You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
In the 1960s, in a lecture cycle of the US Navy postgraduate dental course, Philip Boyne suggested bone grafting of maxillary sinus in order to increase the interarch distance, which is complicated in long-standing edentulous cases due to the atrophic sinus pneumatization. He recommended the lateral window (LW) approach: Caldwell-Luc technique, elevation of Schneiderian membrane, and use of particulate autogenous bone graft.1 Tatum in 1986 and Boyne in 1995 introduced these cases. With more research and experience, their techniques remain pertinent today.2,3
The osteotome technique, which is less invasive for sinus floor elevation, was introduced by Robert Summers at the 1993 meeting of Academy of Osseointegration, followed by the publication of four articles describing its applications.4-7 Throughout the years, many clinicians have modified this procedure.
Various treatments for implant placement in the compromised posterior maxilla are available (Table 1).8 Among these are the placement of shorter implants, placement of tilted implants mesially or distally to the sinus cavity, elongated zygomatic implants in the lateral part of the zygomatic bone, and sinus floor elevation with a one-stage technique using a transalveolar approach (osteotome method), two-stage approach using osteotomes, a one-stage technique using a LW approach, or a two-stage technique with a LW approach, followed by implant placement after a healing period.
Anatomy of Maxillary Sinus
The maxillary sinus is the largest paranasal sinus. It is pyramidal, with the base lying vertically on the medial surface of the lateral nasal wall. The sinus floor is 5 mm to 12.5 mm below the floor of the nose. The dimensions are 15 cc to 20 cc for volume, 32 mm to 34 mm for length, 28 mm to 37 mm for height, and 23 mm to 25 mm for width. The maxillary sinus is surrounded by six bony walls,9 and its enlargement is termed sinus pneumatization. The sinus floor expands with age and is often in close relationship with the apices of the maxillary molars and premolars. With tooth loss, the antrum further expands and the sinus may join the crest of the residual alveolar ridge.10
The septa may divide the sinus. A variable number of septa, referred to as Underwood’s septa, has been reported with a prevalence of 32% in the atrophic/edentulous maxillary segment and 23% in the non-atrophic/dentate maxillary segment with a mean height of 7.9 mm. Commonly, the septum is between second premolar and first molar.11,12
Osteotome Technique
The osteotome technique can help clinicians avoid employing an extensive surgical procedure (atraumatic vs LW or drilling), and this approach can be performed simultaneously with implant placement. The disadvantages are the uncertainty of possible perforation of the sinus membrane, ridge fracture (extremely narrow ridge), and patient discomfort (tapping). This approach is indicated for a flat sinus floor, when residual bone height is at least 5 mm, and when crestal bone width is adequate for implant installation. The osteotome technique is contraindicated in patients with a history of inner ear complications and vertigo and for an oblique sinus floor (> 45° inclination). There is no drilling, and approximately 3 mm to 5 mm of additional bone height can be achieved. The osteotome is pushed apically, laterally displacing the buccal and palatal bones, while the concave tip with a sharpened end of the osteotome pushes bone apically. The instrument is tapered to allow successive osteotome placement.8
Summers describes the ridge expansion osteotomy technique. Each subsequent osteotome fits into the site prepared by the previous osteotome until lateral ridge expansion is achieved. A minimum ridge width of 3 mm is required for the osteotome technique. The technique allows more implants to be placed in a narrower ridge in anterior and posterior sites. The approach is less invasive and has fewer risks compared to split crest and bone spreading.9,11 Summers describes the less invasive methods of elevating sinus floor in which bone is added to the original osteotome sinus floor elevation (OSFE).10 The osteotomy is prepared to within 1 mm to 2 mm of the sinus floor, then widened with the Nos. 2 and 3 osteotomes. Bone is placed into the osteotomy, and the osteotome is advanced with light malleting (no more than 2 mm). More bone is added, and the procedure is repeated at least three times. When the sinus floor is displaced and the graft is freely moving, the implant is tapped into place and acts as the final osteotomy.10 The future site development technique is used when less than 6 mm of bone is between the crest and floor and for augmentation in wider sites. The osteotomes never enter the sinus. A trephine may be used to create a cut in the bone, short of the sinus floor. The tapping of the “bone plug” inward follows. After the bone plug is slightly moveable, the site is “backfilled” with bone graft material and lightly malleted.11
Bone Graft—Is It Necessary?
