You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
To view a clinical case exemplifying the principles discussed in this CE article, click here.
Screw-retained implants have ushered in an era of replacing missing teeth that has continued to progress with improved implant designs, more predictable clinical techniques, and an expanding selection of dental materials to support their use.1,2 There is no doubt that the use of dental implants to replace lost or missing dentition has become commonplace in the contemporary dental practice.3 With modifications to the implant process, the provisionalization procedure has become a treatment option for certain types of tooth replacement techniques, making cementation an issue at the surgical appointment, in addition to completing the final implant-supported restoration.4-6
As implants have continued to enjoy success as a tooth replacement option, constant innovations have been presented to improve esthetics and facilitate the restorative process. Implant manufacturers offer many options for screw-retained and cement-retained restorations.7 One of the major negative issues with cement-retained restorations is retrievability.7
Advantages to screw-retained implant crowns include their use in limited interocclusal spaces, absence of cement in the gingival sulcus area, predictable crown retention on the implant, and retrievability of the crown should it need to be removed. Disadvantages include the screw access opening interfering with occlusal contacts, compromised esthetics, a loosening at the occlusal surface, and the fact that potential altering of the implant placement may be required.7-10 Even with these disadvantages, screw-retained restorations are still a popular treatment option.
An alternative option to screw-retained implant restorations is the cement-retained implant crown. Advantages to cement-retained crowns can include a passive fit of the implant crown, excellent esthetic results, ideal occlusal design, along with the ability to routinely achieve ideal implant placement. An unaltered framework or abutment design can decrease porcelain failure while allowing the use of conventional crown-and-bridge procedures. Additionally, the implant abutment-crown microgap is sealed and can prevent bacterial debris from migrating into the abutment-crown space.7-10
Cement-retained implant restorations are not without issues. Weber et al11 compared peri-implant soft tissues of cement-retained and screw-retained restorations and reported poorer soft tissue health associated with cement-retained restorations. Other reports have documented the adverse effects of excess cement which extruded into the peri-implant soft tissues.12,13 Excess cement contributed to more than 80% of peri-implant disease in one documented study.14 Techniques have been presented to minimize the incidence of having excess cement in the peri-implant area after cementation.15-17 However, clinical examination of the peri-implant area should be a routine procedure to ensure excess cement removal.
Retention of a cement-retained, implant-supported prosthesis depends on many factors; these include taper, length, width, surface area, finish, and number of implant abutments.18 Singer et al found over a 3-year follow-up that most cement failures occurred in implant-supported fixed partial dentures (FPDs) fabricated in the posterior region with short, 3-mm to 4-mm abutment heights.19 Various authors have shown that the choice of cement material, amount of cement space or internal relief, occlusal forces, and type of luting agent can also affect the retentiveness of final restorations.20-28
Cements for Cement-Retained Implant Restorations
When treatment planning cement-retained implant crowns, the clinical success and durability of these definitive restorations include many factors, including the choice and clinical technique for a definitive cement for final cementation. Patient evaluation for cement-retained implant restorations should include a number of criteria based on specific physical properties and handling characteristics.29-31 The ideal properties for this cement should include:
- low viscosity for easy seating
- easy to mix
- extended working time
- short setting time
- film thickness compatible with complete seating
- insolubility in the mouth
- high shear strength
- high tensile strength
- high compressive strength
- biocompatible with gingival tissues
- radiopaque
- easy post-cementation clean-up
Currently, within the variety of cements available, clinicians have a number of choices for cement-retained implants. These cements include resin-modified glass ionomer, conventional glass ionomer, zinc oxide and eugenol, zinc phosphate, and polycarboxylate.
Because of the large number of implant manufacturers with various components specific to each implant system, different provisional and definitive restorative options, and various cement materials, no conclusive recommendations for a standardized cement technique or material exist. Tarcia et al18 surveyed US dental schools on cementation protocols for implant crowns, and this survey provides an important insight into what is currently being taught and recommended by 62 dental schools and postgraduate prosthodontics programs in the United States. For cementation techniques, the most widely used procedure before definitive cementation was air-abrasion to microscopically roughen the intaglio surface of the crown. It was also found that resin-modified glass-ionomer cement was the most frequently used luting agent for cementing implant restorations. Cements used by the dental schools surveyed, in order of popularity, included resin-modified glass-ionomer cement, zinc-oxide and eugenol cement (ZOE), conventional glass-ionomer cement, composite-resin cement, zinc-phosphate cement, and polycarboxylate cement.
