You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
At least several times a week, a clinician is likely to encounter patients with sensitive teeth. The phenomenon is typically caused by thermal changes in the mouth that occur when drinking or ingesting cold beverages or foods, or when inhaling cold air on a winter day. Some patients with hypersensitivity have concerns that the pain indicates a potential toothache or the need for immediate dental attention.
Tooth sensitivity can be due to various reasons, which could include postoperative sensitivity after restorative treatment, a failing restoration that has marginal leakage so that the tooth feels sensitive during normal eating or breathing, or changes in the osmotic gradient due to the types of foods or beverages being ingested. A patient may find it difficult to know the cause of the pain. This article will focus specifically on dentin hypersensitivity.
Patients may report dentin hypersensitivity as a sharp, brief tooth pain irrespective of stimulus.1 Although dentin hypersensitivity can be present in anyone regardless of age, adults are more likely to articulate this complaint. In recent years, baby boomers, individuals who were born between 1946 and 1964, have been aging. In 2014, the youngest baby boomer turned 50 years old, and the oldest turned 68. This portion of the population now nearly numbers 80 million and includes those born in the United States and abroad. More than 40 million adults are 65 years or older.2 By 2050, this will expand to more than 80 million. Also, more than 70% of adults 65 years and older have some or most of their natural teeth. The number of edentulous patients is expected to remain at 9 million until 2020.3 These data strongly suggest a possible increase in the number of patients who will need dental services for the treatment of caries and periodontal disease. These same patients will also likely require more care for dental emergencies caused by infection, pain and trauma, tooth hypersensitivity, and failures of existing dental restorations.
Definition
Also known as tooth sensitivity and root sensitivity, dentin hypersensitivity is a common complaint from patients. Holland and colleagues4 described dentin hypersensitivity as “short, sharp pain arising from exposed dentin in response to stimuli typically thermal, evaporative (air), tactile (rubbing), osmotic or chemical and which cannot be ascribed to any other form of dental defect of pathology.” Dental professionals see dentin hypersensitivity as an exaggerated response to routine stimuli imposed on teeth. With a dental examination, radiographs (if necessary), and diagnostic testing, the finding in most cases is dentin hypersensitivity,5,6 which is typically associated with recession. Tooth whitening with peroxide compounds, a routine restorative procedure, appears to cause similar sensitivity. Although the phenomena of both types of tooth sensitivity appear to be the same, their etiologies are different.7 These differences will be presented later in this article.
Dentin hypersensitivity may make patients uncomfortable during periodontal cleanings and may cause pain when brushing or flossing. Although dentin hypersensitivity does not directly harm the tooth, dentin, or pulp, it can be considered a true pain syndrome.8 Sensitivity pain, which is of short duration, should be distinguished from pain of longer duration that is not treatable with desensitizing agents, which may be the result of pulpal inflammation.9 Typically, dentin hypersensitivity occurs when a tooth is exposed to cold foods, sweets, beverages, or plaque accumulation on exposed root surfaces. Dentin hypersensitivity is considered to be one of the most painful and least successfully treated chronic dental conditions.10
After diagnosis and the etiology has been established, treatment recommendations may include both in-office professionally applied treatments and at-home professionally dispensed therapies or recommendations for over-the-counter (OTC) treatments.11 Clinical follow-up with the patient is necessary to ascertain the therapeutic benefits of treatment recommendations.
Several studies examining the prevalence of dentin hypersensitivity have reported a rate between 4% and 57% in the general population.12-18 The rate is considerably higher among periodontal patients (between 60% and 98%).19,20 Patients who have dentin hypersensitivity may not visit the dentist for the complaint because they do not view it as a significant dental health problem but may mention it at a routine dental appointment.21 Generally, dentin hypersensitivity occurs in patients between the ages 30 and 40 years;22 however, patients can be significantly younger or older. Both genders are affected, although dentin hypersensitivity may be more common in women.23 Root sensitivity has been reported in incisors, canines, premolars, and molars, although it has been observed to be more common in canines and premolars.24,25
Etiology and Physiology
Dentin’s anatomy and physiology account for its sensitivity. Dentin is a porous, mineralized connective tissue with an organic matrix of collagenous proteins and an inorganic component. This is known as hydroxyapaptite. Within dentin are microscopic structures known as dentinal tubules, functioning as micro-canals channeling through the dentin from the pulp cavity to the surface cementum border. The dentinal tubules vary in their configurations and diameters. Depending on depth, one square millimeter of dentin can contain 30,000 tubules. Each tubule contains two types of nerve fibers: myelinated (Type A fibers) and unmyelinated (Type C fibers).27 Type A fibers cause the sensation of dentin hypersensitivity.