In an animal study by Boyne,13 implants protruding into the maxillary sinus following elevation of the sinus membrane without grafting material exhibited spontaneous bone formation over more than half of the implant’s height. The implant design and extent of protrusion influenced the amount of bone formation. Implants with open apices or deep threads had small amounts of new bone growth. Those with rounded apices showed spontaneous bone formation extending around the implants if they only penetrated 2 mm to 3 mm into the maxillary sinus. However, when the same implants penetrated 5 mm into the maxillary sinus, only a partial (50%) growth of new bone was seen toward the implant apex. This is still pertinent today with different implant surfaces and designs available that will continue to evolve.
What Type of Graft?
Researchers of a multicenter retrospective study with 174 implants in 101 patients examined the influence of the grafting material used and found that the type of the grafting material did not affect implant survival. When residual bone height was > 5 mm, the survival rate was 96%. However, when residual bone height was 4 mm or less, the rate decreased to 85.7%.14 Using the osteotome technique, Brägger and coworkers15 investigated the patterns of tissue remodeling after the placement of 25 implants in 19 patients. Composite xenografts and autografts were employed. They concluded that the grafted area apical to the implants underwent shrinkage and remodeling and the original outline of the sinus was eventually consolidated and replaced by a new cortical plate. In another study by Leblebicioglu et al,16 implants were installed into the sinuses of 40 patients using an osteotome technique with no graft or cushion materials; a mean gain of alveolar bone height in scanned panoramic radiographs of 3.9 mm +/-1.9 mm was found. Pjetursson et al17 and Tan et al18 found that when no grafting material was used, some dense structure was often visible apical to the implant, immediately after implant placement. However, after at least 1 year of remodeling, this structure may no longer be detectable and only a moderate amount of bone gain mesially and distally may persist. The researchers also determined that when grafting material is used, a cloudy dome-shaped structure with a hazy demarcation may be visible after implant placement. This size is usually reduced after remodeling but still provides a definite increase in bone volume compared to the preoperative situation.
Complications
Perforation of the Schneiderian membrane is the most common complication of sinus elevation. However, a perforation is not a contraindication to the augmentation. The best treatment is avoidance of a perforation, but perforations do occur and must be corrected.19 Rosen et al14 found that a minimum preoperative ridge height of 5 mm is necessary to achieve adequate elevation of sinus without undue risk of perforation (OSFE with bone). After examining 588 patients, Ferrigno et al20 observed three perforations of the sinus membrane (perforation rate of 2.2%). Tan et al18 concluded that this was the most frequently reported complication, occurring in 3.8% of the procedures.
Success and Implant Survival
Several authors have examined the success and implant survival after insertion using the OSFE technique. They do not compare survival/success rates of implants placed in sites requiring the osteotome technique versus not requiring the site preparation. Ferrigno et al studied the survival and success rates of 588 implants placed in 323 consecutive patients, with a residual bone height from 6 mm to 9 mm.20 After a mean observation period of 5 years, they found rates of 94.8% and 90.8%, respectively. They concluded that the installation of short implants in conjunction with OSFE is predictable and may reduce the indications for more invasive and complex procedures, such as the sinus floor elevation by the lateral approach. The systematic review by Tan et al18 yielded 19 studies on implants placed in transalveolar sinus floor augmented sites. The inclusion criteria for each study included a mean follow-up of at least 1 year of functional loading and a minimum of 10 patients. Of the 4388 implants placed, 103 were lost, of which 55 implants were lost before loading and 28 implants were lost after at least 1 year of function. This resulted in a survival rate of 92.8% after 3 years of function. If residual bone height was less than 8 mm, the survival rate decreased to 91.8%. The postoperative complications outlined in this review were graft infection (most common with a mean of 0.8%) hemorrhage, nasal bleeding, blocked nose, hematomas, and loosening of cover screws resulting in suppuration.