This survey also investigated the protocols for screw-retained implant restorations in terms of how the screw access openings of screw-retained implant restorations are being managed. The retentiveness of the screw-retained restoration has been reported to be affected by the material used to close the screw access opening.22,32 The access of the screw-retained implant crown can provide an esthetic challenge. Weininger et al evaluated several techniques for masking the access opening and reported that using a small amount of opaque resin in combination with composite resin and flexible resin materials provided for a significant esthetic improvement in the implant restoration.33 Other materials that are used to fill in access holes include cotton pellets, rubber-based material, gutta-percha, and an elastic resin.
Clinical Implications of Dental Cements Used for Cement-Retained Implants
Limited studies are available on the retention of implant crowns to metal or ceramic abutments.18 Definitive cements may provide two to four times the amount of retention than provisional cements.24 Certain implant studies have found resin and glass-ionomer-based cements to be the most retentive,25,26,34,35 while others have found zinc phosphate more retentive.27,35 Sheets et al,36 Akca et al,37 and Mansour et al38 all found that polycarboxylate cements have higher retentive strengths than glass ionomer, zinc phosphate, or provisional cements, but caution that retrievability is an issue.
Some practitioners place cement-retained, implant-supported restorations with a provisional cement so that the restoration can be retrieved at a later time. In the case of a cement-retained, implant-supported FPD, the use of a provisional ZOE or acrylic urethane cement allows for the restoration to be more easily removed on a regular basis or if one or more of the abutments of a FPD come loose. A number of studies have investigated the properties of provisional cements used to cement implant-supported restorations. The retrievability of cemented implant-supported FPDs using different provisional cements has been evaluated.37,39-41 These studies found that provisional cements allow for retrievability of an implant restoration but that there were differences with the cements in their retentive ability. When comparing provisional cements to final cements, it was found that the more rigid the cement, the greater the difficulty in retrieving the implant restoration from the abutment.37,42 Provisional cements make the removal and retrievability of implant-supported restorations more predictable. It is important that the clinician's judgment to use a certain type of cement as a luting agent for a cement-retained implant restoration be based on the clinical circumstances and the implant system being used.38
In the esthetic zone, cemented restorations or implants offer a better solution for retention versus screw-retained restorations for the various reasons mentioned earlier in this article. When incorporating a provisional restoration into the initial surgical visit, great care must be taken to ensure that all excess cement is removed. A bone grafting procedure is often required after placement of an implant-supported restoration because cement leakage in the sulcular area can lead to crestal bone loss, graft failure, and soft tissue recession.
The remainder of this article will demonstrate an immediate extraction/implant placement/provisionalization procedure in the esthetic zone, and describe the cementation procedures used by the authors at the time of surgical placement of the implant fixture.
Conclusion
The cementation process in restorative dentistry, whether a provisional or final restoration, is a key step in tooth enhancement or replacement procedures. Choosing a cement can depend on various issues; however, clinician preference usually plays a significant role in cement selection as well as the actual cementation clinical techniques followed. Great care must be taken to remove any excess cement material either in the natural tooth biologic-width area, or the peri-implant sulcular area, to ensure periodontal health to the gingival tissue surrounding the restoration itself. The authors recommend a thorough understanding of the cement material being used in order to properly use the cement to the best of its design characteristics.
References
1. Branemark PI, Hansson BO, Adell R, et al. Osseointegrated implants in the treatment of the edentulous jaw. Experience from a 10-year period. Scand J Plast Reconstruc Surg. 1977;11:1-32.
2. Albrektsson T, Dahl E, Enborm L, Engevall S, et al. Osseointegrated oral implants. A Swedish multicenter study of 8139 consecutively inserted Nobelpharma implants. J Periodontol. 1988; 59:287-296.
3. De Rouck T, Collys K, Cosyn J. Single-tooth replacement in the anterior maxilla by means of immediate implantation and provisionalization: A review. Int J Oral Maxillofac Implants. 2008;23:897-904.