Identifying Patients at Risk
Patients are concerned when dental pain occurs32 and can pinpoint areas of dentin hypersensitivity before a clinical examination is performed. If dentin hypersensitivity is identified when blowing air on a tooth or by scratching during a tactile examination of hard tooth surfaces but the patient has not complained of tooth sensitivity, treatment is not indicated. Treatment should be rendered after patient request and examination.
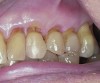
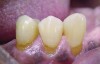
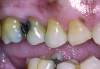
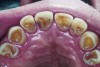
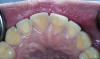
A major predisposing factor to dentin hypersensitivity is exposed root surfaces (Figure 1 through Figure 3).33 Contributors to dentin hypersensitivity include enamel loss with exposed dentin due to attrition and tooth wear caused by bruxism, occlusal habits, and parafunctional activity (Figure 4).34
A study examining adults older than 60 years of age found that almost 32% had root caries or a restored root surface.35 Root caries can indicate periodontal attachment loss and subsequent recession, suggesting at least 30% of adults older than 60 years of age could be at risk for recession in at least one tooth. Another report indicated that at least 22% of adults between 30 and 90 years of age will exhibit recession of at least 3 mm in one or more teeth.36 Age increases the rate of gingival recession.37 Patients who have had or are receiving periodontal therapy are also at risk for dentin hypersensitivity.38 Root sensitivity prevalence has been reported to be 9% to 23% before periodontal therapy and 54% to 55% after treatment (scaling and root planing and periodontal surgery). Root sensitivity intensified 1 to 3 weeks after therapy, and then slowly decreased.
Among the causes of gingival recession are inadequate attached gingiva, prominent roots with a thin alveolar housing or bony dehiscence, toothbrush abrasion, excessive tooth cleaning, excessive flossing, periodontal surgery, factitial habits (eg, picking at the tooth’s cervical with a fingernail), gingival attachment loss due to specific pathologies, and iatrogenic loss of attachment during restorative procedures.39 When the root surfaces are exposed, erosion, abrasion, and abfraction make the cementum and the dentin more vulnerable to caries and loss of tooth substance.40-43
Gingival recession is a predisposing factor for, not a direct cause of, dentin hypersensitivity.23 To have the condition, the patient must have the dentin tubules open at both ends, to the pulp and to the oral cavity. In normal conditions, the tubules harden and become plugged. However, when dentin is cut or abraded, the mineralized matrix creates debris that spreads over the dentin surface; a smear layer is then formed.44,45 This phenomenon occurs in both enamel and dentin.45 But the loss of this smear layer, or the unplugging of the dentinal tubules, contributes to dentin hypersensitivity. Root surfaces that are exposed to toothbrushing with or without the use of toothpaste can be predisposing factors in removing the smear layer.22,46 Acidic byproducts of bacterial plaque can open dentinal tubules; therefore, when the patient does not remove all of the plaque from root surfaces, the tubules can be opened. The use of highly abrasive toothpaste can lead to continued dentinal tubule exposure. Other patient behaviors that present risk are ones that expose the oral cavity to acids, such as ingesting acidic foods and beverages,47-49 ingesting chlorinated pool water when swimming,44 and suffering from bulimia and gastrointestinal reflux disease (Figure 5).51 Patients should be advised to refrain from toothbrushing immediately after ingesting acidic foods or beverages.23
Screening and Diagnosis
Screening for dentin hypersensitivity is not a part of a routine examination unless the patient mentions the pain.52 In 1995, Dutch general practitioners were randomly surveyed on the prevalence, conditions, and treatment of cervical hypersensitivity in their practices.53 UK dentists participated in a similar study in 2002.54 These studies showed that dentists reported 10% of patients as having moderate pain and 1% as experiencing severe pain from the condition. These results indicated to the researchers that issues in screening, perception, and knowledge of dentin hypersensitivity treatment persist.
