You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Saliva is a complex fluid that is essential for the maintenance of good oral and general health. It is composed mostly of water but also, in smaller part, a variety of nonorganic and organic substances such as enzymes, hormones, antibodies, antimicrobial constituents, and growth factors.1 In the oral cavity, saliva is vital because of its function in digestion, mastication, swallowing, and speech, and it enables free movement of oral tissues and maintains mucosal integrity.1-3 Furthermore, saliva proteins are necessary contributors to the lubrication of oral tissues and, thus, guard the mucosal tissues from various injuries, whether chemical or physical. Similarly, the enzymes, immunoglobulin A, and histamines in saliva all have been shown to provide local antimicrobial activity.4
Deficiency or absence of salivary flow, which is common among elderly people, may lead to complaints of dry mouth, or xerostomia. Salivary dysfunction in geriatric patients is mainly due to systemic diseases, medications, and head and neck radiation therapy.4 Research findings about the prevalence of xerostomia in the general population has varied greatly.5,6 Estimates range from 10% to 46%, with 9.7% to 25.8% of men affected and 10.3% to 33.3% of women.7 Among the elderly, it was demonstrated that xerostomia occurs in approximately 35% of individuals over the age of 65.4,8 In older adults, xerostomia can increase the risk for dental caries, particularly root caries, and it may increase the incidence of periodontal diseases and oral infections, such as candidiasis. Furthermore, saliva plays an important role in denture use, and, thus, xerostomia can have a significant and adverse effect on people who wear dentures.7 Patients with this condition may often consume sweet or acidic drinks to help alleviate xerostomia symptoms, thereby increasing the risk for dental caries.9,10
With the increased incidence of xerostomia among the elderly population, dental clinicians need to understand this condition and the various complications it can cause and be prepared to provide treatment options to these patients. This article will discuss the various causes of xerostomia and the chief complications and consequences it has on the oral cavity. Finally, it will present both the pharmacologic and nonpharmacologic agents that are used to aid patients with this condition.
Causes
Three major etiological factors may cause hyposalivation in the elderly population. First, it is now well established that the use of numerous medications is the most common cause of xerostomia, especially among the elderly. Second, salivary disorders in the aging population may result from several medical conditions such as Sjögren’s syndrome, diabetes mellitus, and Alzheimer’s disease.11 Finally, head and neck radiation therapy and chemotherapy can contribute to salivary gland diseases and subsequently to xerostomia.11-13
Drugs That May Cause Xerostomia
The foremost cause of salivary disorders is the use of prescription and nonprescription medications.11 The high rate of polypharmacy among the elderly may lead to many adverse drug reactions,14 including xerostomia. Drugs with xerostomic effects can be found in 42 categories and 56 subcategories.4,15 The most common medications prescribed to the elderly causing hyposalivation are those with anticholinergic properties and sympathomimetic drugs.1,3 Other drugs commonly associated with dry mouth include tricyclic antidepressants, sedatives, and tranquilizers; antihistamines; cytotoxic agents; and antiparkinson and anti-epilepsy medications.11 These agents aim at either inhibiting neurotransmitters from binding to salivary gland membrane receptors or altering ion transport pathways in the acinar cell and, subsequently, may affect salivary gland function, which may result in hyposalivation.11 Moreover, the effect of chemotherapeutic agents on salivary gland function is well known;16 however, xerostomia is usually temporary in these cases.4,7 Finally, radioactive iodine, which is used to treat thyroid cancer, may affect salivary gland function and cause xerostomia.4
In addition to prescription drugs, elderly patients are known to consume many over-the-counter medications.14 Those associated with xerostomia are used to treat allergies, motion sickness, congestion, and diarrhea. Many medications that have been reported to cause xerostomia do not damage salivary gland function, but, rather, the decreased salivary flow is mainly due to polypharmacy and comorbidities.
Table 1 provides a summary of drugs commonly associated with xerostomia.
