white spots”), and superficial discoloration due to smoking or food and beverage ingestion are examples of extrinsic discolorations of the enamel. Caries can be both an intrinsic and extrinsic discoloration.
In some cases superficial stains or extrinsic stains may be removed by external cleaning. A comprehensive examination to include radiographs if endodontic staining or caries is suspected is critical to make recommendations for treatment. As part of a differential diagnosis, the causes of stain need to be carefully ascertained prior to tooth whitening for better predictability and to inform the patient about the prognosis of treatment.
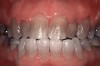
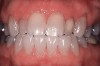
The management of yellow, light brown, and orange stains due to aging, genetics, and stains caused by chromatogenic foods and drinks is highly successful.5 It usually takes 3 to 4 weeks per arch depending on the level of staining. The treatment of brown, orange, and white stains promoted by fluorosis and stains caused by nicotine are slower to respond to tooth whitening. At times, superficial fluorosis stains cannot be completely removed with bleaching. For these cases, the mottled enamel appearance of fluorosis can be treated with a combined microabrasion-macroabrasion technique and then finished with vital bleaching.6 If neither technique provides the patient with an esthetically acceptable result, adhesive direct composite or porcelain veneers can be offered to the patient. Noteworthy is that although white spots are not removed by whitening, they become less perceptible when the remainder of the tooth is lighter.7 Patients should be informed that it typically takes 1 to 3 months of treatment per arch depending on the intensity of the nicotine or fluorosis stains. In general, tetracycline stains are tenacious and are the slowest to respond to tooth whitening. They vary in color and can be dark gray, brown, or blue. Research has shown that tooth whitening can be accomplished using 10% to 20% CP at home for 6 months in patients with tetracycline stains (Figure 2 and Figure 3),8 although it may take longer.
Precautions
There are a few contraindications for tooth-whitening treatment. At-home treatment is not indicated for patients who are allergic to the whitening ingredients. Although there is no evidence of HP as a cause of harm to a fetus or infant, it has been recommended that pregnant and lactating women not undergo whitening due to the increased potential for gingival irritation.9 Patients with history of tooth sensitivity should be cautioned that increased sensitivity might occur, and methods of decreasing tooth sensitivity during treatment should be discussed.
Types of Non-Vital Tooth-Whitening Treatment
Tooth trauma is not uncommon. Pulp responds to trauma in different ways. It can survive, die, or undergo pulp canal obliteration, which is also known as calcific metamorphosis.10 A radiograph of a single dark tooth should always be taken, because teeth may undergo pulpal necrosis without showing any symptoms other than becoming dark. Endodontically treated teeth are susceptible to discoloration from blood products in the dental tubules caused by trauma or endodontic therapy.
There are several options for treating non-vital teeth (Figure 4).11 External tooth whitening using a single-tooth tray is indicated for a tooth that becomes discolored over the years following satisfactory endodontic treatment.11 External whitening aims to avoid the removal of the resin composite from the pulp chamber, thereby avoiding having to enter the tooth and weakening it.
When the clinician has no knowledge of what has occurred during endodontic therapy, internal whitening is recommended (Figure 4). Insufficient cleaning of the pulp chamber, endodontic sealer, and dark or leaking restorations in the access opening can cause discoloration. Internal whitening can be done by applying HP into the pulp chamber and increasing the chemical reaction by the use of heat or light; this is known as the thermocatalytic technique.11 The “walking bleaching” technique uses a mixture of sodium perborate and saline solution or 10% CP. The whitening agent is placed into the chamber and sealed. This treatment requires anywhere from one to six weekly applications.
External and internal whitening can also be used in combination. The walking whitening method can be combined with the single-tooth tray, allowing the patient to whiten externally using 10% to 20% CP.