Sinus Floor Evaluation with Lateral Approach
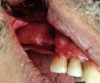
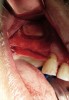
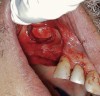
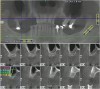
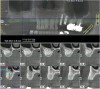
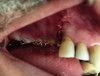
The lateral approach is also used for sinus floor elevation. It is indicated when there is reduced residual bone height, which does not allow standard implant placement or placement of implants in combination with minor sinus floor elevation using the osteotome technique (Figure 1, Figure 2 and Figure 3). Contraindications are excessive interarch distance due to unfavorable crown-to-root ratio, acute or chronic unresolved sinusitis, current sinus pathology (eg, cysts or tumors), lodged root tips in the sinus, history of heavy smoking, a systemic compromise, and psychological problems.
Premedication
The use of many drug combinations has been reported. Among these are amoxicillin 1 g or in the case of allergies, clindamycin 300 mg, both used 1 hour before surgery. If there is a history of chronic or periodic sinus infections, the use of Augmentin® (GlaxoSmithKline, www.gsk.com) 3 days before surgery and up to 7 to 10 days after surgery is recommended. Glucocorticoids (dexamethasone 8 mg) can be prescribed 1 hour beforehand.
One Stage or Two Stage?
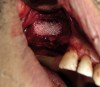
The decision to use the one- or the two-stage technique is mainly based on the amount of residual bone available and the possibility of achieving primary stability for the inserted implants: one-stage sinus floor elevation with simultaneous implant placement and two-stage sinus elevation (delayed installation of the implant). The grafted site matures in approximately 6 to 10 months, according to Wallace et al21 (Figure 4 and Figure 5).
Fugazzotto and Vlassis22 reported a 97.7% success rate of sinus augmentations when they used the LW, LW with simultaneous implant placement, and the crestal approach. They reported a 97% success rate of implants placed in those sites. Also, the survival rate of implants in LW cases was increased when the crestal ridge height was > 3 mm. Jensen et al23 found no significant difference in failure rate when they compared sinus augmentation and simultaneous implant placement verses the two-stage delayed method.
What Kind of Graft?
The type of graft material and its effect on the success of the implants has been examined by many authors. In early studies, the autogenous bone graft was considered the gold standard.5,6 Froum et a24 found that when as little as 20% of autogenous bone was added to the bone substitutes, xenografts alone or in combination with autogenous bone and/or demineralized freeze-dried bone allografts (DFDBA) had statistically significant increases in vital bone formation The mean vital bone formation was 27.1% after healing for 6 to 9 months. Many authors have reported higher survival rates for implants placed into sinuses grafted with 100% xenograft as compared to those placed in sinuses grafted with 100% autogenous bone or composite graft xenograft and autogenous bone.25-27 Every bone grafting material has been used for sinus augmentation: DFDBA particulate,28 anorganic bovine bone particulate,24 nonresorbable hydroxyapatite,29 autogenous block grafts,30 rhBMP-2 collagen sponge,31 and tricalcium phosphate6 (Figure 6).
With or Without a Membrane?
The graft can remain exposed, be covered with a barrier membrane, or be covered with the preserved bone window. Tarnow et al32 performed a split-mouth design study with bilateral sinus grafts for 12 patients with or without covering the LW with a membrane. After 12 months, histologic samples were taken through the LW. The mean percentage of vital bone formation was 25.5% with and 19.9% without covering the barrier. Froum et al24 examined 113 sinuses grafted with either xenograft alone or a composite of xenograft and autograft. The mean vital bone formation was 27.6% with a membrane and 16% without a membrane. Avera et al33 and Wallace et al21 found that the use of resorbable and nonresorbable barrier membranes over LW and graft material aided in graft containment, prevented soft-tissue encleftation, and improved success rates. However, using a 100% autogenous bone versus autogenous bone as a component of a composite bone graft did not affect implant survival.
Is Smoking a Contraindication?
Mayfield et al34 found an implant survival rate of 100% for nonsmokers compared to 43% for smokers after 4 years to 6.5 years of loading for implants placed in combination with bone augmentations (horizontal, vertical, and sinus elevations). Similar reduced survival rates have been corroborated by several other authors.23,35
Peleg et al36 examined 2,132 implants after sinus floor elevation with simultaneous implant placement and found conflicting results. Of the 226 patients, floor elevations (627 implants) were performed for smokers and 505 sinus floor elevations (1,505 implants) for nonsmokers. The survival rate of the implants with up to 9 years’ follow-up was 97.9%, with no statistically significant differences between smokers and nonsmokers.