Salivary Gland Disorders
As the most common disease that causes xerostomia in geriatric patients, Sjögren’s syndrome is an idiopathic autoimmune disorder in which multiple organs and tissues are affected.17 Clinical manifestations of Sjögren’s syndrome present in either primary or secondary forms. Primary Sjögren’s syndrome is characterized by xerostomia and xerophthalmia (dry eyes), and secondary Sjögren’s syndrome can coexist with connective tissue diseases, such as rheumatoid arthritis. Xerostomia is also a common complaint of patients with uncontrolled diabetes,4,7 and this is possibly due to polyuria, dehydration, and autonomic dehydration. Other disorders that have been implicated with xerostomia include hepatitis C, thyroid gland diseases, and adrenal conditions. Finally, psychogenic conditions such as depression, stress, and anxiety, which are common among the elderly, can also result in xerostomia.4,18
Radiation Therapy
Patients undergoing radiation therapy as part of cancer treatment may receive external beam radiation. This can lead to severe and often permanent salivary hypofunction and, thus, may prompt persistent complaints of xerostomia.4,12 Although the prevalence of xerostomia due to radiation therapy varies greatly, it has been reported to be from 73.5% to 93%.19,20 The mechanism causing xerostomia in radiation therapy is not completely understood; however, it has been suggested that acute xerostomia may be due to severe inflammatory action, whereas late-occurring xerostomia probably involves the fibrosis of salivary glands and the lysis of acinar cells.4,21,22
The standard radiation for head and neck neoplasms may imply fractionated doses of 10 grays (Gy) every week over a 5- to 7-week period to an average 60-Gy dose.1 Although the degree of the salivary gland damage depends on the number of salivary glands exposed, length of the radiation, and the area exposed, it has been suggested that the fibrosis and loss of the acinar cells occurs in patients receiving therapeutic dosages that exceed 60 Gy.1,4,8,11 Quality of life in patients receiving radiation therapy is strongly affected by xerostomia and its associated complications.1 For instance, Kakoei et al22 assessed the severity of xerostomia in patients with head and neck cancers after radiation therapy and its impact on quality of life. Their research demonstrated that with each milliliter decrease in saliva secretion, the quality-of-life score decreased 2.25%. Although complete recovery in some cases is possible, xerostomia may develop into an irreversible and lifelong problem with significant debilitating factors.1 That being said, intensity-modulated radiation therapy and dose-delivery techniques can minimize radiation exposure and improve xerostomia-affected quality of life.4,23,24
Oral Complications
Patients with xerostomia have multiple oral health consequences. This is because saliva is important for many functions in the oral environment and gastrointestinal system. It is essential for chewing, speaking, and tasting. Thus, when saliva is lacking, several oral and extraoral disorders can develop, such as Sjögren’s syndrome, caries related to hyposalivation, and periodontal disease.11 Also, saliva is needed to detect and recognize gustatory stimuli, and this may be diminished in patients with xerostomia. Often, to compensate for these deficiencies, patients may alter their food and beverage choices and potentially compromise their nutritional status.11
Another important role of saliva is to aid in the retention and comfort of removable dentures. Absence of saliva in the interface of the denture and mucosa can cause sores and other traumatic ulcerations of the mucosa due to the lack of lubrication and denture retention.1,25
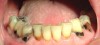
Dental caries, both new and recurrent, is also a frequently occurring infection resulting from lack of saliva. Older adults are particularly vulnerable because many have a greater number of retained natural teeth, previously restored dental surfaces, and gingival recession.11 Recurrent carious lesions are seen particularly in the buccal surfaces of previously restored anterior teeth and in incisal margins4 (Figure 1). Without proper salivary flow to restore the oral pH levels and to regulate bacterial populations, the oral cavity is rapidly colonized with caries-associated microorganisms.11 In regard to periodontal disease, the evidence in the literature is conflicting as to whether individuals with xerostomia are at an increased risk for periodontal disease. Some studies26-31 showed that the periodontal condition of individuals with Sjögren’s syndrome is similar to control individuals, whereas others demonstrated that these patients may have a worse periodontal condition compared to controls.32-34 These studies attributed the poorer periodontal conditions observed in individuals with xerostomia to the decrease in the amount of saliva and, consequently, the increase in plaque.35
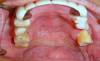
Finally, a lack of saliva may increase the incidence of oral fungal infection, especially candidiasis. Angular cheilitis and atrophy of the tongue papillae or buccal mucosa are common oral mucosal symptoms in patients with xerostomia.36 Closely linked with changes in the oral microbial flora, these conditions are caused mainly by Candida species, which are present in the oral mucosa, intestines, and skin.36,37 The interactions with salivary proteins partly affect Candida oral colonization.38 The oral microbiota may change, thereby increasing the risk for opportunistic infections (Figure 2).
Table 2 summarizes the oral complications and other consequences seen in patients with xerostomia.
