You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Regarding dentistry's spectrum of state-of-the-art treatments, historically, many clinicians and patients have had the perception that complete dentures are at the bottom, whereas cosmetic dentistry is at the top. Today, implant dentistry has closed this gap in the spectrum. An implant-supported fixed prosthesis is the highest state-of-the-art solution that we can offer to our patients who have no teeth or a failing dentition. However, an understanding of fundamental removable prosthodontic principles is critical to the predictability and success of these implant-retained prostheses. According to Walter "Jack" Turbyfill, DDS, "The use of implants will never relieve the dentist of making sure the physiology and the mechanics of the prosthesis is correct."
Restoring the completely edentulous patient presents many challenges. The tooth position, esthetics, phonetics, occlusal plane, vertical dimension of occlusion, and condylar position are all still determined using decades-old removable prosthodontic principles.1Unfortunately, many of these reference points are lost with complete edentulism. Even existing prostheses can falsely represent what patients need or want. In addition, the dentist can be faced with other challenges, including the psychological and emotional effects of tooth loss, medications causing xerostomia, and neuromuscular incoordination.2 It's no wonder that many of today's clinicians tend to shy away from restoring these patients with conventional removable prostheses.
The step-by-step analog approach of fabricating conventional complete dentures has not changed much over the years. Border-molded impressions lead to master casts, upon which baseplates and wax rims are fabricated.3 Excellent communication between the restoring dentist and the laboratory technician is crucial at this stage and often falls short with respect to the anticipated location of anterior teeth, vertical dimension of occlusion, and condylar position. Even with the availability of digital dentistry, it is important for clinicians to be able to obtain the chairside records accurately, evaluate proper esthetics and phonetics, and apply problem-solving for potential mishaps, such as when the teeth are not in the correct position.
Whether complete dentures are used as a definitive restoration, a transitional restoration, or a diagnostic tool, their fabrication must follow a systematic approach. This step-by-step approach requires specific elements to ensure the predictability and success of the final prostheses, including the following:
• Establishing the maxillary incisal edge position
• Establishing the mandibular incisal edge position
• Determining the appropriate vertical dimension of occlusion
• Obtaining an accurate centric relation bite record
• Mounting the casts on an articulator
• Verifying proper phonetics
Establish the Maxillary Incisal Edge Position
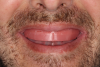
The starting point for complete denture fabrication is determining where the upper anterior teeth need to be in both the vertical and horizontal dimensions. This is accomplished by utilizing a maxillary baseplate and wax rim (Figure 1). The wax rim is contoured and adjusted so that it communicates necessary landmarks to the laboratory technician, including the following:
• Horizontal and vertical maxillary incisal edge position
• Maxillary midline
• Buccal corridors
• Maxillary occlusal plane
• High smile line
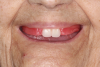
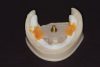
In order to more easily confirm the position of the denture teeth, it is often desirable to set them into the wax rim (Figure 2). Fricative sounds, such as "F" and "V," are used to confirm the ideal maxillary incisal edge position, which should just touch the wet-dry line of the lower lip.4 To observe this, the clinician can have the patient count from 50 to 60 at a conversational speed. Photography, including images of the rest position, high smile, and profile smile, as well as videos of the fricative sounds, should be used as additional tools for communication with the laboratory technician.
Establish the Mandibular Incisal Edge Position
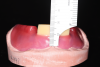
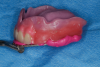
Once the maxillary incisal edge position has been determined, the next step is to establish the mandibular incisal edge position, which is accomplished by using a mandibular baseplate and wax rim. This is fabricated with "speaking wax" in the anterior region (Figure 3). The height of the mandibular wax rim in the anterior region should be 18 mm from the bottom of the vestibule to the anticipated incisal edge position, which approximates the desired location. To prevent interference with mandibular movement during phonetic tests, the posterior part of the rim is reduced below the occlusal plane, and then the rim is notched to accept bite registration material. The mandibular speaking wax is used as the starting point for determining the appropriate vertical dimension of occlusion.
