You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
The dental team is a trusted source of information related to the health and appearance of their patients’ teeth. Although there are a wide variety of highly publicized over-the-counter products on the market, patients should be aware that tooth whitening is best performed under the care of a dental professional. Dental practices—especially those that are experienced in offering tooth-whitening services and related products—have the knowledge and experience to advise patients on appropriate options for their individual cases. Therefore, patients should be encouraged to discuss their desire to whiten their teeth with the dental team to make sure their condition is not due to an underlying problem that requires treatment. Variations among products in all cases include the bleaching agents, concentration of bleaching material, and delivery method, and the oral healthcare professional will be the best source of information whether patients elect in-office, at-home prescribed, or over-the-counter choices.
The Importance of the Patient Evaluation
According to the American Dental Association, the most critical factor in the tooth whitening process is proper examination prior to initiating bleaching treatment.1 During routine visits, dental team members may identify patients who are interested in whitening their teeth and conduct an in-office evaluation to determine the cause of discoloration and the whitening treatments—if any—that are appropriate for their individual case. During this clinical evaluation —which should include both a clinical and radiographic component—the dental professional should check for oral tissue injuries, active gingivitis or periodontal disease, tooth sensitivity, and new or faulty restorations—all of which should be considered both for the health of the patient’s dentition and in the choice of a whitening treatment. The clinical examination includes an evaluation for caries, in addition to screening soft and hard tissue for cancer, abscesses, exposed root surfaces, or other conditions. In addition, factors such as sensitivity, temporomandibular joint issues, and endodontic treatment are considered before a whitening procedure is recommended.2
The dental professional should also determine the specific cause(s) of discoloration as that, too, will impact both the recommended treatment and the patient’s expectations for its success. Typical sources of staining are smoking, food, and drinks; tetracycline; and fluorosis.3 Teeth may also be discolored as a result of traumatic injury or even the endodontic therapy used to treat them.4 In the case of a single dark tooth, a radiograph should always be taken, because teeth may undergo pulpal necrosis without showing any other symptoms.5
Patient Selection Factors
After determining the cause of the discoloration and before recommending a specific treatment, practitioners will take into account whether other factors are contraindications for treatment: allergies to materials, tooth sensitivity, willingness to follow treatment, and financial considerations.6,7
It is essential to manage patient expectations for their results and timetable for achieving them. The type of discoloration, patient’s age, and the concentration and duration of use of the chosen agent will impact the outcome. Patients whose teeth are mildly stained due to fluorosis or tetracycline, slightly darkened due to trauma, or who demonstrate yellowing that is not due to systemic or developmental causes are considered to be appropriate candidates for tooth bleaching, although the required length of treatment from one case to another may differ significantly.3
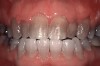
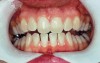
Depending on the level of staining, teeth with yellow, light brown, and orange stains as a result of aging, genetics, food, and drinks (and not developmental or systemic causes) usually respond within 1 to 4 weeks, while those with brown, orange, and white stains from fluorosis or stains caused by nicotine are slower to respond to bleaching—generally requiring 1 to 3 months of treatment.8 Even more resistant to whitening are teeth that tetracycline stained, which may appear dark gray, brown, or blue (Figure 1 and Figure 2). According to Haywood, whitening these teeth at home may take 6 months using 10% carbamide peroxide.8
Therefore, during the consultation, the clinician should discuss all pertinent issues including: whether bleaching is an appropriate option for this condition in this patient; whether other treatments should be performed prior to or in conjunction with the whitening procedure to improve esthetics or minimize side effects; and the method that best meets the patient’s situation, including dentition, finances, and lifestyle.9
The Basics of Bleaching
Bleaching is a non-invasive, conservative treatment and is usually the first option considered—however, it is not the only option, and it is not necessarily the most appropriate treatment, as some people cannot tolerate the agents and not all forms of discoloration are responsive.
