You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
More than 36 million Americans are completely edentulous; 90% of these individuals have dentures.1 Complete edentulism is associated with decreased masticatory function, speech impairment, and unfavorable esthetics (due to loss of support for the facial musculature).2 In the past, losing most or all of one's teeth was considered part of the inevitable aging process, and the only solution available was conventional removable dentures.
Although conventional dentures remain a viable option, there are disadvantages for patients. Dentures require lifestyle adjustments: for example, they must be removed and cleaned daily to avoid problems with hygiene and bad breath, and they can cause difficulties with speaking and eating, especially certain foods. Patients who wear conventional dentures often complain about the instability of the prosthesis, particularly the mandibular denture.3,4 This instability leads to a feeling of insecurity, inefficient mastication, and overall dissatisfaction with the prosthesis. Over time, conventional denture wearers also generally experience significant bone loss in the jaw,5 which causes the dentures to fit poorly, requiring them to be relined or replaced frequently. Bone loss can also change the facial contours, making a person look older.
Implant-supported fixed dentures and overdentures provide two alternatives to conventional dentures. When a full-arch prosthesis is being considered, sometimes a fixed restoration is not feasible, either for financial reasons or because of anatomical factors. For example, patients may have significant bone resorption if they have not received implant treatment after the loss of their teeth or have been wearing traditional dentures for an extended period.6 This condition can make it difficult to achieve the anterior-posterior spread needed for a fixed restoration without sinus lifts, ridge modification, or similar complex treatment. For these patients, an implant overdenture is an option that results in better stability, function, and overall satisfaction than a traditional denture.7 A mandibular implant overdenture improves support and retention, which reduces denture movement and helps in achieving better chewing efficiency and masticatory bite force. Implant-supported prostheses have a high long-term success rate (95.5% after 20 years for implants, compared with 80% for overdentures), especially in the mandible.8,9
Treatment Planning
An overdenture is any removable dental prosthesis that rests on one or more remaining natural teeth, the roots of natural teeth, or dental implants. Overdentures can stop the progression of bone loss and restore the ability to eat and speak properly, improving patients' quality of life. They reduce bone loss by creating tensile stress,10 which occurs when occlusal forces are transmitted to the alveolar bone by the periodontal ligament. Thus, overdentures are one way to delay complete edentulism and help in the preservation of bone. The main feature setting an overdenture apart from a traditional denture is that it gains support and stability from remaining teeth and dental implants.11 The prosthesis is secured with clips or other fasteners, but it can be removed for daily cleaning and repairs when necessary. The factors determining whether an implant-supported overdenture is the best option can be divided into patient level and arch level.
At the patient level, there is a significant quality-of-life effect associated with dentures that improves patient confidence. The first step for the clinician is to determine patients' expectations by listening to their needs, desires, and limitations,12 which will reveal the requisite functional demands of the denture. For example, some patients may be satisfied with minimal movement, allowing a tissue-supported implant. Long-term maintenance requirements for each option are also a consideration. Along with understanding patients' functional requirements, clinicians should understand patients' oral hygiene habits, financial commitment, time frame, and esthetic and phonetic demands. Before beginning any procedures, medical and dental history should be well-documented, and it is critical to examine both the bone and soft tissue that are essential for maintaining the implant and prosthesis.
At the arch level, deciding factors include advanced resorption of alveolar ridges caused by the deficiency of the primary bearing area (buccal shelf), a sharp mylohyoid ridge, and deficiencies due to congenital conditions, trauma, maxillofacial surgery, or failure of a previous fixed implant prosthesis.13 Such deficiencies may not preclude the feasibility of overdentures; however, they may impact the type and number of implants used.
Comparative prospective studies validate the benefit of two or four implants in the edentulous mandible.14,15 When two-implant overdenture groups and four-implant overdenture groups are compared, patient satisfaction appears to be equivalent. Increased minimum of implants in the maxilla compared with the mandible is due to the softer bone and the distribution of occlusal forces. However, the use of just two maxillary implants does not compromise implant survival or patient satisfaction.16-18 Rates in the two-implant overdenture groups compared with four-implant overdenture groups appear to be equivalent in patient satisfaction.19 However, over time, patients with just two implants may complain about fit because bone retention was localized around the implants, whereas other areas experienced bone loss. Implants reduce bone resorption and minimize clinical complications20,21; therefore, the best solution may be to place additional implants to maintain more bone.
Because bone is critical for the long-term success of implant-supported removable dentures, it is one of the primary factors to evaluate. Important factors include the clinical examination, photography, study models, and radiology. Increasingly common, cone-beam computed tomography (CBCT) imaging has improved diagnostic abilities, allowing practitioners to visualize all dimensions of the edentulous bone before surgical intervention.