Postsurgical
Drugs that are often prescribed are amoxicillin 500 mg tid or clindamycin 300 mg tid for 10 days, glucocorticoids (dexamethasone 4 mg for 2 days), ibuprofen 600 mg every 4 to 6 hours for pain if needed, and 0.12% chlorhexidine twice daily for 10 days (Figure 7).
Common complications are perforation of the sinus membrane, excessive bleeding from the bony window or the sinus membrane, injury of the infraorbital neurovascular bundle, implant migration, hematoma, adjacent tooth sensitivity, infection of the grafted sinuses, sinusitis, and sinus perforation.
Vlassis and Fugazzotto in 1999 described the following sinus perforation classification. Class I: Perforation is adjacent to the osteomy site. This type of perforation will usually self repair when the membrane folds on itself following completion of elevation. Treatment should be considered when the perforation is still evident after membrane reflection. Class II: Perforation is in the mid-superior aspect of the osteotomy, extending mesiodistally for two thirds of the dimension of total osteotomy site. It usually occurs with the infracture design of the osteotomy. Repair and treatment are similar to Class I. Class III: Located at the inferior border of the osteotomy at its mesial or distal extent, a Class III perforation is the most common and usually caused by inadequacy of the osteotomy or improper execution of membrane reflection. Treatment is needed to repair the perforation, using a lamellar bone sheet to cover it. Class IV: A Class IV perforation is in the central two thirds of the inferior border of the osteotomy site. It is almost always caused by lack of care when preparing the osteotomy site and results in the perforation with the rotary instrument. Repair is similar to a Class III. Class V: A Class V perforation is a preexisting area of exposure of the sinus membrane caused by a combination of extensive pneumatization and severe ridge resorption. This is obvious only after flap reflection.37
The infection of the grafted sinuses is rare, and the risk increases when a membrane is perforated. Sinus grafting and simultaneous implant placement should be avoided in situations of membrane perforation.23
Sinusitis
Timmenga et al38 evaluated the function of the maxillary sinus after LW sinus floor elevation. Out of 45 patients who had received 85 sinus grafts and underwent endoscopic examination, 5 patients received a diagnosis of sinusitis. The incidence of sinusitis was low and mainly found in patients with an anatomic or functional disorder prior to the sinus grafting. Tidwell et al39 reported preoperative sinusitis was predictive of postoperative acute sinusitis.
Success of the LW Technique
In the consensus Conference of the Academy of Osseointegration, retrospective data were collected from 38 clinicians. There were 1,007 sinus elevations were performed with 2,997 implants placed within 10 years. Most implants were followed for 3 years or more. There were 229 implants lost, resulting in an overall average survival rate of 90%. However, data amongst clinicians were variable depending on the implant type, length, grafting material, and timing of placement.23 Wallace and Froum40 published a systematic review for the effect of maxillary sinus augmentation on the survival of endosseous dental implants. The survival rate of implants placed using sinus lift with a lateral approach was 61.7% to 100% with an average of 91.8%. Rough-surfaced implants had better survival rates than machined-surface implants placed in grafted sinuses. In a systematic review by Pjetursson et al17 of the success of sinus floor elevation and survival of implants inserted in combination with sinus floor elevation, 48 studies were evaluated. Of these, 26 were prospective and 22 were retrospective and included approximately 4,000 patients between 15 and 86 years of age. The follow-up had to be at least 1 year after functional loading. The mean residual bone height at the site of implant placement was as much as 6 mm. The implants were placed simultaneously (one-stage) and delayed (two-stage) installation at 3 to 12 months after sinus grafting. The implant-based analysis showed that annual implant failure rate was 3.5%, resulting in a 3-year implant survival rate of 90.1%. The annual failure rate of machined-surface implants (6.9%) was significantly higher than that for rough-surface implants (1.2%). Perforation of the sinus membrane, the most frequently reported complication of the LW technique, occurred in 19.5% of the procedures. The mean incidence of postoperative graft infection was 2.9%. Graft loss resulting in the inability for implant placement was reported in 1.9% of cases.
