You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
High-tech advances in dentistry are transforming how patients experience dental treatment. Technology offers the opportunity to reduce patient treatment time while improving the treatment outcome: a very desirable combination of features for both the dentist and the patient. Dental lasers are an innovative technology that may provide more efficient, more comfortable, and more predictable treatment outcomes for patients. Dental lasers are based on Albert Einstein’s theory of stimulated emission of radiant energy.1 An active medium is stimulated to generate photons of energy that are released in a beam with a specific wavelength unique to the active medium. Lasers are usually identified by the active medium that is used to generate the radiant energy.2 Dental lasers produce light energy within a narrow frequency range. For example, all neodymium:yttrium-aluminum-garnet (Nd:YAG) lasers of similar design produce light with a wavelength of 1.064 µm.
Laser light energy is distinguished from ordinary light by two properties. The energy emitted by a laser is essentially a light of one color (monochromatic) and, therefore, of a single wavelength.2 In addition, laser light energy is coherent in that each wavelength is identical in physical size and shape. The photons can be collimated into an intensely focused energy beam, which will interact with a target tissue. Dental lasers have a surgical capability because dental tissues have a specific affinity for absorbing laser energy of a specific wavelength.2 The wavelength of the laser is the primary determinant of the degree to which the laser energy is absorbed by the target tissue. Specific target tissues differ in their affinity for specific wavelengths of laser energy. Selection of a specific laser, therefore, is dependant on the desired target tissue.
The underlying principle of using the least amount of laser energy to achieve a treatment objective is very important.3 The primary interaction of a laser with target tissues is photothermal. Laser energy is absorbed by the target tissue and significantly elevates the temperature of the tissue.4,5 When the tissue temperature exceeds 100oC the intracellular water boils causing soft tissue ablation.6,7 If laser energy continues to be absorbed, carbonization or burning occurs with the risk of potential soft-tissue damage. The parameters of beam size (fiber diameter), power setting, and duration of exposure must be monitored carefully to ensure the optimum tissue effects. The optimum tissue response to a laser is vaporization of the target tissue without discoloration or charring. Brown or blackened tissue is a result of absorbing too much heat because of power settings that are too high or slow movement of the fiber tip across the tissue surface.
TYPES AND FEATURES OF DENTAL LASERS
A number of factors should be weighed when considering implementing laser systems into a dental practice. No single wavelength will treat all dental tissues or diseases optimally. Given the variety of available wavelengths, the clinician should first determine the clinical treatment goals and then select the specific laser (wavelength) best suited to achieve them. This requires the clinician to decide what specific procedures are likely to be performed before purchasing a dental laser.
Several types of laser systems are available, with some specific to either hard- or soft-tissue applications. Hard-tissue lasers are capable of treatment procedures for bone and tooth structure. Soft-tissue lasers are capable of treatment procedures for gingival tissues. Laser systems are available in a range of costs, but all require considerable capital investment and educational commitment to effectively integrate into a practice.
Lasers for hard-tissue procedures are considerably larger and more expensive than lasers for soft-tissue procedures. Hard-tissue lasers, designed for the preparation of teeth, are limited to creating the cavity designs predicated by most direct restorative materials. Although very useful for conservative preparations, their use for more advanced cavity preparations for indirect restorations is limited and time-consuming at best. A significant advantage to the use of a hard-tissue laser is the potential to anesthetize the tooth with the laser before completing the preparation. This can result in a very comfortable patient experience without the need for an anesthetic injection. This can be a significant advantage for practices with a high demand for conservative restorative procedures, such as a pediatric practice. In general, soft-tissue lasers have considerably greater applications for most dental practices compared with hard-tissue lasers.
Ergonomic features of the laser unit should be a significant factor in deciding on a particular soft-tissue laser. Many practices have invested in the latest equipment because of its potential dental treatment advantages, but then it never makes it out of the storage closet because it takes longer to set up the equipment than to accomplish the procedure with a more efficient existing instrument. For this reason, portability and ease of use are primary factors to consider. The smaller and more portable the laser unit, the easier it can be located chairside and the more likely it will be used. Additionally, the fewer cables or cords required for the unit offers a similar advantage. If one considers the power cord from the unit to the electrical outlet, the cord from the unit to the foot pedal, and the fiber from the unit to the handpiece, each cord poses a potential problem for placement of the laser in a convenient position for chairside clinical use. Battery-operated or rechargeable lasers do not require a power cord and are not limited to use near an electrical outlet. A wireless foot pedal to operate the laser is a similarly desirable feature because there is no cord limiting the distance the laser must be located from the operator’s foot.
Another consideration is the management of the fiber for laser operation. A typical soft-tissue laser has a fiber within a handpiece. The end of the fiber may need to be cleaved and stripped to expose the inner core of the fiber to prepare it for clinical use. The fiber management should be efficient and easy, and unidose fiber tips make for an efficient setup and convenient delivery system. Unidose tips preclude the need for time-consuming fiber preparation because the disposable tips are ready for clinical use immediately after they are inserted on the end of the handpiece.
