You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Bonding agents in dentistry have a long history. Amalgam restorations were one of the first forms of dental bonding, originating before the 20th century.1 In the mid-20th century, one of the first developed bonding agents, Sevriton Cavity Seal® (Amalgamated Dental/DeTrey), contained glycerophosphoric acid dimethacrylate; unfortunately, the system was not highly effective due to its high polymerization shrinkage and thermal expansion.1 Researchers then developed agents using stronger acids and continued research in bonding; many attempts ultimately failed clinically, such as Cervident® (S.S. White) and other N-phenylglycine and glycidyl methacrylate (NPG-GMA) bonding agents.2 Problems continued to arise regarding the agents attaching to the dentin, which led to several new generations of bonding products. Companies began to create bonding agents that could etch, prime, and adhere in one step, simplifying the several steps that restorative procedures previously took. Initially, these new products did not perform as well as previous generations and had lower bond strength.3 Research continued, and today, researchers have developed new technology that saves time and prevents adhesive failures with what is now known as universal bonding agents.3
Universal bonding agents first came into use in clinical practice in 2011.3 The science behind most universal bonding agents has reflected previous generations of bonding technology while focusing on the need for faster, more efficient dentistry. Universal bonding agents have a fairly broad definition but typically are described as being compatible with total-, self-, and selective-etch techniques and dual- and self-cure materials, as well as being usable with a wide range of materials, including ceramics and zirconia.4 Universal adhesives differ from previous products in the basis of their chemical composition: monomers incorporated in the agents can produce chemical and microchemical bond adhesion.3 Certain adhesive monomers, such as 3D self-reinforcing monomer (3D-SR) and 10-methacryloxydecyl dihydrogen phosphate (MDP), have improved the bond strength of these universal bonding agents while also permitting dentists to use various etching techniques with these products.5 And although one might expect a universal product to come in a one-bottle method, both one-bottle and two-bottle systems remain prominent in the industry. Dentists are free to total-etch, self-etch, or selective-etch while using many varieties of universal bonding agents; having the option to self-etch without having to stock several different products in the office can prove highly beneficial.2 Scotchbond™ Universal (3M) and Tokuyama Universal Bond (Tokuyama Dental) are examples of popular universal bonding agents. Some universal bonding agents can be used with all direct and indirect materials without any additional primer; other universal bonding agents occasionally require additional products.6 Yet, when considering the implications of these types of products' versatility, one can recognize how much inventory a doctor can save. Most dentists stock several hundreds to thousands of dollars of various composite materials, bonding agents, and more to meet the needs of every patient who may walk in the door.7 Having universal products can streamline several procedural steps into one and reduce the need for additional products to complete the restoration, resulting in substantial savings in inventory for a dental office.8
Many of these universal bonding products, however, still require light-curing, and adhesive failures can occur if the light does not fully cure the bonding agent.9 A more recent development involves universal bonding agents that do not require light-curing. Proper polymerization through light-curing can be challenging; restorative failures often occur due to a lack of proper curing.9 Each restorative material and product has a different set of instructions requiring very particular light-curing requirements, but most dentists rely on one or two trusted curing lights that likely do not match the exact curing needs of each different product used.10 Because of so many differences between curing lights, product requirements, and even the method the practitioner uses, there are immense differences between dentists' restorations and adequate energy emitted to the restoration, even when these dentists use the same curing light.10 Deep restorations and post-and-core buildups can also be difficult to fully cure with a light and may need several additional steps to ensure complete curing and light penetration.11 A universal bonding agent that does not require light-curing can lead to reduced restorative failures, improved outcomes, and happier patients.5 Self-curing universal bonding agents have their own specific list of instructions, but a single product that does not rely on exterior forces (such as curing lights' abilities) would reduce the risk of improper curing and bonding for several reasons; for example, not having to light-cure often leads to shorter chairtime for patients, thus reducing the chance of adhesion failure due to blood or saliva contamination.5
Universal bonding agents can also lead to large time savings for a dentist.12 Take, for instance, a patient who would benefit by the quick and efficient completion of a case, such as a very young patient or a case with challenging access; in this instance, having one bonding agent that can fit this need, without having to search through the office for a product that may work better, can save time and worry.3 Particularly when considering the ability of universal bonding agents to be used without primers and in any etch and curing methods, one can see the benefits of a product with these capabilities. Confusion with what additional products are needed is reduced, ultimately lowering the chance of mistakes being made.13 Moreover, some bonding agents do not require surface agitation or light-curing, ultimately reducing chairtime and increasing the number of patients who can have restorations completed in a quick and efficient amount of time.5
Case 1: Direct Restoration
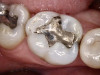
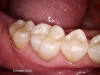
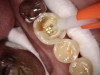
The benefits and ease of a universal bonding agent are demonstrated through the following case example of a Class II restoration. The patient was a 56-year-old woman. At her initial examination, it was observed that her lower right first molar (tooth No. 30) had an old failing amalgam restoration on the occlusal and a mesial fracture line with clinically visible caries (Figure 1). The preoperative bitewing x-ray did not show any mesial caries. The tooth needed a new restoration. The treatment plan was to perform a mesial-occlusal composite filling. A bitewing and periapical x-rays were taken to make sure that there was no other interproximal caries or any periapical lesion. Furthermore, an intraoral photograph taken with an intraoral camera was used to present and to help confirm the caries.