Shorter Implants
Recent clinical studies41-43 on short implants (< or = 9 mm) with rough surfaces designed for high initial stability show survival rates of approximately 95%, which correlate with the survival rate reported for implants after 5 years in a systematic review by Berglundh et al.44 However, there is no difference in survival rate of implants placed in maxilla versus mandible. Splinting and cross-arch stabilization are appropriate treatments. There is a 99% implant survival with 7-mm and 9-mm implants in posterior regions with splinting, as well with other biomechanical methods to decrease stress in implant-to-bone interface. For shorter implants, immediate loading in the maxilla can be successful with cross-arch stabilization.45-48
Recent Reviews
More recent reviews have since been published commenting on the LW sinus lift procedure. Nkenke and Stelzle49 found no clear reasons for a clinician to choose between autogenous bone and a bone substitute; their findings agree with those of Wallace and Froum in 2003.40 Some believe that with an alveolar bone height of 3 mm to 6 mm, there would be fewer complications to sinus lift to 8 mm as opposed to performing a LW to 10 mm. Also, platelet-rich plasma does not improve the clinical outcome of the autogenous or bone substitute grafts.50,51
Conclusion
The choice of a method (ie, short implants, osteotome technique, or lateral approach) should be based on the observed residual bone height of the alveolar crest and clinician’s preference. Selecting less-invasive therapy (eg, the use of shorter implants) has been the trend; however, sinus elevation is the most predictable for vertical augmentation. With sinus elevation, there is no clinical difference with the type of graft material; however, the use of a membrane is recommended. Smoking is not an absolute contraindication to performing the sinus lift procedure. Based on the alveolar bone height of approximately 7 mm, the guideline for sinus elevation is < 7 mm for the LW and >7 mm for the osteotome technique.
References
1. Boyne PJ, James RA. Grafting of the maxillary sinus floor with autogenous marrow and bone. J Oral Surg. 1980;38:613-616.
2. Tatum J Jr. Maxillary and sinus implant reconstructions. Dent Clin North Am. 1986;30:207-229.
3. Boyne PJ. Use of HTR in tooth extraction sockets to maintain alveolar ridge height and increase concentration of alveolar bone matrix. Gen Dent. 1995;43(5):470-473.
4. Summers RB. A new concept in maxillary implant surgery: the osteotome technique. Compend Contin Educ Dent. 1994;15(2):152-162.
5. Summers RB. The osteotome technique: Part 2—the ridge expansion osteotomy (REO) procedure. Compend Contin Educ Dent. 1994;15(4):422-436.
6. Summers RB. The osteotome technique: Part 3—less invasive methods of elevating the sinus floor. Compend Contin Educ Dent. 1994;15(6):698-710.
7. Summers RB. The osteotome technique: Part 4—future site development. Compend Contin Educ Dent. 1995;16(11):1090-1099.
8. Misch CE. Maxillary sinus augmentation for endosteal implants: organized alternative treatment plans. Int J Oral Implantol. 1987;4(2):49-58.
9. Moss-Salentijn L. Anatomy and Embryology. In: Blitzer A, Lawson W, Friedman W, eds. Surgery of the Paranasal Sinuses. Philadelphia, PA: WB Saunders; 1985.
10. Navarro JAC. The Nasal Cavity and Paranasal Sinuses: Surgical Anatomy. Berlin, Germany: Springer; 2001.
11. Ulm CW, Solar P, Krennmair G, et al. Incidence and suggested surgical management of septa in sinus-lift procedures. Int J Oral Maxillofac Implants. 1995;10(4):462-465.
12. Kim MJ, Jung UW, Kim CS, et al. Maxillary sinus septa: prevalence, height, location, and morphology. A reformatted computed tomography scan analysis. J Periodontol. 2006;77(5):903-908.
13. Boyne PJ. Analysis of performance of root-form endosseous implants placed in the maxillary sinus. J Long Term Eff Med Implants. 1993;3(2):143-159.
14. Rosen PS, Summers R, Mellado JR, et al. The bone-added osteotome sinus floor elevation technique: multicenter retrospective report of consecutively treated patientsInt J Oral Maxillofac Implants. 1999;14 (6):853-858.
15. Brägger U, Gerber C, Joss A, et al. Patterns of tissue remodeling after placement of ITI dental implants using an osteotome technique: a longitudinal radiographic case cohort study. Clin Oral Implants Res. 2004;15(2):158-166.
16. Leblebicioglu B, Ersanli S, Karabuda C, et al. Radiographic evaluation of dental implants placed using an osteotome technique. J Periodontol. 2005;76(3):385-390.