Determine the Appropriate Vertical Dimension of Occlusion
According to the Academy of Prosthodontics' glossary of prosthodontic terms, vertical dimension of occlusion is defined as "the distance between two selected anatomic or marked points (usually one on the tip of the nose and the other on the chin) when in maximal intercuspal position."5 It is one of the most researched topics in complete denture construction because it can be highly variable, depending on the technique used to determine it. The classic work of Earl Pound, DDS, demonstrates that establishing the "vertical dimension of speech" is the most accurate way of determining the appropriate vertical dimension of occlusion in the completely edentulous patient because it always indicates the most open and the most closed usable space for the teeth, regardless of the amount of bone loss or the age of the patient.6
Establishing the vertical dimension of speech, specifically when the patient is making the "S" sound, provides a way to use the anterior teeth as controls for determining the vertical dimension of occlusion. To create "S" sounds when speaking at conversational speed, the mandible moves forward to the "closest speaking space," which occurs when the lower incisal edges approximate the upper incisal edges or lingual surfaces of the upper anterior teeth by 1.0 mm to 1.5 mm. A clear "S" sound is formed when air is forced through this space.6
The "S" sound is used to determine the vertical dimension of speech because it is a constant and reliable movement whether the patient has teeth or not. The muscles that are used to move the mandible into the position to make the "S" sound are programmed during a patient's growth and development stage. The amount of forward movement exhibited by the mandible varies and is dependent upon the patient's skeletal classification. For example, the mandible will move a further distance to make the "S" sound in a patient with a skeletal class 2 relationship than in one with a skeletal class 1 relationship.7
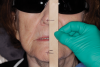
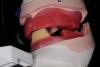
After the maxillary anterior tooth position has been set by the maxillary wax rim, the mandibular wax rim, with the speaking wax in place, is placed into the patient's mouth, and the patient is asked to count from 60 to 70 at conversational speed. The clinician observes the mandibular movement and adjusts the speaking wax until a reasonably clear "S" sound can be made. If the mandibular wax is hitting the upper teeth or anterior rim, its height is adjusted down. It can also be adjusted in the labial-lingual direction (Figure 4).
Another determinant of the vertical dimension of occlusion that is important to note is the amount of "posterior speaking space" available. This is the amount of space between the posterior teeth when the mandible moves forward to enunciate the "S" sound.8 As with the amount of forward movement of the mandible, the amount of space between the posterior teeth will vary depending on the patient's skeletal classification. A patient with a skeletal class 2 relationship will have more posterior speaking space than a patient with a skeletal class 1 relationship. If the posterior teeth are touching when the patient enunciates the "S" sounds, it is an indicator that the vertical dimension of occlusion is too great.
The method of determining the closest speaking space to establish the vertical dimension of occlusion should not be confused with the method of determining freeway space in centric relation.9 Freeway space is the space between the occluding surfaces of the maxillary and mandibular teeth when the mandible is in the physiologic rest position.5 The measure of freeway space contributes to the vertical dimension when the muscles of the mandible are completely at rest, whereas the closest speaking method captures measurements when the muscles of the mandible are active in the full function of speech. The physiologic rest position has been shown to be highly variable; therefore, it does not provide an accurate means of determining the vertical dimension of occlusion in edentulous patients (Figure 5).10
Once the upper and lower incisal edge positions have been determined to establish the closest speaking space for a proper "S" sound, the vertical dimension of speech has been established. The vertical dimension of occlusion should be slightly less than the vertical dimension of speech, otherwise tooth contact will occur during vocalization.
Obtain an Accurate Centric Relation Bite Record
Centric relation, which is defined as the "maxillomandibular relationship, independent of tooth contact, in which the condyles articulate (with the thinnest avascular portion of their respective disks) in the anterior-superior position against the posterior slopes of the articular eminences,"5 is a reproducible reference point. In removable prosthodontics, it is important to restore the completely edentulous patient's occlusion in harmony with centric relation at the appropriate vertical dimension of occlusion.11 This minimizes defective occlusal contacts, which can create looseness, soreness, and instability of complete dentures.
Prior to recording centric relation, it must first be verified by the patient. This is done by bimanual manipulation, loading the condyles with three incremental levels of loading (Figure 6). After each level of loading, the patient is asked if there is any sign of tension or tenderness in either temporomandibular joint. If the answer is no at each level, then the clinician can accept that the patient is in centric relation.12 The wax rims are not inserted into the patient's mouth during verification because centric relation is a jaw-to-jaw position and independent of wax rim position or contact.
Once centric relation is verified, it is recorded with a centric relation bite record. The most accurate way to record centric relation in the completely edentulous patient is with a Gothic arch tracer. There are many advantages of using a Gothic arch tracer, including that it eliminates physical interferences of the rims, it stabilizes the baseplates during recording, and it seats the condyles in centric relation during the functional movements when the Gothic arch is being traced.13
When attaching the gothic arch tracer, it is preferred to use a separate set of baseplates. The maxillary baseplate holds the striking plate (Figure 7), and the mandibular baseplate holds the pin (Figure 8). After the baseplates are seated intraorally, the patient is asked to move his or her mandible forward and backward, to the right and then backward, and to the left and then backward. This series of movements is repeated several times, which serves as practice for the patient and also helps to deprogram the muscles to allow for proper seating of the condyles in centric relation.