In the past, a surgical guide was used to place implants for aiding the retention and support of dentures. This time-consuming process involved the duplication of the current denture, sometimes requiring multiple inconvenient appointments for patients. Now, although surgical guides are still useful, one of the best techniques for designing overdentures for edentulous patients is a dual-arch scan.22 First, marks for placement are put on the prosthesis, which is inserted in the patient's mouth and scanned. Then the prosthesis is removed and scanned alone. The final step in a dual scan is to merge the files to determine the soft-tissue position and design a plan for the teeth. Before the implants are placed, the prosthesis must fit precisely, or a new prosthesis should be created. Otherwise, no matter the retention design, the patient will not be satisfied with how the overdentures feel.
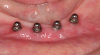
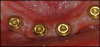
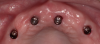
The degree of retention for overdenture attachments depends on design, location, alignment of supporting dental implants, and the type of attachments. A variety of retention designs are available for attaching the overdenture, including clips and bars, ball attachments, magnets, and telescopic copings (Figure 1 through Figure 3).23 Studies show that bar attachments have a higher retention force than magnet attachments.24-26Placement in viable bone and angulation of the implants are critical. Inadequate space for prosthetic components can result in an overly contoured prosthesis, excessive occlusal vertical dimension, fractured teeth adjacent to the attachments, attachments separating from the denture, fracturing of the prosthesis, and overall patient dissatisfaction.27 CBCT scanning and online planning technologies allow clinicians to evaluate each implant location in 360 degrees.
Placing the Prosthesis
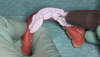
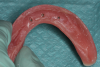
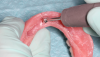
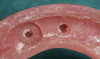
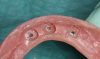
The first step in preparing to place the prosthesis is to make an impression of the overdenture with a light-body impression material to show position of the attachments (Figure 4). A sharp-pointed bur is used to drill straight through the center of the implant position so that when the impression material is pulled out, the exact center of the implant position is revealed (Figure 5 and Figure 6). Next, a drill with a sharp point should be fit into that hole, giving, in this case, a 4-mm deep by 4-mm wide receptacle for the attachment (Figure 7 and Figure 8). The last bur is used to create an undercut all around the receptacle area to help with retention (Figure 9 and Figure 10).
After the chosen abutments are placed and the prosthesis is drilled, it is time for the pick-up. The first step is to verify there is enough space by determining vertical dimension. After the vertical seats properly, block-out spacers and material should be used over the head of each abutment to make sure the denture does not become locked in place. This blocks out the area immediately surrounding the abutment, allowing the full resilient function of the pivoting metal denture cap. A light-cure or self-cure acrylic resin should be placed in the prosthesis reservoirs and around the abutments.
Finally, the denture should be inserted. The patient should be guided into occlusion without compressing the soft tissue while the overdenture material sets. After the acrylic has cured, the denture should be removed and the white spacer should be discarded, leaving only the metal denture cap. A retention insert can then be placed into the denture cap, seated securely, and leveled with the rim of the cap. Then the prosthesis should be delivered by seating the overdenture onto the abutments. Any minor modifications to the occlusion and tissue side of the denture can be made; it should then be polished. The patient should be instructed on how to properly insert and remove the prosthesis.
For implant-maintained soft-tissue-supported prostheses, maintenance is crucial. The silicone or plastic ring-inserts inside the denture will require replacement every year. The overdenture will require a laboratory hard reline every 3 years. Statistically, the overdenture will need to be replaced every 7 to 10 years. Hygiene is imperative. Twice-annual cleanings, an oral cancer screening, photographs to compare changes over time, and radiographs of the implants once a year are also important. Cleaning tools and products specific to denture and implant maintenance can be recommended to the patient.
Options for Patients
Another attachment alternative is known as implant-retained implant-supported, which is still removable. It includes a 5-mm titanium abutment and a gold cap on the inside. It requires more space than other options, about 12 mm.
Overdentures are not just for fully edentulous patients. Removable overdentures are also an option for patients with partial dentures. Overdentures not only improve speech and dental function but have been shown to dramatically increase social confidence and emotional well-being. Thorough review of a patient's biologic, functional, and personal requirements is vital for determining the most satisfying and clinically successful option.
About the Author
David A. Little, DDS
Private Practice
Adjunct Clinical Professor
University of Texas Health Dental School
San Antonio, Texas
References
1. American College of Prosthodontists. Facts & Figures. https://www.gotoapro.org/facts-figures/. Accessed November 9, 2019.
2. Sharma AJ, Nagrath R, Lahori M. A comparative evaluation of chewing efficiency, masticatory bite force, and patient satisfaction between conventional denture and implant-supported mandibular overdenture: an in vivo study. J Indian Prosthodont Soc. 2017;17(4):361-372.
3. Pietrokovski J, Harfin J, Mostavoy R, et al. Oral findings in elderly nursing home residents in selected countries: quality of and satisfaction with complete dentures. J Prosthet Dent. 1995;73(2):132-135.