17. Pjetursson BE, Tan WC, Zwahlen M, et al. A systematic review of the success of sinus floor elevation and survival of implants inserted in combination with sinus floor elevation. J Clin Periodontol. 2008;35(8 suppl):216-240.
18. Tan WC, Lang NP, Zwahlen M, et al. A systematic review of the success of sinus floor elevation and survival of implants inserted in combination with sinus floor elevation. Part II: transalveolar technique. J Clin Periodontol. 2008;35(8 suppl):241-254.
19. Fugazzotto PA, Vlassis J. A simplified classification and repair system for sinus membrane perforations. J Periodontol. 2003;74(10):1534-1541.
20. Ferrigno N, Laureti M, Fanali S. Dental implants placement in conjunction with osteotome sinus floor elevation: a 12-year life-table analysis from a prospective study on 588 ITI implants. Clin Oral Implants Res. 2006;17(2):194-205.
21. Wallace SS, Froum SJ, Cho SC, et al. Sinus augmentation utilizing anorganic bovine bone (Bio-Oss) with absorbable and nonabsorbable membranes placed over the lateral window: histomorphometric and clinical analyses. Int J Periodontics Restorative Dent. 2005;25(6):551-559.
22. Fugazzotto PA, Vlassis J. Long-term success of sinus augmentation using various surgical approaches and grafting materials. Int J Oral Maxillofac Implants. 1998;13(1):52-58.
23. Jensen OT, Shulman LB, Block MS, et al. Report of the Sinus Consensus Conference of 1996. Int J Oral Maxillofac Implants. 1998;13(suppl):11-45.
24. Froum SJ, Tarnow DP, Wallace SS, et al. Sinus floor elevation using anorganic bovine bone matrix (OsteoGraf/N) with and without autogenous bone: a clinical, histologic, radiographic, and histomorphometric analysis—part 2 of an ongoing prospective study. Int J Periodontics Restorative Dent. 1998;18(6):528-543.
25. Hallman M, Sennerby L, Lundgren S. A clinical and histologic evaluation of implant integration in the posterior maxilla after sinus floor augmentation with autogenous bone, bovine hydroxyapatite, or a 20:80 mixture. Int J Oral Maxillofac Implant. 2002;17(5):635-643.
26. Hallman M, Hedin M, Sennerby L, et al. A prospective 1-year clinical and radiographic study of implants placed after maxillary sinus floor augmentation with bovine hydroxyapatite and autogenous bone. J Oral Maxillofac Surg. 2002;60(3):277-284; discussion 285-286.
27. Valentini P, Abensur DJ. Maxillary sinus grafting with anorganic bovine bone: a clinical report of long-term results. Int J Oral Maxillofac Implants. 2003;18(4):556-560.
28. Chanavaz M. Sinus grafting related to implantology. Statistical analysis of 15 years of surgical experience (1979-1994). J Oral Implanto. 1996;22(2):119-130.
29. Small SA, Zinner ID, Panno FV, et al. Augmenting the maxillary sinus for implants: report of 27 patients. Int J Oral Maxillofac Implants. 1993;8(5):523-528.
30. Wannfors K, Johansson B, Hallman M, et al. A prospective randomized study of 1- and 2-stage sinus inlay bone grafts: 1-year follow-up. Int J Oral Maxillofac Implants. 2000;15(5):625-632.
31. Boyne PJ, Marx RE, Nevins M, et al. A feasibility study evaluating rhBMP-2/absorbable collagen sponge for maxillary sinus floor augmentation. Int J Periodontics Restorative Dent. 1997;17(1):11-25.
32. Tarnow DP, Wallace SS, Froum SJ, et al. Histologic and clinical comparison of bilateral sinus floor elevations with and without barrier membrane placement in 12 patients: part 3 of an ongoing prospective study. Int J Periodontics Restorative Dent. 2000;20(2):117-125.
33. Avera SP, Stampley WA, McAllister BS. Histologic and clinical observations of resorbable and nonresorbable barrier membranes used in maxillary sinus graft containment. Int J Oral Maxillofac Implants. 1997;12(1):88-94.
34. Mayfield LJ, Skoglund A, Hising P, et al. Evaluation following functional loading of titanium fixtures placed in ridges augmented by deproteinized bone mineral. A human case study. Clin Oral Implants Res. 2001;12(5):508-514.