Next, the striking plate is covered with a permanent black marker, and the patient is asked to make the functional movements again to create the tracing. When the pin is located at the point where the three lines of the tracing intersect, the jaw is in centric relation (Figure 9). Using a bur, a dimple is created on the striking plate at the intersection of these lines. The patient is then instructed to retrude his or her mandible until the pin falls into the dimple, which holds the patient in the centric relation position. Once in position, an injectable bite registration material is used to index the upper and lower baseplates.
Mounting the Casts on an Articulator
The baseplates and wax rims are used to transfer the correct orientation of the master casts to a semi-adjustable articulator by way of a facebow and the centric relation bite record.14 The posterior part of the maxillary rim is notched so that the bite registration material on the fork forms a solid index (Figure 10).
First, the maxillary cast is mounted on the articulator. Then the baseplates with the gothic arch record are placed on the edentulous casts, which allows the lower edentulous cast to be mounted on the articulator. The pin on the articulator is set to zero for reference. Once the mounting stone is set, the gothic arch record is removed, and the initial set of baseplates and wax rims that communicate incisal edge position are placed on the mounted edentulous casts. The pin on the articulator is then adjusted so that the speaking wax is just out of contact with the upper wax rim (Figure 11). This pin setting represents the appropriate vertical dimension of occlusion that has been determined for the patient.
Using this vertical dimension of occlusion, the laboratory technician will set the remaining teeth in a lingualized occlusal scheme that allows for bilateral balanced occlusion in harmony with centric relation.15 Lingualized occlusion does not permit the anterior teeth to touch, which is why the pin is set to prevent the speaking wax from touching the upper wax rim.
Verify Proper Phonetics
At the try-in appointment, the esthetics and phonetics are verified, and the patient is given the opportunity to approve the setup prior to finalization. The patient is asked to repeat the fricative and "S" sounds, and these are evaluated. When this approach to denture fabrication is followed, establishing proper phonetics becomes a very predictable and reliable process for the clinician.
Conclusion
Rehabilitating the completely edentulous patient is not an easy task for most clinicians. However, when a systematic approach is used, clinicians are able to predictably determine the appropriate tooth positions necessary to restore proper esthetics, phonetics, and function (Figure 12). This becomes especially important when implant-retained prostheses are planned because these prosthetic restorations have no adaptive capacity.
Queries regarding this course may be submitted to authorqueries@aegiscomm.com
About the Author
Kimberley D. Daxon, DDS
Senior Faculty
The Dawson Academy
St. Petersberg, Florida
Daxon Dentistry
St. Petersberg, Florida
References
1. Pound E, Murrell GA. An introduction to denture simplification. J Prosthet Dent. 1971;26(6):570-580.
2. Massad J, Cagna D, Goodacre C, et al. Application of the Neutral Zone in Prosthodontics. Hoboken, NJ: Wiley Blackwell; 2017:3-23.
3. Tucker KM. Accurate record bases for jaw relation procedures. J Prosthet Dent. 1966;16(2):224-226.
4. Silverman MM. The whistle and swish sound in denture patients. J Prosthet Dent. 1967;17(2):144-148.
5. The glossary of prosthodontic terms: ninth edition. J Prosthet Dent. 2017;117(5S):e1-e105.
6. Pound E. The vertical dimension of speech: the pilot of occlusion. J Calif Dent Assoc. 1978;6(2):42-47.
7. Silverman MM. The speaking method in measuring vertical dimension. 1952. J Prosthet Dent. 2001;85(5):427-431.
8. Pound E. Controlling anomalies of vertical dimension and speech. J Prosthet Dent. 1976;36(2):124-135.
9. Niswonger ME. The rest position of the mandible and centric relation. JADA. 1934;21(9):1572-1582.
10. Turrell AJ. Clinical assessment of vertical dimension. J Prosthet Dent. 1972;28(3):238-246.
11. Hickey JA. Centric relation, a must for complete dentures. Dent Clin North Am. 1964;8:587-600.
12. Dawson P. Functional Occlusion: From TMJ to Smile Design. Maryland Heights, MO: Mosby; 2007:57-68.
13. Kapur KK, Yurkstas AA. An evaluation of centric relation records obtained by various techniques. J Prosthet Dent. 1957;7(6):770-786.
14. Thorpe ER, Smith DE, Nicholls JI. Evaluation of the use of a face-bow in complete denture occlusion. J Prosthet Dent. 1978;39(1):5-15.
15. Parr GR, Ivanhoe JR. Lingualized occlusion. An occlusion for all reasons. Dent Clin North Am. 1996;40(1):102-112.