Types of Vital Tooth-Whitening Treatment
At-Home with Dentist-Prescribed Products
At-home tooth-whitening treatment is dentist-prescribed and home-applied by the patient using a fitted tray. The 10% concentration of CP used in trays overnight has been considered the “gold standard.” This technique is still the most common whitening procedure, and the literature heavily supports the efficacy and safety of this method.12 More recently, HP products have been introduced for day-wear trays. HP is active for 30 to 60 minutes. CP is active for up to 10 hours, with about 50% of the active agent being used in the first 2 hours.13 Ultimately, the patient can choose between day or night treatment. Apart from that, there is no difference in whitening efficacy when the trays are made with or without a reservoir.14
In-Office
The in-office systems typically use a high concentration of HP (15% to 40%). The HP needs to be in contact with the outer enamel surface for a period of time in order to develop its whitening potential. The oral tissues must be protected during the procedure. Then, the whitening gel is applied on the facial surfaces of the teeth for a few minutes three to four times, depending on the manufacturer’s instructions. Some manufacturers recommend that the gel be exposed to a light source such as light-emitting diodes (LED) and mercury metal halide light to accelerate the whitening process. The use of a light source in order to increase the tooth-whitening effect remains debatable. However, there is a strong body of evidence that supports the effectiveness of in-office whitening, whether used with or without the whitening light.15
The dentist is in complete control of the process throughout the in-office treatment, providing the option of termination at any time. Usually, color change results can be observed after a single visit. The high cost is a disadvantage, and patients usually desire to continue whitening at home. One study showed that 5 days of at-home whitening with 10% CP for 8 hours per day produces tooth-whitening results similar to one 1-hour in-office treatment with 25% HP. In addition, after the one in-office treatment, all patients wanted to continue to whiten their teeth at home.16
At-Home with OTC Products
Teeth can also be whitened at-home without professional supervision using OTC products. OTC products include whitening strips, paint-on brushes, rinses, toothpastes, dental floss, and chewing gums. The main advantage of OTC products is their low cost. Do they all remove intrinsic stains? There is strong evidence supporting the effectiveness of whitening strips for removing intrinsic stains, while whitening toothpastes, gum, and floss are removal agents for superficial stains; rinses and paint-on brushes have some whitening effect, but it is without clinical relevance.17 It is necessary, however, for users to be careful with self-applied whitening products that contain peroxide, because they have the potential to produce oral irritation and tooth hypersensitivity.
With any of the aforementioned types of vital tooth-whitening treatments, the choice is based on the patient’s preference, financial situation, and motivation to comply with the treatment protocol. Patients who desire to finish whitening in a short period of time are good candidates for in-office treatment, even though it may require more than one visit to achieve maximum lightness. Those who present financial limitations may opt to whiten using OTC products.
Tooth Sensitivity Management
Studies have reported that tooth sensitivity during whitening is usually mild to moderate but transient.18 Early reports stated that tooth sensitivity and gingival irritation were experienced in 15% to 78% of patients undergoing external tooth whitening. More current research has reported patients’ tooth sensitivity to be mild and experienced by 25% to 35% of the study subjects.16 This reduction in tooth sensitivity is due to the inclusion of desensitizing agents such as ACP (amorphous calcium phosphate), fluoride, and potassium nitrate in the whitening gel formulas. Gingival irritation does not seem to be a concern any longer16; it can be avoided when whitening at home if the patient trims the tray and removes any whitening gel excess away from the gingival tissue. In-office, the tissue must be very well isolated.
Noteworthy is that there is no evidence of any long-term consequences that have resulted from tooth sensitivity and/or gingival irritation.19
Patients experiencing tooth sensitivity can be instructed to wear the whitening tray every other night, or to wear it a couple of hours a day instead of overnight. Another alternative is to apply desensitizing gels with potassium nitrate, potassium fluoride, or high-concentration fluoride toothpaste in the tray and wear it for 30 minutes prior to treatment. A reduction in the concentration of CP may also help.
Further Considerations
Concerns have been raised regarding the effect of whitening on enamel microhardness, composite bond strength, and genotoxicity. Although in-vitro studies showed a decrease in enamel microhardness, clinical studies did not show any difference in enamel hardness after tooth whitening. The overwhelming majority of studies showed a reduction of resin composite bond strength when that procedure is performed within 1 day after tooth-whitening treatment.20 Those authors also commented that the bond strength returns to normal after a time lapse. Consequently, studies recommend delaying placement of resin composite restorations from 1 to 3 weeks after tooth whitening.20 It is common practice to wait at least 2 weeks in order to avoid any debonding of material and to stabilize tooth color. HP is genotoxic in-vitro, but such activity is not expressed in-vivo. Clinical studies have not shown the development of pre-neoplastic or neoplastic oral lesions.