4. Petrungaro PS. An update on implant placement and provisionalization in extraction, edentulous and sinus grafted sites: A clinical report on 3200 sites over 8 years. Compend Contin Educ Dent. 2008;29(5):288-300.
5. Petrungaro PS. Immediate restoration of implants utilizing a flapless approach to preserve interdental tissue contours. Pract Proced Aesthet Dent. 2005;17(2):A-H.
6. Petrungaro PS. Creation and preservation of natural soft tissue emergence profiles around dental implants in the esthetic zone. J Cosmetic Dent. 2009;24(4):66-80.
7. Hebel KS, Gajjar RC. Cement-retained versus screw-retained implant restorations: achieving optimal occlusion and esthetics in implant dentistry. J Prosthet Dent. 1997;77:28-35.
8. Chee W, Felton DA, Johnson PF, Sullivan DY. Cemented versus screw-retained implant prostheses: Which is better? Int J Oral Maxillofac Implants. 1999;14:137-141.
9. Karl M, Rosch S, Graef F, et al. Static implant loading caused by as-cast metal and ceramic-veneered superstructures. J Prosthet Dent. 2005;93:324-330.
10. Heckmann SM, Karl M, Wichmann MG, et al. Cement fixation and screw retention: parameters of passive fit. An in vitro study of three-unit implant supported fixed partial dentures. Clin Oral Implants Res. 2004;15:466-473.
11. Weber HP, Kim DM, Ng MW, et al. Peri-implant soft-tissue health surrounding cement-and screw-retained implant restorations: a multi-center, 3-year prospective study. Clin Oral Implants Res. 2006;17:375-379.
12. Pauletto N, Lahiffe BJ, Walton JN. Complications associated with excess cement around crowns on osseointegrated implants: a clinical report. Int J Oral Maxillofac Implants. 1999; 14:865-868.
13. Gapski R, Neugeboren N, Pomeranz AZ, Reissner MW. Endosseous implant failure influenced by crown cementation: a clinical case report. Int J Oral Maxillofac Implants. 2008;23:943-946.
14. Thomas GW. The positive relationship between excess cement and peri-implant disease: a prospective clinical endoscopic study. J Periodontol. 2009;80:1388-1392.
15. Dumbrigue HB, Abanomi AA, Cheng LL. Techniques to minimize excess luting agent in cement-retained implant restorations. J Prosthet Dent. 2002;87:112-114.
16. Schwedhelm ER, Lepe X, Aw TC. A crown venting technique for the cementation of implant-supported crowns. J Prosthet Dent. 2003;89:89-90.
17. Wadhwani CP, Piñeyro A. Technique for controlling the cement for an implant crown. J Prosthet Dent. 2009;102:57-58.
18. Taric DY, Alvarado VM, Truong ST. Survey of United States dental schools on cementation protocols for implant crown restorations. J Prosthet Dent. 2010;103:68-79.
19. Singer A, Serfary V. Cement-retained implant-supported fixed partial dentures: a 6-month to 3-year follow-up. Int J Oral Maxillofac Implants. 1996;11:645-649.
20. Ongthiemsak C, Mekayarajjananonth T, Winkler S, Boberick KG. The effect of compressive cyclic loading on retention of a temporary cement used with implants. J Oral Implantol. 2005;31:115-120.
21. Wolfart M, Wolfart S, Kern M. Retention forces and seating discrepancies of implant-retained castings after cementation. Int J Oral Maxillofac Implants. 2006;21:519-525.
22. Emms M, Tredwin CJ, Setchell DJ, Moles DR. The effects of abutment wall height, platform size, and screw access channel filling method on resistance to dislodgement of cement-retained, implant-supported restorations. J Prosthodont. 2007;16:3-9.
23. Kim Y, Yamashita J, Shotwell JL, et al. The comparison of provisional luting agents and abutment surface roughness on the retention of provisional implant-supported crowns. J Prosthet Dent. 2006;95:450-455.
24. Covey DA, Kent DK, St. Germain HA, Koka S. Effects of abutment size and luting cement type on the uniaxial retention force of implant-supported crowns. J Prosthet Dent. 2000;83:344-348.