Treatment
Because identifying the cause of xerostomia is essential, the initial step in the management of patients with this condition is to establish a diagnosis. For instance, older patients may have several comorbidities and may take many medications that can, in turn, precipitate xerostomia. As such, reviewing the patient’s medical and drug histories may be beneficial. Moreover, if a patient is identified as having xerostomia, the dental clinician should evaluate the patient for any oral and dental complications and then treat as needed. Patients with xerostomia should be encouraged to drink water while eating and eliminate sweets, sweeteners in foods and drinks, and various other sugar products due to the increased incidence of dental caries.1,7,11 After establishing a diagnosis, the clinician can suggest treatment options. Management of xerostomia is divided into two categories: local and systemic salivary stimulation.
Local Salivary Stimulation
Local salivary stimulation includes the use of saliva substitutes to try to help reduce xerostomia. Saliva substitutes used commercially in North America frequently are carboxymethylcellulose based and are often short in relief duration.39 For instance, sugarless gums are an effective local stimulant because the chewing motion increases salivation. Another local measure is the use of vitamin C. Björnström et al40 compared the effectiveness of vitamin C to artificial saliva and other saliva stimulants in patients with xerostomia and found vitamin C was more effective than artificial saliva; however, vitamin C has a detrimental effect on teeth enamel. Other local measures include adhesive discs to lubricate the mouth (eg, Oramoist®, DenTek, www.dentek.com; OraCoat® XyliMelts®, OraHealth Corporation, www.oracoat.com) and various water-soluble lubricants (K-Y® Jelly, Reckitt Benckiser, www.k-y.com; Taro-Gel®, Taro Pharmaceuticals Inc., www.taro.ca; Biotene® products, GlaxoSmithKline, www.biotene.com) that can be applied by foam brush or finger.39 Although these measures are used with various success rates in many patients, their main disadvantage is limited effectiveness during the night when symptoms are most severe.4
Systemic Salivary Stimulation
Stimulation of saliva can be achieved using pharmacologic interventions. Drugs used to increase salivary flow are termed sialagogues. These medications are effective in increasing salivary secretions and have been shown to decrease xerostomic complaints in patients. Four main drugs are included in this category: pilocarpine, cevimeline, bethanechol chloride, and anethole trithione.11,41-43
Pilocarpine—Pilocarpine is a muscarinic agonist that can stimulate cholinergic receptors on the surface of acinar cells.40-42 Findings from several trials have shown that the use of this drug can significantly reduce the symptoms of radiation-induced xerostomia when pilocarpine is administered orally during radiation therapy.44-47 Recommended dosages are 3 mg to 5 mg, three times per day. Adverse effects such as sweating, nausea, dizziness, and increased pulmonary secretions have been reported.4,11,41,42 Because pilocarpine can cause dysfunction of the gastrointestinal, urinary, cardiovascular, and pulmonary systems, healthcare professionals should prescribe this medication with caution in patients with asthma, chronic pulmonary disease, and cardiovascular disorders.
Cevimeline—Another cholinergic agonist used for the treatment of xerostomia is cevimeline, which has been shown to have a higher affinity for M1 and M3 muscarinic receptor subtypes.48 Because M2 and M4 receptors are found on cardiac and lung tissues, cevimeline treatment should help with salivary secretions but also lower the adverse effects on pulmonary and cardiac function seen with pilocarpine.49 Cevimeline is contraindicated in patients with asthma,4 and its use in patients with narrow-angle glaucoma has also been cautioned.
Several studies demonstrated improvement of xerostomia when cevimeline was used.49,50 Moreover, in a double-blind, multi-dose, placebo-controlled phase-3 study that gauged salivary gland function in almost 200 patients with Sjögren’s syndrome, Fox et al51 showed that this agent considerably improved salivary flow rates and reduced xerostomia. The recommended dose for cevimeline is 30 mg, three times per day. Although in many studies cevimeline was well tolerated,49-51 side effects of this drug may include nausea, vomiting, diarrhea, runny nose, and excessive sweating.