Overall, tooth-whitening products are safe for use by the human population.21,22
References
1. Fasanaro TS. Bleaching teeth: history, chemicals, and methods used for common tooth discolorations. J Esthet Dent. 1992;4(3):71-78.
2. Haywood VB, Heymann HO. Nightguard vital bleaching. Quintessence Int. 1989;20(3):173-176.
3. Cooper JS, Bokmeyer TJ, Bowles WH. Penetration of the pulp chamber by carbamide peroxide bleaching agents. J Endod. 1992;18(7):315-317.
4. McCaslin AJ, Haywood VB, Potter BJ, et al. Assessing dentin color changes from nightguard vital bleaching. J Am Dent Assoc. 1999;130(10):1485-1490.
5. Haywood VB, Leonard RH, Nelson CF, Brunson WD. Effectiveness, side effects and long-term status of nightguard vital bleaching. J Am Dent Assoc. 1994;125(9):1219-1226.
6. Strassler HE. Clinical case report: treatment of mild-to-moderate fluorosis with a minimally invasive treatment plan. Compend Contin Educ Dent. 2010;31(1):54-58.
7. Leonard RH Jr, Bentley C, Eagle JC, et al. Nightguard vital bleaching: a long-term study on efficacy, shade retention, side effects, and patients’ perceptions. J Esthet Restor Dent. 2001;13(6):357-369.
8. Haywood VB, Leonard RH, Dickinson GL. Efficacy of six-months nightguard vital bleaching of tetracycline-stained teeth. J Esthet Dent. 1997;9(1):13-19.
9. Haywood VB. Commonly asked questions about nightguard vital bleaching. J Indiana Dent Assoc. 1993;72(5):28-33.
10. Feiglin B. Dental pulp response to traumatic injuries—a retrospective analysis with case reports. Endod Dent Traumatol. 1996;12(1):1-8.
11. Haywood VB, DiAngelis AJ. Bleaching the single dark tooth. Inside Dentistry. 2010;6(8):42-52.
12. Niederman R, Tantraphol MC, Slinin P, et al. Effectiveness of dentist-prescribed, home-applied tooth whitening. A meta analysis. J Contemp Dent Pract. 2000;1(4):20-36.
13. Matis BA. Tray whitening: What the evidence shows. Compend Contin Educ Dent. 2003;24(4A):354-362.
14. Matis BA, Hamdan YS, Cochran MA, Eckert GJ. A clinical evaluation of a bleaching agent used with and without reservoirs. Oper Dent. 2002;27(1):5-11.
15. Buchalla W, Attin T. External bleaching therapy with activation by heat, light or laser—a systematic review. Dent Mater. 2007;23(5):586-596.
16. da Costa JB, McPharlin R, Paravina RD, Ferracane JL. Comparison of at-home and in-office tooth whitening using a novel shade guide. Oper Dent. 2010;35(4):381-388.
17. Demarco FF, Meireles SS, Masotti AS. Over-the-counter whitening agents: a concise review. Braz Oral Res. 2009;23 Suppl 1:64-70.
18. Tredwin CJ, Naik S, Lewis NJ, Scully C. Hydrogen peroxide tooth-whitening products: review of adverse effects and safety issues. British Dent J. 2006;200(7):371-376.
19. Li Y. The safety of peroxide-containing at-home tooth whiteners. Compend Contin Educ Dent. 2003;24(4A):384-389.
20. Attin T, Hannig C, Wiegand A, Attin R. Effect of bleaching on restorative materials and restorations—a systematic review. Dent Mater. 2004;20(9):852-861.
21. Munro IC, Williams GM, Heymann HO, et al. Tooth-whitening products and the risk of oral cancer. Food Chem Toxicol. 2006;44(3):301-315.
22. Mahony C, Felter SP, McMillan DA. An exposure-based risk assessment approach to confirm the safety of hydrogen peroxide for use in home tooth bleaching. Regul Toxicol Pharmacol. 2006;44(2):75-82.
About the Author
Juliana B. da Costa, DDS, MS
Associate Professor
Preclinical Director
Department of Restorative Dentistry
Oregon Health & Science University
School of Dentistry
Portland, Oregon