You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Disclosures: Dr. Blatz has received honoraria from Nobel Biocare and Kuraray Noritake Dental, and research support from 3M ESPE. Ms. Sawyer is a paid consultant for Kuraray Noritake.
Several new materials and technologies have had a tremendous impact on clinical dentistry and helped revolutionize traditional restorative treatment concepts. Zirconium-dioxide (ZrO2, zirconia) ceramics have fundamentally changed clinical applications and the range of indications for all-ceramic restorations, from single-tooth restoration to full-mouth implant-supported rehabilitations.1-3
The first CAD/CAM-fabricated zirconia (more accurately termed yttria-stabilized zirconium dioxide, or yttria-stabilized tetragonal zirconia polycrystals [Y-TZP]) coping was introduced in the late 1990s to provide a strong and more esthetic framework for a porcelain-fused-to-zirconia (PFZ) restoration. Nobel Procera® Zirconia (Nobel Biocare, Nobelbiocare.com) was the first popular product, followed by LavaTM Zirconia (3M ESPE, 3mespe.com) in the early 2000s. The demand for PFZ crowns increased rapidly due their esthetic properties and the zirconia core material of more than 1000 MPa in high flexural strength. Early studies and clinical experiences, however, indicated high incidences of chipping and fractures, especially within the veneering porcelain.1 Better understanding of the material enabled the development of veneering porcelains that better matched the physical and thermal properties of the zirconia framework.2,3 Consequently, researchers conducting newer clinical studies could not find differences in the long-term performance between PFZ and porcelain-fused-to-metal (PFM) crowns.3-5 Still, widespread concerns about veneer-porcelain chipping and the more technique-sensitive firing and handling of zirconia persisted, and ultimately led to the development of CAD/CAM-fabricated monolithic full-contour zirconia restorations that did not require application of a veneering porcelain.
Numerous products have entered the market. In the meantime, millions of full-contour zirconia restorations have been inserted and their use has proven to be an efficient and cost-effective alternative to layered indirect restorations due the CAD/CAM fabrication process. Translucency of this second generation of zirconia materials was slightly improved compared with first-generation materials while retaining similar flexural strength values. However, customization and individual shading had to be achieved through soaking or applying liquid dye to the milled green-stage or presintered material and external staining after sintering.
To simplify the process, some manufacturers have introduced preshaded zirconia blanks, some of them with multiple layers of slightly different shades between dentin and enamel areas to better simulate the appearance of natural teeth. Restorations made with multilayered zirconia can still be modified and customized to a certain degree with external stains or simply polished to the desired luster.
The latest generation of zirconia materials has a significantly higher degree of translucency, providing greatly improved esthetics. The use of multilayer high-translucent zirconia materials, in particular, provides a great range of esthetic possibilities, specifically for anterior teeth.6 The higher translucency is achieved by slight changes of the yttria (Y2O3) content (5 mol% or more instead of the conventional 3 mol%), which is used to stabilize the tetragonal zirconia phase, causing a higher amount of cubic phase particles. Cubic zirconia offers significantly greater light transmission but lower physical strength. High-translucent zirconia has flexural strength values between 550 MPa and 800 MPa, depending on the degree of translucency; the higher the translucency, the lower the flexural strength.7 Its specific properties make it a viable material alternative for the esthetic zone. If bonded properly, it can be even used for laminate veneers and onlays.
Ceramic Bonding
Ceramic materials are brittle and cannot undergo plastic deformation as metal alloys do. Therefore, their modulus of elasticity and behavior under functional stress is different from metals. The crystalline structure allows for crack propagation when the surface is damaged or external forces become excessive. Therefore, the type of luting agent and technique for permanent cementation have a significant influence on the clinical success of all-ceramic restorations.8,9 In general, adhesive bonding with composite resins and adequate pretreatment of the abutment tooth and ceramic bonding surface have the ability to support ceramic restorations, improve retention, reduce microleakage, and increase fracture resistance of the restoration and abutment tooth.10 The clinical procedures and surface pretreatment steps differ, depending on the composition and mechanical properties of the ceramic substrate.8 The two major categories of ceramic materials are silica based (ie, feldspathic, leucite-reinforced, lithium disilicate) and non-silica–based high-strength ceramics, which include alumina and zirconia. The quality and durability of the bond between the composite resin and ceramic are key for clinical success.8-10 They typically depend on the surface topography of the substrate, surface energy, and chemical interaction with the resin.8 As with any adhesive interactions, contamination of the bonding surfaces has adverse effects on bond strengths.