Bethanechol chloride—Used extensively to treat dry mouth, bethanechol chloride is a cholinergic commonly prescribed to treat urinary retention and neurogenic atony of the bladder.5 This medication is used as a sialagogue because it stimulates the parasympathetic nervous system, which causes the release of acetylcholine at the nerve endings, triggering saliva production.52 Several reports demonstrated the effectiveness of bethanechol chloride as a drug to manage dry mouth.53-56 Moreover, in a recent double-blind randomized prospective trial, Jaguar et al57 examined the prophylactic use of bethanechol chloride to prevent salivary gland dysfunction during radiation therapy. A total of 97 patients were allocated into two groups: bethanechol chloride or placebo. The authors demonstrated that the bethanechol chloride group significantly improved salivary flow and concluded bethanechol chloride was effective in decreasing salivary gland damage.57 Bethanechol chloride is given in doses ranging from 10 mg to 50 mg three to four times per day.52 Some reported adverse effects include gastrointestinal upset, sweating, and miosis.52
Anethole trithione—Anethole trithione has been shown to increase the receptor sites on salivary acinar cells.4,52 Several clinical trials demonstrated its effectiveness in helping patients with xerostomia.58,59 A study by Epstein et al58 showed that patients who took anethole trithione had an improvement in saliva flow. Moreover, the combination of pilocarpine and anethole trithione was shown to have a synergistic effect on salivary secretion.60 The recommended dose for this drug is 25 mg three times daily. The reported side effects are gastrointestinal upset, flatulence, and abdominal pain.52
Table 3 lists the pharmacologic agents used for the treatment of xerostomia along with their recommended doses and the adverse effects associated with their use.
Conclusion
Salivary flow decreases with increasing age. This may lead to complaints of xerostomia. This dysfunction in geriatric patients is due largely to various systemic diseases, medications, and head and neck radiation therapy. This article reviewed these main causes and the primary oral consequences of xerostomia, along with the various treatment options for the management of this condition. Often challenged when encountering patients with dry mouth, clinicians must effectively diagnose and properly treat this condition.
Disclosure
The author had no disclosures to report.
About the Author
Aviv Ouanounou, BSc, MSc, DDS
Assistant Professor
Department of Clinical Sciences (Pharmacology)
Faculty of Dentistry
University of Toronto
Toronto, Ontario, Canada
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Mravak-Stipetić M. Xerostomia - diagnosis and treatment. Medical Sciences. 2012;38:69-91.
2. Guggenheimer J, Moore PA. Xerostomia: etiology, recognition and treatment. J Am Dent Assoc. 2003;134(1):61-69.
3. Scully C, Felix DH. Oral medicine—update for the dental practitioner: dry mouth and disorders of salivation. Br Dent J. 2005;199(7):423-427.
4. Gupta A, Epstein JB, Sroussi H. Hyposalivation in elderly patients. J Can Dent Assoc. 2006;72(9):841-846.
5. Murray Thomson W, Poulton R, Mark Broadbent J, Al-Kubaisy S. Xerostomia and medications among 32-year-olds. Acta Odontol Scand. 2006;64(6):249-254.
6. Jansson C, Johansson S, Lindh-Astrand L, et al. The prevalence of symptoms possibly related to the climacteric in pre- and postmenopausal women in Linköping, Sweden. Maturitas. 2003;45(2):129-135.
7. Hopcraft MS, Tan C. Xerostomia: an update for clinicians. Aust Dent J. 2010;55(3):238-244.
8. Lenander-Lumikari M, Loimaranta V. Saliva and dental caries. Adv Dent Res. 2000;14(1):40-47.
9. Saunders RH Jr, Meyerowitz C. Dental caries in older adults. Dent Clin North Am. 2005:49(2):293-308.
10. Ship JA, Pillemer SR, Baum BJ. Xerostomia in the geriatric patient. J Am Geriatr Soc. 2002;50(3):535-543.
11. Turner MD, Ship JA. Dry mouth and its effects on the oral health of elderly people. J Am Dent Assoc. 2007;138 suppl:15S-20S.
12. Shiboski CH, Hodgson TA, Ship JA, Schiødt M. Management of salivary hypofunction during and after radiotherapy. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;103 suppl:S66. e1-e19.
13. Bergdahl M. Salivary flow and oral complaints in adult dental patients. Community Dent Oral Epidemiol. 2000;28(1):59-66.
14. Ouanounou A, Haas DA. Pharmacotherapy for the elderly dental patient. J Can Dent Assoc. 2015;80:F18.
15. Sreebny LM, Schwartz SS. A reference guide to drugs and dry mouth—2nd edition. Gerodontology. 1997;14(1):33-47.
16. Epstein JB, Tsang AH, Warkentin D, Ship JA. The role of salivary function in modulating chemotherapy-induced oropharyngeal mucositis: a review of the literature. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2002;94(1):39-44.
17. Fox RI. Clinical features, pathogenesis, and treatment of Sjögren’s syndrome. Curr Opin Rheumatol. 1996;8(5):438-445.