35. Bain CA, Moy PK. The association between the failure of dental implants and cigarette smoking. Int J Oral Maxillofac Implants. 1993;8(6):609-615.
36. Peleg M, Garg AK, Mazor Z. Predictability of simultaneous implant placement in the severely atrophic posterior maxilla: a 9-year longitudinal experience study of 2132 implants placed into 731 human sinus grafts. Int J Oral Maxillofac Implants. 2006;21(1):94-102.
37. Vlassis JM, Fugazzotto PA. A classification system for sinus membrane perforations during augmentation procedures with options for repair. J Periodontol. 1999;70(6):692-699.
38. Timmenga NM, Raghoebar GM, Boering G, et al. Maxillary sinus function after sinus lifts for the insertion of dental implants. J Oral Maxillofac Surg. 1997;55(9):936-639.
39. Tidwell JK, Blijdorp PA, Stoelinga PJ, et al. Composite grafting of the maxillary sinus for placement of endosteal implants. A preliminary report of 48 patients. Int J Oral Maxillofac Surg. 1992;21(4):204-209.
40. Wallace SS, Froum SJ. Effect of maxillary sinus augmentation on the survival of endosseous dental implants. A systematic review. Ann Periodontol. 2003;8(1):328-343.
41. Fugazzotto PA, Beagle JR, Ganeles J, et al Success and failure rates of 9 mm or shorter implants in the replacement of missing maxillary molars when restored with individual crowns: preliminary results 0 to 84 months in function. A retrospective study. J Periodontol. 2004;75(2):327-332
42. Renouard F, Nisand D. Short implants in the severely resorbed maxilla: a 2-year retrospective clinical study. Clin Implant Dent Relat Res. 2005;7(suppl 1):S104-S110.
43. Renouard F, Nisand D. Impact of implant length and diameter on survival rates.Clin Oral Implants Res. 2006;17(suppl 2):35-51.
44. Berglundh T, Persson L, Klinge B. A systematic review of the incidence of biological and technical complications in implant dentistry reported in prospective longitudinal studies of at least 5 years. J Clin Periodontol. 2002;29(suppl 3):197-212; discussion 232-233.
45. Koo KT, Wikesjö UM, Park JY, et al. Evaluation of single-tooth implants in the second molar region: a 5-year life-table analysis of a retrospective study. J Periodontol. 2010;81(9):1242-1249.
46. Misch CE, Steignga J, Barboza E, et al. Short dental implants in posterior partial edentulism: a multicenter retrospective 6-year case series study. J Periodontol. 2006;77(8):1340-1347.
47. Misch CE. Short dental implants: a literature review and rationale for use. Dent Today. 2005;24(8):64-66, 68.
48. Romanos GE, Nentwig GH. Immediate functional loading in the maxilla using implants with platform switching: five-year results. Int J Oral Maxillofac Implants. 2009;24(6):1106-1112.
49. Nkenke E, Stelzle F. Clinical outcomes of sinus floor augmentation for implant placement using autogenous bone or bone substitutes: a systematic review. Clin Oral Implants Res. 2009;20(suppl 4):124-133.
50. Esposito M, Grusovin MG, Rees J, et al. Effectiveness of sinus lift procedures for dental implant rehabilitation: a Cochrane systematic review. Eur J Oral Implantol. 2010;3(1):7-26.
51. Esposito M, Grusovin MG, Rees J, et al. Interventions for replacing missing teeth: augmentation procedures of the maxillary sinus. Cochrane Database Syst Rev. 2010 Mar 17;3:CD008397.
About the Authors
Georgios Tasoulis, DMD
Clinical Instructor, Department of Periodontics
Columbia University College of Dental Medicine
New York, New York
Suellan Go Yao, DMD
Clinical Instructor, Department of Periodontics,
Columbia University College of Dental Medicine,
New York, New York
James Burke Fine, DMD
Associate Dean for Postdoctoral Education, Professor of Clinical Dentistry,
and Postdoctoral Director of the Division of Periodontics,
Columbia University College of Dental Medicine,
New York, New York
Attending Dental Surgeon
Presbyterian Hospital Dental Service
New York, New York
Private Practice
Hoboken, New Jersey
Faculty practice at Columbia University
New York, New York