Hydrofluoric-acid etching, followed by application of a silane-coupling agent, is recommended for glassy-matrix ceramics.11 Hydrofluoric-acid etching selectively dissolves the glass matrix and produces a porous, irregular surface of increased wettability. Application of a silane-coupling agent on the etched ceramic surface increases adhesion through mechanical interlocking and coupling the silica (silicon oxides) to the organic matrix of resin materials by means of siloxane bonds.11 The intaglio surfaces of silica-based ceramic restorations should not be treated with blunt surface-roughening methods such as air-particle abrasion or grinding as they may create microcracks, which function as crack initiators and may lead to fractures.
High-strength, metal-oxide–based ceramics such as alumina and zirconia are typically considered “cementable” due to their high inherent flexural strength, which exceed typical chewing forces.8 Therefore, zirconia-based crowns and bridges with adequate retention and ceramic material thickness can be cemented conventionally. Resin-modified glass-ionomer or self-adhesive resin cements are preferred and provide at least a certain level of adhesion to both teeth and ceramic without additional time-consuming and technique–sensitive priming steps.9,12 Manufacturers’ instructions should be followed closely, as some recommend air-particle abrasion with aluminum-oxide before cement application,13 while others do not. Some self-adhesive resin cements can be “tack cured” with a curing light for a few seconds, leaving the cement in a doughy stage for easy removal of excess material before complete polymerization.12 In general, one should carefully clean any indirect restoration before final cementation, for example in ethanol or acetone in an ultrasonic cleaning unit.
The APC Zirconia-Bonding Concept
While considered “cementable,” some zirconia restorations benefit from insertion with composite resin-luting agents. These include zirconia restorations that are less strong, are thin, lack retention, or rely on resin bonding, such as resin-bonded fixed prostheses14 or bonded laminate veneers. The success of resin bonding relies on the proper materials selection and adequate treatment of tooth and restoration bonding surfaces.8
The abutment tooth is treated with a bonding agent as recommended by the manufacturer. Only dentin bonding agents specifically indicated for indirect restorations should be selected, as many self-etch adhesives are limited to direct restorations due to their increased film thickness and photopolymerization.15
The resin bond to high-strength ceramics has been investigated for more than 2 decades now. The classic articles by Kern and his colleagues16-18 demonstrated that for high-strength ceramics, many bonding protocols work in the short term, but that strong and durable long-term resin bonds are achieved only after surface pretreatment with air-particle abrasion and use of an adhesive composite-resin luting agent that incorporates special adhesive phosphate monomers, especially 10-methacryloyloxydecyl-dihydrogen phosphate (MDP).16-18 In fact, some of those adhesive resin cements were developed to bond to metal-alloy restorations.
Our first research studies on bonding to alumina and zirconia started in the early 2000s and have, in the meantime, comprised thousands of specimens and most surface pretreatment and cement options commonly available.8,9,12,13,19-21 In contrast to other studies, which used polished ceramic samples, we investigated the actual intaglio surfaces of CAD/CAM-fabricated ceramic restorations. We found that, in addition to the adhesive composite resins, specific primers containing adhesive phosphate monomers, ie, MDP, have the ability to better wet the slightly rough surfaces and provide superior long-term bond strengths to air-particle–abraded high-strength ceramics. Several other treatments have been examined, including the use of various acid etchants and plasma coating. Some have shown promising results, but limited feasibility in daily clinical practice routine.
To practically achieve the high and long-term durable resin bond strengths to zirconia, we recommend a three-step approach. To simplify this protocol, we have termed it the “APC zirconia-bonding concept:” APC-Step A: Air-particle abrade the bonding surface with aluminum oxide; APC-Step P: Apply special zirconia primer; and APC-Step C: Use dual-cure or self-cure composite resin cement.