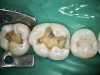
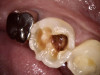
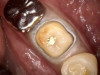
After anesthetic with 2% lidocaine with 1:100,000 epinephrine, a rubber dam was placed. The existing amalgam was removed using an inverted cone diamond bur and a small round diamond bur. The photograph showed recurrent and mesial caries. Removal of all the soft caries was performed using carbide round burs with a slow-speed handpiece. To make a clean and neat cavity preparation, all the superficial caries and stains were removed conservatively with a small round diamond bur. Then an intraoral photograph was taken to ensure that no caries was left behind (Figure 2).
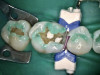
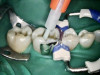
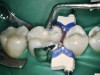
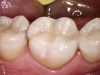
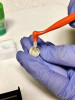
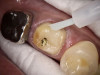
After a clean and neat cavity preparation, liner was placed on the deep cavity surface to mask the dark amalgam stain. The liner was light-cured for 20 seconds. A wide bevel was placed on the occlusal surface, and then a ring and matrix were placed. A selective enamel etching was performed with 37% phosphoric acid (Figure 3), rinsed, and dried. Universal bond was prepared by adding one drop from each bottle of the adhesive product into a mixing well and then briefly mixing. The bond was then placed (Figure 4) and air-dried with low air for 5 seconds, then with stronger air for another 5 seconds. No light-curing was needed for this bonding system. Then, one-shade composite was placed in small increments using a condenser. Before light-curing, some occlusal anatomy was created using hand instruments, including an acorn-shaped burnisher (Figure 5) and blue titanium CIB3. The occlusal adjustments and more detailed anatomy were created using a football-shaped diamond bur and a needle-shaped diamond bur. The final finishing and polishing were done using a large, coarse disc, a fine-needle diamond bur, and white Arkansas stone. A postoperative photograph (Figure 6) showed how the restoration blended naturally with the tooth. Figure 7 and Figure 8 feature a bitewing x-ray and photograph of the tooth taken during the 6-month recall examination.
This Class II restoration demonstrated the versatility and ease of use provided by universal bonding agents. These bonding agents, such as the one used in this case, provide an all-in-one bond system that does not require light-curing, surface agitation, or a post-placement wait period.5 Universal bonding agents save time when multiple restorations in quadrant dentistry are performed. Additional activators and primers were not needed, reducing inventory cost and chairtime compared with using a non-universal bonding agent.5 A final benefit involves the reduced risk of failure in cases such as deep Class II restorations and post-and-core buildups that are difficult to reach and fully cure with light-curing.11 These agents also offer high bond strength and no postoperative sensitivity.
When using a universal bonding agent with a universal composite, the author recommends always making a clean and neat cavity preparation without leaving any superficial caries and stains that could show through the potential translucency of the composite. Any dark amalgam stains should be masked with an opaquer. Also, a wide bevel should be made on the enamel surface so that the composite can blend well with the existing enamel and dentin. Finally, proper hand instruments and burs should be used for occlusal anatomy to create a natural-looking restoration.
Case 2: Indirect Restoration
The benefits of universal bonding agents are demonstrated further with the following indirect restoration case example. This restoration was completed in August of 2020. The patient was a 41-year-old man. During the complete examination, it was noted that his lower left first molar (tooth No. 19) was worn and broken with a very deep cavity (Figure 9). The patient described a history of spontaneous pain. The photograph was taken with an intraoral camera. A preoperative periapical x-ray revealed large caries in the pulp chamber. The patient was referred to an endodontist for root canal treatment. After the endodontic treatment was completed, a periapical x-ray was taken before the start of the crown preparation and impression for the laboratory.
After anesthetic with 2% lidocaine with 1:100,000 epinephrine, the temporary filling material was removed. A post space was made on the distal canal with a drill using a slow-speed handpiece. A medium-sized, gold-plated post was passively cemented and cured for 20 seconds. Then the tooth was acid-etched with 37% phosphoric acid, rinsed, and dried. After the tooth was well dried, universal bond was placed and lightly air-dried (Figure 10). No light-curing was needed for this bonding system. After placing a first retraction cord impregnated with epinephrine, the final crown margin preparation was completed. Then the second retraction cord was placed before the final impression. Figure 11 (with second cord) shows the tooth with a buildup material and retraction cords impregnated with epinephrine. After 10 minutes, the second retraction cord was removed and the final impression for a crown was taken using a polyvinyl siloxane. Then the impression was sent to the laboratory.