As described by McCaslin et al,10 the objective of the whitening process is to allow the oxidizing agent—carbamide peroxide (CP) or hydrogen peroxide (HP)—which is held in close contact to teeth for a specific amount of time, to penetrate into the tooth to enable a chemical reaction to occur and dislodge or decolor the chromatic particles. (Note that 30% CP corresponds to about 10% HP; therefore 20% CP corresponds to 7% HP and 10% CP corresponds to about 3.5% HP.) With CP, that agent penetrates into the tooth, and it is broken down into urea (which extends its shelf life) and HP. The urea in turn breaks down into ammonia and carbon dioxide, while the HP converts to oxygen and water and “frees the chemically reactive free radical perhydroxyl (HO2-) with great oxidative power.” The peroxide both removes discoloration inside the tooth and changes the color of the dentin.10
Treatment Delivery Options
The American Dental Association describes four categories of tooth whitening/bleaching treatment methods: professionally applied (in the dental office); dentist-prescribed/dispensed (patient home-use); consumer-purchased/over-the-counter (OTC) (applied by patients); and other non-dental options such as treatments or kits sold in non-dental retail settings, for example mall kiosks, salons, spas, and cruise ships.1
In all cases, before applying whitening agent, surfaces should be cleaned thoroughly to remove film and debris, and to differentiate extrinsic from intrinsic stains.11
In-office treatment—There is little doubt that the most effective whitening treatments are those delivered by the dental team in the office. With the dentist in complete control, there is no learning curve or need for compliance by the patient, and the practitioner can monitor results—focusing on specific teeth, and terminating or modifying treatment if the patient experiences side effects. According to Haywood, few patients are satisfied with results achieved after one in-office bleaching treatment, and these are generally patients with an initial shade of A2 or lighter on a Vita Classic shade guide.12 Dentists should inform patients at the outset that they will likely need from two to six treatments—the cost of which should be specified—to achieve satisfactory results, and that the wait time for shade stabilization is at least 2 weeks and can be as much as 6 weeks for higher concentrations of material.12 Haywood also reports that the use of light does not improve the final outcome of in-office bleaching, although teeth may temporarily appear whiter as a result of the dehydration the light causes.12
Prescribed at-home treatments—Treatments that are prescribed by the dentist but applied at home by patients using a custom-fitted bleaching tray are less expensive than in-office treatments, but require more time to produce optimal results (Figure 3 and Figure 4). They may involve overnight/an 8-hour time period using 10% CP or a shorter time period using a much stronger agent—25% to 38% CP or 10%HP.6 Evidence supporting home treatment includes a study showing that 5 days of at-home whitening with 10% CP overnight (8 hours) yielded tooth whitening comparable to a 1-hour in-office treatment with 25% hydrogen peroxide. In addition—reflecting a common desire of patients—after in-office treatment, most request continuation of tooth whitening at home.13
Over-the-counter treatments—Among the over-the-counter whitening products found through consumer platforms are systems composed of whitening strips, paint-on brushes, rinses, toothpastes, dental floss, chewing gums, and combinations of these components, some of which include whitening trays. Their bleaching agents may be similar to those offered by dental practices but their efficacy varies greatly and depends on their method of placement and contact with the teeth.6 There is evidence that the whitening strips can be effective for the removal of intrinsic stains and that whitening toothpastes, gum, and floss can aid in the removal of extrinsic stains.14
Short Term Side Effects
All tooth whitening methods involving the use of chemical agents are subject to side effects, which vary in severity from one patient to the next.