APC-Step A
After restoration cleaning, zirconia should be air-particle abraded (APC-Step A) with alumina or silica-coated alumina particles; some call this procedure sandblasting or microetching. A chairside microetcher using small particles (50 μm to 60 μm) at a low pressure (below 2 bar) is sufficient.9,13,20-22 The overall effect of alumina pretreatment seems more important than actual surface roughening, especially with its ability to effectively decontaminate the bonding surfaces.22 As the effects of air-particle abrasion on the flexural strength of zirconia have been discussed extensively, most existing studies indicate that particularly small particles actually provide a strengthening effect.23
APC-Step P
The subsequent step includes application of a special ceramic primer (APC-Step P), which typically contains special adhesive phosphate monomers, onto the zirconia bonding surfaces.24,25 The monomer MDP, which is also used in some dentin bonding agents and cements, has been shown to be particularly effective to bond to metal oxides. Such primers may also increase bonding abilities of other cements, such as resin-modified glass ionomers, to zirconia.26 However, it is highly suggested to stay within recommended company product lines for bonding agents, primers, and cements, and to not interchange products from different manufacturers, which may have similar names, but likely different chemical compositions that may not be compatible with each other. Some clinicians may be confused due to the fact that some special zirconia primers also contain silanes, which make them universally applicable to various materials, including silica-based ceramics. But remember that silanes have no contributing effect to long-term bond strengths to metal-oxide–based ceramics unless they are coated with a silica-based ceramic or silica-containing particles.21
APC-Step C
Dual- or self-cure composites (APC-Step C) should be used to ensure adequate polymerization/conversion beneath the zirconia restoration, which reduces light transmission.8 However, high-translucent zirconia transmits enough light that the shade of the cement or composite-resin luting agent influences the final appearance of such restorations. It is, therefore, highly recommended to verify the anticipated appearance with try-in pastes and select the most adequate cement shade based on the individual situation and shade of the abutment tooth.
The APC zirconia-bonding concept is not limited to teeth and also applied in the laboratory, for example for implant reconstructions that include cemented zirconia components.
For new high-translucent zirconia products with lower flexural strength, proper bonding is even more important and may be necessary for restorations fabricated at minimum thickness. It is mandatory for bonded restorations such as resin-bonded fixed dental prostheses,14 laminate veneers, and inlays/onlays,27,28 all of which can be fabricated from zirconia with excellent longevity, as long as they are bonded correctly.14
The described APC zirconia-bonding concept is not new but rather a culmination of research studies spanning 2 decades to identify effective, yet clinically feasible, bonding protocols. Findings from recent systematic literature reviews, which evaluated the data of more than 140 different zirconia-bonding studies, arrived at the same conclusions.29,30 It is, of course, our goal to continue the search for possibly even more effective bonding methods to broaden clinical indications and increase the longevity of zirconia-based restorations.
Case Presentation
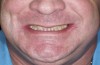
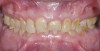
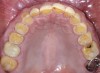
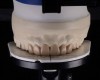
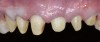
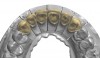
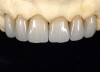
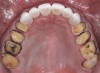
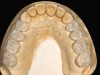
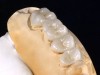
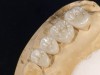
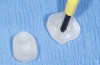
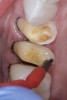
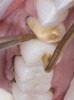
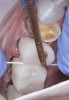
A 40-year-old patient presented with the chief complaint: “My teeth are cracking, and I would like to have my original bite.” Dental findings included Class I occlusion with slight misalignment between teeth Nos. 8 and 9. Generalized severe occlusal wear and slight Class I mobility of teeth Nos. 23 to 26 were noted. Caries lesions were found on teeth Nos. 2, 4, 6, 8, 9, and 14 and abfraction lesions on teeth Nos. 4, 5, 10, 11, 13, 20, and 21. Figure 1 through Figure 3 depict the preoperative situation. Full-mouth rehabilitation was suggested. The goals for the restorative treatment were management of erosive etiology, conservation of tooth structure, and long-term protection of the restorations. A diagnostic wax-up was instrumental in determining functional and esthetic