18. Bergdahl M, Bergdahl J. Low unstimulated salivary flow and subjective oral dryness: association with medication, anxiety, depression, and stress. J Dent Res. 2000;79(9):1652-1658.
19. Dirix P, Nuyts S, Vander Poorten V, et al. The influence of xerostomia after radiotherapy on quality of life: results of a questionnaire in head and neck cancer. Support Care Cancer. 2008;16(2):171-179.
20. Pow EH, Kwong DL, McMillan AS, et al. Xerostomia and quality of life after intensity-modulated radiotherapy vs. conventional radiotherapy for early-stage nasopharyngeal carcinoma: initial report on a randomized controlled clinical trial. Int J Radiat Oncol Biol Phys. 2006;66(4):981-991.
21. Hensley ML, Schuchter LM, Lindley C, et al. American Society of Clinical Oncology clinical practice guidelines for the use of chemotherapy and radiotherapy protectants. J Clin Oncol. 1999;17(10):3333-3355.
22. Kakoei S, Haghdoost AA, Rad M, et al. Xerostomia after radiotherapy and its effect on quality of life in head and neck cancer patients. Arch Iran Med. 2012;15(4):214-218.
23. Eisbruch A, Ten Haken RK, Kim HM, et al. Dose, volume, and function relationships in parotid salivary glands following conformal and intensity-modulated irradiation of head and neck cancer. Int J Radiat Oncol Biol Phys. 1999;45(3):577-587.
24. Chambers MS, Garden AS, Kies MS, Martin JW. Radiation-induced xerostomia in patients with head and neck cancer: pathogenesis, impact on quality of life, and management. Head Neck. 2004;26(9):796-807.
25. Chandu GS, Hombesh MN. Management of xerostomia and hyposalivation in complete denture patients. Ind J Stomatol. 2011;2(4):263-266.
26. Almståhl A, Kroneld U, Tarkowski A, Wikström M. Oral microbial flora in Sjögren’s syndrome. J Rheumatol. 1999;26(1):110-114.
27. Ravald N, List T. Caries and periodontal conditions in patients with primary Sjögren’s syndrome. Swed Dent J. 1998;22(3):97-103.
28. Tseng CC. Periodontal status of patients with Sjögren’s syndrome: a cross-sectional study. J Formos Med Assoc. 1991;90(1):109-111.
29. Tervahartiala T, Ingman T, Sorsa T, et al. Proteolytic enzymes as indicators of periodontal health in gingival crevicular fluid of patients with Sjögren’s syndrome. Eur J Oral Sci. 1995;103(1):11-16.
30. Boutsi EA, Paikos S, Dafni UG, et al. Dental and periodontal status of Sjögren’s syndrome. J Clin Periodontol. 2000;27(4):231-235.
31. Kuru B, McCullough MJ, Yilmaz S, Porter SR. Clinical and microbiological studies of periodontal disease in Sjögren syndrome patients. J Clin Periodontol. 2002;29(2):92-102.
32. Najera MP, al-Hashimi I, Plemons JM, et al. Prevalence of periodontal disease in patients with Sjögren’s syndrome. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1997;83(4):453-457.
33. Celenligil H, Eratalay K, Kansu E, Ebersole JL. Periodontal status and serum antibody responses to oral microorganisms in Sjögren’s syndrome. J Periodontol. 1998;69(5):571-577.
34. Rhodus NL, Michalowicz BS. Periodontal status and sulcular Candida albicans colonization in patients with primary Sjögren’s Syndrome. Quintessence Int. 2005;36(3):228-233.
35. Antoniazzi RP, Miranda LA, Zanatta FB, et al. Periodontal conditions of individuals with Sjögren’s syndrome. J Periodontal. 2009;80(3):429-435.
36. Shinozaki S, Moriyama M, Hayashida JN, et al. Close association between oral Candida species and oral mucosal disorders in patients with xerostomia. Oral Dis. 2012;18(7):667-672.
37. Miyasaka NR, Unterkircher CS, Shimizu MT. Catalase activity of different Candida species after exposition to specific antiserum. Braz J Microbiol. 2008;39(1):35-39.
38. Janket SJ, Jones JA, Rich S, et al. Xerostomic medications and oral health: the Veterans Dental Study (part I). Gerodontology. 2003;20(1):41-49.
39. Wiseman M. Focusing on quality of life. Alpha Omegan. 2015;108(2):30-37.
40. Björnström M, Axéll T, Birkhed D. Comparison between saliva stimulants and saliva substitutes in patients with symptoms related to dry mouth. A multi-centre study. Swed Dent J. 1990;14(4):153-161.