Soft-Tissue Effects
Higher-concentration whitening agents can produce a chemical “burn” when they contact soft tissues, causing tissues to turn white and the patient to experience mild discomfort. This discomfort and change in color disappear once the tissues rehydrate. In the office, strategies for protecting tissues include the use of a rubber dam or other protective barrier during treatment.11 In addition, many professionally delivered systems include a light-cured resin in a syringe to confine the agent to the teeth. The clinician may also place flexible spreaders in the mouth to protect cheeks and lips from contact with the whitening agent.11
Hard Tissue—Tooth Sensitivity
The very factors that deliver the fastest and most dramatic results are most likely to lead to the most commonly reported side effect of bleaching: sensitivity. These factors include the highest concentrations of peroxide, the longest amount of agent–tooth contact time, and higher temperatures—such as those caused by bleaching lights—used to increase the speed of the chemical reaction.15
Sensitivity was demonstrated by 25% to 35% of study subjects noted by Da Costa and others.13 It is difficult to predict which patients other than those who have experienced sensitivity in the past will suffer this discomfort after whitening. Therefore, it is essential to inquire before commencing treatment, and patients can be tested for the likelihood of sensitivity with a blast of compressed air.16
To reduce or prevent sensitivity, the clinician should use the strategies mentioned above to confine the agent to the teeth. However, if sensitivity worsens, the patient should discontinue bleaching for 1 to 2 days. Persistent severe sensitivity can be treated with 5% potassium nitrate with fluoride.16
Restorations and Whitening
Before commencing a whitening treatment, the impact of whitening on existing or future restorations should be examined. Patients with restorations may find that as their natural teeth are lightened, their existing restorations will appear darker and may require replacement to match the new tooth shade. However, darker teeth with facial veneers can be lightened somewhat by placing an agent-filled tray on the lingual side of the tooth for several days to a few weeks. In this case, the modification will be viewed through the veneers, therefore improvements may not meet patient expectations.11
According to Attin, any restorative treatment in the esthetic zone should be delayed until bleaching is completed and the color of the teeth has stabilized, as it is not possible to accurately predict the ultimate shade change.17 Haywood reports that it can take 2 to 6 weeks after in-office bleaching to see the actual color change.12 Beyond the esthetic issues that make bleaching prior to restoration preferred are concerns about the effect of bleaching on dentin and enamel bonding. Research suggests that bleaching can have a negative impact on dentin and enamel bonding.17 However, based on Haywood’s writings, it seems prudent to delay placement of bonded restorations until at least 2 weeks after the completion of bleaching for esthetic reasons alone.12
Safety Concerns
Research has not shown development of pre-neoplastic or neoplastic oral lesions due to whitening.18,19 However, the ADA position paper expresses a number of concerns related to “non-dental whitening venues,” including “the long-term safety of unsupervised bleaching procedures, due to abuse and possible undiagnosed or underlying oral health problems,” and cautions that the rate of adverse events from use or abuse of home-use OTC products is likely under-reported to the U.S. Food and Drug Administration (FDA) Medwatch system.1
Conclusion
There are many good reasons for all dentists—even those who don’t offer in-office whitening themselves—to be well versed in tooth whitening procedures and products, including their risks and benefits, and to actively support their patients’ desire to improve the color of their teeth. By inquiring about this concern and screening patients for medical sources of discoloration, they can reinforce their role as a trusted provider of oral health information while being poised to help patients avoid ineffective treatments or deal with uncomfortable side effects.
Candidates cleared for whitening after a thorough examination should also be screened for sensitivity, and if it occurs as a result of any type of treatment, be offered treatments such as with 5% potassium nitrate with fluoride. In addition, dentists who offer highly effective in-office treatment should take steps to prevent or reduce side effects by minimizing agent contact with tissues..
The dental team can also help manage patients’ expectations—eg, the cost of treatment, length of time required to effectively treat different types of stains, and the limitations of bleaching restored teeth.
Finally, patients planning to use at home products should be able to turn to their practitioner for substantive advice on the most effective and safe among them, and how to get best results. In this regard, the dental team can offer product recommendations based on science and their experience with the products. As highly trusted providers of health care services, oral healthcare professionals are in a unique position to work closely with their patients to help them choose and use safe and effective products that improve outcomes and increase satisfaction.