treatment goals and establishing new anterior guidance (Figure 4). A comprehensive, step-by-step treatment approach was applied, which, after periodontal pretreatment, caries control, and provisionalization, included definitive preparation (Figure 5) and restoration of the maxillary anterior teeth to establish anterior occlusal guidance. CAD/CAM–fabricated full-contour monolithic high-translucent zirconia crowns (Katana™ UTML Ultra Translucent Multi-Layered, Kuraray Noritake Dental, kuraraynoritake.com) were fabricated (Figure 6 and Figure 7) and cemented with self-adhesive resin cement (Panavia SA, Kuraray Noritake Dental). Figure 8 demonstrates the cemented anterior crowns and refined conservative preparations of posterior teeth, which were performed with minimal tooth-structure removal. High-translucent monolithic zirconia onlays and crowns were fabricated (Katana Zirconia UT, Kuraray Noritake Dental) (Figure 9 to Figure 12). The posterior restorations were adhesively bonded following the APC zirconia-bonding concept. APC-Step A involved air-particle abrasion with 50-μm aluminum oxide at 1.5 bar with a chairside microetcher (Figure 13), followed by application (APC-Step P, Figure 14) of a special ceramic primer (ClearfilTM Ceramic Primer, Kuraray Noritake) with adhesive phosophate monomers (MDP). Relative moisture and contamination control was achieved with cotton rolls and retraction cords. Rubber dam placement, which is always preferred, was difficult in this situation. The enamel surfaces of the abutment teeth were selectively etched (Figure 15) with 35% phosphoric acid (K-Etchant Gel, Kuraray Noritake Dental) and the dentin conditioned (Figure 16) with a self-etch dentin primer (Panavia V5 Tooth Primer, Kuraray Noritake Dental). A dual-cure adhesive resin (Panavia V5 Paste Universal, Kuraray Noritake Dental) was dispensed directly into the restorations with an automix syringe. The restorations were inserted, and excess cement was carefully removed (Figure 17 and Figure 18) before light polymerization (Figure 19). Postoperative views depict the treatment outcome (Figure 20 to Figure 22).
Conclusions
Reliable cementation protocols and materials are fundamental for clinical success of indirect ceramic dental restorations, including those made from zirconia materials. New high-translucent zirconia ceramics have favorable optical properties and can be applied as monolithic full-contour restorations in various clinical indications for posterior and anterior teeth. Resin bonding supports ceramic restorations and is necessary for onlays, laminate veneers, and resin-bonded fixed dental prostheses. The APC zirconia-bonding concept is based on decades of research on how to achieve high and long-term durable bond strengths to zirconia. It includes three practical steps: (A) air-particle abrasion, (P) zirconia primer, and (C) adhesive composite resin.
About the Authors
Markus B. Blatz, DMD, PhD
Professor of Restorative Dentistry
Chair
Department of Preventive and Restorative Sciences
School of Dental Medicine
University of Pennsylvania
Philadelphia, Pennsylvania
Marcela Alvarez, DDS, MSD
Private Practice
San Antonio, Texas
Kimiyo Sawyer, RDT
President
Cusp Dental Laboratory
Malden, Massachusetts
Marco Brindis, DDS
Assistant Professor of Clinical Prosthodontics and Interim Chair
Department of Prosthodontics
Louisiana State University School of Dentistry
New Orleans, Louisiana
Queries to the authors regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Komine F, Blatz MB, Matsumura H. Current status of zirconia-based fixed restorations. J Oral Sci. 2010;52(4);531-539.
2. Blatz MB, Bergler, M, Ozer F, et al. Bond strength of different veneering ceramics to zirconia and their susceptibility to thermocycling. Am J Dent. 2010;23(4):213-216.
3. Saito A, Komine F, Blatz MB, Matsumura H. A comparison of bond strength of layered veneering porcelains to zirconia and metal. J Prosthet Dent. 2010;104(4):247-257.
4. Ozer F, Mante FK, Chiche G, et al. A retrospective survey on long-term survival of posterior zirconia and porcelain-fused-to-metal crowns in private practice. Quintessence Int. 2014;45(1):31-38.
5. Takeichi T, Katsoulis J, Blatz MB. Clinical outcome of single porcelain-fused-to-zirconium dioxide crowns: a systematic review. J Prosthet Dent. 2013;110(6):455-61.
6. Bergler M, Blatz MB, Mante FK. Translucency of full-contour zirconia ceramics. J Dent Res. 2015;94(Spec issue A):3534 (Abstr).
7. Conejo J, Kobayashi K, Mante F, Blatz MB. Flexural strength of new high-translucent zirconia and lithium disilicate ceramics with two specimen dimensions. J Dent Res. 2016;95(Spec issue B):1162 (Abstr).
8. Blatz MB, Sadan A, Kern M. Resin-ceramic bonding: a review of the literature. J Prosthet Dent. 2003;89(3):268-274.
9. Blatz MB, Oppes S, Chiche G, et al. Influence of cementation technique on fracture strength and leakage of alumina all-ceramic crowns after cyclic loading. Quintessence Int. 2008;39(1):23-32.