41. Johnson JT, Ferretti GA, Nethery WJ, et al. Oral pilocarpine for post-irradiation xerostomia in patients with head and neck cancer. N Engl J Med. 1993;329(6):390-395.
42. Vivino FB, Al-Hashimi I, Khan Z, et al. Pilocarpine tablets for the treatment of dry mouth and dry eye symptoms in patients with Sjögren syndrome: a randomized, placebo-controlled, fixed-dose, multicenter trial. P92-01 Study Group. Arch Intern Med. 1999;159(2):174-181.
43. Petrone D, Condemi JJ, Fife R, et al. A double-blind, randomized, placebo-controlled study of cevimeline in Sjögren’s syndrome patients with xerostomia and keratoconjunctivitis sicca. Arthritis Rheum. 2002;46(3):748-754.
44. Haddad P, Karimi M. A randomized, double-blind, placebo-controlled trial of concomitant pilocarpine with head and neck irradiation for prevention of radiation-induced xerostomia. Radiother Oncol. 2002;64(1):29-32.
45. Zimmerman RP, Mark RJ, Tran LM, Juillard GF. Concomitant pilocarpine during head and neck irradiation is associated with decreased posttreatment xerostomia. Int J Radiat Oncol Biol Phys. 1997;37(3):571-575.
46. Valdez IH, Wolff A, Atkinson JC, et al. Use of pilocarpine during head and neck radiation therapy to reduce xerostomia and salivary dysfunction. Cancer. 1993;71(5):1848-1851.
47. Rieger JM, Jha N, Lam Tang JA, et al. Functional outcomes related to the prevention of radiation-induced xerostomia: oral pilocarpine versus submandibular salivary gland transfer. Head Neck. 2012;34(2):168-174.
48. Iwabuchi Y, Masuhara T. Sialogogic activities of SNI-2011 compared with those of pilocarpine and McN-A-343 in rat salivary glands: identification of a potential therapeutic agent for treatment of Sjögren’s syndrome. Gen Pharmacol. 1994;25(1):123-129.
49. Chambers MS, Posner M, Jones CU, et al. Cevimeline for the treatment of postirradiation xerostomia in patients with head and neck cancer. Int J Radiat Oncol Biol Phys. 2007;68(4):1102-1109.
50. Brimhall J, Jhaveri MA, Yepes JF. Efficacy of cevimeline vs. pilocarpine in the secretion of saliva: a pilot study. Spec Care Dentist. 2013;33(3):123-127.
51. Fox RI, Petrone D, Condemi J, et al. Randomized placebo controlled trial of SNI-2011, a novel M3 muscarinic receptor agonist for the treatment of Sjögren’s syndrome [abstract 288]. Arthritis Rheum. 1998;41:S80.
52. Grisius MM. Salivary gland dysfunction: a review of systemic therapies. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2001;92(2):156-162.
53. Everett HC. The use of bethanechol chloride with tricyclic antidepressants. Am J Psychiatry. 1975;132(11):1202-1204.
54. Schubert DS. The use of bethanechol chloride with phenothiazines: a case report. Am J Psychiatry. 1979;136(1):110-111.
55. Jham BC, Teixeira IV, Aboud CG, et al. A randomized phase III prospective trial of bethanechol to prevent radiotherapy-induced salivary gland damage in patients with head and neck cancer. Oral Oncol. 2007;43(2):137-142.
56. Gorsky M, Epstein JB, Parry J, et al. The efficacy of pilocarpine and bethanechol upon saliva production in cancer patients with hyposalivation following radiation therapy. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2004;97(2):190-195.
57. Jaguar GC, Lima EN, Kowalski LP, et al. Double blind randomized prospective trial of bethanechol in the prevention of radiation-induced salivary gland dysfunction in head and neck cancer patients. Radiother Oncol. 2015;115(2):253-256.
58. Epstein JB, Decoteau WE, Wilkinson A. Effect of Sialor in treatment of xerostomia in Sjögren’s syndrome. Oral Surg Oral Med Oral Pathol. 1983;56(5):495-499.
59. Schiødt M, Oxholm P, Jacobsen A. Treatment of xerostomia in patients with primary Sjögren’s syndrome with sulfarlem. Scand J Rheumatol Suppl. 1986;61:250-252.
60. Epstein JB, Schubert MM. Synergistic effect of sialagogues in management of xerostomia after radiation therapy. Oral Surg Oral Med Oral Pathol. 1987;64(2):179-182.