4. Berg E. The influence of some anamnestic, demographic, and clinical variables on patient acceptance of new complete dentures. Acta Odontol Scand. 1984;42(2):119-127.
5. Bergman B, Carlsson GE. Clinical long-term study of complete denture wearers. J Prosthet Dent. 1985;53(1):56-61.
6. López-Roldán A, Abad DS, Bertomeu IG, et al. Bone resorption processes in patients wearing overdentures. A 6-years retrospective study. Med Oral Patol Oral Cir Bucal. 2009;14(4):E203-209.
7. Thomason JM, Kelly SA, Bendkowski A, Ellis JS. Two implant retained overdentures-a review of the literature supporting the McGill and York consensus statements. J Dent. 2012;40(1):22-34.
8. Ettinger RL, Qian F. Abutment tooth loss in patients with overdentures. J Am Dent Assoc. 2004;135(6):739-746.
9. Vercruyssen M, Marcelis K, Coucke W, et al. Long-term, retrospective evaluation (implant and patient-centred outcome) of the two-implants-supported overdenture in the mandible. Part 1: survival rate. Clin Oral Implants Res. 2010;21(4):357-365.
10. Samra RK, Bhide SV, Goyal C, Kaur T. Tooth supported overdenture: a concept overshadowed but not yet forgotten! J Oral Res Rev. 2015;7(1):16-21.
11. Boven GC, Raghoebar GM, Vissink A, Meijer HJ. Improving masticatory performance, bite force, nutritional state and patient's satisfaction with implant overdentures: a systematic review of the literature. J Oral Rehabil. 2015;42(3):220-233.
12. Pjetursson BE, Lang NP. Prosthetic treatment planning on the basis of scientific evidence. J Oral Rehab.2008;35(suppl 1):72-79.
13. Nissan J. Implant-supported overdentures: benefits and risks. In: Mersel A, ed. Oral Rehabilitation for Compromised and Elderly Patients. Cham, Switzerland: Springer; 2018:183-191.
14. Visser A, Raghoebar GM, Meijer HJ, et al. Mandibular overdentures supported by two or four endosseous implants. A 5-year prospective study. Clin Oral Implants Res.2005;16(1):19-25.
15. Stoker GT, Wismeijer D, van Waas MAJ. An eight-year follow-up to a randomized clinical trial of aftercare and cost-analysis with three types of mandibular implant-retained overdentures. J Dent Res. 2007;86(3):276-280.
16. Ekfeldt A, Christiansson U, Eriksson T, et al. A retrospective analysis of factors associated with multiple implant failures in maxillae. Clin Oral Implants Res. 2001;12(5):462-467.
17. Kronström M, Widbom C, Soderfeldt B. Patient evaluation after treatment with maxillary implant-supported overdentures. Clin Implant Dent Relat Res. 2006;8(1):39-43.
18. Weingart D, ten Bruggenkate CM. Treatment of fully edentulous patients with ITI implants. Clin Oral Impl Res. 2000;11(suppl 1):69-82.
19. Timmerman R, Stoker GT, Wismeijer D, et al. An eight-year follow-up to a randomized clinical trial of participant satisfaction with three types of mandibular implant-retained overdentures. J Dent Res. 2004;83(8):630-633.
20. Awad MA, Lund JP, Dufresne E, Feine JS. Comparing the efficacy of mandibular implant-retained overdentures and conventional dentures among middle-aged edentulous patients: satisfaction and functional assessment. Int J Prosthodont.2003;16(2):117-122.
21. Doundoulakis JH, Eckert SE, Lindquist CC, Jeffcoat MK. The implant-supported overdenture as an alternative to the complete mandibular denture. J Am Dent Assoc. 2003;134(11):1455-1458.
22. Misch CE. Contemporary Implant Dentistry. 3rd ed. London, England: Elsevier Health Sciences; 2007.
23. Savabi O, Nejatidanesh F, Yordshahian F. Retention of implant-supported overdenture with bar/clip and stud attachment designs. J Oral Implantol. 2013;39(2):140-147.
24. Burns DR, Unger JW, Elswick RK Jr, Giglio JA. Prospective clinical evaluation of mandibular implant overdentures: part II-patient satisfaction and preference. J Prosthet Dent. 1995;73(4):364-369.
25. Naert I, Gizani S, Vuylsteke M, Van Steenberghe D. A 5-year prospective randomized clinical trial on the influence of splinted and unsplinted oral implants retaining a mandibular overdenture: prosthetic aspects and patient satisfaction. J Oral Rehabil. 1999;26(3):195-202.
26. Mericske-Stern R, Grütter L, et al. Clinical evaluation and prosthetic complications of single tooth replacements by non-submerged implants. Clin Oral Implants Res. 2001;12(4):309-318.
27. Bansal S, Aras MA, Chitre V. Guidelines for treatment planning of mandibular implant overdenture. J Dent Implant. 2014;4(1):86-90.