25. Bernal G, Okamura M, Muñoz CA. The effects of abutment taper, length and cement type on resistance to dislodgement of cement-retained, implant-supported restorations. J Prosthodont. 2003;12:111-115.
26. Schneider RL. Evaluation of the retention of castings to endosseous dental implants. J Prosthet Dent. 1987;58:73-78.
27. GaRey DJ, Tjan AH, James RA, Caputo AA. Effects of thermocycling, load-cycling, and blood contamination on cemented implant abutments. J Prosthet Dent. 1994;71:124-132.
28. Squier RS, Agar JR, Duncan JP, Taylor TD. Retentiveness of dental cements used with metallic implant components. Int J Oral Maxillofac Implants. 2001;16:793-798.
29. Powers JM, Sakaguchi RL. Cements. In: Craig's Restorative Dental Materials. 12th ed, 2006;480-511.
30. Rosenstiel SF, Land MF, Crispin BJ. Dental luting agents: a review of the current literature. J Prosthet Dent. 1998;80:280-301.
31. McComb D. Adhesive luting cements—classes, criteria, and usage. Compend Contin Dent Educ. 1996;17:759-774.
32. Koka S, Ewoldson NO, Dana LC, Beatty MW. The effect of cementing agent and technique on the retention of a CeraOne gold cylinder: a pilot study. Implant Dent. 1995;4:32-35.
33. Weininger B, McGlumphy E, Beck M. Esthetic evaluation of materials used to fill access holes of screw-retained implant crowns. J Oral Implantol. 2008;34:145-149.
34. Pan YH, Ramp LC, Lin CK, Liu PR. Comparison of luting protocols and their effect on the retention and marginal leakage of a cement-retained dental implant restoration. Int J Oral Maxillofac Implants. 2006;21:587-592.
35. Clayton GH, Driscoll CF, Hondrum SO. The effect of luting agents on the retention of marginal adaptation of the CeraOne implant system. Int J Oral Maxillofac Implants. 1997;12:660-665.
36. Sheets JL, Wilcox C, Wilwerding T. Cement selection for cement-retained crown technique with dental implants. J Prosthodont. 2008;17:92-96.
37. Akça K, Iplikçioglu H, Cehreli MC. Comparison of uniaxial resistance forces of cements used with implant-supported crowns. Int J Oral Maxillofac Implants. 2002;17:536-542.
38. Mansour A, Ercoli C, Graser G, et al. Comparative evaluation of casting retention using the ITI solid abutment with six cements. Clin Oral Implants Res. 2002:343-348.
39. Ramp MH, Dixon DL, Ramp LC, et al. Tensile bond strengths of provisional luting agents used with an implant system. J Prosthet Dent. 1999;81:510-514.
40. Lepe X, Bales DJ, Johnson GH. Retention of provisional crowns fabricated from two materials with the use of four temporary cements. J Prosthet Dent. 1999;81:469-475.
41. Michalakis KX, Pissiotis AL, Hirayama H. Cement failure loads of 4 provisional luting agents used for cementation of implant-supported fixed partial dentures. Int J Oral Maxillofac Implants. 2000;15:545-549.
42. Pan YH, Lin CK. The effect of luting agents on the retention of dental implant supported crowns. Chang Gung Med J. 2005;28:403-410.
Disclosure
This CE lesson was supported by an unrestricted educational grant from Parkell.