Diode soft-tissue lasers are available commercially, with the desirable ergonomic features described above. At present, they are the most portable of the soft-tissue lasers. The diodes are made from semiconductor crystals and emit light when an electrical current is passed through them. The crystals will determine the specific wavelength of the diode laser. Diode lasers in the 800-nm to 830-nm range use a semiconductor active medium of aluminum, gallium, and arsenide. Diode lasers in the 980-nm range use a semiconductor active medium of indium, gallium, and arsenide.6 Diode lasers are available in several wavelengths, such as 810 nm, 940 nm, and 980 nm. These wavelengths have been selected because of their commercial availability and the energy absorption characteristics in soft tissues. Although, it has been suggested that one or the other of these wavelengths is more efficient or “better” for soft-tissue removal than another, the wavelength is only one factor in determining the power output and cutting efficiency of a diode laser. The fiber diameter and power (watts) setting are also significant factors in determining the actual cutting efficiency. In general, the smaller the fiber diameter and the higher the power density, the more efficient the laser will cut soft tissues.
There are a number of commercially available diode lasers, such as the SIROlaser (Sirona Dental Systems, LLC, Charlotte, NC), the ezlase 940 (Biolase Technology, Inc, Irvine, CA), and the Odyssey® Navigator (Ivoclar Vivadent, Inc, Amherst, NY). They are all compact, easily portable diode lasers for soft-tissue applications. The SIROlaser weighs 450 g and has an ergonomic handpiece with a finger switch and touch-screen controls. It has interchangeable optical fibers of 200 nm and 300 nm. The ezlase 940 uses a 940-nm wavelength, is compact in size, and offers 200-nm, 300-nm, and 400-nm disposable tips as well as a wireless foot switch. The Odyssey Navigator is a 3 W, 810 nm diode laser. It is very compact, weighing only 2.5 lbs. The unit has touch-screen controls, a wireless foot pedal, an ergonomic handpiece, and unidose fiber tips of 400-nm diameter. It is a rechargeable unit that can run on battery power for up to 45 minutes before recharging.
USES OF DENTAL LASERS
The ability to record the cavity preparation for a ceramic or cast restoration is a critical factor in fabricating a well-fitting result. Retraction and surgical removal of soft tissues are particular benefits of a diode laser. Soft-tissue management for a final impression is dependant on the ability to create sufficient space to visualize the prepared margins while maintaining a dry field. This is true for traditional impression materials as well as for the newer digital impression systems. These systems include chairside systems, such as CEREC® 3 (Sirona Dental Systems, LLC) and E4D Dentist™ (D4D Technologies LLC, Dallas, TX), and laboratory-direct systems, such as Lava™ Chairside Oral Scanner (C.O.S.) (3M ESPE, St. Paul, MN) and iTero™ (Cadent, Carlstadt, NJ).
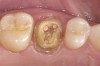
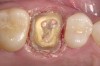
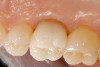
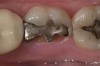
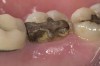
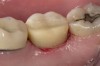
Digital impression systems are able to accurately image only those areas that are visible and isolated. A diode laser can remove obstructive soft tissues efficiently and provide a field that can be maintained free of blood and moisture.2 Therefore, these lasers can be invaluable restorative tools, making immediate analogue or digital impressions possible. Immediate restoration of teeth with ceramic materials during a single appointment is a hallmark of chairside computer-aided design/computer-aided manufacture (CAD/CAM) systems. With CAD/CAM systems, the operating field must be well isolated during the imaging process to record an accurate image of the cavity margins. Figure 1 illustrates a case of a porcelain crown with a temporary restoration after endodontic treatment. After the crown and temporary restoration were removed, the remaining cavity margin was subgingival, limiting access for imaging (Figure 2). A diode laser (Odyssey Navigator) was used to recontour the gingival tissues to establish good retraction and a dry field, and accurate images of the tooth were made immediately (Figure 3 through Figure 6). Electrosurgery has been a common choice of clinicians to excise gingival tissues effectively while simultaneously creating adequate hemostasis. Heat generation occurs to a degree where irreversible damage to the alveolar crest may result, leading to recession and exposure of restorative margins that may be objectionable to the patient.8 Careful control of the diode laser power settings and fiber tip movement ensure that the soft-tissue contours will not recede after healing and the margin placement will remain in the same position (Figure 7 and Figure 8).
Soft-tissue lasers may be considered an effective diagnostic tool as well as a therapeutic tool. A common clinical occurrence is the cuspal fracture of posterior teeth. Unfortunately, sometimes the level of fracture on the tooth is significantly subgingival and can pose a diagnostic dilemma as to the restorability of the tooth. Occasionally, by the time the patient presents for an evaluation of the problem, the soft tissues have overgrown the fractured area of the tooth, and determining the sulcus depth, available tooth structure, and potential impact on the biologic width can be difficult (Figure 9 and Figure 10). A scalpel can be used to remove the hyperplastic gingiva to gain access to the fractured tooth. However, this results in a bloody field with poor visibility. There are several reported advantages of lasers compared with the use of a scalpel. These include increased coagulation that yields a dry surgical field and better visualization; tissue surface sterilization with a reduction in bacterial counts; decreased swelling, edema, and scarring; decreased pain; faster healing; and increased patient acceptance.5,9 A soft-tissue laser can serve as a diagnostic tool, as the hyperplastic tissue can be excised easily, maintaining a blood-free environment. This affords better visibility for evaluating the depth of the tooth fracture (Figure 11). If sufficient tooth remains, the tooth may be restored or temporized immediately (Figure 12).