In a 2003 questionnaire taken by Canadian dentists and dental hygienists designed to evaluate a practitioner’s perception and clinical management of dentin hypersensitivity,52 fewer than 50% of the respondents considered differential diagnoses, even though dentin hypersensitivity is a diagnosis of exclusion. A total of 64% of the dentists and 77% of the hygienists identified bruxism and malocclusion as triggers of dentin hypersensitivity. The researchers observed that only 7% of dentists and 5% of dental hygienists correctly chose erosion as a primary cause, and that 17% of dentists and 48% of hygienists were not able to pinpoint the commonly accepted hypersensitivity theory.
In this same survey, dentin hypersensitivity management was studied. Only half of the respondents reported that they could manage dentin hypersensitivity pain, and only 50% of those respondents would consider altering predisposing factors as a means to manage pain. The findings showed that practitioners do not understand the mechanisms for how desensitizing toothpastes work to relieve pain. More than half of the dentists (56%) and dental hygienists (68%) believed that desensitizing toothpastes helped to prevent dentin hypersensitivity, while 31% of the dentists and 16% of hygienists did not think that desensitizing toothpastes relieved dentin hypersensitivity.
Improved education on the etiology and treatment of dentin hypersensitivity may benefit dental professionals. As part of any screening for dentin hypersensitivity, the clinician should determine whether a localized or generalized problem exists. In-office treatments are usually sufficient for localized, isolated tooth dentin hypersensitivity. For generalized conditions in which significant recession is evident on multiple teeth, an at-home treatment regimen may be more suitable.
Tooth Whitening Induced Sensitivity
Although dentin hypersensitivity and tooth-whitening sensitivity appear to be the same symptomatically, their etiologies show that they are not. Patients report dentin hypersensitivity as sharp, short-lasting tooth pain irrespective of the stimulus. Tooth sensitivity caused by tooth whitening has been described as mild to intolerable pain.55-57 Tooth-whitening sensitivity starts during the whitening procedure but sensitivity levels return to normal after or during the whitening treatment.5 Sensitivity has been the highest-reported adverse reaction in tooth whitening procedures.5,58-60
In clinical research studies, tooth sensitivity during whitening, either with at-home tray delivery or in-office procedures, has been reported in 18% to 78% of patients.58-60 Clinical observations suggest that it is fleeting and has no long-term effects.61 Some dental professionals had believed this transient sensitivity was caused by gingival recession. However, research has shown that gingival recession is not a factor in tooth hypersensitivity when whitening.62
It has been suggested that the etiology of tooth hypersensitivity during peroxide-based tooth whitening is directly related to the rapid penetration of the peroxide through the enamel and dentin into the pulp, causing a reversible pulpitis.63,64 A correlation has been made that higher concentrations of peroxide-based whitening products have more reports of tooth sensitivity.65,66
For patients at risk, in many cases because of a past history of tooth sensitivity while whitening, recommendations to minimize tooth sensitivity during peroxide-based whitening include using lower concentrations of whitening products, using carbamide peroxide whitening gels, recommending the use of potassium nitrate- and fluoride-containing whitening gels, and using a potassium nitrate-containing OTC toothpaste applied topically daily for 2 weeks before initiating whitening procedures.5
Conclusion
Dental professionals should understand the causes of hypersensitivity. A patient should be evaluated based on risk factors that may be present. Once a diagnosis has been made and the factors have been identified, the dental professional can create a treatment plan for the patient’s dentin hypersensitivity. As part of the routine dental examination, dental professionals should ask patients about any sensitive teeth. Depending on the severity of the condition, clinical management of dentin hypersensitivity may include both in-office and self-applied at-home therapies.3,67,68
About the Author
Howard E. Strassler, DMD
Professor and Director of Operative Dentistry
Department of Endodontics, Prosthodontics, and Operative Dentistry
University of Maryland
Baltimore, Maryland