About the Authors
Paul S. Petrungaro, DDS, MS
Private Practice
Minneapolis, Minnesota, and Chicago, Illinois
Raymond A. Hellickson, DDS
Private Practice
St. Anthong, Minnesota
Michael D. Smilanich, DDS
Private Practice
River Falls, Wisconsin
Case Study: Immediate Tooth Removal, Implant Placement, and Provisionalization
Paul S. Petrungaro, DDS, MS; Raymond A. Hellickson, DDS; Michael D. Smilanich, DDS
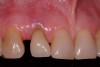
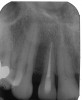
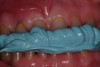
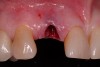
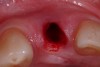
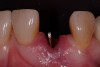
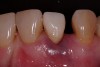
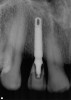
A 54-year-old, non-smoking woman presented with a root fracture at the maxillary right lateral incisor (Figure 1). The patient presented with a 10-mm pocket at the mid-facial probing depth, and a Grade 2 mobility. The preoperative peri-apical digital radiograph can be seen in Figure 2. A natural diastema existed on the distal aspect of the right maxillary incisor, and the patient did not wish to have this corrected. To hold the natural tissue emergence profiles throughout the treatment phase, the immediate implant placement and provisionalization procedure was chosen to treat the affected site. Before the procedure, an occlusal index and registration was taken so that when the retrofitting of the natural tooth shell was accomplished, the exact location of the natural tooth shell could be seated on the implant abutment at the time of implant placement (Figure 3). After administration of an appropriate local anesthetic, tooth No. 7 was removed by an atraumatic technique to preserve the natural soft tissue emergence profiles present pre-surgically (Figure 4). After tooth removal, debridement of the extraction socket was accomplished by curettage of the socket, followed by rotary instrumentation with a course #8 round diamond to ensure removal of all remnants of the periodontal ligament, granulation tissue, and localized debris. To aid in the debridement, the patient was started on a preoperative administration of Augmentin 875 mg, taken the day before treatment, and once again 1 hour before the surgical visit. The patient then continued this antibiotic course for a total of 10 days.
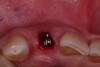
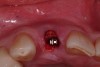
After placement of the surgical guide, the initial site coring was accomplished (Figure 5). The surgical site was widened to 2.8 mm in diameter and 13 mm in length. A Zimmer® (Zimmer Dental) 3-mm x 13-mm one-piece implant was then seated into the previously made osteotomy site (Figure 6). A facial osseous defect existed on the facial of the implant surface, by loss of the facial plate (Figure 7). An allogenic graft, Puros® large-particle cancellous mineralized chips (Zimmer Dental), were placed into the facial defect to obliterate the void on the facial of the implant surface (Figure 8). Once the grafting procedure is accomplished, the provisionalization procedure was started.
The natural tooth root was removed from the extracted right maxillary lateral incisor. The crown portion of the tooth was hollowed out, following the flow of the cemento-enamel junction of the tooth shell. The tooth shell was then acid-etched, and bonding agent was applied to the inside of the shell. A provisional coping, ZocProv 3® (Zimmer Dental) was roughened, and a bonding agent was applied to the outside surface and placed over the abutment portion of the one-piece implant intraorally. The tooth shell was then placed into the bite registration (Figure 9). The shell was filled with regular composite (Figure 10), and placed over the provisional coping, intraorally, and the complex was light-cured (Figure 11).
After the curing process, the complex was removed from the mouth, and inspection of the provisional complex showed the provisional coping registered in the tooth-shell composite complex (Figure 12). The margins were corrected with flowable composite, and the provisional was contoured. The final provisional can be seen in Figure 13. The provisional was filled with provisional cement (Figure 14) and placed over the abutment. After the cement set, and cement expressed into the sulcular space was removed, an explorer was used to remove the excess cement from the sulcular space. A peri-apical x-ray was taken to evaluate the peri-implant space.
The restoration was evaluated for occlusal contact. In any clinical case, if any occlusion exists on the implant restoration, it must be removed so that a non-functional restoration exists. This allows for the implant complex to mature free of occlusion for the 3-month healing phase. The immediate postoperative clinical view of this case, centric occlusion, can be seen in Figure 15, while the complete postoperative facial view is seen in Figure 16. Note how the contoured line angles and facial emergence profile of the retrofitted natural tooth allows for passive pressure on the natural tissue emergence profiles preserved throughout the surgical process. The immediate postoperative digital peri-apical radiograph can be seen in Figure 17. The implant was allowed to integrate for 3 months, at which time the soft tissue contours will have had the same time frame to mature. The provisional restoration will then be removed, and routine implant prosthetic procedures will be initiated.
About the Authors
Paul S. Petrungaro, DDS, MS
Private Practice
Minneapolis, Minnesota, and Chicago, Illinois
Raymond A. Hellickson, DDS
Private Practice
St. Anthong, Minnesota
Michael D. Smilanich, DDS
Private Practice,
River Falls, Wisconsin