References
1. Tooth whitening/bleaching: treatment considerations for dentists and their patients. ADA Council on Scientific Affairs. September 2009 (revised November 2010). https://www.ada.org/sections/about/pdfs/HOD_whitening_rpt.pdf. Accessed April 5, 2013.
2. Haywood VB. The pre-bleaching exam: components and considerations. Inside Dental Assisting. January/February 2013. https://www.cdeworld.com/courses/4650. Accessed April 15, 2013.
3. Strassler HE, Professionally dispensed vital tooth bleaching: an update on the newest whitening materials. Inside Dentistry. March 2010;6(3). https://www.dentalaegis.com/id/2010/03/professionally-dispensed-vital-tooth-bleaching. Accessed April 15, 2013.
4. Feiglin B. Dental pulp response to traumatic injuries—a retrospective analysis with case reports. Endod Dent Traumatol. 1996;12(1):1-8.
5. Haywood VB, DiAngelis AJ. Bleaching the single dark tooth. Inside Dentistry. 2010;6(8):42-52.
6. da Costa J. The tooth-whitening process: an update. Compend Contin Educ Dent. 2012; Nov/Dec. https://www.cdeworld.com/courses/4633. Accessed April 15, 2013.
7. Strassler HE. At-home vital tooth bleaching. Inside Dentistry. February 2011. https://www.dentalaegis.com/id/2011/02/at-home-vital-tooth-bleaching-a-current-status-update-on-professionally-dispensed-and-otc-methods. Accessed April 5, 2013.
8. Haywood VB, Leonard RH, Dickinson GL. Efficacy of six-months nightguard vital bleaching of tetracycline-stained teeth. J Esthet Dent. 1997;9(1):13-19.
9. Haywood VB. Pre-bleaching exam vital for optimum whitening. Compend Contin Educ Dent. 2012:33(1). https://www.dentalaegis.com/cced/2012/01/pre-bleaching-examination-for-optimum-tooth-whitening. Accessed April 15, 2013.
10. McCaslin AJ, Haywood VB, Potter BJ, et al. Assessing dentin color changes from nightguard vital bleaching. J Am Dent Assoc. 1999;130(10):1485-1490.
11. Marshall K, Berry TG, Woolum J. Teeth whitening considerations. Inside Dental Assisting. January/February 2012. https://www.cdeworld.com/courses/4575. Accessed April 15, 2013.
12. Haywood VB. In-office bleaching: Lights, applications, and outcomes. Current Practice. 2009;6(4).
13. da Costa JB, McPharlin R, Paravina RD, Ferracane JL. Comparison of at-home and in-office tooth whitening using a novel shade guide. Oper Dent. 2010;35(4):381-388.
14. Demarco FF, Meireles SS, Masotti AS. Over-the-counter whitening agents: a concise review. Braz Oral Res. 2009;23 Suppl 1:64-70.
15. Strassler HE. Professional tooth whitening: a minimally invasive esthetic treatment. Inside Dental Assisting. September/October 2012. https://www.dentalaegis.com/ida/2012/10/professional-tooth-whitening-a-minimally-invasive-esthetic-treatment. Accessed April 8, 2013.
16. Swift E. Tooth sensitivity and whitening. Compend Contin Educ Dent. 2005;26(9 Suppl 3):4-10.
17. Attin T, Hanniq C, Wiegand A, Attin R. Effect of bleaching on restorative materials and restorations-a systematic review. Dent Mater. 2004;20:852-861.
18. Munro IC, Williams GM, Heymann HO, et al. Tooth-whitening products and the risk of oral cancer. Food Chem Toxicol. 2006;44(3):301-315.
19. Mahony C, Felter SP, McMillan DA. An exposure-based risk assessment approach to confirm the safety of hydrogen peroxide for use in home tooth bleaching. Regul Toxicol Pharmacol. 2006;44(2):75-82.