Chromophores are tissue elements that absorb laser light energy, such as hemoglobin, melanin, or other pigmented proteins.7 Because they are not present in dental hard tissues, metal alloys, or porcelain, the diode laser has little affinity for these structures and has no apparent affect on them. This allows for the safe use of the diode laser near these materials and structures.
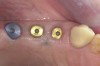
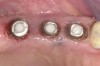
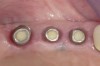
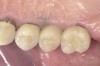
Soft-tissue lasers are also useful for creating the desired soft-tissue contours around implants because the diode laser does not interact with metals. At times, soft-tissue contours around healing abutments do not conform to the desired cervical contour of the planned restoration, such as when the gingival tissues heal against the parallel-sided healing abutment and restrict the cervical space for the abutment and crown. This contour may prevent complete seating of the final restoration as the cervical contours are developed in the final restoration (Figure 13). A diode laser can be used to modify the gingival contour to match the crown contour at delivery or temporization to create the desired tissue contours. The fine tip of a laser offers excellent control to create the desired tissue contours (Figure 14 through Figure 16).
A unique aspect of working with a dental laser is that it cuts only at the end of the tip, which influences the angle and movement of the fiber tip across the tissues for optimal effectiveness. There is no side-cutting effect, and some practice is required to learn the proper fiber tip alignment. Laser energy flows freely from the fiber tip of a diode laser unless the end of the fiber has been initiated, or carbonized, concentrating the energy at the tip of the fiber. An initiated, or carbonized, fiber is used for surgical procedures. This causes the laser energy to be absorbed at the fiber tip and allows for surgical removal of tissue by using heat. However, there are applications for a noninitiated fiber tip as well. A noninitiated fiber tip allows the laser energy to escape the fiber end freely and flood the irradiated tissue with laser energy.
A noninitiated fiber can be used to desensitize aphthous ulcers. Patients with recurrent aphthous ulcers find it difficult to eat and even speak at times because of the pain associated with the ulcer. There are several alternatives to offer some degree of pain control to patients through topical agents. However, according to manufacturers’ recommendations, the diode laser can be used to desensitize the ulcer throughout the healing period. It is used in a noncontact technique where the power setting is increased and the distance from the fiber tip to the ulcer is decreased over several applications to desensitize the nerve endings in the ulcerated area. Anecdotal evidence has shown that this procedure results in pain relief over the remaining period of healing.
CONCLUSION
Laser technology is available for both hard- and soft-tissue applications. Most general practices will realize more soft-tissue procedures and applications for laser technology than hard-tissue ones. Laser technology can be very valuable for creating well-isolated and immediately dry operating fields for restorative treatment. Dental lasers are an innovative technology that may provide more efficient, more comfortable, and more predictable treatment outcomes for patients.
DISCLOSURE
The author has received grant/research support from Ivoclar Vivadent, Inc.
REFERENCES
1. Maiman TH. Stimulated optical radiation in ruby. Nature. 1960;187(4736):493-494.
2. Cobb CM. Lasers in periodontics: a review of the literature. J Periodontol. 2006;77(4):545-564.
3. Dederich D. Laser/tissue interaction. Alpha Omegan. 1991;84(4):33-36.
4. White JM, Goodis HE, Kudler JJ. Thermal effects on intraoral soft tissue, teeth, and bone in vitro. In: Proceedings of the Third International Congress on Lasers in Dentistry. Salt Lake City, UT:University of Utah Printing Services; 1992:189-190.
5. Wigdor HA, Walsh JT Jr, Featherstone JD, et al. Lasers in dentistry. Lasers Surg Med. 1995;16(2):103-133.
6. Coluzzi DJ. Lasers in dentistry. Compend Contin Educ Dent. 2005;26(6A Suppl):429-436.
7. Parker S. Verifiable CPD paper: laser-tissue interaction. Br Dent J. 2007;202(2):73-81.
8. Kalkwarf KL, Krejci RF, Edison AR, et al. Lateral heat production secondary to electrosurgical incisions. Oral Surg Oral Med Oral Pathol. 1983;55(4):344-348.
9. Bader HI. Use of lasers in periodontics. Dent Clin North Am. 2000;44(4):779-792.
About the Author
Dennis J. Fasbinder, DDS
Director, Advanced Education in General Dentistry Program, and Clinical Professor, University of Michigan School of Dentistry, Ann Arbor, Michigan; Private Practice, Ann Arbor, Michigan; Founding Member, 21st Century Practice Solutions, Dallas, Texas