After 2 weeks, the crown was back from the laboratory. The temporary was removed, the crown was placed on the tooth, the interproximal contacts were checked with dental floss, and the occlusion was examined. Before the final cementation, a bitewing x-ray was taken to confirm the seal of the mesial and distal margins. After the seal was confirmed, the tooth was isolated with cotton rolls, and universal bond was prepared, applied to the crown (Figure 12) and tooth (Figure 13), and lightly air-dried. Cement was placed on the crown, and the crown was then placed on the tooth (Figure 14). Figure 15 shows the crown after the final cementation. The cement and universal bond pairing allowed for self-etch adhesion and required no additional activators or primers.
This indirect restoration again demonstrated the versatility of universal bonding agents. Throughout this procedure the clinician did not need to be concerned whether light-curing would be sufficient to fully cure the bonding agent, and even through such an expansive restoration, he could rely on the bonding agent to maintain its strength for a long-lasting, sturdy result.11
Conclusion
Bonding agents have gone through generations of development to reach their current level of technology. Although each doctor may have his or her own preference, universal bonding agents provide the strength and reliability needed in modern dentistry. With some of these universal bonding agents no longer requiring light-curing, doctors can feel secure knowing that their restorations will have a reduced chance of adhesive failure often seen in light-cured restorations. As demonstrated by the two cases above, universal bonding agents can leave behind beautiful and strong restorations with a long-lasting lifetime. As technology continues to improve, new developments will continue; however, universal bonding agents represent some of dentistry's most important developments for today's dentists.
About the Author
James Chae, DDS, MS
Private Practice
Diamond Bar, California
References
1. Anusavice K, Shen C, Rawls HR. Phillips' Science of Dental Materials. 12th ed. St. Louis, MO: Saunders; 2013:258.
2. Helvey GA. The history of adhesive bonding. Kerr University Online Learning Center. https://cdeworld.com/courses/4508-the-history-of-adhesive-bonding. Published April 2011. Accessed September 14, 2020.
3. Sofan E, Sofan A, Palaia G, et al. Classification review of dental adhesive systems: from the IV generation to the universal type. Ann Stomatol (Roma). 2017;8(1):1-17.
4. Understanding the newest generation of adhesives: universal bonding agents. The Dental Advisor. 2013;30(2):1-2.
5. Tokuyama Universal Bond Technical Report Ver 1.2. Tokuyama Dental Corp. https://cdn2.hubspot.net/hubfs/4088199/TOKUYAMA%20UNIVERSAL%20BOND%20TR%20170221.pdf. Published February 21, 2017. Accessed July 19, 2020.
6. Total versatility. Uncompromising performance. 3M. https://multimedia.3m.com/mws/media/1275587O/3m-scotchbond-universal-adhesive-total-versatility.pdf. Published 2016. Accessed July 21, 2020.
7. Adams-Mott A. What are the average expenses of dentists? Chron. https://smallbusiness.chron.com/average-expenses-dentists-47536.html. Accessed September 16, 2020.
8. Dudney TE. Saving time and money with 8th-generation bonding agents. Dental Economics. https://www.dentaleconomics.com/science-tech/article/16384966/saving-time-and-money-with-8thgeneration-bonding-agents. Published June 1, 2018. Accessed September 16, 2020.
9. Jadhav S, Hegde V, Aher G, Fajandar N. Influence of light curing units on failure of direct composite restorations. J Conserv Dent. 2011;14(3):225-227.
10. Kachalia P. Don't take light curing for granted: improper curing can lead to failure. Dental Economics. https://www.dentaleconomics.com/science-tech/article/16389522/dont-take-light-curing-for-granted-improper-curing-can-lead-to-failure. Published December 5, 2017. Accessed July 20, 2020.
11. Moore BK, Platt JA, Borges G, et al. Depth of cure of dental resin composites: ISO 4049 depth and microhardness of types of materials and shades. Oper Dent. 2008;33(4):408-412.
12. Pouyanfar H, Tabaii ES, Aghazadeh S, et al. Microtensile bond strength of composite to enamel using universal adhesive with/without acid etching compared to etch and rinse and self-etch bonding agents. Open Access Maced J Med Sci. 2018;6(11):2186-2192.
13. 3M. Five things you need to know about adhesives. Dental Products Report. https://multimedia.3m.com/mws/media/1524496O/3m-single-bond-universal-adhesive-dpr-article.pdf. Accessed July 24, 2020.