10. Burke FJ, Fleming GJ, Nathanson D, Marquis PM. Are adhesive technologies needed to support ceramics? An assessment of the current evidence. J Adhes Dent. 2002;4(1):7-22.
11. Blatz MB, Sadan A, Maltezos C, et al. In vitro durability of the resin bond to feldspathic ceramics. Am J Dent. 2004;17(3):169-172.
12. Blatz MB, Bergler M. Clinical application of a new self-adhesive resin cement for zirconium-oxide ceramic crowns. Compend Contin Educ Dent. 2012;33(10):776-781.
13. Blatz MB, Phark JH, Ozer F, et al. In vitro comparative bond strength of contemporary self- adhesive resin cements to zirconium oxide ceramic with and without air-particle abrasion. Clin Oral Investig. 2010;14(2):187-192.
14. Maggio M, Bergler M, Kerrigan D, Blatz MB. Treatment of maxillary lateral incisor agenesis with zirconia-based all-ceramic resin bonded fixed partial dentures: a case report. Amer J Esthet Dent. 2012;2(4):226-237.
15. Ozer F, Blatz MB. Self-etch and etch-and-rinse adhesive systems in clinical dentistry. Compend Contin Educ Dent. 2013;24(1):12-20.
16. Kern M, Thompson VP. Bonding to glass infiltrated alumina ceramic: adhesive methods and their durability. J Prosthet Dent. 1995;73(3):240-249.
17. Kern M, Wegner SM. Bonding to zirconia ceramic: adhesion methods and their durability. Dent Mater. 1998;14(1):64-71.
18. Wegner SM, Kern M. Long-term resin bond strength to zirconia ceramic. J Adhes Dent. 2000;2(2):139-147.
19. Blatz MB, Sadan A, Arch GH Jr, Lang BR. In vitro evaluation of long-term bonding of Procera AllCeram alumina restorations with a modified resin luting agent. J Prosthet Dent. 2003;89(4):381-387.
20. Blatz MB, Sadan A, Martin J, Lang B. In vitro evaluation of shear bond strengths of resin to densely-sintered high-purity zirconium-oxide ceramic after long-term storage and thermal cycling. J Prosthet Dent. 2004;91(4):356-362.
21. Blatz MB, Chiche G, Holst S, Sadan A. Influence of surface treatment and simulated aging on bond strengths of luting agents to zirconia. Quintessence Int. 2007;38(9):745-753.
22. Quaas AC, Yang B, Kern M. Panavia F 2.0 bonding to contaminated zirconia ceramic after different cleaning procedures. Dent Mater. 2007;23(4):506-512.
23. Song JY, Park SW, Lee K, et al. Fracture strength and microstructure of Y-TZP zirconia after different surface treatments. J Prosthet Dent. 2013;110(4):274-280.
24. Koizumi H, Nakayama D, Komine F, et al. Bonding of resin-based luting cements to zirconia with and without the use of ceramic priming agents. J Adhes Dent. 2012;14(4):385-392.
25. Nakayama D, Koizumi H, Komine F, et al. Adhesive bonding of zirconia with single-liquid acidic primers and a tri-n-butylborane initiated acrylic resin. J Adhes Dent. 2010;12(4):305-310.
26. Alnassar T, Ozer F, Chiche G, Blatz MB. Effect of different ceramic primers on shear bond strength of resin-modified glass ionomer cement to zirconia. J Adhes Sci Technol. 2016; DOI: 10.1080/01694243.2016.1184404.
27. Blatz MB. Long-term clinical success of all-ceramic posterior restorations. Quintessence Int. 2002;33(6):415-426.
28. Mante FK, Ozer F, Walter R, et al. The current state of adhesive dentistry: a guide for clinical practice. Compend Contin Educ Dent. 2013;34:Spec 9:2-8.
29. Özcan M, Bernasconi M. Adhesion to zirconia used for dental restorations: a systematic review and meta-analysis. J Adhes Dent. 2015;17(1):7-26.
30. Inokoshi M, De Munck J, Minakuchi S, Van Meerbeek B. Meta-analysis of bonding effectiveness to zirconia ceramics. J Dent Res. 2014;93(4):329-334.